International Archives of Nursing and Health Care
Understanding the Factors Associated with Abortion among Women Seeking Abortion Related Health Services in Phuentsholing General Hospital, Bhutan
Kinley Wangdi1,2* and Manish Raj Gurung1
1Phuentsholing General Hospital, Phuentsholing, Bhutan
2Research School of Population Health, The Australian National University, ACT, Australia
*Corresponding author: Kinley Wangdi, Research School of Population Health, College of Medicine, Biology and Environment, The Australian National University, ACT, Australia, E-mail: dockinley@gmail.com
Int Arch Nurs Health Care, IANHC-2-059, (Volume 2, Issue 5), Review Article; ISSN: 2469-5823
Received: August 24, 2016 | Accepted: October 24, 2016 | Published: October 28, 2016
Citation: Wangdi K, Gurung MR (2016) Understanding the Factors Associated with Abortion among Women Seeking Abortion Related Health Services in Phuentsholing General Hospital, Bhutan. Int Arch Nurs Health Care 2:059. 10.23937/2469-5823/1510059
Copyright: © 2016 Wangdi K, et al. This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited.
Abstract
Introduction: Abortion is illegal in Bhutan. However, "Medical Termination of Pregnancy" (MTP) had been allowed by the Ministry of Health and Education since 1999. The aims of this study were to understand the trend of abortion and associated factors leading to induced abortion in Phuentsholing General Hospital (PGH).
Methods: A retrospective study to understand the trends of all forms of abortion was carried out using secondary data from PGH data repository. The trend was analyzed between the periods 1st January 2008 to 31st December 2011. A prospective study was also carried out between 1st March 2012 and 28th February 2014 using a structured interviewer administered questionnaire on patients seeking medical care for abortion related ailments in PGH.
Results: The retrospective analysis showed that a total of 465 cases (average 9.75 cases/month) were treated in PGH. In the prospective study the median age of the respondents was 26 years (range 18-42 years). Most participants were older than 25 years 57.1% (44), married 93.4% (71), house wives, 59.7% (46) and primary or secondary level educated 45.5% (35). The main underlying reason for induced abortion was that the family was complete and not ready for family at 22.2% (6) each. In multivariate analysis, second month of pregnancy is less likely to undergo induced abortion, AOR 0.03 (95% CI 0.042, 0.805).
Conclusions: Phuentsholing General Hospital treated almost 10% of the total abortion in Bhutan with an average of 9.75 cases per month. The main reasons for undergoing induced abortion were family was complete and not ready for the family.
Keywords
Abortion, Induced, Bhutan
Introduction
It is estimated around 42 million women worldwide seek an abortion for unintended pregnancy each year, and 20 million resort to unsafe abortions with 98% of them in developing countries [1]. Unsafe abortion is defined as a procedure for terminating an unintended pregnancy carried out either by persons lacking the necessary skills or in an environment that does not conform to minimal medical standards, or both [2,3]. Fourteen percent of all unsafe abortions in low- and middle-income countries are among women aged 15-19 years. About 2.5 million adolescents have unsafe abortions every year, and adolescents are more seriously affected by complications than older women [4]. Deaths attributed to unsafe abortions in developing countries are estimated at 80,000 annually, i.e. 400 deaths per 1,00,000 abortions. Each day 192 women die because of complications associated with unsafe abortions which amount to one woman every eight minutes, all of them in developing countries [5].
The Penal Code of Bhutan states that abortion is illegal except when it is conducted to save the life of the mother or when the pregnancy is a result of rape, or when the mother is mentally unsound [6,7]. In 1999 the Ministry of Health and Education legalized the "Medical Termination of Pregnancy" (MTP). To carry out medical termination, the certification of two medical doctors is required. However, the number of abortion for medical reasons is minimal according to hospital sources [8]. Its incidence is expected to be low considering that there is still a strong adherence to Buddhist beliefs and given society's acceptance of children born out of wedlock. However, according to some studies, over the years a growing number of Bhutanese women are seeking unsafe abortion in the neighbouring areas of India [6,8,9]. Obtaining accurate data for abortions is challenging, and especially so for unsafe induced abortion [7,10].
In Phuentsholing General Hospital (PGH), women seeking treatment for complications associated with unsafe abortion were seen routinely. Therefore, the aims of this study were to understand the trend and burden of abortions and factors associated with an abortion amongst women attending PGH. Additional aims were to determine the contraceptive use and underlying reasons for not using contraceptives.
Methods
Study area
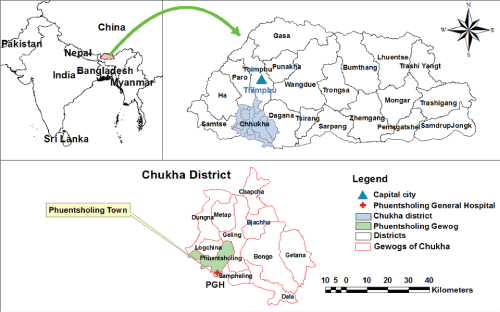
The study was conducted in Phuentsholing General Hospital (PGH) under Chukha Dzongkhag. Phuentsholing Town is the second largest city in Bhutan. It is located 171 km south of Thimphu, and is the commercial hub of Bhutan. Indian town of Jaigaon located next to Phuentsholing allows easy access for a variety of reasons including employment, commercial and entertainment purposes to name a few. PGH is a 50 bedded hospital, with specialist services in General Surgery and Obstetrics and Gynaecology, besides the general care of the patients. The hospital caters to the people of Phuentsholing Town and other sub-districts of Phuentsholing, and Sampheling (Figure 1). PGH serves as the referral centre for gynaecological services from the neighboring health centres of Gedu Hospital (Chukha Dzongkhag), Samtse Hospital, Gomtu Hospital and Sibsoo Hospital under Samtse Dzongkhag, and Lhamozingkha BHU I under Dagana Dzongkhag. The total population of Phuentsholing for the year 2015 was approximately 24,721 [11,12].
Retrospective study
The retrospective study was conducted to understand the trend of abortion from all causes in PGH from 1st January 2008 to 31st December 2011. The data was extracted by two researches (KW and MRG) from admission forms of admitted patients and monthly morbidity reporting forms from the hospital data repository and crossed checked with the District Health Office (DHO) data base to validate the completeness of data. The data extracted were monthly reported abortions from all causes and sub-divided into Outpatient Department (OPD) patients and In-Patients.
Prospective study
The prospective study was conducted from 1st March 2012 to 28th February 2014 using a questionnaire. Based on other published studies, a standard questionnaire was modified into four parts with both closed and open-questions [13,14]. The part one of questionnaire related to demographic information of the participants; and part two related to reasons for undergoing abortion and methods used for abortion. Parts three and four of questionnaire were on outcome and complications of abortion and contraceptive information, respectively.
Attempts were made to administer the questionnaire to all the patients seeking abortion associated care in PGH: In-patient, Emergency Department and patients attending OPD. Patients who consented to participate in the study were included in the study after consent forms were signed. The questionnaire was administered to the participants by the female nurses of PGH. The interviewers were given one day training on administering the questionnaire. The outcome of the abortion was obtained for each participant from the admission and discharged forms.
Statistical Analysis
Descriptive statistics (frequencies and mean) was used to describe the demographic characteristics and outcome of the event. The types of abortion were stratified by potential covariates and compared using Pearson's chi-squared test. Bivariate and multivariable logistic regression was used to examine the independent correlates with induced abortion built using backward elimination to identify significant covariates. An alpha value of 0.20 was used to determine which variables remained in the model. A value of p ≤ 0.05 was considered significant. Data analysis was carried out using STATA Intercooled 10. Ethical approval for this study was provided by the Research Ethics Board of Health (REBH), MoH, Royal Government of Bhutan (reference number: REBH/Approval/11/018). Written informed consent was obtained from every respondent. Interviewers explained the general purpose, benefits, and any risks of the survey to each respondent in his or her local language, and respondents had the right to refuse participation in the survey at any point.
Results
Retrospective study
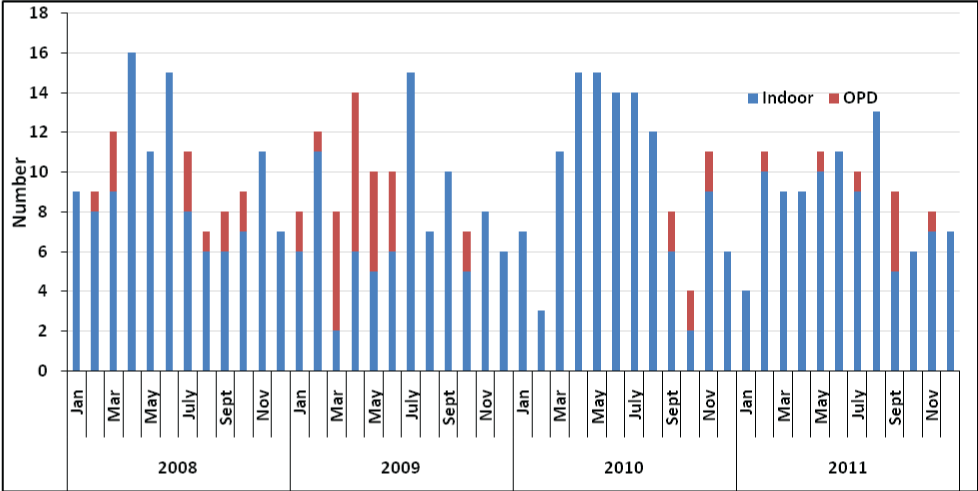
The retrospective study of four years showed that on an average, 9.75 cases per month (range 3-16) reported to hospital for abortion associated care. During this period, the highest cases were reported in 2008 with 125 cases (mean-10.42) and the lowest in 2011 with 108 cases (mean-9) (Table 1). The trend of abortion continued to be constant throughout year (Figure 2).
.
Figure 2: Abortion trend- total along with trends amongst In-Patients and OPD in Phuentsholing General Hospital, 2008-2011.
View Figure 2
![]()
Table 1: Summary of abortion trend extracted from PGH data base from 2008-2011.
View Table 1
Prospective study
Socio-demographic characteristics: A total of 77 patients were recruited for the prospective study over two years from 1st March 2012 to 28th February 2014. This included both induced and spontaneous abortions. The median age of the patients was 26 years (range 18-42 years). Most of the patients were older than 25 years accounting up to 57.1% (44). Primary or secondary level educated women made up the most patients 45.4% (35) followed by those women with no formal education at 39.0% (30). A majority of patients were married 93.4% (71); house wife and private employee made up the most patients at 59.7% (46) and 28.6% (22), respectively. More than forty eight percent (37) of participants had 1-2 children, 34.2% (26) did not have any children. Of those who had children, 38.7% (27) of the children were in the age range of 1-5 years. Most of the women were one to two months pregnant. The commonest method of abortion amongst those who induced abortion was taking medicine (85.2%) (Table 2).
![]()
Table 2: Socio-demographic characteristic of study participants, induced abortion and other forms of abortion.
View Table 2
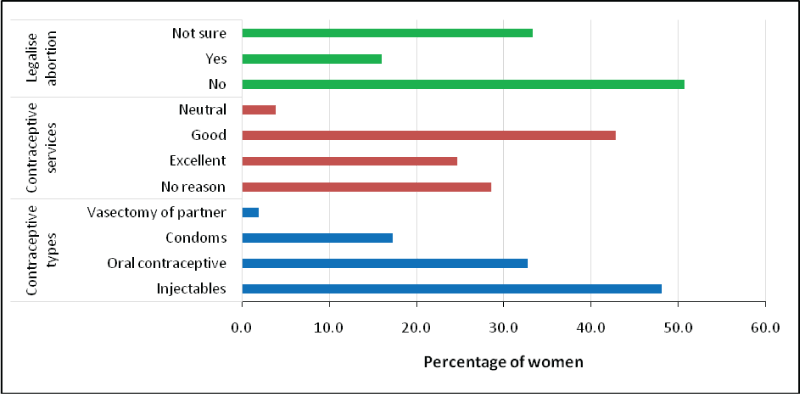
Contraceptive use and types of abortion: Two third of the study participants used contraceptives 67.5% (52). The most common type of contraceptive was injectable contraceptives followed by oral contraceptive, 48.1% (25) and 32.7% (17) respectively. Nearly half of the respondents, 41.9% (33) reported that quality of contraceptive services were good while 24.7% (19) reported the services were excellent. More than 22.0% (17) failed to give any reasons for not using contraceptive. Half of the participants 49.4% (38) said that abortion should not be legalized as a form of contraceptives, 32.5% (25) were unsure whether abortion should be legalized, however, 15.6% (12) responded that abortion should be legalized (Figure 3).
.
Figure 3: Contraceptive types and opinion regarding the quality of services and legalization of abortion as contraceptive methods.
View Figure 3
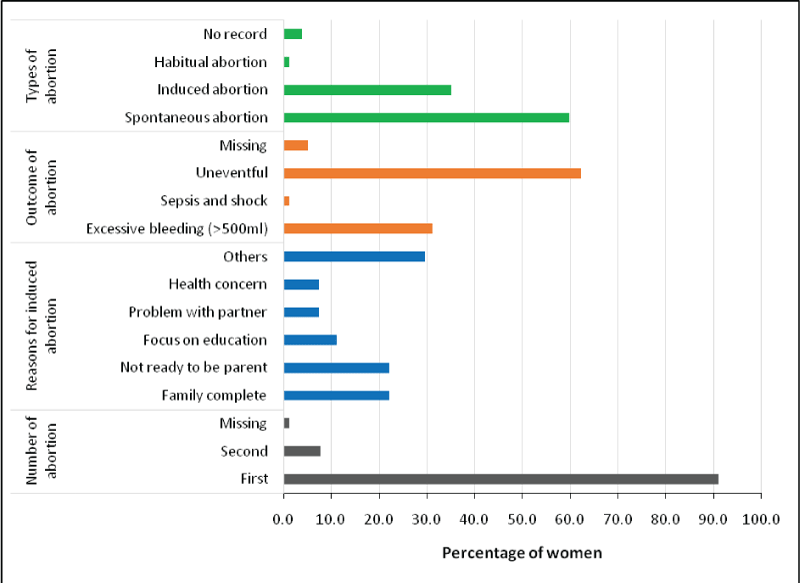
The commonest type of abortion was spontaneous abortion (abortion that occurred naturally without medical or surgical intervention) followed by induced abortion (both medical and surgical outside the hospital) at 59.7% (46) and 35.1% (27) respectively. The commonest outcome of the abortion was uneventful at 62.3% (48). In 31.2% (24) of participants had excessive bleeding (> 500 ml) and only one patient had serious complication of sepsis and shock (1.3%) due to spontaneous or induced abortion outside hospital. A very few participants 7.4% (2) each stated that contraceptive failure was the result of the pregnancy and did not want to continue pregnancy as a concern for the health of the participants and problem with the partner. For most of the participants 90.9% (70), this was the first abortion while it was second abortion for 7.8% (6) (Figure 4).
Determinants of induced abortion:Married women were less likely to undergo induced abortion as compared to those who were single, living together, student and divorcee. Months of pregnancy were significantly associated with other types of abortion (Table 2).
In multivariate analysis, only one variable was significant predictors of induced abortion. Women in second month of pregnancy were less likely to undergo abortion as compared to those in first month of pregnancy (AOR = 0.03, (95% CI 0.042, 0.805) (Table 3).
![]()
Table 3: Multivariate logistic regression to find out association between the induced abortions with demographic variables.
View Table 3
Discussion
Abortion from all causes have increased during the study period in Bhutan from 928 to 1190 [8,15-17]. However, there was fluctuation of abortion cases in PGH with highest reported in 2010 and lowest in 2009. In 2010, PGH treated about 10% of total abortion cases in the country. This could be as a result of induced abortion in Indian town of Jaigon because abortion as a form of contraceptive is illegal in Bhutan. In our study more than half of the women were admitted for induced abortion with some complications such as bleeding and internal injury. These complications can lead to abortion-related morbidity [18,19]. The morbidity due to unsafe abortion, particularly in developing countries, results in a heavy burden on women, their families and the health care system [20,21]. Restrictive laws on abortion also inhibit people from seeking medical care.
Despite significant annually reported abortion from all causes in PGH from 2008-2011, the study failed to enrol adequate number of participants. One of the possible impediments in enrolling participants in the study was due to the social stigma associated with abortion. Secondly, undergoing abortion is seen as morally incorrect and religiously sinful, given large proportion of Bhutanese are Buddhists. Social and cultural beliefs against abortion are other barriers to accessing services. Whether legal or illegal, abortion is frequently censured by religious teachings and ideologies, hidden due to fear of reprisals or because of social condemnation and restrictive laws. Similar finding had been reported in other studies [22,23]. Higher rates of unintended pregnancy in an environment in which abortion is illegal and highly stigmatized may result in increased morbidity and mortality as a result of unsafe abortion [24].
The main reasons for induced abortion were family being complete, not ready to start a family, and focus on education [25-27]. Even though the contraceptive use among the participants was 67.5%, women failed to avail contraceptive services which are offered free of cost in Bhutan. Generally, contraceptive rate in Bhutan stands at 65.6% for 2011 [28]. Present study did not explore the reasons for low contraceptive use in PGH. However, it has been highlighted in literature that the main reasons teenager did not use contraceptive services was due to the attitude and responses from the service provider [29]. Despite offering free contraceptives in Bhutan, the accessibility may be one of the main barriers for availing the services. The free contraceptives in the hospitals and health centers have limited hour of services, opening from 9:00 AM and closing at 3:00 PM. Similarly, emergency contraceptive such as pills over morning are available but restricted in the hospitals only (personal communication). These services are not provided during the other times except for the condoms which are provided at many locations such as hotels and other public places. However, the availability of condoms is not monitored regularly. Improvement in access to emergency contraceptives could reduce unwanted pregnancy and thereby unsafe abortion.
Married women were less likely to undergo induced abortion as compared to those who are single, student, living together and divorcee in this study, which is in agreement with number of studies but contradicted a study from Ghana [30-33]. This finding of women in non-marital unions is more likely to choose induced abortion because single women have options when faced with unplanned pregnancies. The month of pregnancy was significant factor in multivariate analysis. As the pregnancy progressed the risk of induced abortion decreased. This could be as a result of complications associated with undergoing abortion as the pregnancy progressed [34].
The study has various limitations. Firstly, due to small number of study participants the power of study was weak. Secondly, interviewer being the nurses from the hospital introduced interviewer bias. Thirdly, all cases of abortion could not be recruited because of the heavy clinical works and responsibilities. Despite the limitations, this study shows that there are significant numbers of women undergoing induced abortion. Therefore, it is recommended to conduct similar study in other hospitals to find out the true burden of induced abortion.
Conclusions
There were significant cases of abortion from all causes that reported to PGH for abortion associated care. The common types of abortion were spontaneous abortion followed by induced abortion. The main reasons for induced abortion were completion of family and not ready to have another child. The commonest complication was loss of blood more than 500 ml. Also use of contraceptives among the study population was higher than the contraceptive rates of Bhutan.
Acknowledgement
Our deepest gratitude goes to all the individuals who participated in this survey. We are very grateful to all the nurses who were actively involved in carrying out data collection. We acknowledge UNICEF, Bhutan and Reproductive programme, Department of Public Health (DoPH), Ministry of Health (MoH) for providing funds to carry out this study and Research Ethics Board of Health (REBH), MoH, for clearing the ethics.
Author Contribution
KW and MRG conceived the idea. KW developed the questionnaires, analysed and interpreted data and drafted the manuscript. MRG helped in data collection, compilation, and critical revision of the manuscript. Both authors read and approved the final version of the manuscript.
Conflict of Interest
We declare no conflict of interest.
References
-
WHO (2007) Unsafe abortion: global and regional estimates of incidence of unsafe abortion and associated mortality in 2003. (5th edn), Geneva, Switzerland.
-
WHO (2008) Unsafe abortion. Sixth Edition.
-
Sedgh G, Henshaw S, Singh S, Ahman E, Shah IH (2007) Induced abortion: estimated rates and trends worldwide. Lancet 370: 1338-1345.
-
Bingham A, Drake JK, Goodyear L, Gopinath CY, Kaufman A, et al. (2011) The role of interpersonal communication in preventing unsafe abortion in communities: the dialogues for life project in Nepal. J Health Commun 16: 245-263.
-
Shah I, Ahman E (2009) Unsafe abortion: global and regional incidence, trends, consequences, and challenges. J Obstet Gynaecol Can 31: 1149-1158.
-
Peldon S (2011) Should abortion be legalized? Bhutan Observer.
-
(2008) Ministry of Health. Adolescent Health and Development, A country profile. Ministry of Health, Thimphu, Bhutan.
-
MoH (2011) Annual Health Bulletin 2010. Thimphu: Minstry of Health, Royal Goverment of Bhutan.
-
Choden J, Pem R, Pathak A (2015) Prevalence, determinants and outcomes of unplanned pregnancy and perspectives on termination of pregnancy among women in Nganglam, Bhutan. Bhutan Health Journal 1: 30-37.
-
GNHC (2010) Population and development situation analysis 2010. Thimphu, Bhutan: Gross National Happiness Commission.
-
(2008) National Statistics Bureau. Dzongkhag Population Projection 2006-2015.
-
(2006) Office of the Census Commissioner. Results of Population & Housing, Census of Bhutan 2005.
-
Dahlbäck E, Maimbolwa M, Kasonka L, Bergström S, Ransjö-Arvidson AB (2007) Unsafe induced abortions among adolescent girls in Lusaka. Health Care Women Int 28: 654-676.
-
Lema VM, Rogo KO, Kamau RK (1996) Induced abortion in Kenya: its determinants and associated factors. East Afr Med J 73: 164-168.
-
MoH (2008) Annual Health Bulletin 2008. Thimphu, Bhutan: Ministry of Health, Royal Government of Bhutan.
-
MoH (2009) Annual Health Bulletin 2009. Thimphu, Bhutan: Ministry of Health, Royal Government of Bhutan.
-
MoH (2011) Annual Health Bulletin 2011. Thimphu, Bhutan: Ministry of Health, Royal Government of Health.
-
Sama CB, Aminde LN, Angwafo FF (2016) Clandestine abortion causing uterine perforation and bowel infarction in a rural area: a case report and brief review. BMC Res Notes 9: 98.
-
Ikeanyi ME, Okonkwo CA (2014) Complicated illegal induced abortions at a tertiary health institution in Nigeria. Pak J Med Sci 30: 1398-1402.
-
Singh S (2006) Hospital admissions resulting from unsafe abortion: estimates from 13 developing countries. Lancet 368: 1887-1892.
-
Grimes DA, Benson J, Singh S, Romero M, Ganatra B, et al. (2006) Unsafe abortion: the preventable pandemic. Lancet 368: 1908-1919.
-
Rossier C (2007) Abortion: an open secret? Abortion and social network involvement in Burkina Faso. Reprod Health Matters 15: 230-238.
-
Cockrill K, Upadhyay UD, Turan J, Greene Foster D (2013) The stigma of having an abortion: development of a scale and characteristics of women experiencing abortion stigma. Perspect Sex Reprod Health 45: 79-88.
-
Gipson JD, Hirz AE, Avila JL (2011) Perceptions and practices of illegal abortion among urban young adults in the Philippines: a qualitative study. Stud Fam Plann 42: 261-272.
-
Vallely LM, Homiehombo P, Kelly-Hanku A, Whittaker A (2015) Unsafe abortion requiring hospital admission in the Eastern Highlands of Papua New Guinea--a descriptive study of women's and health care workers' experiences. Reprod Health 12: 22.
-
Levandowski BA, Kalilani-Phiri L, Kachale F, Awah P, Kangaude G, et al. (2012) Investigating social consequences of unwanted pregnancy and unsafe abortion in Malawi: the role of stigma. Int J Gynaecol Obstet 2: S167-171.
-
Dahlbäck E, Maimbolwa M, Yamba CB, Kasonka L, Bergström S, et al. (2010) Pregnancy loss: spontaneous and induced abortions among young women in Lusaka, Zambia. Cult Health Sex 12: 247-262.
-
MoH (2014) Annual Health Bulletin 2013. Thimphu: Ministry of Health, Royal Govenment of Bhutan.
-
Wood K, Jewkes R (2006) Blood blockages and scolding nurses: barriers to adolescent contraceptive use in South Africa. Reprod Health Matters 14: 109-118.
-
Schwandt HM, Creanga AA, Danso KA, Adanu RM, Agbenyega T, et al. (2011) A comparison of women with induced abortion, spontaneous abortion and ectopic pregnancy in Ghana. Contraception 84: 87-93.
-
Kalyanwala S, Zavier AJ, Jejeebhoy S, Kumar R (2010) Abortion experiences of unmarried young women in India: evidence from a facility-based study in Bihar and Jharkhand. Int Perspect Sex Reprod Health 36: 62-71.
-
Maina BW, Mutua MM, Sidze EM (2015) Factors associated with repeat induced abortion in Kenya. BMC Public Health 15: 1048.
-
Mote CV, Otupiri E, Hindin MJ (2010) Factors associated with induced abortion among women in Hohoe, Ghana. Afr J Reprod Health 14: 4.
-
Nkwabong E, Mbu RE, Fomulu JN (2014) How risky are second trimester clandestine abortions in Cameroon: a retrospective descriptive study. BMC Womens Health 14: 108.