International Journal of Anesthetics and Anesthesiology
The Effects of High-Dose Sugammadex on Erythrocyte Deformability in Rats with Renal Failure Generated by Unilateral Ureteral Obstruction
Füsun Bozkirli1, Fikriye Dogrul1, Faruk Metin Comu2, Hande Arpaci3, Ömer Bayrak4, Mustafa Arslan1* and Yusuf ünal1
1Department of Anaesthesiology and Reanimation, Gazi University Medical Faculty, Turkey
2Department of Physiology, Kirikkale University Medical Faculty, Turkey
3Department of Oral and Maxillofacial Surgery, Ankara University Faculty of Dentistry (Anaesthesiology Reanimation specialist), Turkey
4Department of Urology, Gazi University Medical Faculty, Turkey
*Corresponding author: Dr. Mustafa Arslan, Gazi University Medical Faculty, Department of Anaesthesiology and Reanimation, 06510 Ankara, Turkey, Tel: 90-312-202-67-39, E-mail: marslan36@yahoo.com/mustarslan@gmail.com
Int J Anesthetic Anesthesiol, IJAA-2-032, (Volume 2, Issue 3), Original Article; ISSN: 2377-4630
Received: April 14, 2015 | Accepted: August 15, 2015 | Published: August 18, 2015
Citation: Bozkirli F, Dogrul F, Comu FM, Arpaci H, Bayrak O, et al. (2015) The Effects of High-Dose Sugammadex on Erythrocyte Deformability in Rats with Renal Failure Generated by Unilateral Ureteral Obstruction. Int J Anesthetic Anesthesiol 2:032. 10.23937/2377-4630/2/3/1032
Copyright: © 2015 Bozkirli F, et al. This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited.
Abstract
Background: Obstructive nephropathy is a common cause of renal insufficiency in adults. Unilateral ureteral obstruction (UUO) is a well-established model known to imitate the process of obstructive nephropathy in a simple, accelerated and species-independent manner. Free oxygen radicals also have been reported to be involved in the formation of renal damage. Erythrocyte deformability and plasma viscosity are of crucial importance in the perfusion of tissues and organs. The aim of this study is to evaluate the effect of high dose Sugammadex on erythrocyte deformability UUO in rats.
Materials and methods: 30 male Wistar albino rats weighing between 225 and 300 gm were randomly divided into five groups. Group C (control; n=6), Group UUO-1 week (UUO-1; n=6), Group UUO-1 week-96S (UUO-1-rocuronium-96mg sugammadex; n=6), Group UUO-3 week (UUO-3; n=6) and Group UUO-3 week-96S (UUO-3- rocuronium-96mg sugammadex; n=6). Rats in the control and UUO groups received NaCl 0.9% at the same volume. At the end of of the follow-up period, animals' erythrocyte deformability was measured from blood samples.
Results: The deformability index was significantly increased in the UUO rats (p<0.0001). It was significantly increased in Group UUO-3-96S when compared to Group C, UUO-1 and UUO-3 (p<0.0001, p=0.016, p=0.007, respectively).
Conclusion: In this study we showed the safety profile of high-dose Sugammadex in UUO-1 rats in terms of erythrocyte deformability. But after three weeks of UUO, high-dose of Sugammadex implementation affected erythrocyte deformability. Our findings may lead future animal and human studies to investigate the effects of Sugammadex on erythrocyte deformability and micro/macrovascular circulation.
Keywords
Erythrocyte deformability, Unilateral ureteral obstruction, Sugammadex
Introduction
One of the most common causes of renal insufficiency in children and adults is obstructive nephropathy. Unilateral ureteral obstruction (UUO) is a well-known model to imitate the obstructive nephropathy process in a simple, accelerated and species-independent manner [1,2]. Previous studies have revealed that morphological lesions in the obstructed kidney are peritubular capillaries rarefaction, tubular atrophy, inflammatory infiltration, widen interstitial space, and progressive tubulointerstitial fibrosis [3,4]. Compensatory hypertrophy of the contralateral kidney is another characteristic feature in the UUO [5].
Hu et al showed that the ratio of kidney weight to body weight gradually declined in the obstructed kidney 72 hours to 2 weeks after ligation, and the cortical thickness also decreased time-dependently from 24 hours to 3 months post-ligation in another study published in Peptides [6]. In the contralateral kidney, the glomerular size gradually increased throughout the observation period, which is capable of compensating for the damaged renal unit of the obstructed kidney [5]. Both animal models and human kidney biopsy studies have shown that the hypertrophy of the contralateral kidney is another typical feature of obstructive nephropathy [2].
Because of the obstruction, of the obstruction, pathological changes in glomerular and particularly interstitial fields occur with the effect of several vasoactive factors and cytokines. Leukocyte infiltration plays the most important role in the development of obstructive nephropathy. Free oxygen radicals have also been reported to play a role in the formation of renal damage, in addition to the factors of prostaglandins (PG), angiotensin (ANG) II, growth factors and nitric oxide (NO) [7].
Sugammadex is a new agent that is used for the rapid reversal the effects of steroid structured non depolarizan muscle relaxants (NDMR) (primarily rocuronium, and to a lesser extent vecuronium) on tissue [8]. The safety profile and use of Sugammadex at 2mg/kg and 4mg/kg has been shown [8]. The reported side-effects of Sugammadex include non-specific hypotension, coughing and anaphylaxis, although the latter is a matter of ongoing debate [9]. In addition, several studies have suggested an elongated clotting time with Sugammadex, although a recent study showed no significant difference between measured clotting time values of patients treated with Sugammadex and control groups [10]. In this study we investigated the effect of high-dose Sugammadex on erythrocyte deformability of unilateral ureteral obstruction in rats.
Materials and Methods
Animals and experimental protocol
This study was conducted in the GUDAM Laboratory of Gazi University with the consent of the Experimental Animals Ethics Committee of Gazi University. All the procedures were performed according to the accepted standards of the Guide for the Care and Use of Laboratory Animals.
In the study, raised under the same environmental conditions, were used. For at least one week prior to surgery, the animals were housed in standard cages in a pathogen-free environment, with free access to food (until 2 h before the anaesthetic procedure) and water and with a 12h light/dark cycle. The animals were randomly separated into four groups, each containing six rats.
30 male Wistar albino rats weighing between 225 and 300 gm were randomly divided into five groups. Group C (control; n=6), Group UUO-1 week (UUO-1; n=6), Group UUO-1 week-96S (UUO-1-rocuronium-96mg sugammadex; n=6), Group UUO-3 week (UUO-3; n=6) and Group UUO-3 week-96S (UUO-3- rocuronium-96mg sugammadex; n=6).
Renal failure was induced in the left ureter distal of four groups of rats (Early Period Renal Failure-Control, Early Period Renal Failure-1mg/kg Rocuronium-96mg/kg Sugammadex, Late Period Renal Failure-Control, Late Period Renal Failure-1mg/kg Rocuronium-96mg/kg Sugammadex) under ketamine anesthesia with a low abdominal incision, and then the suture was placed with 2.0 mersilene and was kept there for 1 week for the early period, and 3 weeks for the late period.
At the end of 1 week for the early period and 3 weeks for the late period, 100mg.kg-1 ketamine was administered intraperitoneally and tracheostomy was performed in all the animals in the supine position via 12G cannula; intubation was performed on all animals. The oesophaguses of animals were strictly protected while the tracheostomy was being performed. Intubation cannula was fixed carefully. Ventilation was maintained by a ventilatory machine at room temperature. Rate was 70-100/min, tidal volume was 2.5-3 ml and positive end-expiratory pressure was 2mmHg.
There were five experimental groups: Group C (control; n=6), Group UUO-1 week (UUO-1; n=6), Group UUO-1 week-96S (UUO-1-rocuronium-96mg sugammadex; n=6), Group UUO-3 week (UUO-3; n=6) and Group UUO-3 week-96S (UUO-3- rocuronium-96mg sugammadex; n=6). The rats in the control and UUO groups received NaCl 0.9% at the same volume. Following the reversal of the muscle-relaxant effects of rocuronium, rats were allowed to breathe spontaneously.
Anaesthesia was maintained by repetitive injections of 20mg.kg-1 ketamine if a positive reaction to surgical stress or intermittent tail pinch was observed.
After the two-hour follow-up period intracardiac blood samples were obtained from all the rats. Heparinized total blood samples were used to prepare erythrocyte packs. Deformability measurements were performed using erythrocyte suspensions with 5% haematocrit in a phosphate-buffered saline (PBS) buffer.
Deformability measurements
Blood samples were carefully taken, and the measurement process was as fast as possible to avoid haemolysis of the erythrocytes. The collected blood was centrifuged at 1000rpm for 10 min. Serum was removed, in addition to the buffy coat on the erythrocytes. An isotonic PBS buffer was added to the collapsing erythrocytes, and this was centrifuged at 1000 rpm for 10 min. The liquid on the upper surface was removed. Finally, pure red cell packs were obtained from the washing process, which was repeated three times. The erythrocyte packs were mixed with the PBS buffer to generate a suspension with a value of 5% Htc. These erythrocyte suspensions were used for the measurement of deformability. The collection and the deformability measurements of the erythrocytes were performed at 22℃.
A constant-current filtrometer system was used in the measurement of the erythrocyte deformability. Samples to be measured were prepared with 10 ml of erythrocyte suspension and PBS buffer. The flow rate was held constant at 1.5 ml/min with an infusion pump. A 28mm nucleoporin polycarbonate filter with a 5μm pore diameter was preferred. Pressure changes while the erythrocytes passed through the filter were detected by a pressure transducer, and the data were transferred to the computer with the help of an MP30 data equation system (Biopac Systems Inc., Commat, USA). The calculations were performed with related computer programmes by measuring the pressure changes at various times. Pressure calibration of the system was performed before each sample measurement. The buffer (PT) and the erythrocytes (PE) were passed through the filtration system, and the changes in pressure were measured. The relative refractory period value (Rrel) was calculated by relating the pressure value of the erythrocyte suspension to the pressure value of the buffer. An increasing Rrel in the deformability index was interpreted as adversely affecting the deformability of the erythrocytes [11].
Statistical analysis
The statistical analyses were performed with the SPSS 20.0 software programme; p<0.05 was considered statistically significant. The findings were expressed as mean ± standard deviation. The data were evaluated with Kruskal-Wallis variance analysis. The variables with significance were evaluated with a Bonferroni corrected Mann-Withney U test.
Results
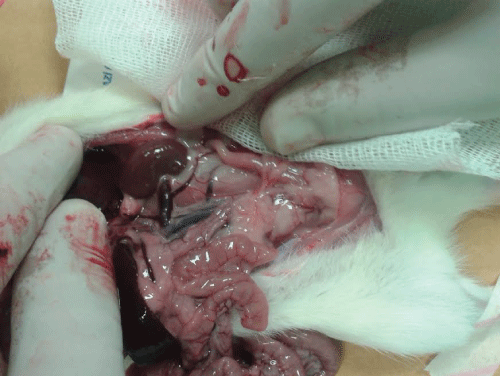
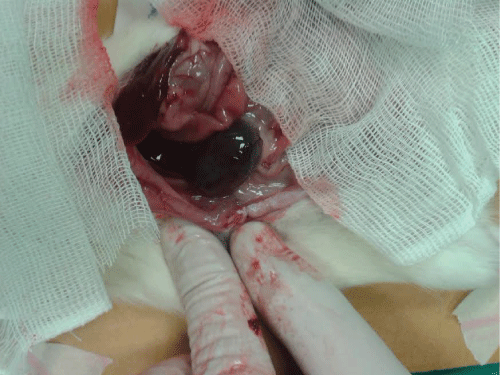
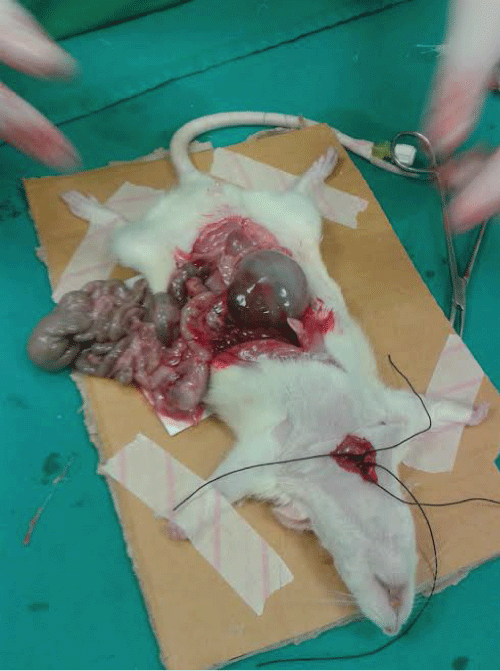
Macroscopic renal appearances of the related groups are shown in figure-1-3.
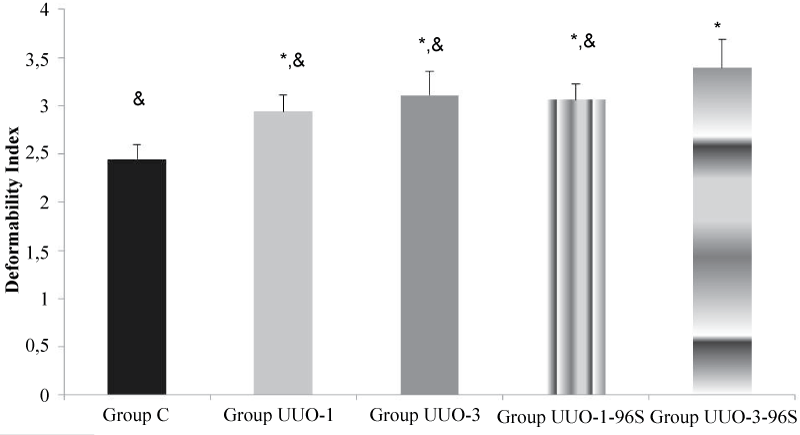
The deformability index was measured 2.44 ± 0.18, 2.94 ± 0.18, 3.11 ± 0.17, 3.06 ± 0.28 and 3.39 ± 0.10 for Group C, UO-1, UO-3, UO-1-96S and UO-3-96S, respectively.
The deformability index was significantly increased in the UUO rats (p<0.0001). However, it was similar in Groups UUO-1 and UUO-1-96S (p=0.258). It was significantly increased in Group UUO-3-96S when compared to Group C, UUO-1 and UUO-3 (p<0.0001, p=0.016, p=0.007, respectively) (Figure 4). The relative resistance was increased in the group UUO-3 high-dose Sugammadex application.
.
Figure 4: Erythrocyte deformability values of the groups. Each bar represents the mean ± sd.
* p<0.05 compared to Group C; & p<0.05 compared to Group UUO-3-96S
View Figure 4
Discussion
Erythrocytes are fundamental elements of blood; they are responsible for vital functions such as oxygen/carbon dioxide and metabolic product exchange. Changes in erythrocyte shape and geometry generate the most important proportion of flow resistance. Erythrocyte deformability, aggregation, plasma fibrinogen and globulins have key roles to play in maintaining a sufficient flow pattern [12].
It has been attributed to platelet dysfunction, abnormal platelet-vessel wall interactions and altered rheological properties of blood flow [13-17].
As summarised by Noris and Remuzzi, uremic bleeding depends on 1. abnormal platelet-vessel wall interactions ( enhanced vascular PGI2 production, altered PGI2 degradation, altered ratio of Factor VIII to von Willebrand Factor), anemia (altered platelet adesion, altered blood rheology), 3. abnormal production of Nitric Oxide and 4. platelet dysfunction (decreased platelet calcium content, reduced ADP platelet pool, reduced cAMP platelet content, reduced platelet capacity to form TxA2 in response to Platelet Activating Factor [18].
The life span of erythrocytes in the circulation seems to be related with the factors affecting the mechanical properties (cell deformability) [19]. In hemodialysis patients, the breakdown of erythrocyte deformability as the result of erythrocyte membrane lipid peroxidation initiated by free radicals and splenic sequestration is reported be among the the most important factors causing a decrease in the life span of erythrocytes [20-23].
Comu et al. reported that they found the results of erythrocyte deformability EI (Elongation index) values, obtained under shear stress of 30, decreased in all groups compared to the control group in their study. Although there was an increase in the Pentoxifylline+Quercetin group in comparison with the ATN group, they stated that it didn't show statistical significance [24].
There is only one study (18) that investigates renal histopathological changes in rats after different doses (16 versus 96mg/ml) of sugammadex. Bostan et al. [25] showed histopathological damage in high dose group (96mg/kg) while blood urea, creatinine and electrolyte levels were similar that in both control and low dose group.
In our study we found that high-dose Sugammadex aplication in UUO-3 is related with impaired erythrocyte deformability while there was no difference the between erythrocyte deformability index of UUO-1 rats treated with high-dose Sugammadex.
According to our study results we can state that high-dose Sugammadex leads to no harmful effects on erythrocyte deformability in UUO-1 rats. But after three weeks UUO of high-dose Sugammadex has affected the implementation of erythrocyte deformability. This is the first study in the literary investigating effects of Sugammadex on erythrocyte deformability of UUO rats. Future human studies may provide an insight into the Sugammadex effect on human erythrocyte deformability and microcirculation.
References
-
Chevalier RL (1999) Molecular and cellular pathophysiology of obstructive nephropathy. Pediatr Nephrol 13: 612-619.
-
Hu P, Zhao XQ, Wang J, Cai J, Hu B, et al. (2013) Simplified stereological evaluation of renal morphology after unilateral ureteral obstruction. Int J Med Sci 10: 385-391.
-
Hu P, Wang J, Zhao XQ, Hu B, Lu L, et al. (2013) Overexpressed C-type natriuretic peptide serves as an early compensatory response to counteract extracellular matrix remodeling in unilateral ureteral obstruction rats. Mol Biol Rep 40: 1429-1441.
-
Yang J, Dai C, Liu Y (2002) Hepatocyte growth factor gene therapy and angiotensin II blockade synergistically attenuate renal interstitial fibrosis in mice. J Am Soc Nephrol 13: 2464-2477.
-
Dicker SE, Shirley DG (1972) Compensatory hypertrophy of the contralateral kidney after unilateral ureteral ligation. J Physiol 220: 199-210.
-
Hu P, Wang J, Hu B, Lu L, Xuan Q, et al. (2012) Increased urinary C-type natriuretic peptide excretion may be an early marker of renal tubulointerstitial fibrosis. Peptides 37: 98-105.
-
Yildiz M, Pekdemir M, Akpolat N, Durukan P, Seçkin, et al. (2008) Investigation of acute effects of diclofenac sodium on rat kidney with unilateral ureteral obstruction. Turk J Emerg Med 8: 103-109.
-
Fuchs-Buder T, Meistelman C, Raft J (2013) Sugammadex: clinical development and practical use. Korean J Anesthesiol 65: 495-500.
-
Baldo B (2012) Sugammadex and rocuronium-induced anaphylaxis. Anaesthesia 67: 1174-1175.
-
Raft J, Betala Belinga JF, Jurkolow G, Desandes E, Longrois D, et al. (2011) [Clinical evaluation of post-surgical bleeding after a sugammadex injection]. Ann Fr Anesth Reanim 30: 714-717.
-
Arslan M, Comu FM, Kip G, Alkan M, Kiraz HA, et al. (2014) Effect of dexmedetomidin on erythrocyte deformability during ischemia reperfusion injury of heart in diabetic rats. Bratisl Lek Listy 115: 494-497.
-
Singh M, Shin S (2009) Changes in erythrocyte aggregation and deformability in diabetes mellitus: a brief review. Indian J Exp Biol 47: 7-15.
-
Di Minno G, Martinez J, McKean ML, De La Rosa J, Burke JF, et al. (1985) Platelet dysfunction in uremia. Multifaceted defect partially corrected by dialysis. Am J Med 79: 552-559.
-
Castillo R, Lozano T, Escolar G, Revert L, López J, et al. (1986) Defective platelet adhesion on vessel subendothelium in uremic patients. Blood 68: 337-342.
-
Livio M, Gotti E, Marchesi D, Mecca G, Remuzzi G, et al. (1982) Uraemic bleeding: role of anaemia and beneficial effect of red cell transfusions. Lancet 2: 1013-1015.
-
Malyszko J, Malyszko JS, Mysliwiec M, Buczko W (2005) Hemostasis in chronic renal failure. Rocz Akad Med Bialymst 50: 126-131.
-
Goldstein DE, Little RR, Wiedmeyer HM, England JD, McKenzie EM (1986) Glycated hemoglobin: methodologies and clinical applications. Clin Chem 32: B64-70.
-
Noris M, Remuzzi G (1999) Uremic bleeding: closing the circle after 30 years of controversies? Blood 94: 2569-2574.
-
Bull BS, Breton-Gorius J, Beutler E (1991) Morphology of erythron. In: Williams WY, Beutler E, Erslev AJ, Lichtman MA (eds). Hematology. Mc Graw Hill, NewYork, USA.
-
McCay PB (1985) Vitamin E: interactions with free radicals and ascorbate. Annu Rev Nutr 5: 323-340.
-
Rosenmund A, Binswanger U, Straub PW (1975) Oxidative injury to erythrocytes, cell rigidity, and splenic hemolysis in hemodialyzed uremic patients. Ann Intern Med 82: 460-465.
-
Stocks J, Offerman EL, Modell CB, Dormandy TL (1972) The susceptibility to autoxidation of human red cell lipids in health and disease. Br J Haematol 23: 713-724.
-
Ersoy A, Ersoy C, Dilek K, Usta M, Güllülü M, et al. (2002) The effect of different doses of vitamin C treatment on renal anemia. Uludag üniversitesi Tip Fakültesi Dergisi 28: 5-9.
-
Çomu FM, Andiç MF, Edremitlioglu M, DikmenogluN (2009) Quercetin ve Pentoksifilinin akut böbrek yetmezliginde böbrek perfüzyonu ve eritrosit deformabilitesine etkisi. Türk Fizyolojik Bilimler Dernegi 35. Ulusal Fizyoloji Kongresi, özet kitabi poster no 31: sayfa 102.
-
Bostan H, Kalkan Y, Tomak Y, Tumkaya L, Altuner D, et al. (2011) Reversal of rocuronium-induced neuromuscular block with sugammadex and resulting histopathological effects in rat kidneys. Renal Fail; 33: 1019-1024.