International Journal of Anesthetics and Anesthesiology
Severe Respiratory Suppression Secondary to Buprenorphine Treated with Volume Assured Pressure Support (VAPS)
Robert J Farney1*, Boaz Markewitz1, Amanda M McDonald2 and Jill Rhead3
1University of Utah School of Medicine, 50 North Medical Drive, Salt Lake City, Utah 84108, USA
2Intermountain Sleep Disorders Center, LDS Hospital, Salt Lake City, Utah 84143, USA
3Department of Surgery, Intermountain Medical Center, 5121 Cottonwood St, Murray UT 84157, USA
*Corresponding author: Robert J Farney, University of Utah School of Medicine, 50 North Medical Drive, Salt Lake City, Utah 84108, USA, E-mail: robertjfarney@gmail.com
Int J Anesthetic Anesthesiol, IJAA-2-035, (Volume 2, Issue 4), Case Report; ISSN: 2377-4630
Received: October 13, 2015 | Accepted: November 13, 2015 | Published: November 16, 2015
Citation: Farney RJ, Markewitz B, McDonald AM, Rhead J (2015) Severe Respiratory Suppression Secondary to Buprenorphine Treated with Volume Assured Pressure Support (VAPS). Int J Anesthetic Anesthesiol 2:035. 10.23937/2377-4630/2/4/1035
Copyright: © 2015 Farney RJ, et al. This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited.
Abstract
The optimal therapy of chronic opioid induced sleep disordered breathing (SDB) is unclear. Supplemental oxygen may potentially prolong central apneas and increase respiratory suppression. Continuous positive airway pressure (CPAP) is generally ineffective or may even augment central apneas. Therapy with an Adaptive Servo-Ventilation (ASV) device is the most successful option for most etiologies of central apnea including opioids, but we have observed a subpopulation with OISDB that do not respond well.
We evaluated a 31 year-old female by means of serial attended polysomnography who was admitted for opioid detoxification and who developed severe respiratory suppression following induction therapy with buprenorphine/naloxone. Opioid induced SDB was manifest by bradypnea, ataxic breathing, central apnea (apnea/hypopnea index or AHI 107/hr) and hypoxemia (SpO2 74%). Supplemental oxygen corrected hypoxemia but severe central apnea and bradypnea persisted. ASV was ineffective despite high pressure settings (AHI 122/hr). Ventilation was normalized (AHI 1/hr) and hypoxemia was corrected (SpO2 92%) with volume assured pressure support (VAPS) without supplemental oxygen
The efficacy of ASV in idiopathic central apneas or Cheyne-Stokes respiration may relate to specific pathogenic factors such as high loop gain with low apneic threshold or phase delay related to cardiac disease but with a fundamentally intact respiratory pattern generator. In patients with opioid induced SDB, the pattern generator appears dysfunctional. In these cases, VAPS in which maintenance of alveolar ventilation is the primary goal may be superior to ASV in which prevention of hyperventilation overshoot and hypocapnia are the objectives. Attended polysomnography is necessary in order to reliably validate the efficacy of therapy.
Keywords
Opioids, Buprenorphine/Naloxone (Suboxone), Central sleep apnea, Biot's respiration/Ataxic breathing, Adaptive Servo-Ventilation, Volume Assured Pressure Support
Abbreviations
SDB: Sleep Disordered Breathing, AHI: Apnea plus Hypopnea Index, CPAP: Continuous Positive Airway Pressure, ASV: Adaptive Servo-Ventilation, PS: Pressure Support, EPAP: Expiratory Positive Airway Pressure, VAPS: Volume Assured Pressure Support
Introduction
The prevalence of sleep disordered breathing associated with chronic μ-opioid therapy, including partial agonists, varies from 42 to 85% [1,2]. Central apnea and ataxic breathing are the most characteristic manifestations of opioid induced sleep disordered breathing [3-6], however non-apneic hypoxemia and obstructive apneas are also observed [7]. Unfortunately, treatment in these cases is usually challenging and there are no consensus guidelines that define indications or therapy for opioid-related breathing disturbances. The main options include withdrawal or reducing the dose of opioids, selecting a semi-synthetic partial μ-opioid agonist (e.g. buprenorphine in lieu of methadone [8-12]), avoidance of other potential respiratory suppressants, supplemental oxygen and positive airway pressure. Continuous positive airway pressure (CPAP) is generally ineffective [13-15]. Bilevel pressure therapy, particularly using adaptive servo-ventilation (ASV), is often but not consistently successful [13-16]. In the present case, ASV was unsuccessful however bi-level positive airway pressure using a volume assured pressure support device (VAPS) was efficacious.
Case Report
31 year old female with opioid dependency (roxycodone 180 mg/day) was admitted for detoxification with buprenorphine/naloxone 2.0 mg/0.5 mg (Suboxone). She took her last roxycodone dose (30 mg) 72 hours before admission at which time she was experiencing withdrawal symptoms of aches, pains, nausea, vomiting, diarrhea, hot and cold sweats. She had a history of sleep onset and maintenance insomnia, loud disruptive snoring, nocturnal gasping, bruxism, somniloquy, morning headaches, and hypersomnolence. She denied symptoms of restless legs syndrome, involuntary sleep attacks, sleep paralysis and cataplexy. Co-morbid conditions included anxiety/depression and obesity (81.8 kg, 165 cm, BMI 30 kg/m2). Neck circumference measured 40.5 cm and pharynx was Mallampati Class IV.
Therapy with Suboxone was initiated 24 hours after admission (onesublingual tablet twice per day and one tablet as needed every two hours). Other prescribed medications included clonazepam (Klonopin) 0.5 mg, methocarbamol (Robaxin) 750 mg, duloxetin (Cymbalta) 60 mg, andolanzapine (Zyprexa) 10 mg.
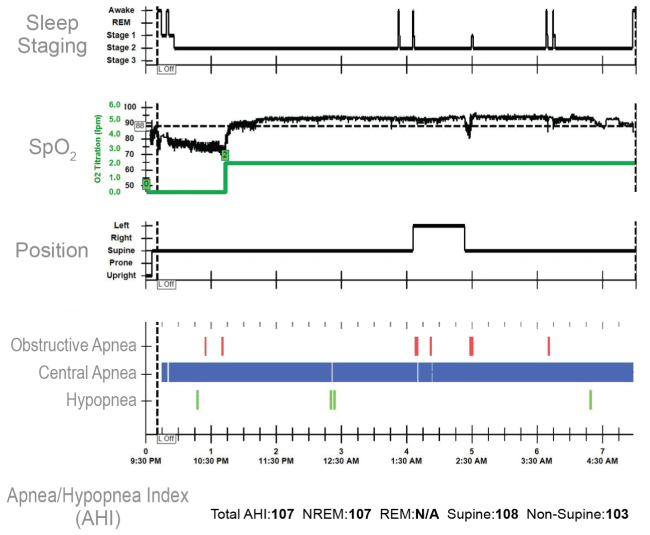
.
Figure 1A: Baseline Polysomnogram with room air and oxygen breathing (2 L/min via nasal cannula).
Standard attended 19-channel polysomnography was performed and manually scored according to criteria established by the American Academy of Sleep Medicine [24]. Airflow was detected by nasal pressure transducer and by oral-nasal thermistors. Apneas were scored on the basis of absence of thermistor airflow for ≥ 10 seconds. Obstructive apneas were defined by the presence of respiratory effort; central apneas by the absence of respiratory effort. Hypopneas were defined as a ≥ 30% reduction in airflow for 10 seconds associated with ≥ 3% decrease in SpO2. The Apnea/Hypopnea Index (AHI) was computed as the total of defined respiratory events divided by the total sleep time in hours. The AHI was determined for the total night, during non-rapid eye movement, rapid eye movement, supine and non-Supine sleep.
View Figure 1A
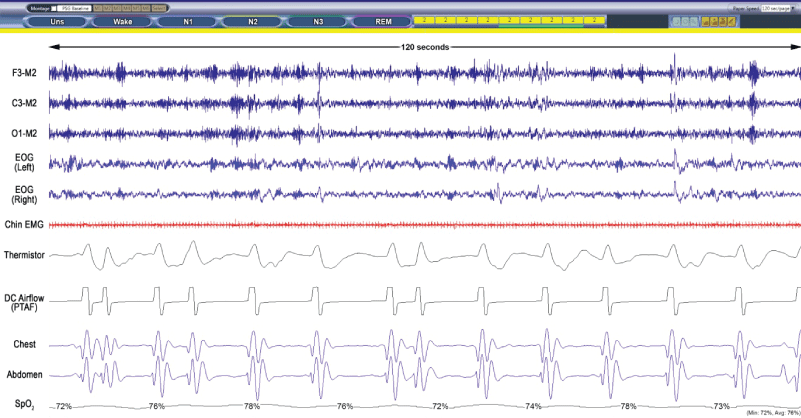
.
Figure 1B: Baseline Polysomnogram raw data breathing room air (120 s).
Screenshot obtained during Stage N2 while breathing room air. The patient was mostly supine and slightly elevated on several pillows. The respiratory pattern is characterized as irregular or ataxic with frequent central apneas of variable duration. The respiratory rate measured 7/min and the SpO2 nadir measured 74%. The central AHI measured 105/hour and the obstructive AHI measured 1/hour sleep. There was no positional difference in the AHI.
View Figure 1B
Forty-five hours after receiving her first dose of Suboxone and 20 minutes after her last scheduled evening dose at bedtime (total dose of ten tablets), she underwent comprehensive polysomnography (Figure 1A). Sleep architecture was notable for absent rapid eye movement sleep and nearly continuous uninterrupted Stage N2 sleep. Nasal cannula oxygen (2 L/min) was added due to severe hypoxemia (SpO276 - 86%) and bradypnea (6/min), noted even while awake during biocalibrations. Measurements of PaCO2 or surrogates were not available. The apnea/hypopnea index (AHI) measured 107/hour with almost all central apneas and mild ataxic breathing (Figure 1B). Hypoxemia was corrected with oxygen however the underlying apneas and ataxic breathing persisted (Figure 1C).
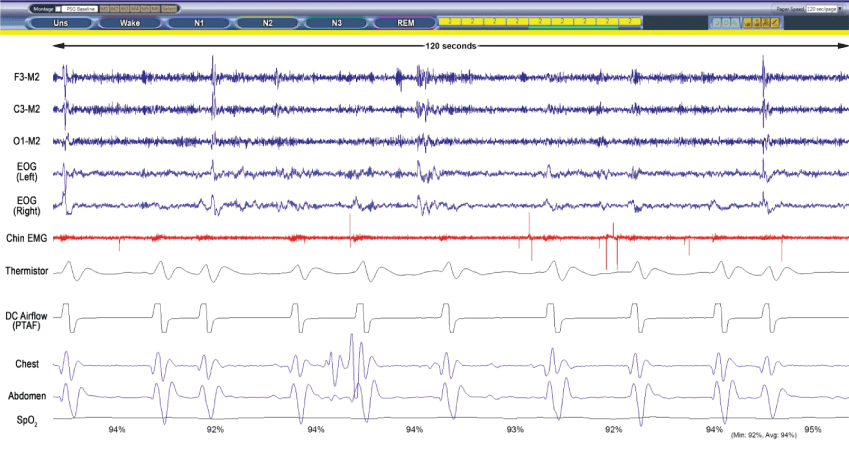
.
Figure 1C: Baseline Polysomnogram raw data breathing oxygen (120 s).
Screenshot obtained during Stage N2 while breathing supplemental oxygen. Ataxic breathing with central apneas that tended to be slightly prolonged compared to room air breathing. The respiratory rate measured approximately 5/min with a SpO2 of 92-94%.
View Figure 1C
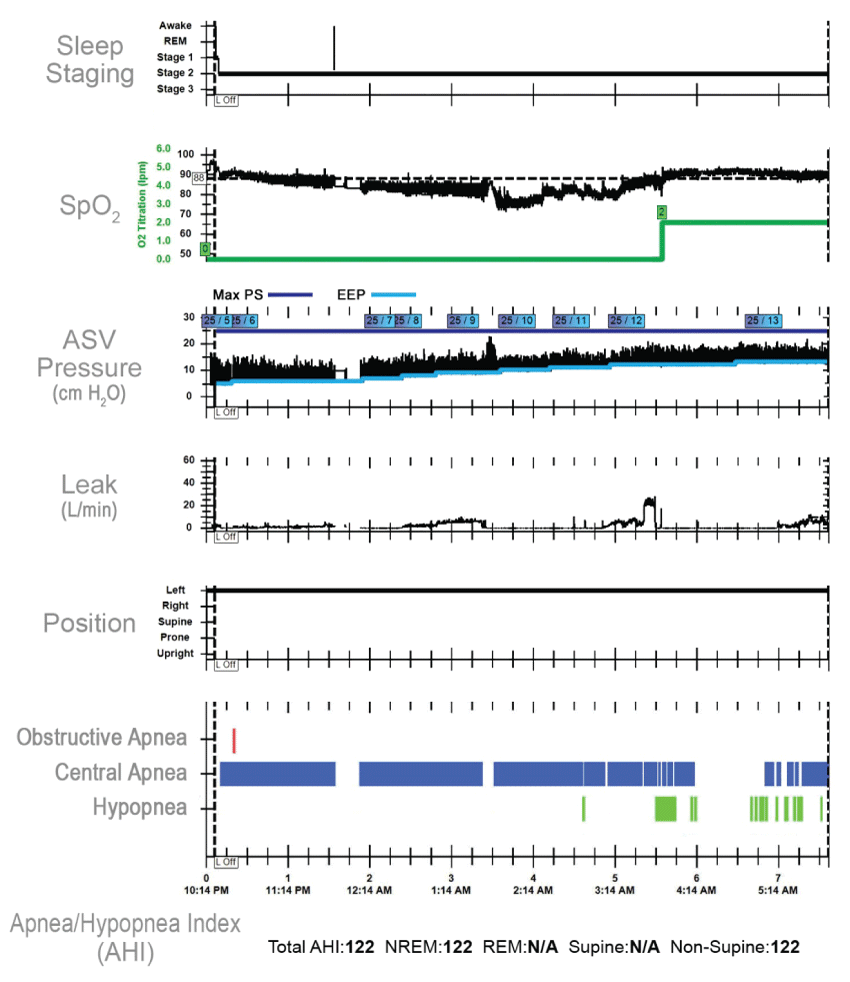
.
Figure 2A: ASV Polysomnogram breathing room air and oxygen.
See Legend for Figure 1A regarding polysomnography and text for details of ASV parameters. The actual expiratory positive airway pressure (EPAP) and variable inspiratory pressures are shown above in the third panel (black). The set maximal inspiratory pressure is shown in dark blue and the set EPAP is shown in light blue. Of note, the sleep pattern is highly unusual and consists of essential uninterrupted Stage N2 without rapid eye movement sleep or awakenings.
View Figure 2A
Suboxone was continued in order to manage withdrawal symptoms and polysomnography was repeated on subsequent nights. A full face mask was used on each night. Despite maximal therapy with ASV (expiratory positive airway pressure or EPAP of 5 - 13, pressure support or PS of 3 - 15 and maximum pressure 25 cm H2O) and supplemental oxygen (2 L/min), central apneas and ataxic breathing persisted (AHI 122/hour) (Figures 2A, Figure 2B and Figure 2C).
.
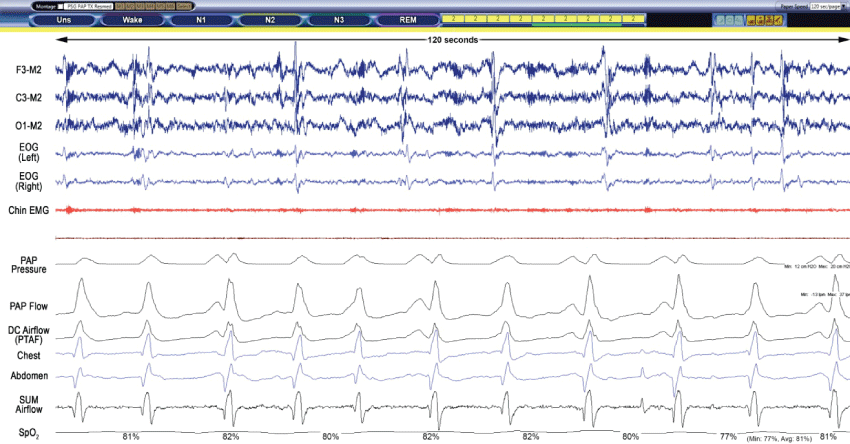
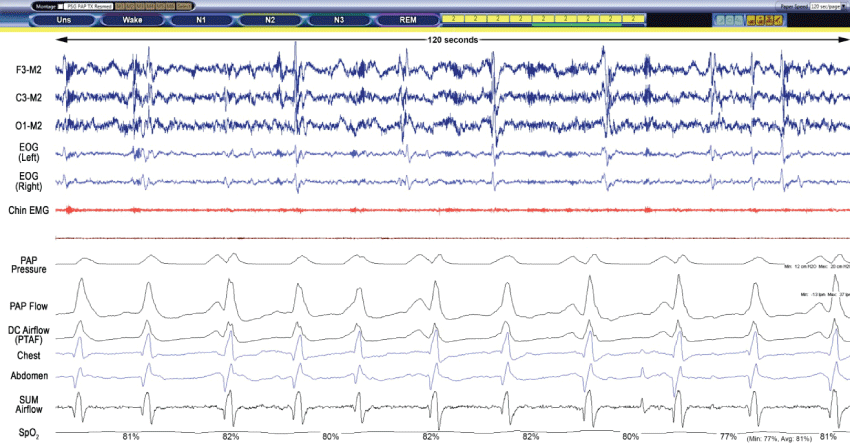
Figure 2B: ASV Polysomnogram raw data breathing room air (120 s).
Screenshot obtained during Stage N2 while breathing room air and EPAP 12-13 cm H2O. The underlying rhythm is slightly irregular but mainly consists of isolated breaths with a rate of 5/min and hypoxemia (SpO2 nadir 77%).
View Figure 2B
.
Figure 2C: ASV Polysomnogram raw data breathing oxygen (120 s).
Screenshot obtained during Stage N2 while breathing supplemental oxygen and EPAP 13.0 cm H2O. There appear to be a few meager attempts to breathe with an effective respiratory rate of approximately 4/min and SpO2 of 92%.
View Figure 2C
With VAPS (tidal volume/kg 10 ml, respiratory rate 12/min, EPAP of 4-8 and PS of 3 - 15 cm H2O), arterial oxygenation was stable (mean SpO2 91%) and the AHI measured 1/hour (Figure 3A and Figure 3B). Rapid eye movement sleep was absent on all studies with positive airway pressure, consistent with our earlier descriptions of patients with opioid induced SDB [4,13].

.
Figure 3A: VAPS Polysomnogram breathing room air.
See Legend for figure 1A regarding polysomnography and text for details of VAPS parameters. The actual end-expiratory pressure (EPAP) and variable inspiratory pressures are shown above in the third panel (black). The set maximal inspiratory pressure is shown in dark blue and the set EPAP is shown in light blue.
View Figure 3A
.
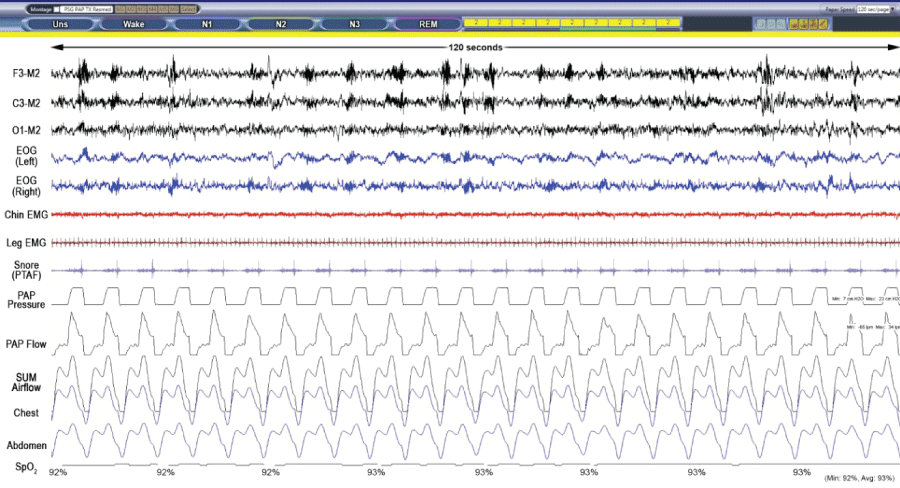
Figure 3B: VAPS Polysomnogram raw data breathing room air (120 s).
Screenshot obtained during Stage N2 while breathing room air and EPAP 8 cm H2O. The SpO2 measured 92% and the respiratory rate was 12/min.
View Figure 3B
Discussion
The optimal respiratory therapy for patients with opioid induced sleep disordered breathing is unclear. For example, the efficacy of oxygen with or without any modality of positive airway pressure during sleep has not been scientifically evaluated although supplemental oxygen is often used clinically. Experimental evidence in awake normal volunteers shows that respiratory depression from remifentanil infusion is more pronounced in hyperoxia than normoxia [17]. At the present time, bilevel positive airway pressure with fixed pressures and a back-up rate or servo-adaptive devices with variable pressure support, set or variable EPAP and back-up rate (e.g. ASV) appear to be the most effective therapy [14,15]. Nevertheless, marked respiratory disturbances may persist in some patients despite maximal or near maximal positive airway pressure settings [13,18].
Advancements of our understanding of the pathogenesis of sleep apnea have been crucial for expanding options and optimizing therapy for obstructive sleep apnea [19]. Successful treatment of obstructive sleep apnea, at least as measured by reduction of the AHI, is most often accomplished by strategies to mechanically stabilize collapsible airways, for example with CPAP. However, in addition to the intrinsic properties of the airway, the pathogenesis of obstructive apnea is also a function of high loop gain and the arousal response. Accordingly, alternative treatments that are focused on optimizing respiratory control or drive may be beneficial such as: (1) reduction of chemoreceptor gain with supplement oxygen; (2) reduction of plant gain with selective increments of inspiratory CO2; and (3) sedatives to blunt the exaggerated arousal response and ventilatory overshoot [19].
Compared to obstructive sleep apnea, the pathogenesis of sleep disordered breathing associated with opioids is more complex, underscored by the diversity of pathologic breathing patterns that are observed in clinical practice. In some case series, obstructive apneas have been reported [15], however opioids more often alter respiratory pattern generation leading to bradypnea, ataxia and central apneas [2-4] as in the present case. The central apnea patterns are highly variable and may be characterized by fairly regular intervals with clusters of a few breaths with differing tidal volumes or by markedly irregular underlying breathing patterns with interspersed apneas. Very long hypopneas and profound hypoxemia may occur that presumably reflects reduced respiratory drive and suppressed arousal responses.
Periodic breathing such as Cheyne-Stokes respiration is associated with a hypersensitive feedback loop (i.e. elevated loop gain) and effectiveness of positive airway pressure therapy may be predicted based on the estimation of loop gain [20]. It appears that the pattern generator is intrinsically intact but the characteristic waxing and waning of tidal volume pattern is produced due to misaligned afferent information and efferent output. Similarly, the pathogenesis of idiopathic central sleep apnea is probably due to a low apnea threshold with high loop gain and low arousal threshold. In both cases, the respiratory pattern generator is intrinsically normal. The underlying respiratory rates are not irregular. The effectiveness of adaptive servo-ventilation is achieved because the bi-level pressure device algorithms stabilize the PCO2 so that the pattern generator does not create hyperventilation overshoot, hypocapnia and secondary central apneas.
In contrast, there is no evidence at this point that implicates hypocapnia secondary to high loop gain or exaggerated arousal responses with opioid breathing disturbances. Opioids interfere with the basic pattern generating process such that irregular breathing patterns are produced with both variable rate and amplitude. These disturbances have been attributed to blockade of opioid sensitive neurons located in the pre-Botzinger complex and preservation of "quantal" breathing rhythm with opioid insensitive pre-inspiratory neurons located in the retrotrapezoid nucleus/parafacial respiratory group [21,22].
There are two positive pressure devices with multiple modalities used for in-lab titration studies of patients with sleep apnea (Philips Respironics Omnilab and ResMed VPAP Tx). In the present case, we used the ResMed system. Importantly, there are substantial proprietary differences of the internal machine algorithms [23]. With both devices, expiratory positive airway pressure (EPAP) can be variable or set in order maintain upper airway patency and to eliminate obstructive apneas. Inspiratory pressure support (PS) varies to adjust tidal volume and eliminate central apneas. A backup respiratory rate is optional on the Philips Respironics Omnilab but is automatic on the ResMed VPAP Tx.
ASV therapy may not be optimal in opioid patients with hypoventilation or severe respiratory suppression as reflected by bradypnea in the present case. Volume assured pressure support might be more appropriate similar to patients with neuromuscular or obstructive pulmonary diseases. In order to explore the pathogenesis and define the best pressure therapy for patients with opioid induced SDB, further studies are needed in which both modalities are compared. Whether or not positive pressure devices with different proprietary algorithms for delivering adaptive servo-ventilation or volume assured pressure support are interchangeable also needs to be considered.
Disclosure Statement
We have no financial support, conflict of interest, off-label or investigational use of product to report.
References
-
Correa D, Farney RJ, Chung F, Prasad A, Lam D, et al. (2015) Chronic opioid use and central sleep apnea: a review of the prevalence, mechanisms, and perioperative considerations. Anesth Analg 120: 1273-1285.
-
Farney RJ, McDonald AM, Boyle KM, Snow GL, Nuttall RT, et al. (2013) Sleep disordered breathing in patients receiving therapy with buprenorphine/naloxone. Eur Respir J 42: 394-403.
-
Farney RJ, Walker JM, Cloward TV, Rhondeau S (2003) Sleep-disordered breathing associated with long-term opioid therapy. Chest 123: 632-639.
-
Walker JM, Farney RJ, Rhondeau SM, Boyle KM, Valentine K, et al. (2007) Chronic opioid use is a risk factor for the development of central sleep apnea and ataxic breathing. J Clin Sleep Med 3: 455-461.
-
Teichtahl H, Prodromidis A, Miller B, Cherry G, Kronborg I (2001) Sleep-disordered breathing in stable methadone programme patients: a pilot study. Addiction 96: 395-403.
-
Wang D, Teichtahl H, Drummer O, Goodman C, Cherry G, et al. (2005) Central sleep apnea in stable methadone maintenance treatment patients. Chest 128: 1348-1356.
-
Sharkey KM, Kurth ME, Anderson BJ, Corso RP, Millman RP, et al. (2010) Obstructive sleep apnea is more common than central sleep apnea in methadone maintenance patients with subjective sleep complaints. Drug Alcohol Depend 108: 77-83.
-
Johnson RE, Fudala PJ, Payne R (2005) Buprenorphine: considerations for pain management. J Pain Symptom Manage 29: 297-326.
-
Kahan M, Srivastava A, Ordean A, Cirone S (2011) Buprenorphine: new treatment of opioid addiction in primary care. Can Fam Physician 57: 281-289.
-
Walsh SL, Preston KL, Stitzer ML, Cone EJ, Bigelow GE (1994) Clinical pharmacology of buprenorphine: ceiling effects at high doses. Clin Pharmacol Ther 55: 569-580.
-
Dahan A, Yassen A, Bijl H, Romberg R, Sarton E, et al. (2005) Comparison of the respiratory effects of intravenous buprenorphine and fentanyl in humans and rats. Br J Anaesth 94: 825-834.
-
Dahan A, Yassen A, Romberg R, Sarton E, Teppema L, et al. (2006) Buprenorphine induces ceiling in respiratory depression but not in analgesia. Br J Anaesth 96: 627-632.
-
Farney RJ, Walker JM, Boyle KM, Cloward TV, Shilling KC (2008) Adaptive servoventilation (ASV) in patients with sleep disordered breathing associated with chronic opioid medications for non-malignant pain. J Clin Sleep Med 4: 311-319.
-
Javaheri S, Harris N, Howard J, Chung E (2014) Adaptive servoventilation for treatment of opioid-associated central sleep apnea. J Clin Sleep Med 10: 637-643.
-
Guilleminault C, Cao M, Yue HJ, Chawla P (2010) Obstructive sleep apnea and chronic opioid use. Lung 188: 459-468.
-
Cao M, Cardell CY, Willes L, Mendoza J, Benjafield A, et al. (2014) A novel adaptive servoventilation (ASVAuto) for the treatment of central sleep apnea associated with chronic use of opioids. J Clin Sleep Med 10: 855-861.
-
Niesters M, Mahajan RP, Aarts L, Dahan A (2013) High-inspired oxygen concentration further impairs opioid-induced respiratory depression. Br J Anaesth 110: 837-841.
-
Farney RJ, Walker JM (2015) Central Sleep Apnea Due to Medication or Substance. In: Olsen E.J. WJW, editor. Case Book of Sleep Medicine International Classification of Sleep Disorders. (2nd edn) American Academy of Sleep Medicine 201-207.
-
Dempsey JA, Smith CA2 (2014) Pathophysiology of human ventilatory control. Eur Respir J 44: 495-512.
-
Sands SA, Edwards BA, Kee K, Turton A, Skuza EM, et al. (2011) Loop gain as a means to predict a positive airway pressure suppression of Cheyne-Stokes respiration in patients with heart failure. Am J Respir Crit Care Med 184: 1067-1075.
-
Mellen NM, Janczewski WA, Bocchiaro CM, Feldman JL (2003) Opioid-induced quantal slowing reveals dual networks for respiratory rhythm generation. Neuron 37: 821-826.
-
Janczewski WA, Feldman JL (2006) Distinct rhythm generators for inspiration and expiration in the juvenile rat. J Physiol 570: 407-420.
-
Javaheri S, Brown LK, Randerath WJ (2014) Positive airway pressure therapy with adaptive servoventilation: part 1: operational algorithms. Chest 146: 514-523.
-
Berry RB, Gamaldo CE, Harding SM, Lloyd RM, Marcus CL, et al. (2015) The AASM Manual for the Scoring of Sleep and Associated Events: Rules, Terminology and Technical Specifications, Version 2.2 http://www.aasmnet.org. Darien, Illinois: American Academy of Sleep Medicine.





