International Archives of Urology and Complications
An Unusual Cause of Massive Hematuria: Arterio-Ureteral Fistula, and Review of the Literature
Andrea Orosa Andrada*, Inés Laso García, Francisco de Asís Donis Canet, José Javier Fabuel Alcáñiz, Luís López-Fando Lavalle and Francisco Javier Burgos Revilla
Department of Urology, Ramón y Cajal University Hospital, Madrid, Spain
*Corresponding author: Andrea Orosa Andrada, Department of Urology, Ramón y Cajal University Hospital, Madrid, Spain, E-mail: andreaorosa@hotmail.com
Int Arch Urol Complic, IAUC-1-010, (Volume 1, Issue 2), Case Report; ISSN: 2469-5742
Received: August 14, 2015 | Accepted: September 19, 2015 | Published: September 21, 2015
Citation: Andrada AO, García IL, Canet FAD, Alcáñiz JJF, Lavalle LLF, et al. (2015) An Unusual Cause of Massive Hematuria: Arterio-Ureteral Fistula, and Review of the Literature. Int Arch Urol Complic 1:010. 10.23937/2469-5742/1510010
Copyright: © 2015 Andrada AO, et al. This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited.
Abstract
Background: Arterio-ureteral fistula is an uncommon diagnosis with a high rate of mortality. An early diagnosis is the key for a successful treatment and should be included in the differential diagnosis of patients with unexplained hematuria. We report a clinical case and a review of the literature.
Case report: We present the case of a patient with massive hematuria with a previous urological pathology that required the placement of double J stent and vascular abdominal surgery. The delay in the diagnosis and treatment might lead to the death of the patient.
Conclusions: We review the literature and realized a few case series have been reported. Due to this scarcity there are no diagnostic protocols, which may minimize unnecessary diagnostic tests, increase the speed of diagnosis and improve the outcomes of the treatment. To decrease mortality, clinical awareness of the possibility of an arterio-ureteral fistula is essential to make an early diagnosis. A multidisciplinary approach must be carried out by urologists, vascular surgeons and radiologists.
Introduction
Arterio-ureteral fistulas occur rarely, but an early detection and treatment are essential because they are often life-threatening. We perform a bibliographic review and report a case of uretero-iliac fistula.
Case Report
83-year-old man hospitalized in the Internal Medicine Department because of a respiratory tract infection. During his stay, the patient suddenly starts with monosymptomatic gross hematuria. He had a previous urological history of ureteral stricture treated by means of a double J ureteral stent a month ago. He also had a personal history of coronary heart disease, chronic renal failure and a peripheral occlusive arterial disease, treated with an aortobiiliac bypass ten years ago. He received chronic anti-platelet therapy with clopidogrel and antithrombotic therapy with vitamin K antagonist.
Hemogram showed 8.5 g/dl of hemoglobin, and the serum creatinine was 5.26 mg/dl (baseline 3 mg/dl). Ultrasonography showed normal kidneys, without hydronephrosis, with well-placed double J stent. The bladder was completely full of clots. The cystoscopy allowed us to see a clot appearing through the left ureteral meatus.
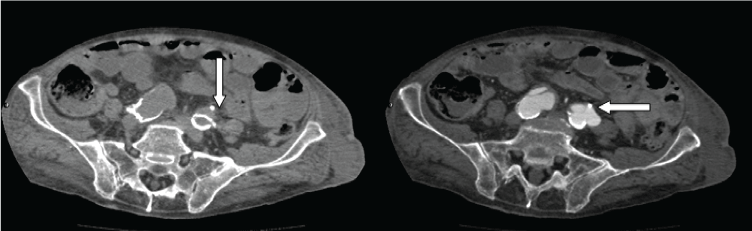
A computed tomography angiography was performed, showing an aneurysm of the left common iliac artery by the uretero-iliac crossing. The double J stent presented an extra-anatomical tract into the left iliac artery adventitia, without extravasation of contrast material (Figure 1 and Figure 2). In the presence of a suspected arterio-ureteral fistula, the patient was taken emergently to the operating room. A combined vascular and urological approach was performed. The Vascular Surgery Department performed an arterial catheterization of the common left iliac artery and left branch of the by-pass and also a catheterization of the left hypogastric artery. An Endurant 16 × 13 × 92 endoprosthesis was placed and embolization of hypogastric left artery with 10 mm-diameter coils was performed. The angiography after the procedure showed the refill of the aneurysmal sac, so Coda balloon remodelling was done, allowing a late refill of the sac in angiography. They proceeded to the occlusion of the proximal branch of the bypass and endoprosthesis, with persistence of the late refill, suggesting a IV type leakage. The cystocopy showed a massive hematuria through the left meatus.
.
Figure 1: CT angiography shows an aneurysm of the left common iliac artery and the relation with the ureter.
View Figure 1
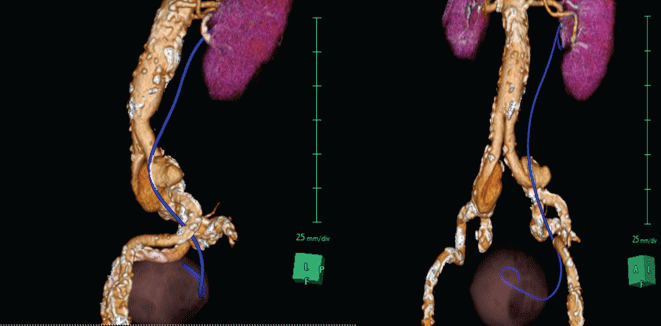
.
Figure 2: CT reconstruction shows the relation between aneurysm of the left common iliac artery and the double J stent.
View Figure 2
A more aggressive procedure was dismissed by both Departments, Urology and Vascular surgery due to the poor general situation of the patient. The necropsy was offered to the patients's family but they denied it.
Discussion
An arterio-ureteral fistula is a rare diagnosis and an unusual cause of gross hematuria. The incidence of this type of fistula is low, with only a few cases reported, so the incidence is not clearly established. In consequence of its scarcity, the diagnosis can easily be delayed, so the suspicion is very important for the determination of this condition.
Only a few cases have been reported in the literature, one of the most recent reviews is Roderick systematic review [1] in 2009. It points out the difficulty in establishing the diagnostic approach and therapeutic management.
There are many risk factors that contribute to the development of the arterio-ureteral fistula: a history of abdominal or pelvic cancer surgery, vascular abdominal surgery, urinary deviation surgery, radiotherapy or ureteral stenting [1]. Other authors have also cited infection and pregnancy as risk factors [2,3].
The pathophysiology behind the development of these fistulas is still uncertain. An arterio-ureteral fistula is the final result of an eroding inflammatory fibrotic process of a constantly pulsating artery in poor condition against a fragile ureter, resulting in necrosis [4]. There are predisposing factors like external beam radiotherapy and pelvic surgical procedures that can disrupt the vasa vasorum, leading to changes in the media and adventitia of the large arteries. For this reason the arteries are more susceptible to rupture and necrosis [5]. Furthermore, the indwelling ureteral stents have contributed to an increase in the cases of arterio-ureteral fistulas. When an ureteral stent is placed, it acts as a counter-brace, leading to alterations in ureteral elasticity by transmitting the systolic arterial wave onto the ureteral wall [3]. Ureteral stent size also plays a role in fistula development [6]. Research has shown that the larger the size of the stent, the wall compression will be higher, leading to ischemic changes [7].
The dominating symptom is gross hematuria. It can be intermittent and during periods of hematuria, the bleeding may be massive with hypotension and even shock. Sometimes the hematuria can be combined with flank or abdominal pain. A few patients had symptoms of urinary tract infection. In patients with a stent or catheter , bleeding may have been provoked or exaggerated while changing the catheter or the stent [8].
The presence of flow from the artery into the ureter (or vice versa) on diagnostic imaging proves the existence of an arterio-ureteral fistula. Ureteral contrast studies and angiography confirmed most cases, but it's necessary a flow of ≥ 3 mL/s to see the fistula in the angiography. Provocation of the blood clot during angiography or occlusion of the ureter during ureteral contrast studies could excite active bleeding and increase the accuracy of these 2 tests, but this could be dangerous and requires extensive preparation [9,10]. Negative findings do not rule out the presence of an arterio-ureteral fistula, because angiography and ureteral contrast studies confirmed only 69% and 52%, respectively, of arterio-ureteral fistulas in patients in whom these procedures were performed. Often, surgery remains essential to determine the diagnosis, even in modern practice [1]. Cystoscopy can localize the bleeding to one of the ureteral orifices. If orificial bleeding is pulsating, an arterio-ureteral fistula is likely. CT of the abdomen and pelvis is usually negative or non-specific and the bleeding is only rarely seen; however, the use of contrast increase the sensitivity of this test [8].
The treatment should be multidisciplinary between an urologist, a vascular surgeon and a radiologist. Currently, an endovascular approach should be applied when possible, but open surgery will remain necessary in some cases. Patients treated with non-invasive methods have lower mortality rate, and this could be due to the fact that most of the risk factors for arterio-ureteral fistulas also complicate open surgical treatment [11]. The reported mortality rate has decreased from 69% before 1980 to 13% in the most recent reviews [1], partly as a result of an earlier diagnosis and new surgical advances. Not all endoluminal treatments can be used in every patient. Infected vascular graft material, fistula size or aneurysms originating from a vascular anastomosis could impede the use of vascular stents [4], with the need to perform an open surgery. A non-invasive urological possible approach is to close off the ureter leaving coils. In these cases, a nephrostomy catheter should be placed. Good results have been published combining vascular stents with ureteral coils [12].
Conclusions
The arterio-ureteral fistula is a rare entity, but it can be life-threatening. This condition should be considered in patients with unexplained hematuria with risk factors associated. Studies like angiography or ureteral contrast test can diagnose the fistula, especially when active bleeding is present. The treatment requires a multidisciplinary cooperation, taking into account the endovascular approach as far as possible.
References
-
van den Bergh RC, Moll FL, de Vries JP, Lock TM (2009) Arterioureteral fistulas: unusual suspects-systematic review of 139 cases. Urology 74: 251-255.
-
Krambeck AE, DiMarco DS, Gettman MT, Segura JW (2005) Ureteroiliac artery fistula: diagnosis and treatment algorithm. Urology 66: 990-994.
-
Dervanian P, Castaigne D, Travagli JP, Chapelier A, Tabet G, et al. (1992) Arterioureteral fistula after extended resection of pelvic tumors: report of three cases and review of the literature. Ann Vasc Surg 6: 362-369.
-
van den Bergh RC, Moll FL, de Vries JP, Yeung KK, Lock TM (2008) "Arterio-ureteral fistula: 11 new cases of a wolf in sheep's clothing. J Urol 179: 578-581.
-
Puppo P, Perachino M, Ricciotti G, Zinicola N, Patrone PE (1992) Ureteroarterial fistula: a case report. J Urol 148: 863-864.
-
Finney RP (1978) Experience with new double J ureteral catheter stent. J Urol 120: 678-681.
-
Chew BH, Knudsen BE, Denstedt JD (2004) The use of stents in contemporary urology. Curr Opin Urol 14: 111-115.
-
Bergqvist D, Pärsson H, Sherif A (2001) Arterio-ureteral fistula-a systematic review. Eur J Vasc Endovasc Surg 22: 191-196.
-
Awakura Y, Yamamoto M, Fukuzawa S, Okuno H, Hashimura T, et al. (1997) A case of uretero-aortic fistula. Hinyokika Kiyo 43: 299-301.
-
Vandersteen DR, Saxon RR, Fuchs E, Keller FS, Taylor LM Jr, et al. (1997) Diagnosis and management of ureteroiliac artery fistula: value of provocative arteriography followed by common iliac artery embolization and extraanatomic arterial bypass grafting. J Urol 158: 754-758.
-
Feuer DS, Ciocca RG, Nackman GB, Siegel RL, Graham AM (1999) Endovascular management of ureteroarterial fistula. J Vasc Surg 30: 1146-1149.
-
Bilbao JI, Cosín O, Bastarrika G, Rosell D, et al. (2005) Treatment of ureteroarterial fistulae with covered vascular endoprostheses and ureteral occlusion. Cardiovasc Intervent Radiol 28: 159-163.





