International Journal of Anesthetics and Anesthesiology
Cost - Benefit Analysis of Focused Pre-Operative Transthoracic Echocardiography in the Pre-Operative Clinic in Patients at Increased Cardiac Risk Presenting for Non-Cardiac Surgery - A Pilot Study
David Neale1, Daryl Williams2 and David Canty1-3*
1Department of Anaesthesia and Perioperative Medicine, Monash Medical Centre, Australia
2Department of Anaesthesia and Pain Management, Royal Melbourne Hospital, Australia
3Department of Surgery, University of Melbourne, Australia
*Corresponding author: David Canty, Department of Surgery, The University of Melboune, Victoia 3010, Australia, Tel: +61-3-9035-8118, Fax: +61-3-8679-3353, E-mail: dcanty@unimelb.edu.au
Int J Anesthetic Anesthesiol, IJAA-1-023, (Volume 2, Issue 1), Original Research Article; ISSN: 2377-4630
Received: January 24, 2015 | Accepted: March 11, 2015 | Published: March 13, 2015
Citation: Neale D, Williams D, Canty D (2015) Cost - Benefit Analysis of Focused Pre-Operative Transthoracic Echocardiography in the Pre-Operative Clinic in Patients at Increased Cardiac Risk Presenting for Non-Cardiac Surgery - A Pilot Study. Int J Anesthetic Anesthesiol 2:023. 10.23937/2377-4630/2/1/1023
Copyright: © 2015 Neale D, et al. This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited.
Abstract
Background and aims: In a prospective observational study, focused transthoracic echocardiography (TTE) performed in the preoperative clinic on 100 patients with increased cardiac risk resulted in a change in management of 54% and a net reduction in use of hospital resources. The aims of this study are to apply a cost benefit analysis to demonstrate whether or not this translated into saving money for the hospital.
Methods: Data from a previous study examining management changes resulting from preoperative focused TTE were collated. Cost estimates were obtained for management changes, and total costs and savings were calculated.
Results: The use of focused TTE in the perioperative period may have saved a total of $AUD 22,772.32 or $AUD 227 for each patient (n=100). Based on the performance of two focused TTE examinations each day in the preoperative clinic, a potential saving of greater than $AUD 100,000 per year is estimated.
Conclusion: This pilot study demonstrates proof of concept that focused transthoracic echocardiography performed before elective non-cardiac surgery may be more cost-effective than conventional comprehensive transthoracic echocardiography.
Introduction
The use of focused transthoracic echocardiography (TTE) in the perioperative period to guide patient management is increasing due to increases in the availability of portable ultrasound devices with improved imaging capability and an expanding number of anaesthetists and perioperative physicians skilled in their use [1]. Whilst conventional (comprehensive) TTE performed by an echocardiography laboratory remains a useful diagnostic tool, its limited availability and cost restricts its use. However the major disincentive for requesting a preoperative comprehensive TTE is the time taken for the study to be performed and reported, which may lead to a delay in surgery [2], which is inconvenient for the patient and could lead to deterioration of medical or surgical disease. A focused TTE, recently endorsed and reviewed by the American Society of Echocardiography [3], utilises the same echocardiography techniques as conventional TTE but is performed as a bedside test by the treating doctor to answer a clinical question to aid clinical decision-making in real time. There is no need to wait for a third party to perform and report the echo examination. Focused TTE is entirely focused on categorising the haemodynamic state and distinguishing between significant from and non-haemodynamically significant valve and chamber pathologies. It provides specific information relevant to perioperative care in time for surgery.
Preoperative focused TTE has been demonstrated to significantly change the perioperative management in patients presenting for surgery [4-6] and has recently been included in consensus guidelines for cardiovascular assessment and management of patients before non-cardiac surgery [7]. In 2012 Canty et al. reported a change in management of 54% of 100 patients referred for assessment by an anaesthetist in the preoperative clinic prior to surgery, who received a preoperative focused TTE from an independent anaesthetist trained in TTE [5]. The TTE findings triaged patients to those with significant cardiac pathology leading to a step-up in care (in 20% of patients), and those without, leading to a step-down in care (34%). Management was also altered in asymptomatic patients aged over 65 years (step-up in 10%, step-down in 15%). An overall reduction in hospital resource use (cardiology referral, invasive monitoring and intensive care) and improved efficiency (less delays and hospital visits) resulted, however this has not been subjected to cost benefit analysis.
A cost-benefit has been reported with the use of routine intra-operative transoesophageal echocardiography (TOE) for cardiac surgery [8,9], and there is also evidence to suggest a cost advantage for focused TTE rather than comprehensive examination in some patients referred to cardiologists [2,10]. However, there have been no reported studies investigating the potential cost savings associated with performance of focused TTE in the pre-operative clinic. The aims of this study were to quantify the costs of performing focused TTE in the pre-operative clinic of a major tertiary referral centre, as well as to identify potential cost savings to patient care, based on data from the report of Canty et al. [5].
Methods
Patient-based data from previous research was used to conduct this project, thus ethics approval and consent was not required. In this retrospective post-hoc analysis of the study reported by Canty [5], the costs and savings for performance of anaesthetist-performed focused TTE were estimated in Australian dollars ($AUD). Indications for TTE included signs and symptoms indicating possible cardiac disease [5]. Figure 1 summarises the management changes in 100 patients who received a focused TTE in the preoperative clinic. As a reference group, patients were also included with no suspicion of cardiac disease other than age greater than 65 years.
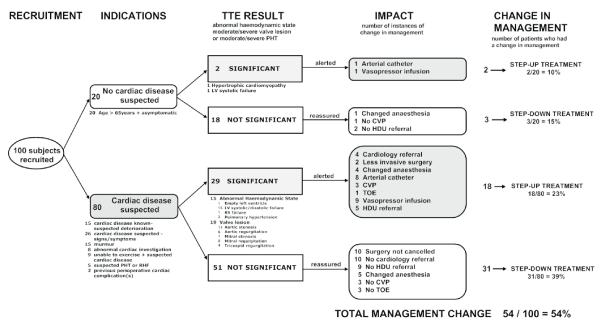
Summary of management changes following focused transthoracic echocardiography (Reproduced with permission from Wiley) from Canty DJ et al. [5].
CVP: Central venous pressure monitoring, HDU: High Dependency Unit, PHT: Pulmonary Hypertension, RHF: Right Heart Failure, TOE: Transoesophageal
Echocardiography
View Figure 1
Focused TTE was conducted on all patients in the supine position following the iHEART scan protocol (Haemodynamic Echocardiography Assessment in Real Time [11]), a focused study designed to diagnose haemodynamically significant ventricular and valve disease and abnormal haemodynamic state. The protocol includes 2-D and colour flow Doppler but not spectral Doppler and uses the parasternal, apical and subcostal windows. The echocardiography protocol is designed to be performed in less than ten minutes. Significant cardiac abnormalities were defined as those that could result in haemodynamic instability from anaesthesia or surgery. This included one or more of the following: an abnormal haemodynamic state (hypovolaemia, vasodilation, LV systolic and/or diastolic failure, RV failure as defined by Royse [12]), valve stenosis or regurgitation of at least moderate severity according to recognised guidelines [13,14], and a pericardial effusion greater than 0.5cm.
The cost of performing individual transthoracic echocardiograms was based on an industry quote for a new Sonosite� M-turbo ultrasound machine (Sonosite, Bothwell WA, USA), including a probe suitable for conducting transthoracic echocardiography, as well as consumables related to performance of TTE. Cost assumed a ten-year lifespan of the ultrasound machine with no resale value following this. Provision was also made for annual servicing of the machine at the industry accepted rate of 10% of the purchase price per year, as well as a replacement probe. An estimate of transthoracic echocardiograms performed annually was calculated based on the conduction of two examinations per day in the pre-operative clinic.
Costs of preoperative referral for cardiology assessment postoperative care in the high dependency unit (HDU) were based on state government costing, with annual indexation applied for cost increase of data from prior to 2013 [15,16]. Where HDU referral was made as a management change, the cost of a single night was attributed. The costs of performing preoperative comprehensive TTE by the echocardiography laboratory and intraoperative TOE by an anaesthetist were based on the current Australian Medicare Benefits Schedule. The cost of a comprehensive TTE includes the cost of the performance of the examination and preliminary report by the sonographer and review by a cardiologist. Costs of all other components (including medications, intravascular devices, sterile equipment and transducers) were sourced from hospital departments responsible for their purchase and supply.
Where �vasopressor infusion� was instituted as a management change, cost was based on the use of metaraminol, due to it being the most commonly used vasopressor at the institution in which the study was conducted, as well as its ability to be used in the absence of central venous access (a separate management change).
For the management change of �surgery not cancelled�, each case was assumed as one third of a session (allowing three procedures per half day session), with the cost of a single operating theatre session obtained from the hospital finance department. Each case not cancelled was deemed a saving in theatre time.
Management changes of �changed anaesthesia� and �less invasive surgery� were excluded from cost calculations due to the inability to quantify costs or savings attributable to these management changes.
The cost associated with training staff was not included in this study, as at present training is funded by individuals and not the hospital. Additionally, the time cost of performing focused transthoracic echocardiography was not included, as it is designed to be performed in less than ten minutes and hence have minimal impact on patient flow through pre-admission clinic. In the study, the anaesthetist was temporarily relieved from their anaesthesia duties by available extra staff to allow them the flexibility to perform the focused TTE when required
The savings to the hospital of reversing the decision to cancel surgery in 10 patients was difficult to determine due to the possibility of finding a replacement patient. Cancellation of surgery would normally result in referral for further investigations and review. A conservative savings of one follow-up preoperative clinic attendance with the anaesthetist was used per patient that had the decision to cancel surgery reversed due to the focused TTE.
Once individual costs had been quantified, the net total costs and savings according to Figure 1 were calculated. Finally, a total cost saving per patient undergoing pre-operative TTE was obtained by dividing the total saved by the number of patients.
Results
The patient characteristics and type of scheduled surgery are listed in table 1. The indications for preoperative focused TTE are listed in table 2. Net results of management changes due to conduction of focused TTE are listed in table 3 and the resulting cost-benefit analysis is shown in table 4.
![]()
Table 1: Patient characteristics and surgical data of 100 patients who received a focused transthoracic echocardiogram in the preoperative clinic
View Table 1
![]()
Table 2: Indications for preoperative focused TTE in 100 patients who received focused transthoracic echocardiography in the preoperative clinic.
View Table 2
![]()
Table 3: Net management changes due to focused transthoracic echocardiography performed on 100 patients in the preoperative clinic [6]
View Table 3
![]()
Table 4: Cost benefit analysis of focused transthoracic echocardiography performed on 100 patients attending the preoperative clinic.
View Table 4
Of the 100 patients who received a focused TTE, 80 patients were suspected of having cardiac disease and in 67 of these patients, the anaesthetist stated that they would have ordered a comprehensive TTE had the patient not been included in the study. Thus in 67 patients the decision to order comprehensive TTE was reversed, as a focused TTE was performed instead, which was reported as savings of the cost of performing 67 comprehensive TTE examinations.
Total ultrasound expenses are based on an industry quote of $37,000 for the ultrasound unit, yearly servicing of $3,700, replacement of a probe ($5,000) and consumables. Calculations for arterial and central venous catheter insertion and monitoring include the cost of catheters, transducers and sterile equipment used for their insertion.
Table 3 indicates the estimated total costs and savings calculated when the data from table 2 is applied to the patient data in figure one. The overall cost saving for the 100 patients studied was $22,772.32, which equates to a cost saving of $227.72 for each of the one hundred patients.
In the original study by Canty et al., the treatment plan of the anaesthetist caring for the patient on the day of surgery was identical to the plan made in pre-operative clinic in 83 out of 91 patients [5]. In the remaining eight patients there were eight fewer arterial and four fewer central venous catheters inserted, and three fewer referrals for postoperative HDU. Based on the costs above, this equates to a total saving of $3,438.75. Of these 83 cases, there was therefore an additional savings of $41.43 per patient.
Discussion
This study demonstrates that, as well as influencing anaesthetic management of patients, focused TTE performed in the pre-admission clinic has clear financial benefits. Although the exact number of eligible patients presenting to each clinic is unknown, the conservative estimate of two TTE examinations per day would lead to an annual saving of greater than $100,000, and potentially greater savings with performance of a higher number of focused TTE examinations. Whilst the results reflect savings at a single institution, they could be readily applied to many large tertiary hospitals. In addition to the financial benefits of implementing such a program to the pre-operative clinic, the low annual capital cost, minimal time impact and lack of patient morbidity make focused TTE a useful addition. Delays to surgery may also be avoided, leading to further cost savings [17]. There may also be reduced burden placed upon cardiology outpatient services, particularly comprehensive TTE services.
The retrospective nature of this study that lacks a control arm represent important limitations of this study and any conclusions made need to be made with caution. However this pilot study provides proof of concept that focused transthoracic echocardiography may be more cost-effective than the current standard of care using comprehensive TTE, which supports further prospective investigation. Other limitations include inherent variability of some costs, particularly of non-tangible items such as the cost of an HDU bed or cardiology referral. There is also a recognised difference between the cost of items to the hospital and their actual cost [18]. The inability to quantify costs of �less invasive surgery� or �change of anaesthesia� may also lead to inaccuracies of total cost or savings. The proportion of patients referred to cardiology who subsequently underwent a comprehensive TTE was also unable to be quantified. Having such information may have further clarified potential cost savings. The number of nights spent by patients in HDU would also influence total cost savings, as all cases in this study were assumed as single night stays.
The cost of a last minute cancellation (the day before surgery) is difficult to estimate and depends on whether or not another patient can be substituted on the operating list. If this is possible then there is not much in terms of direct costs other than another extra preoperative clinic appointment or follow-up consultation ($150 per hour for an anaesthetist). However the indirect costs to the patient who has had their surgery cancelled are substantial, especially if annual leave has been taken from work. If the operating time cannot be utilised then one minute of operating time is estimated at $100 per minute inclusive of fixed and variable costs (this includes anaesthetic and surgical wages) [19]. A more conservative cost of $80 per minute may be used if the anaesthetic and surgical wages are not included. For an operative time (including operating theatre preparation, anaesthesia, surgery) of 90 minutes this would equate with $7,200. In our analysis we made the assumption that a replacement patient was not found resulting in �loss� of one third of an operating theatre session time, assuming that on average three procedures are performed per half day operating session. Our finance department calculated this at $3,330. This therefore represents a conservative cost saving. However as there were 10 patients who had the decision to cancel their surgery reversed, this would represent the principal proportion of the overall savings ($33,300 for 10 patients) and result in an overall savings of $550 per patient, and $270,000 per year. It is likely that the savings from prevention of last minute cancellation of surgery varies between hospitals and funding arrangements. However if this savings is removed from the analysis, then the savings due to focused preoperative TTE is still $212.72 per patient with an estimated annual saving of over $100,000.
As mentioned, the cost of training anaesthetists to perform focused TTE is at present borne by individuals rather than institutions, and it is acknowledged that a lack of suitably qualified practitioners in the pre-admission clinic may limit implementation of a TTE program. Funding of training in focused TTE by institutions may increase the availability of qualified practitioners, but would have significant impact on overall cost required to implement such a program.
Possible future areas of research following this study may include the use of patient outcomes data to further quantify potential costs and savings to hospitals. Including costs associated with patient outcomes such as prolonged recovery stay, prolonged inpatient stay and perioperative cardiac events may lead to an even greater saving, given the substantial costs associated with major intra-operative and post-operative morbidity which may potentially be averted. This may be analysed with clinically validated decision-tree software such as TreeAge� (TreeAge Software Inc.,Williamstown, MA, USA). An example is published by Auguste et al. [20].
Although the results of this study do not show direct benefit to patient outcome, the significant cost saving is suggestive of less patient morbidity. In a retrospective study, Canty et al. demonstrated an associated reduction in mortality after hip fracture surgery in patients who received a preoperative TTE, which remains to be proven in a prospective study [21]. Hence further areas of study may also extend to cost benefit analysis for patients undergoing focused TTE outside the pre-admission clinic, such as those presenting for non-elective surgery.
Conclusion
This pilot study demonstrates proof of concept that focused transthoracic echocardiography performed before elective non-cardiac surgery may be more cost-effective than conventional comprehensive transthoracic echocardiography.
Acknowledgments
We thank Prof Tom Marwick (Menzies Research Institute, Tasmania) and Colin Royse (Department of Surgery, University of Melbourne) for supervision. We also thank Mr Allan Manser (Pharmacy, Monash Medical Centre), perioperative nursing staff (Monash Medical Centre), and staff from the department of finance from Monash Medical Centre and Royal Melbourne Hospital for assistance with cost determination.
References
-
Royse CF, Canty DJ, Faris J, Haji DL, Veltman M, et al. (2012) Core review: physician-performed ultrasound: the time has come for routine use in acute care medicine. Anesth Analg 115: 1007-1028.
-
Badano LP, Nucifora G, Stacul S, Gianfagna P, Pericoli M, et al. (2009) Improved workflow, sonographer productivity, and cost-effectiveness of echocardiographic service for inpatients by using miniaturized systems. Eur J Echocardiogr 10: 537-542.
-
Spencer KT, Kimura BJ, Korcarz CE, Pellikka PA, Rahko PS, et al. (2013) Focused cardiac ultrasound: recommendations from the American Society of Echocardiography. J Am Soc Echocardiogr 26: 567-581.
-
Canty DJ, Royse CF (2009) Audit of anaesthetist-performed echocardiography on perioperative management decisions for non-cardiac surgery. Br J Anaesth 103: 352-358.
-
Canty DJ, Royse CF, Kilpatrick D, Bowman L, Royse AG (2012) The impact of focused transthoracic echocardiography in the pre-operative clinic. Anaesthesia 67: 618-625.
-
Canty DJ, Royse CF, Kilpatrick D, Williams DL, Royse AG (2012) The impact of pre-operative focused transthoracic echocardiography in emergency non-cardiac surgery patients with known or risk of cardiac disease. Anaesthesia 67: 714-720.
-
Kristensen SD, Knuuti J, Saraste A, Anker S, Botker HE, et al. (2014) 2014 ESC/ESA Guidelines on non-cardiac surgery: cardiovascular assessment and management: The Joint Task Force on non-cardiac surgery: cardiovascular assessment and management of the European Society of Cardiology (ESC) and the European Society of Anaesthesiology (ESA). Eur Heart J 35: 2383-2431.
-
Bettex DA, Pretre R, Jenni R, Schmid ER (2005) Cost-effectiveness of routine intraoperative transesophageal echocardiography in pediatric cardiac surgery: a 10-year experience. Anesth Analg. 100: 1271-1275.
-
Fanshawe M, Ellis C, Habib S, Konstadt SN, Reich DL (2002) A retrospective analysis of the costs and benefits related to alterations in cardiac surgery from routine intraoperative transesophageal echocardiography. Anesth Analg 95: 824-827.
-
Kimura BJ, Blanchard DG, Willis CL, DeMaria AN (2002) Limited cardiac ultrasound examination for cost-effective echocardiographic referral. J Am Soc Echocardiogr 15: 640-646.
-
Faris JG, Veltman MG, Royse CF (2009) Limited transthoracic echocardiography assessment in anaesthesia and critical care. Best Pract Res Clin Anaesthesiol 23: 285-298.
-
Royse CF (2009) Ultrasound-guided haemodynamic state assessment. Best Pract Res Clin Anaesthesiol 23: 273-283.
-
Baumgartner H, Hung J, Bermejo J, Chambers JB, Evangelista A, et al. (2009) Echocardiographic assessment of valve stenosis: EAE/ASE recommendations for clinical practice. J Am Soc Echocardiogr 22: 1-23.
-
Zoghbi WA, Enriquez-Sarano M, Foster E, Grayburn PA, Kraft CD, et al. (2003) Recommendations for evaluation of the severity of native valvular regurgitation with two-dimensional and Doppler echocardiography. See comment in PubMed Commons below J Am Soc Echocardiogr 16: 777-802.
-
Victorian Government DoH (2013) Fees and Charges for Acute Health Services in Victoria. Available from: http://health.vic.gov.au/feesman/fees6.htm
-
Health NSWMo (2011) Cost of Care Standards 2009-10
-
Ferschl MB, Tung A, Sweitzer B, Huo D, Glick DB (2005) Preoperative clinic visits reduce operating room cancellations and delays. Anesthesiology 103: 855-859.
-
Marwick TH (2005) Can we justify the cost of echocardiography? Lessons from outcomes research. Eur J Echocardiogr 6: 155-163.
-
Macario A (2010) What does one minute of operating room time cost? J Clin Anesth 22: 233-236.
-
Auguste P, Barton P, Hyde C, Roberts TE (2011) An economic evaluation of positron emission tomography (PET) and positron emission tomography/computed tomography (PET/CT) for the diagnosis of breast cancer recurrence. Health Technol Assess 15: iii-iv, 1-54.
-
Canty DJ, Royse CF, Kilpatrick D, Bowyer A, Royse AG (2012) The impact on cardiac diagnosis and mortality of focused transthoracic echocardiography in hip fracture surgery patients with increased risk of cardiac disease: a retrospective cohort study. Anaesthesia. 67: 1202-1209.x





