International Archives of Nursing and Health Care
Using Quality Improvement Methods to Implement Guidelines to Decrease the Proportion of Urinary Retention in Orthopaedic Care
Ann-Christine Andersson1*, Rose-Marie Johansson2, Mattias Elg1,3, Boel Andersson Gäre1 and Lennart Christensson2
1Professor, The Jönköping Academy for Improvement of Health and Welfare, School of Health and Welfare, Jönköping University, and Director, Futurum, Region Jönköping County, Sweden
2Ryhov County Hospital and Qulturum, Region Jönköping County, and Department of Nursing Science, School of Health and Welfare, Jönköping University, Sweden
3Department of Management and Engineering, Linköping University, Sweden
*Corresponding author:
Ann-Christine Andersson, The Jönköping Academy for Improvement of Health and Welfare, School of Health and Welfare, Jönköping University, Hälsohögskolan i Jönköping, Box 1026, 551 11 Jönköping, Sweden, Tel: +46725241060, E-mail: Ann-Christine.Andersson@ju.se
Int Arch Nurs Health Care, IANHC-3-065, (Volume 3, Issue 1), Original Research; ISSN: 2469-5823
Received: September 01, 2016 | Accepted: March 07, 2017 | Published: March 09, 2017
Citation: Ann-Christine A, Rose-Marie J, Elg M, Gäre BA, Christensson L (2017) Using Quality Improvement Methods to Implement Guidelines to Decrease the Proportion of Urinary Retention in Orthopaedic Care. Int Arch Nurs Health Care 3:065. 10.23937/2469-5823/1510065
Copyright: © 2017 Andersson, et al. This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited.
Abstract
In patients treated with indwelling urethral catheter (IUC), complications such as catheter associated urinary tract infections are common, while underuse of IUC may cause harmful urinary retention (UR). A quality improvement (QI) program called 'Indwelling urethral catheter (IUC) - only when needed' was developed in Jönköping County Council, Sweden, aiming at creating a new approach: hospital staff should be able to identify and manage patients with risk of UR, prevent UR or treat UR without delay, and only use urinary IUCs on appropriate indications. The aim of this study was to describe the process of application of the quality improvement program. The Model for Improvement was used, and process coaches were appointed in the participating units. Their training was based on clinical issues and facts about UR, IUCs, guidelines, QI methods and measurements. Data were collected through prospective and retrospective patient record reviews, and differences were analyzed by inferential statistics.
Before the intervention, only two patients out of 296 were cared for following the guidelines perfectly. During the intervention, adherence to guidelines showed a rising trend, and reached a new stable level, with an average of 67% adherence to guidelines. A systematic improvement program supported by coaches and improvement tools can increase the adherence to new guidelines and incorporate them into local practice. This study also shows that adherence to guidelines can improve patient safety, in this case a decreased risk for and incidence of UR in an orthopaedic patient population.
Keywords
Guidelines, Indwelling urinary catheters, Model for improvement, Orthopaedic care, Quality improvement, Urinary retention
Introduction
Urinary retention (UR) is a well-known complication which can result in bladder damage and need for indwelling urethral catheter (IUC) treatment [1]. The incidence of UR varies widely between different diagnoses in orthopedic hospital care [2]. Patients treated with IUC experience an increased risk of complications such as catheter associated urinary tract infections (CAUTI), [3] iatrogenic urethral injuries, [4] and discomfort [5]. Urinary tract infections are the most common health care acquired infections and nearly 80% of these are catheter associated [6]. Over use and misuse of IUC during hospital care is commonly reported, [7] and delayed detection of UR in orthopaedic care is common [8]. Bladder damage caused by UR and/or CAUTI and/or iatrogenic urethral injuries increase the risk of morbidity and mortality, [4,9-13] prolongs hospital stays with increased costs [14-16] and decreases quality of life [17].
Preventive Urinary Retention
If patients at risk of UR are identified and examined with bladder ultrasonography and achieve an optimal voiding situation, UR can be prevented or existing UR can be treated without delay [18]. The most efficient method to prevent CAUTI is to avoid unnecessary catheterizations and to remove catheters as soon as possible [19]. Bundles of interventions focusing on strategies such as UR protocols and IUC stop reminders to reduce UR and unnecessary catheter use have been successful, particularly when coupled with implementation strategies to address common barriers [20].
The Quality Improvement Program
At the beginning of this study no general guidelines for minimizing UR and IUC existed for patients during hospital care. A quality improvement (QI) program called 'Indwelling urethral catheter (IUC) - only when needed' was developed in cooperation between researchers, an expert group [18] in the Region Jönköping County (RJC). The aim of the QI program was to implement a new and different work approach, which meant that hospital staff should identify and manage patients with risk of UR, prevent UR or treat UR without delay, and use urinary catheters with appropriate indications by using guidelines. The QI program was introduced between 2008 and 2012 and included all adult patients admitted to hospital care in the RJC. The guidelines consisted of five sections specifying risk factors of urinary retention, described in Johansson, et al. [18]. The aim of this study was to describe the process of implementing the program, to evaluate if a systematic quality improvement program increased the adherence to guidelines, and to examine the effects of implementing the program on the presence of UR.
Methods
Study setting
This study was conducted to develop the process of UIC in orthopaedic care and involved patients and professionals at the emergency unit, the operating theatre, the postoperative care unit and an orthopaedic ward, in one hospital in the RJC in Sweden. The orthopaedic clinic provides both acute and elective services. Bladder damage caused by UR and both overuse and misuse of IUC had been identified as severe quality issues. In a former study we described the routines given to patients with hip fractures and it was found that nurses seldom adhere to recommended actions and UR was found in 18 of 48 (38%) patients [21].
The quality improvement program
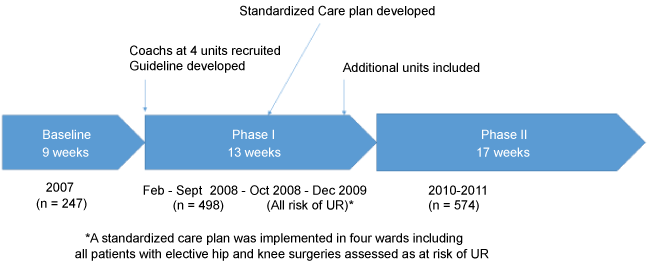
The QI program was performed in three phases: baseline, Phase I and Phase II (Figure 1). Baseline measures were performed during a nine-week period before the QI program started. Phase I was on going for a 13-week period and Phase II over a 17-week period.
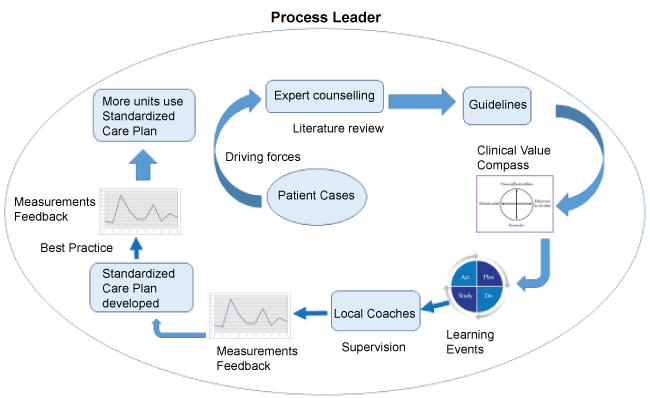
As a theoretical framework for the QI program, the Model for Improvement was used [22]. This model provided a 'trial-and-learning approach' and a frame for which knowledge and program components were needed. The developed QI program consisted of eight components and started off in real patient cases/stories serving as a driving force to start improvement [23,24]. A process leader guided the QI program. For staff to know what to do, when and by whom, guidelines for preventing and handling UR and urinary catheter treatment were developed by an expert group, based on a literature review and expert consensus published locally and in scientific journals [18]. The participating units used the Value Compass [25] and learning events using the plan-do-study-act (PDSA) cycles were conducted. Local coaches guided and supervised the staff at the units, [26] and measurements and feedback were provided. The QI programme developed a standardized care plan. The consequent use of the care plan together with the guidelines was considered goal fulfilment when measuring (Figure 2). A long version of the guidelines was published on the hospital's intranet and a short pocket version was prepared, for easy use in clinical work.
Two coaches, one registered nurse and one assistant nurse, were elected in each of the four involved units and they had time allocated to contribute to the QI program. The coaches' learning was provided in groups and consisted of three learning events over a six-month period. To increase the prerequisites to identify barriers and local problems arising at each unit the coaches learned and constructed a cause and effect ('fishbone') diagram [22]. The training was based on patient cases and local issues and included facts about UR, urinary catheters, the guidelines, PDSA and measurements. To support coaches' continouous learning, learning events were offered to all coaches for two hours, every six months. The learning events included collaboration between coaches and training in process and result analysis. Physicians, registered nurses and assistant nurses were offered learning events performed by the coaches and the process leader. At regular meetings in the units the new guidelines, working procedures and results were discussed with the unit staff.
When the programme was implemented the staff registered the number of performed bladder ultrasonography procedures and the number of residual urine measures. In order to evaluate guideline adherence the coaches reviewed a sample of ten patient records every month, selected by systematic consecutive sampling [27]. The records for the first ten patents that met the eligibility criteria were reviewed. This data were presented as run charts on each unit's whiteboard and was published on the hospital intranet. The staff had fulfilled the goals when 80% of the subsequent measurements were in accordance with the guidelines. In order to make the run charts more understandable and to visualise when the goals were fulfilled, a system with 6 'stars' (one star for each subsequent measurement) was introduced. Regularly, the staff received feedback on guideline adherence from the coaches and every other month by the process leader. In order to sustain guideline adherence and continued improvement, the coaches reviewed ten patient records six months after the units had fulfilled the goals, selected by the same systematic consecutive sampling procedure [27]. If the concordance with guidelines still was 80% or more, a new review was performed every six months. If the result was below 80%, the staff had to reflect and plan how to improve adherence to fulfil the 'stars' goal.
In this study one of the researchers (RMJ) was both process leader and researcher. The process leader task was to coach the coaches to improve the care, educate and facilitate coordination and practical issues. The researcher role was to collect and analyse data together with the research group, and give feedback, working together with the coaches, staff and leaders to identify causes for variation in the data and instigate ideas for improvement.
Data Collection
Data were collected through prospective and retrospective patient record review by RMJ. The manual patient record reviews were performed according to a protocol. To be included in the study the patients had to be 18 years or older; admitted to the orthopaedic ward during the selected weeks; assessed as having risk of UR or UR and/or treatment with IUC. Baseline data including age, sex and actual diseases/surgery were collected before the intervention. To study the impact of the interventions we identified the proportion of patients who had a 'perfect care' as process measure, and the proportion of patients with UR as an outcome measures. 'Perfect care' was defined as the staff having identified the risk of UR, performed bladder ultrasonography, handled and documented UR and urinary catheters as prescribed in the guidelines, in all four wards. In this study, urinary retention was defined as occurring when a patient is unable to pass urine and post-void residual urine is more than 400 ml and at risk of UR when post-void urine is more than 200 ml [18]. The intervention was started in March 2008 and prospective patient data were included every five weeks starting in April 2008 to May 2012 (except the weeks in June-August and the last two weeks of December and the first two weeks of January).
Analysis
Difference in group characteristics is presented as means, standard deviations and percentage. Time series data was analysed using statistical process control techniques in order to detect significant changes over time. In particular, p-charts were used, which show fractions of non-conforming data, i.e., improvement related to the interventions. Control limits in the control charts were set at 3 sigma. Statistical Process Control (SPC) methods were applied for continuous data analysis [28]. SPC supports separating signal from noise that is distinguishing common-cause and special-cause variation.
Results
In the intervention Phase I, the guidelines were distributed and three learning events were held for coaches between February and September 2008. Thereafter the coaches were offered continued learning events every six months. The process leader supervised the coaches in using the PDSA model between the continued learning events until the ward had six subsequent measurements which adhered to the guideline in 80% of patients or more. In October 2008, a delegation with a general ordination to treat patients with elective hip and knee surgeries with IUC was given to the nurses. The general ordination content instruction was to insert IUC at the operating theatre and end it at the postoperative care ward. This short-term IUC aimed at preventing UR during surgery. Statistical sampling was started on the four wards during the period 2008-2009 and was ended when each unit fulfilled the goal in the patient record review. A model of 'Standard care plans' about UR and IUC for each patient was developed in 2009. The national 'Safe Delivery' campaign was started in October 2008. One of the researchers (RMJ) gave feedback on results from the research record review and described patient cases when she met coaches at learning events, staff at meetings at each unit, and to specific physicians meeting once in 2008 and once in 2009. Adherence to guidelines in the intervention Phase I showed a rising adherence trend, but it was still an instable process during the period even if systematic improvements took place.
Intervention Phase II: The learning events continued, coaches were leaving and new coaches were educated during the period. The coaches started reviewing ten patient records every month between 2009 and 2011. The orthopaedic ward started in 2009 and fulfilled the goal with six subsequent measurements following the guidelines with 80% or more in February 2011. The postoperative care unit started in 2011 and ended in April 2012. The emergency unit started in 2010 and the operating theatre in 2011, and did not fulfil their goal until after the study period in 2013. There was sustained improvement, with an average 67% adherence according the guidelines at a new, stable level (Figure 3).
.
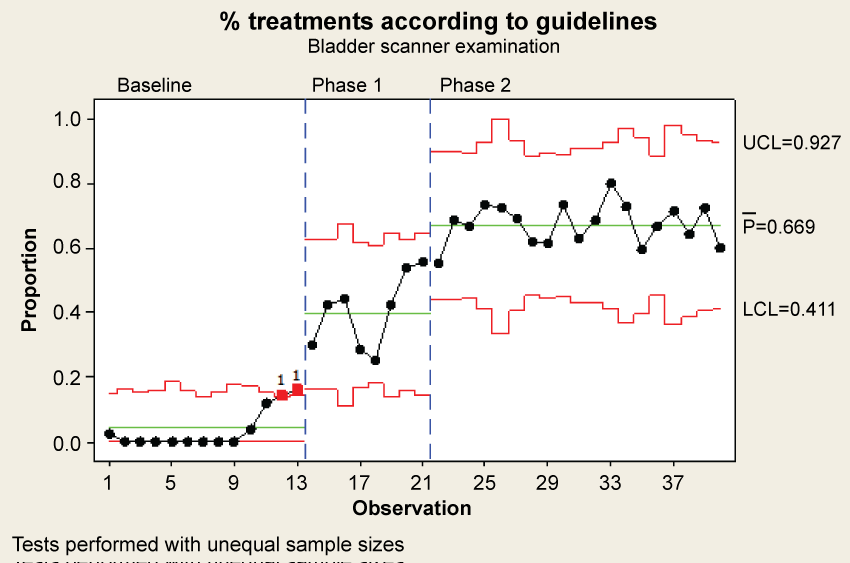
Figure 3: Percentage of orthopaedic patients at risk of UR, existed UR and/or treated with IUC who were treated according to the guidelines, as documented in the patient's record prior to and during the intervention. The phases are initiated after week 9, 13, and 17. The individual value is represented through the percentage of treatments according to guidelines. The observation on the x-axis is weekly basis.
UCL = Upper Control Limit, LCL = Lower Control Limit,
= average of % treatments, ▀ = significantly different from other values within the time period.
View Figure 3
During the four-year study period, a total of 1389 patient records have been reviewed, and 1319 (95%) of those patients had either UR or were at risk to get UR. The number of patients admitted to the orthopaedic ward and included in the study varied from 19 to 47 patients per week. Baseline data was collected during a nine-week period in 2007 and included 247 patients. Data in the intervention Phase I were collected during a 13-week period in 2007, which included 498 patients, and during Phase II for 17 weeks, which included 574 patients. The average age of the included patients was 64 at baseline and 69 at intervention Phase II. There were more women in the intervention's Phase II, 354 (58%) compared with the baseline data 153 (52%). There was no difference between the groups according to acute surgery, elective surgery or acute nonsurgical illness (Table 1).
![]()
Table 1: Characteristics of the patients included in the study.
View Table 1
At baseline there were only two patients out of 296 who got care in complete accordance with the guidelines. Baseline indicates a very low level of treatments according to guidelines (near zero percentage). Phase I shows an increasing trend from the two first observations with signals below lower control limit and two signals at the end of Phase I with signals above the upper control limit. Phase II shows a pattern with high percentage of treatments according to guidelines (on average 67%). The last phase also exhibits a stable process pattern (Figure 3).
When > 200 ml post-void residual urine was used as an indicator for being at risk of UR a clear trend was seen. The baseline data indicates a high number of patients assessed (on average 60%), according to guidelines, as at risk of UR. Phase I shows a decreasing trend and the Phase II shows a pattern with low percentage of patients at risk of UR (on average 11%) (Figure 4).

.
Figure 4: Percentage of orthopaedic patients assessed, according to guideline, as at risk of UR with preventable UR, as documented in the patient's record prior to and during the intervention. The phases are initiated after week 9, 13, and 17.
UCL = Upper Control Limit, LCL = Lower Control Limit,
= average of % treatments.
View Figure 4
Discussion
The review of the patient records shows that almost all patients in this orthopaedic study population had risk of UR, but there were no general guidelines on how to handle it before the intervention. This study shows an increased adherence to the guidelines over a two-year period with sustained results in the intervention Phase II, on average 67%. The proportion of UR was probably even higher in the group of patients at risk of UR before the intervention and in the group after the intervention handled without adherence to guidelines.
The result shows that it is possible to prevent UR arising in patients during orthopaedic care and treatment, and it is important to distinguish whether UR is an inevitable complication or if it is an adverse event that could have been prevented. By adherence to the suggested guidelines it is possible to start treatment of UR without delay, which decreases the risk of bladder damage and the need of treatment with urinary catheters [1]. With full adherence to the guidelines it may be possible to reduce UR further and increase the use of IUC on appropriate indications. Systematic implementation of evidence-based knowledge in clinical practice is challenging [29] and the knowledge from quality improvement research is still weak and under-theorized [30]. There is a need to bridge the gap between evidence, theory and practice by combining professional knowledge and quality improvement knowledge [31]. Developing the understanding of how QI intervention-programs work remains an important task, since such understanding is needed to avoid inappropriate interventions and learn from effective interventions [32].
Knowledge about contextual factors is important in quality improvement, [33] and therefore the coaches were important in this program, since they worked in their own familiar context and could understand how to use, adapt and transform the guidelines into their settings. Learning events and measurements were time-consuming both for the process leader and the coaches. Consequently, changes take time and the interventions need to be developed iteratively to be adopted to the local context [34]. In all participating units, other QI projects were ongoing simultaneously, and the process leader had to support and encourage coaches and wards individually to integrate the new guidelines into their local routines.
According to earlier studies, common barriers to 'Bladder Bundle implementation' and appropriate urinary catheter use include difficulty with nurse and physician engagement, patient and family request for indwelling catheters, and catheter insertion practices and customs in the emergency department [35]. In this study the coaches were trained and served as mediators helping staff to incorporate the new guidelines in their local practice. The increased adherence to the guidelines measured after the test period indicate this to be one successful way to implement new routines into local practice. Other strategies to address barriers were identified as explicitly discussing the risks of indwelling urinary catheters with patients and families, and engaging with emergency department nurses and physicians to implement a process that ensures that appropriate indications for catheter use are followed [31]. In this study, the patients and families were not explicitly involved. Getting feedback on what you accomplish is an important part of change and improvement work [26,36]. The feedback presented at staff meetings about the fulfillment of goals according to patient records probably increased the consequent use of the guidelines. Health care staff needs to understand the benefit of measures and to enhance that, showing results and visualization locally are important [37]. This was therefore considered in those interventions, and the results were visualized on whiteboards in the unit's corridor and goal fulfillment was encouraged with the placement of 'gold stars' next to the results.
Limitations
In the baseline registration, patient record data was scanty and incomplete, which may have affected the outcome of the review false positively. There were also differences in the study groups between the two phases (Table 1). The patients were older during the intervention period and the proportion of women was higher compared to baseline, but there was no difference in the number of patients with urinary retention between the groups.
Conclusions
A systematic improvement process using coaches and improvement tools can increase the adherence to new guidelines and incorporate them sustainably into local practice. This study also shows that adherence to guidelines can improve patient care, in this case decrease the number of patients at risk of UR in an orthopaedic patient population. This methodology, to use an improvement program to implement guidelines would certainly be suitable in other care departments and patient populations not only in IUC treatments. The guidelines were designed in co-operation with practice, to be easy to use in clinical work.
Acknowledgements
The authors would like to thank the contributing clinics and the professionals who took part in this project. We would also like to thank the persons who contributed in the expert group and development of the intervention.
Contribution
ACA took over and finished the writing of the paper, RMJ was the project leader, collected and analyzed data, ME assisted and finished the analysis and commented on the paper, BAG assisted in designing the study and commented on the paper, LC assisted in designing the study, analysis and finishing the paper. All authors can take responsibility for the accuracy of data and analysis.
Competing Interests
The authors have no competing interests to declare.
Funding and all Other Required Statements
This research was part of the second author's (R-M J) PhD studies, funded by Futurum, Region Jönköping County's PhD program, and the improvement part of the project was supported by the Center for Learning and Innovation in Healthcare, Qulturum, Jönköping Region County.
References
-
Mustonen S, Ala-Houhala I, Tammela TL (1999) Proteinuria and renal function during and after acute urinary retention. J Urol 161: 1781-1784.
-
Baldini G, Bagry H, Aprikan A, Carli F (2009) Postoperative urinary retention: anesthetic and perioperative considerations. Anesthesiology 110: 1139-1157.
-
Tambyah PA (2004) Catheter-associated urinary tract infections: diagnosis and prophylaxis. Int J Antimicrob Agents 24: S44-S48.
-
Aaronson DS, Wu AK, Blaschko SD, McAninch JW, Garcia M (2011) National incidence and impact of noninfectious urethral catheter related complications on the Surgical Care Improvement Project. J Urol 185: 1756-1760.
-
Saint S, Lipsky BA, Goold SD (2002) Indwelling urinary catheters: a one-point restraint? Ann Intern Med 137: 125-127.
-
Sanjay Saint, Jennifer A Meddings, David Calfee, Christine P Kowalski, Sarah L Krein (2009) Catheter-associated urinary tract infection and the Medicare rule changes. Ann Intern Med 150: 877-884.
-
Holroyd-Leduc JM, Sen S, Bertenthal D, Sands LP, Palmer RM, et al. (2007) The relationship of indwelling urinary catheters to death, length of hospital stay, functional decline, and nursing home admission in hospitalized older medical patients. J Am Geriatr Soc 55: 227-233.
-
Unbeck M, Dalen N, Muren O, Lillkrona U, Härenstam KP (2010) Healthcare processes must be improved to reduce the occurrence of orthopaedic adverse events. Scand J Caring Sci 24: 671-677.
-
Baines RJ, Langelaan M, de Bruijne MC, Asscheman H, Spreeuwenberg P, et al. (2013) Changes in adverse event rates in hospitals over time: a longitudinal retrospective patient record review study. BMJ Qual Saf 22: 290-298.
-
Saint S (2000) Clinical and economic consequences of nosocomial catheter-related bacteriuria. Am J Infect Control 28: 68-75.
-
Wald HL, Epstein AM, Radcliff TA, Kramer AM (2008) Extended use of urinary catheters in older surgical patients: a patient safety problem? Infect Control Hosp Epidemiol 29: 116-124.
-
Klevens RM, Edwards JR, Richards CL Jr, Horan TC, Gaynes RP, et al. (2007) Estimating health care-associated infections and deaths in U.S. hospitals, 2002. Public Health Rep 122: 160-166.
-
Verhamme KM, Sturkenboom MC (2007) Mortality in men admitted to hospital with acute urinary retention. BMJ 335: 1164-1165.
-
Hakvoort RA, Elberink R, Vollebregt A, Ploeg T, Emanuel MH (2004) How long should urinary bladder catheterisation be continued after vaginal prolapse surgery? A randomised controlled trial comparing short term versus long term catheterisation after vaginal prolapse surgery. BJOG 111: 828-830.
-
Kashefi C, Messer K, Barden R, Sexton C, Parsons JK (2008) Incidence and prevention of iatrogenic urethral injuries. J Urol 179: 2254-2257.
-
Wu AK, Auerbach AD, Aaronson DS (2012) National incidence and outcomes of postoperative urinary retention in the Surgical Care Improvement Project. Am J Surg 204: 167-171.
-
Thomas K, Oades G, Taylor-Hay C, Kirby RS (2005) Acute urinary retention: what is the impact on patients' quality of life? BJU Int 95: 72-76.
-
Johansson RM, Malmvall BE, Andersson-Gäre B, Larsson B, Erlandsson I, et al. (2013) Guidelines for preventing urinary retention and bladder damage during hospital care. J Clin Nurs 22: 347-355.
-
Tenke P, Köves B, Johansen TE (2014) An update on prevention and treatment of catheter-associated urinary tract infections. Curr Opin Infect Dis 27: 102-107.
-
Jennifer Meddings, Mary A M Rogers, Sarah L Krein, Mohamad G Fakih, Russell N Olmsted, et al. (2013) Reducing unnecessary urinary catheter use and other strategies to prevent catheter-associated urinary tract infection: an integrative review. BMJ Qual Saf 23: 277-289.
-
Johansson RM, Christensson L (2010) Urinary retention in older patients in connection with hip fracture surgery. J Clin Nurs 19: 2110-2116.
-
Langley GL, Moen R, Nolan KM, Nolan TW, Norman CL, et al. (2009) The Improvement Guide: A Practical Approach to Enhancing Organizational Performance. (2nd edn), Jossey-Bass Publishers, San Francisco.
-
Hibbard JH (2003) Engaging Health Care Consumers to Improve the Quality of Care. Med Care 41: 161-170.
-
Wilcock PM, Brown GC, Bateson J, Carver J, Machin S (2003) Using patient stories to inspire quality improvement within the NHS Modernization Agency collaborative programmes. J Clin Nurs 12: 422-430.
-
Nelson EC, Mohr JJ, Batalden PB, Plume SK (1996) Improving Health Care, Part 1: The Clinical Value Compass. Joint Comm J Qual Imp 22: 243-258.
-
Godfrey MM, Andersson Gare B, Nelson EC, Nilsson M, Ahlstrom G (2014) Coaching interprofessional health care improvement teams: the coachee, the coach and the leader perspectives. Nurs Manag 22: 452-464.
-
Polit DF, Beck CT (2012) Nursing Research: Generating and Assessing Evidence for Nursing Practice. (9th edn), Wolters Kluwer Health/Lippincott Williams & Wilkins, Philadelphia.
-
Benneyan JC, Lloyd RC, Plsek PE (2003) Statistical process control as a tool for research and healthcare improvement. Qual Saf Health Care 12: 458-464.
-
Grol R, Grimshaw J (2003) From best evidence to best practice: effective implementation of change in patients' care. Lancet 362: 1225-1230.
-
Shojania KG, Grimshaw JM (2005) Evidence-based quality improvement: the state of the science. Health Aff (Millwood) 24: 138-150.
-
Batalden PB, Stoltz PK (1993) A framework for the continual improvement of health care: building and applying professional and improvement knowledge to test changes in daily work. Jt Comm J Qual Improv 19: 424-447.
-
Dixon-Woods M, Leslie M, Carolyn Tarrant, Julian Bion (2013) Explaining Matching Michigan: an ethnographic study of a patient safety program. Implementation Science 8: 70.
-
Kaplan HC, Brady PW, Dritz MC, Hooper DK, Linam WM (2010) The influence of context on quality improvement success in health care: a systematic review of the literature. Milbank Q 88: 500-559.
-
Laura J Damschroder, David C Aron, Rosalind E Keith, Susan R Kirsh, Jeffery A Alexander, et al. (2009) Fostering implementation of health services research findings into practice: a consolidated framework for advancing implementation science. Implementation Science 4: 50.
-
Sarah L Krein, Christine P Kowalski, Molly Harrod, Jane Forman, Sanjay Saint (2013) Barriers to reducing urinary catheter use: a qualitative assessment of a statewide initiative. JAMA Intern Med 173: 881-886.
-
Dixon-Woods M, McNicol S, Martin G (2012) Ten challenges in improving quality in healthcare: lessons from the Health Foundation´s programme evaluations and relevant litterature. BMJ Qual Saf 21: 876-884.
-
Mountford J, Shojania KG (2012) Refocusing quality measurement to best support quality improvement: local ownership of quality measurement by clinicians. BMJ Qual Saf 21: 519-523.