International Archives of Nursing and Health Care
Educational Intervention to Improve Nursing Practice in the Critical Care Setting
Ann-Charlotte Falk* RN, CCRN, MSN, PhD
Department of Neurobiology, Karolinska University Hospital, Sweden
*Corresponding author: Ann-Charlotte Falk RN, CCRN, MSN, PhD, Karolinska Institute, Department of Neurobiology, Alfred Nobels allé 23, Division of Nursing, Intensive Care, Karolinska University hospital , SE-171 76 Stockholm, Sweden, E-mail: ann-charlotte.falk@karolinska.se
Int Arch Nurs Health Care, IANHC-1-002 (Volume 1, Issue 1), Research Article; ISSN: 2469-5823
Received: March 13, 2015 | Accepted: May 22, 2015 | Published: May 26, 2015
Citation: Ann-Charlotte F (2015) Educational Intervention to Improve Nursing Practice in the Critical Care Setting. Int Arch Nurs Health Care 1:002. 10.23937/2469-5823/1510002
Copyright: © 2015 Ann-Charlotte F. This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited.
Abstract
A variety of educational interventions may have an impact on patient assessment and patient outcome. Studies have reported an inconsistency in the use of Neurological assessments performed by nurses, such as the Glasgow Coma Scale (GCS) in the acute care setting. The aim of this study is to evaluate the impact of an educational intervention for nurses on the number of performed neurological assessments over time.
Intervention: A total of 60 health care staff was offered education on neurological assessment (GCS) of Pediatric Intensive Care Unit (PICU) at a level one-trauma center.
Methods: A quasi-experimental design to evaluate the change in the number of performed neurological assessments in children. The amount of GCS assessments was compared before and after the educational intervention.
Findings: The educational intervention showed a significant increase in GCS assessments during the one and two-month periods after the intervention but with a decline at three months post-intervention.
Keywords
Continuing educational, Interventions, Outcome, Nursing, Critical Care
Introduction
Studies have shown that a variety of educational interventions may have an impact on patient assessment and patient outcome; however, the majority has been results from medical education of residents [1,2]. To my knowledge, only a few studies describing Continuing Medical Education (CME) for nurses in the clinical setting and there is a shortage of evidence for it's effectiveness and efficacy [3,4]. The rapid development of both medical and technical techniques in critical care during recent years has placed a high demand on the personal ability of health care staff to collect and analyze important information at the right time. This high demand on a personal level makes the planning of educational interventions even more important if the learning is to be successful, effective and improve patient outcome. In the acute care setting the ability to identify patients in need of acute interventions is essential. To facilitate the early detection of complications during care, health care professionals use a variety of assessment tools. For patients with a traumatic brain injury, the assessment of conscious level is crucial, and the primary tool is the Glasgow Coma Scale (GCS) [5,6]. The ultimate goal in the use of GCS is to identify those in need of acute intervention as early as possible and thus prevent secondary brain injuries [7], thereby reducing both mortality and morbidity among patients. From a clinical and educational point of view, all healthcare professionals working in emergency care should use assessment of conscious level as easily as other routine observations of vital signs [8]. However, several studies have reported an inconsistency in the use of GCS in the clinical setting, and it is recognized that education and training is required to ensure that the tool is used as a valid indicator of patient status [9].
Reports on interventions concerning continued education for nurses working in critical care areas show support for different implementation approaches, but they lack descriptions of theoretical and educational considerations [10]. In the clinical setting the need for an educational intervention concerning the assessment of GCS has been expressed and the lack of studies of successful educational interventions for nursing in the critical care area shows the need for further studies.
Theoretical Framework
The educational session was planned with an objective goal (to improve the frequency of neurological assessment) but also with the adult learning theory [11] in mind. The theory is based on the assumption that learning occurs when learners decide what they need to learn; it is not based on the teacher's view of what the learners need to know. Adult learning assumptions are:
• Adults prefer learner-centered learning, which provides greater control and autonomy in the learning process.
• Adult learning is rooted in the acquisition of learning skills and the use of a reflective process
• Experience is the core of adult learning
• Adults value learning that helps them deal with real-life situations
To achieve learning the learner is treated as an independent and self-directed learner, which includes taking into account the health care professionals' own educational needs, providing a comfortable climate for learning, and involving learners in the planning of the session [12].
Therefore, the aim of this study was to evaluate educational interventions based on adult learning theory in the critical care setting and their impact on the frequency of neurological assessment over time.
Research Design
Quasi-experimental, using one group, with before and after measurements performed to evaluate changes in performed neurological assessment in children cared for in a PICU.
Sample
A total of 60 health care staff (Reg.nurses n=30 and nurses aids n=30.) with theoretical knowledge and experience (range: 1-30 years) from critical care was offered education on neurological assessment of children in the PICU at a level one-trauma center. The PICU had eight beds and cared for children (0-18 years) with both medical and surgical conditions. The educational intervention was performed on three occasions during November 2012. All health care staff had taken an introduction course during the first year of employment, consisting of neurological assessment of children and clinical experience of care of children requiring intensive care.
Intervention
The educational session included one seminar lasting 1.5 hours on three occasions which was planned by the author. The author, with a pedagogical education and with clinical experience of critical care, conducted all sessions. The purpose of the session was to define neurological assessment (the how, when and why) for educated nursing staff in critical care with basic knowledge in neurological disorders in children and the regular assessment of vital signs, describe the role of the GCS and provide evidence to support the importance of detecting early signs of change in neurological performance. The educational intervention was planned with an adult learning theory, which included taking account of the health care professionals' own educational needs based in their knowledge and experience from critical care. This was evaluated at the beginning of each session by asking the staff what they wanted and needed to know in relation to neurological assessment; creating a comfortable learning climate and engaging in a dialog with the participants which involved the learners in the planning of the session; encouraging the learners to formulate their own learning goals in writing; and using actual cases from the clinical setting to visualize the learning objectives [1,11]. All this required a flexible teaching role with the focus on the participant's demands and not on the teacher's own specialized knowledge.
Procedure
Data from the registry system of patient care at the PICU concerning the amount of assessments of GCS was collected in retrospect and entered into an Excel database. Descriptive statistics was analyzed (numbers and per cent). The demographic variables, such as the number of patients and their diagnoses, were collected to verify that the frequencies were not dependent on the number of patients or their diagnosis using a T-test. A p-value < 0.005 was considered statistically significant. To analyze the impact of the educational intervention a before measure (Pearson Chi-Square for nominal variables) of the frequencies (n, %) of performed neurological assessment during the month of October compared to November, December and January was performed. All analysis was conducted using IBM SPSS version 20.0.
Ethical considerations
Ethical approval was not obtained since no personal information was collected from individual health care personnel and the study was considered to measure quality of care. Therefore, the local ethical committee would not consider the application for ethical approval. The manager of the ward approved the study.
Findings
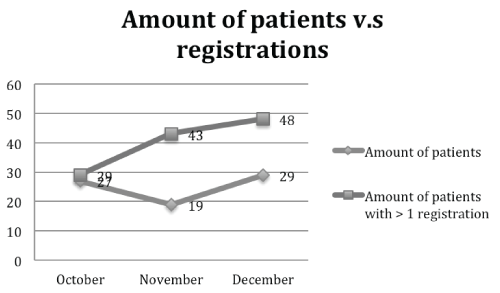
A total of 60 health care staff participated in the educational intervention. Our result showed a significant (Chi-square= 64.56, df=2, p=< 0.001) increase in assessments during the one and two-month periods after the intervention (Figure 1).
.
Figure 1: Number of patients vs. number of patients with more than one registration
View Figure 1
There was also a significant increase in the total number of registrations/patient and was not dependent on the number of patients or the diagnosis of the patient (Figure 2).
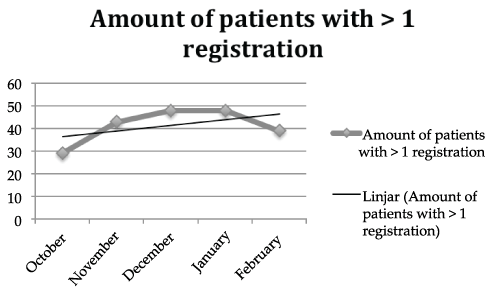
The result shows an increase of registrations of GCS during the first two months but a decline after three months (Figure 3).
.
Figure 3: Number of patients with more than one registration during the three-month period after the educational intervention
View Figure 3
Discussion
The result shows a positive result of an educational intervention for nurses aimed to increase the frequency of neurological assessment (GCS) in children receiving critical care.
The significant change in nursing behavior could be a result of the educational session planned with adult learning theories in mind as well as several teaching approaches during the educational session. The result is well in line with the result described by Bloom [4] who states that combining teaching techniques for physicians such as: interactive education, audit and feedback, reminders, clinical practice guidelines and using opinion leaders all show a positive effect on medical care and patient outcome. This positive result could also be a result of both improved knowledge concerning the assessment of GCS and its value for patient care, or the fact that the participants' own experience was included in the session.
However, the health care professionals, especially in the critical care unit, who sometimes have an intense workload, need feedback on their assessments to sustain a change in behavior. This result is well in line with the result of Howell et al. [13] and Flodgren et al. [14] that also showed a decline in a positive change three months post-education. With this in mind, not only knowledge but also changes in behavior could result from educational interventions, but more than one intervention is needed to further develop sustainable change, even after an intervention using adult learning theories. As described by Davies et al. [3] and Bloom [4] studies concerning outcome after CME has to consider: different practitioners, hospital settings and behaviors to understand the full effect of an educational intervention. The rapid development of both medical and technical techniques during care and especially in critical care puts high demand on both organizations and the individual health care professionals to continuously develop clinical skills to improve the quality of patient care. As discussed by Bloom [4] it is clear that the least-effective education methods in the clinical setting are didactic lectures and distributing printed materials alone. How clinical education should be performed in the future should be in focus for research and quality improvement programs so that educational interventions are evaluated with the right outcome.
There are several limitations to this study. To evaluate the impact on patient care i.e. improved outcome measured by mortality and morbidity rates, this study should have been evaluated using a long-term follow-up, which was not possible during this time period. Due to the fact that there is a small incidence (four per cent as reported by Snoek et al. [15] of neurological deterioration after a brain injury, the impact of measuring GCS has to be measured over several years for a valid result.
The small sample and the short period of evaluation time could have had an impact on the result. To further study the impact of using adult learning theories, several teachers/facilitators and several clinical settings should be compared.
Conclusion
Educational interventions using adult learning theories are well suited to promote learning in the clinical setting in order to encourage changes in nursing behavior. To achieve sustainable change in behavior, repeated feedback is necessary; therefore when planning an educational intervention continued feedback should also be prearranged.
References
-
Davis D, O'Brien MA, Freemantle N, Wolf FM, Mazmanian P, et al. (1999) Impact of formal continuing medical education: do conferences, workshops, rounds, and other traditional continuing education activities change physician behavior or health care outcomes? JAMA 282: 867-874
-
Marinopoulos SS, Dorman T, Ratanawongsa N, Wilson LM, Ashar BH, et al. (2007) Effectiveness of continuing medical education. Evid Rep Technol 149: 1-69.
-
Davis DA, Thomson MA, Oxman AD, Haynes RB (1995) Changing physician performance. A systematic review of the effect of continuing medical education strategies. JAMA 274: 700-705.
-
Bloom B (2005) Effects on continuing medical education on improving physician clinical care and patient health: A review of systematic reviews. International Journal of Technology Assessment in Health Care, 21: 380-385.
-
Teasdale G, Jennett B (1974) Assessment of coma and impaired consciousness. A practical scale. Lancet 2: 81-84.
-
MRC CRASH Trial Collaborators, Perel P, Arango M, Clayton T, Edwards P, et al. (2008) Predicting outcome after traumatic brain injury: practical prognostic models based on large cohort of international patients. BMJ 336: 425-429
-
National institute for health and clinical excellence (2013) Head injury (CG56) Triage, assessment, investigation and early management of head injury in infants, children and adults.
-
Palmer R, Knight J (2006) Assessment of altered conscious level in clinical practice. Br J Nurs 15: 1255-1259.
-
Fischer J, Mathieson C (2001) The history of the Glasgow Coma Scale: implications for practice. Crit Care Nurs Q 23: 52-58.
-
Ross A, Crumpler J (2007) The impact of an evidence-based practice education program on the role of oral care in the prevention of ventilator-associated pneumonia. Intensive Crit Care Nurs 23: 132-136.
-
Knowles M (2007) The modern practice of adult education. From pedagogy to andragogy. Cambridge Prentice Hall Regents, Englewood Cliffs, NY 07632
-
Schön DA (1987) Educating the reflective practitioner: toward a new design for teaching and learning in the profession. San Francisco: Jossey-Bass.
-
Howell D, Butler L, Vincent L, Watt-Watson J, Stearns N (2000) Influencing nurses' knowledge, attitudes, and practice in cancer pain management. Cancer Nurs 23: 55-63.
-
Flodgren G, Conterno LO, Mayhew A, Omar O, Pereira CR, et al. (2013) Interventions to improve professional adherence to guidelines for prevention of device-related infections. Cochrane Database Syst Rev 3: CD006559.
-
Snoek JW, Minderhoud JM, Wilmink JT (1984) Delayed deterioration following mild head injury in children. Brain 107: 15-36.