International Journal of Anesthetics and Anesthesiology
Allergy to General Anesthetics: Evaluation of Patients Profile
Carla Irani*, C. Saade, C. Dagher and P. Yazbeck
Hotel Dieu de France hospital, St Joseph University, Beirut, Lebanon.
*Corresponding author: Carla Irani, Internal Medicine Allergy, Hotel Dieu de France hospital, St Joseph University, Beirut, Lebanon, Tel: 9613495496; E-mail: iranica@yahoo.com
Int J Anesthetic Anesthesiol, IJAA-1-013, (Volume 1, Issue 3), Original Article; ISSN: 2377-4630
Received: September 01, 2014 | Accepted: October 28, 2014 | Published: November 02, 2014
Citation: Irani C, Saade C, Dagher C, Yazbeck P (2014) Allergy to General Anesthetics: Evaluation of Patients Profile. Int J Anesthetic Anesthesiol 1:013. 10.23937/2377-4630/1/3/1013
Copyright: © 2014 Irani C, et al. This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited.
Introduction
8 millions procedures requiring anesthesia are performed yearly in France with 75% of them being general anesthesia. In 45% of those procedures, a NMBA (neuromuscular blocking agents) is used [1]. The incidence of allergy to general anesthetics ranges between 1/20000 in Australia and 1/350 in Great-Britain [2,3]. The incidence of peranesthestic allergic reactions estimated in 1996 in France was 1/9000, all drugs confounded and the incidence of allergic reactions to NMBA was evaluated to be 1/6500 anesthesia. Allergic reactions can be benign or fatal in some cases (6%), presenting with urticaria /angioedema or systemic manifestations (dyspnea, bronchospam) and a severe anaphylactic shock [4] requiring a cardiopulmonary resuscitation and the administration of adrenaline [5]. Thus, it is important to prevent this IgE mediated allergy [6-8] by recognizing the profile of patients at risk. Although many studies have identified the profile of patients allergic to drugs [9], very few studied the particularity of general anesthetics. Our study evaluates the prevalence of sensitization to general anesthetics in our institution. It determines as well the profile of patients sensitized to general anesthetics.
Methods
This is a retrospective observational study conducted between January and December 2009.
Inclusion criteria are as following
1. Patients referred from the department of anesthesiology to our clinic for evaluation, because of positive history of allergy such as: allergic rhinitis, asthma, and food or drug allergy
2. Prior history (greater than 6 weeks ago) of per-operative allergic reaction
Exclusion criteria were
1. Patients with antihistaminics, benzodiazepines, tricyclics antidepressors and vasoconstrictors intake within one week
2. Pregnant women
3. Very poor skin condition
1176 patients were included in order to determine the prevalence of sensitization to general anesthetics. Then, 2 groups of patients were designed to compare their characteristics: the group of patients sensitized to general anesthetics and the group of patients sensitized to other drugs.
A prick test was performed in all patients referred to our clinic by the anesthesiology department in Hotel Dieu de France whenever an allergy to general anesthetics was suspected. The protocol used for the prick test is the following: the positive control is the histamine and the negative control would be a physiological saline. The cut-off is a diameter of 3mm. We tested the following drugs with the consecutive dilutions by a prick test: Meperidine (10mg/ml), morphine (10mg/ ml), tramadol (50mg/ml), alfentanil (0.5mg/ml), sufentanil (0.005mg/ ml), fentanyl (0.05mg/ml), ketamine (10mg/ml), propofol (10mg/ ml), etomidate (2mg/ml), midazolam (5mg/ml), thiopental (25mg/ ml), vecuronium (4mg/ml), rocuronium (10mg/ml), atracurium (10mg/ml), cisatracurium (2mg/ml), succinylcholine (50mg/ml), xylocaine (10mg/ml), bupivacaine (2.5mg/ml).
The diagnosis of other drug allergies such as antibiotics was based upon the clinical symptoms as described by the patient. A positive dosage of the IgE specific to antibiotics was also used to confirm the diagnosis. However, a negative result didn't eliminate the diagnosis knowing the low sensibility of the IgE.
The data analysis as well as the graphic representations was performed by using Excel software. Proportions and percentages for both groups and means were used for the descriptive analysis. The comparative analysis was done with the Chi2 test used for personal history of allergy and gender, and the z-test for the age factor.
Results
Descriptive analysis
17 patients of 1176 (1,44%) were diagnosed as sensitized to general anesthetics (Table 1). The mean age and the standard deviation were 46.4 ± 7.4 (α=5%). Among the 17 patients sensitized to general anesthetics, 12 were female (70,6%). The proportion of patients with a positive history of allergy was70,6% (12/17). On the other side, the number of patients with a drug allergy is 9/17 (52,9%). 6/9 has an allergy to penicillin, 4/9 has an allergy to NSAIDs and 2/9 were allergic to sulfa drugs.
![]()
Table 1: Number of patients diagnosed as sensitized to general anesthetics
View Table 1
Among the patients sensitized to general anesthetics, 16 of 17 (94,1%) of patients had a direct mast cell degranulation with histamine release with morphine and mepiridine, but the diameter of wheal and flare was less than 3mm. 3/16(18.75) had sensitization to sufentanil, 3/17(18.75) had sensitization toalfentanil and 2/17(11.76) had sensitization tofentanyl. 8/17 (47,1%) had a sensitization to NMBA, 3/17 (17,6%) was sensitized to etomidate, 3/17 (17,6%) had a sensitization to ketamine and 2 of 17 (11,8%) were sensitized to propofol (Figure 1).
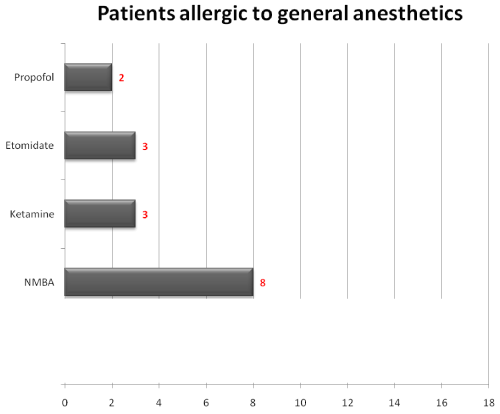
Figure 1: Patients allergic to general anesthetics
View Figure 1
Among the patients diagnosed with a sensitization to NMBA, 4/8 had a sensitisation toatracurium, 3/8 to vecuronium, 3/8 were sensitized to rocuronium and 2/8 had a sensitisation tocisatracurium (Figure 2).
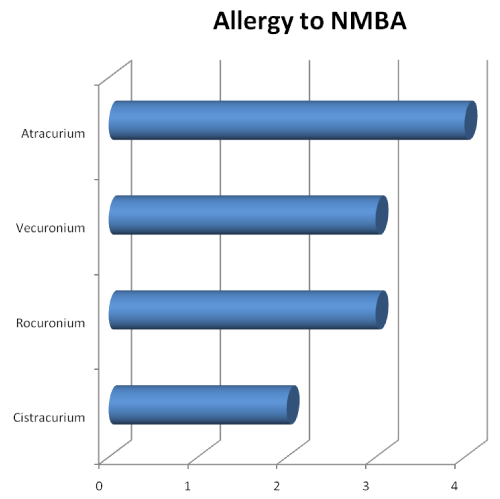
Figure 2: Allergy to NMBA
View Figure 2
The rate of cross-reactions among the patients sensitised to NMBA was evaluated as high as 37,5% in our study (3/8). 172 patients of 1176 (14,6%) were diagnosed with an allergy to other drugs. 98 were female (57%). The mean age and the standard deviation for this group of patients were 40,9 ± 2.7 (α=5%). 55,8% (96/172) had a personal history of allergy whether it was a food, cutaneous or respiratory allergy.
Comparative analysis
a. Age: The z-test was performed for this variable and the result obtained wasn't statistically significant: z= 1.38< 1.96, α=5%.
b. Personal history: 55.8% (96/172) of the patients allergic to drugs have a personal history of food, cutaneous and respiratory allergy. On the other side, 70,6% (12/17) of the patients allergic to general anesthetics had a previous history of allergy. The Chi2 test was performed with a result of 1,07, which was considered non significant (α=5%).
c. Gender : 12/17 (70,6%) of patients with an allergy to general anesthetics were female whereas 57% of patients diagnosed with a drug allergy were female.(Figure 3) The Chi2 test was performed but the result wasn't statistically significant (p=1.07,α=5%).
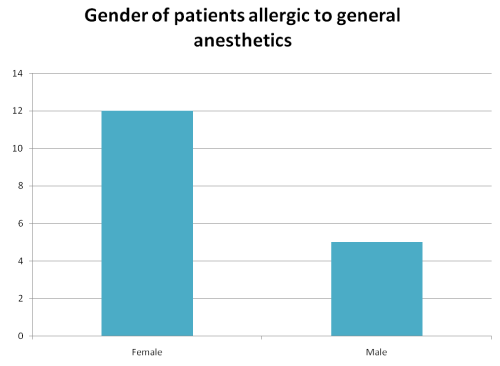
Figure 3: Gender of patients allergic to general anesthetics
View Figure 3
Discussion
The incidence of allergy to general anesthetics is rare and ranges between 1/20000 in Great-Britain and 1/350 in Australia [2,3]. Thus, few studies were designed to examine the different aspects of this kind of allergy, especially its prevalence and its risk factors.
Our study has aimed to determine the characteristics of patients having a sensitization to general anesthetics. The diagnostic workup included the clinical symptoms, the prick tests [10] the tryptase level and the specific IgE useful in the diagnosis of allergy [11,12].
In our study, the prevalence of the allergy to general anesthetics was 17/1176 (1.4%) patients seen in our clinic. The incidence of allergic reactions is usually reported in the literature instead of its prevalence.
Furthermore, the NMBA (47,1%) in particular the atracurium were the most encouteredagent in allergy, followed by vecuronium, rocuronium and finally cistracurium. 16 of 17 (94,1%) patients had a degranulation to morphine and mepiridine, but 3/16(18.75) had sensitization to sufentanil, 3/17(18.75) had sensitization to alfentanil and 2/17(11.76) had sensitization to fentanyl .There is a difference between our results and those of other studies with the exception of the results of a Spanish study in 2000 [13].
An article published in the Singapore Medical Journal in 2008 [7] mentioned that 65% of patients are actually allergic to the NMBA. This result matches the value found in other studies [2,8,14].
This is best explained by the presence of a quaternary ammonium common to all NMBA which is responsible for this kind of allergy [8].
Furthermore, this study showed [7] that 13% of patients were diagnosed as having a sensitisation to opioids. When it comes to the NMBA, the allergy to atracurium and vecuronium is the most frequent in Lebanon when compared to France [7] where rocuronium (even though less histamine releasing) and atracurium are the most frequently encountered.
The rate of cross-reactions in our study was 37.5% which is lower than the rate found in other studies (65%) [15,16]. However, this rate justifies the need to test all the NMBA when an allergy to one of them is confirmed [11]. It is important to mention that 15 to 20% of patients [17,18] in France and even more in Australia (50 à 60%) [19] who present for the first time an allergy to a NMBA ,were never exposed before to these drugs [20] making the diagnosis more difficult.
The mean age of the patients sensitized to general anesthetics is 46,4 ± 7,4, which is compatible to the fact that adult patients are more frequently affected than young patients [9]. A
A female predominance was noticed in our study with a value of 70,6%, similarly to the results in literature (70%) [3]. 70,6% had a medical history of allergy (respiratory, cutaneous or food allergy), which is considered in the literature as a risk factor to allergy to general anesthetics [11].
The comparative analysis in our study which is new of its kind showed that the group of patients allergic to general anesthetics is similar to the group of patients allergic to drugs when it comes to age, gender and personal history of allergy (cutaneous, respiratory and food allergy): in fact, being a adult women with a past history of allergy is a risk factor for the allergy to general anesthetics as well as to drugs.
Thus, when those characteristics are present, one should suspect a possible allergy to general anesthetics in the preoperative consultation.
Few other studies evaluated the implication of other factors such as pholcodine in the occurrence of the allergy to general anesthetics [21-24]. It is an analogue to morphine that has a quaternary ammonium and is used in the preparation of antitussives.
It is necessary however to perform other studies with larger samples in order to identify better the risk factors of the allergy to general anesthetics and thus prevent it.
Conclusion
The allergy to general anesthetics is uncommon and few studies evaluated the prevalence of this allergy and its risk factors.
The sensitization to NMBA is the most frequently encountered in Lebanon similar to France, Great-Britain and other countries.
The rate of cross-reactions is 37.5%; that justifies the need to test other NMBA once a patient is allergic to one of them.
Furthermore, the patients sensitized to general anesthetics have a particular profile: an adult female with a personal history of allergy. Those characteristics are useful to consider testing for anesthetics.
Other studies need to be done in order to determine the different characteristics of the patients allergic to general anesthetics. Also, it is important to agree on a common diagnostic tool with a high positive predictive value (PPV) to confirm the allergy to general anesthetics. The prick test is the best diagnostic tool available.
Combining the skin prick test and our clinical knowledge of the risk factors for the allergy to general anesthetics can improve our diagnosis skills and can help us make a proper diagnosis with an attempt to prevent peri-operative anaphylaxis due to general anesthetics.
Limitations of the Study
Our study is retrospective and focuses on the risk factors of allergy to general anesthetics. The prick skin test was done with the undiluted form of the anesthetic agent, or in other words at the same concentration as administered to the patient for anesthesia. However, some of those risk factors such as the profession weren't studied because of the lack of information in the patient's file. A larger sample of patients allergic to general anesthetics could have been more informative. However, knowing the incidence of this allergy, it is challenging to gather a larger number of patients.
References
-
Laxenaire MC (1999) Epidemiologie des reactions anaphylactoidesperanesthesiques, Quatrieme enquete multicentrique (juillet 1994-decembre 1996). Ann Fr Anesth Reanim18: 796-809.
-
McD. Deal S, Manthri PR, Gadiyar V, Wildsmith JAW (2000) Histaminoid reactions associated with rocuronium. Br J Anaesth 84: 108-111.
-
Draisci G, Nucera E, Pollastrini E, Forte E, Zanfini B, et al. (2007) Anaphylactic reactions during cesarean section. Int J Obstet Anesth16: 63–67.
-
Rance F, Abbal M, Didier A (2002) Allergies et hypersensibilités chez l'enfant et chez l'adulte : aspects epidémiologiques, diagnostiques et principes de traitement. Rev Fr Immunol Clin 42: 378-401.
-
Currie M, Kerridge RK, Bacon AK, Williamson JA (2005) Crisis management during anaesthesia: anaphylaxis and allergy. Qual Saf Health Care 14: e19.
-
Moneret-Vautrin DA, Mertes PM (2010) Anaphylaxis to general anesthetics. Chem Immunol Allergy 95: 180-189.
-
Mouton-Faivre C, Laxenaire MC, Mertes PM (2003) Realisation pratique du bilan allergologique cutané à visée anesthésique, dans le respect des recommandations pour la pratique clinique : qui tester, quoi tester, comment tester ? Revue françaised'allergologie et d'immunologieclinique 43: 281-288.
-
Mertes PM, Regnier MA, Hasdenteufel F, Guéant-Rodriguez RM, Mouton-Faivre C, et al. (2010) Controverse : la sensibilisation aux ammoniums quaternaires est impliquée dans l'allergie aux curares. Revue Françaised'Allergologie 50: 174-178.
-
Guglielmi L, GuglielmiP,Demoly P (2006) Drug Hypersensitivity: Epidemiology and Risk Factors. Curr Pharm Des 12: 3309-3312.
-
Chong YY, Caballero MR, Lukawska J, Dugué P (2008) Anaphylaxis during general anaesthesia: one-year survey from a British allergy clinic. Singapore Med J 49: 483-487.
-
Moneret-Vautrin DA (2002) Tests cutanés pour le diagnostic d'allergie aux curares. AnnalesFrançaisesd'Anesthésie et de Reanimation 21: 97-107.
-
Dewachter P, Mouton-Faivre C, Pertek JP, Boudaa C, Mertes PM (2005) Interet des tests cutanés pour le choix d'un curare après une réaction anaphylactique. Ann Fr Anesth Reanim 24: 543-546.
-
Sanchez Palacios A, Ortiz Ponce M, Rodriguez Perez A (2000) Allergic reactions and pseudoallergies in surgical interventions with general anesthesia. Allergol Immunopathol 28: 24-36.
-
Fernanda Santos Silva (2008) Severe intraoperative anaphylactic reaction: Aprotinin and Rocuronium. J Cardiothorac Vasc Anesth 22: 740-743.
-
Ebo DG, Fisher MM, Hagendorens MM, Bridts CH, Stevens WJ (2007) Anaphylaxis during anaesthesia: diagnostic approach. Allergy 62: 471-487.
-
Fisher MM, Munro I (1983) Life threatening anaphylactoid reactions to muscle relaxants. Anesth Analg 62: 559-564.
-
Mertes PM, Laxenaire MC, Alla F (2004) Anaphylactic and anaphylactoid reactions occurring during anaesthesia in France, seventh epidemiologic survey. Ann Fr Anesth Reanim 23: 1133-1143.
-
Dewachter P (2002) La prévention du risque allergique peut-elle être assurée par une médication préanesthésique ?.Ann Fr Anesth Reanim 21: 151-167.
-
Baldo BA, Fisher MM, Pham NH (2009) On the origin and specificity of antibodies to neuromuscular blocking drugs: an immunochemical perspective. Clin Exp Allergy 39: 325-344.
-
Cottenceau V, Dewachter P, Nouette-Gaulain K, Sztark F (2008) Des injections préalables de curares sans effet indésirable n'affranchissent pas du risque de choc anaphylactique. Annales Françaisesd'Anesthésieet de Réanimation 27: 509e1-509e3.
-
Florvaag E, Johansson SG, Oman H, Venemalm L, Degerbeck F, et al. (2005) Prevalence of IgE antibodies to morphine: Relation to the high and low incidences of NMBA anaphylaxis in Norway and Sweden. Acta Anaesthesiol Scand 49: 437-444.
-
Florvaag E, Johansson SG, Oman H, Harboe T, Nopp A (2006) Pholcodine stimulates a dramatic increase of IgE in IgE-sensitized individuals. Allergy 61: 49-55.
-
Harboe T, Johansson SG, Florvaag E, Oman H (2007) Pholcodine exposure raises serum IgE in patients with previous anaphylaxis to neuromuscular blocking agents. Allergy 62: 1445-1450.
-
Johansson SG, Florvaag E, Oman H, Poulsen LK, Mertes PM, et al. (2009) National pholcodine consumption and prevalence of IgE- sensitization: a multicentre study. Allergy 65: 498-502.





