Since the supine position worsens obstructive sleep apnea (OSA) by promoting upper airway collapse, patients may avoid supine sleep in order to mitigate its effects. However, the avoidance of supine sleep during polysomnography (PSG) may result in a missed diagnosis of OSA. This study aims to examine the association between the presence/absence of supine sleep and the diagnosis of OSA during PSG.
This cross-sectional analysis of a prospective cohort study analyzed the demographic, anthropometric, and PSG results in 243 patients who underwent PSG for suspected OSA. The crude and adjusted association between the absence/presence of supine sleep and OSA diagnosis during PSG was determined using Pearson Chi-square testing and binary logistic regression model fitting, respectively.
Adult patients suspected of OSA who had no supine sleep during PSG had statistically significant lower odds ratio [crude odds ratio (OR) = 0.26, 95%CI: 0.08, 0.81, p = 0.014] of being diagnosed with OSA compared to those who achieved some supine sleep. This association remained robust despite adjusting for known confounders such as age, BMI, and comorbid coronary heart disease (CHD) [adjusted OR = 0.13, 95%CI: 0.03, 0.48, p = 0.002].
Absence of supine sleep during PSG reduces the odds of an OSA diagnosis, even after adjusting for age, BMI, and CHD. Sleep laboratory policies should consider incorporating protocols that encourage patients to achieve some supine sleep during polysomnography in order to facilitate OSA diagnosis.
Obstructive sleep apnea (OSA) is characterized by complete or partial upper airway obstruction during sleep, resulting in respiratory arousals, sleep fragmentation, and/or oxygen desaturation [1]. OSA is the most common sleep-related breathing disorder, affecting 10-17% of men and 3-9% of women in the United States [2]. Risk factors include obesity, age, male gender, menopause, wide neck circumference, adenotonsillar hypertrophy, and other craniofacial features that cause pharyngeal narrowing [3,4]. The supine position worsens OSA by promoting posterior displacement of the uvula, soft palate and tongue [5-11]. A case-control study found that sleeping in the supine posture doubled the magnitude of the apnea-hypopnea index (AHI) [7]. Up to 56% of 666 Israeli patients with OSA were found to have positional OSA, defined as a lateral respiratory disturbance index (RDI) less than half of the supine RDI [12]. These Israeli patients with positional OSA not only were, on average, two years younger but also had lower body mass index (BMI), less severe RDI, and better sleep than those with non-positional OSA [12]. A retrospective analysis of 3,813 patients who underwent full-night polysomnography (PSG) at a sleep disorders center in Turkey reported an estimated 39.9% prevalence of positional OSA [13]. The patients with positional OSA were described to be younger and have less severe OSA compared to those with non-positional OSA [13]. A retrospective study of 326 US Veterans conducted in two sleep centers in the United States reported a decreasing prevalence of positional OSA with increasing severity of the disease: 49.5% for mild, 19.4% for moderate, and 6.5% for severe OSA [14]. The same investigators also found that patients with more severe OSA tend to spend less time in the supine position during REM sleep than non-REM sleep [15]. The avoidance of the supine position may represent a form of self-treatment to reduce the severity of OSA. A prospective cohort study of 100 consecutive patients found supine-only OSA to be twice as common (23% vs. 10%) and to be associated with a higher AHI than REM-only OSA [16]. George and colleagues suggested that this adverse effect of supine sleep position on the AHI was found to occur only during non-rapid eye movement sleep (NREM) and not during rapid eye movement (REM) sleep [8].
On the other hand, the diagnosis of OSA may be missed if patients avoided the supine position during PSG [14,17,18]. The study of US Veterans also reported that only 33% of patients achieved adequate supine sleep time, defined as > 15 minutes during a full-night PSG, and up to 82.5% failed to do so during a split-night PSG [14]. Sunnergren, et al. study of 265 subjects with clinical hypertension found that 5 out of 81 patients would have been diagnosed with OSA while 16 of 53 patients diagnosed with mild OSA would have been reclassified as moderate or severe if they slept in the supine position [18]. However, it is not known whether sleeping in the supine position during PSG can predict the presence and severity of OSA. It is also unclear how often the avoidance of the supine position occurs during PSG in a general clinical population. Although a supine sleep time > 15 minutes during PSG is suggested [14], no systematic study has been conducted to determine the optimal supine sleep duration for accurate OSA diagnosis. Our hypothesis is that the absence of sleep in the supine position influences the detection of OSA during PSG. Thus, we aimed to examine the association between sleeping in the supine position during PSG and the diagnosis of OSA.
This cross-sectional study was based on data from a prospective cohort study on factors associated with CPAP adherence in adult OSA patients 18 years and older who underwent polysomnography from November 11, 2011 until December 31, 2012 at the SLU Care Sleep Disorders Center at Saint Louis University (SLU). The study was approved by the SLU Institutional Review Board (Protocol ID: 23557, date of approval: September 3, 2013) in accordance with the declaration of Helsinki. The study collected information on demographics, sleep symptoms, co-morbidities, anthropometric measures, polysomnographic findings, and CPAP adherence on patients who underwent clinical evaluation for OSA at our center.
A total of 503 patients who underwent diagnostic polysomnography (PSG) for suspected OSA from November 1, 2011 until December 31, 2012 were screened for eligibility for the study. The inclusion criteria were as follows: (1) Age 18 to 90 years old; (2) Clinical suspicion of OSA; (3) CPAP naïvete; (4) Willingness to use CPAP; and (5) Consent to participate in the study. The exclusion criteria were as follows: (1) Age < 18-years-old; (2) Refusal to use CPAP; (3) Previous or current CPAP use; (4) Self-pay or lack of health insurance preventing use of CPAP; (5) Inability to read, comprehend, or complete research questionnaires. After screening for eligibility based on inclusion and exclusion criteria, a total of 243 participants were included in the sample (Figure 1).
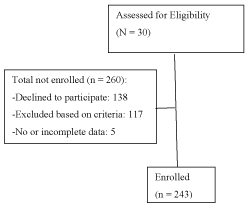 Figure 1: Flow diagram of participants assessed for eligibility and participation in the study. View Figure 1
Figure 1: Flow diagram of participants assessed for eligibility and participation in the study. View Figure 1
All the participants underwent a comprehensive clinical sleep evaluation by their referring academic physicians from the Pulmonary, Neurology, or Psychiatry Clinics, by one of the board-certified sleep medicine specialists (i.e., 1 pulmonologist/intensivist, 1 neurologist, or 1 psychiatrist), or by the collaborating nurse practitioner (a doctor of nurse practice with extensive clinical experience in pulmonary disease/critical care medicine/sleep medicine) at our accredited sleep disorders center prior to being scheduled for PSG at our sleep laboratory. The following parameters were recorded during the in-laboratory diagnostic PSG: electro-oculogram, chin electromyogram, electroencephalogram, anterior tibial muscle electromyogram, electrocardiogram, snore sonogram, oronasal thermistor airflow, pressure transducer airflow, thoracic and abdominal respiratory inductive plethysmogram (RIP), pulse oximetry, and body position via an accelerometer in the (RIP) belt. Audiovisual recording was conducted using a microphone and an infrared camera, which allowed the PSG technologist to visually confirm and manually record the body position. The American Academy of Sleep Medicine (AASM) Scoring Manual version 1.0 was used to stage sleep and to score respiratory events [19]. An apnea was defined as complete cessation breathing for at least 10 seconds. The apnea was considered obstructive or central depending on whether it was accompanied by persistent thoracic and/or abdominal respiratory effort. A hypoponea required a ≥ 30% reduction in airflow accompanied by a ≥ 4% oxygen desaturation. Respiratory effort-related arousals were scored but were not included in the analysis. As per our sleep laboratory protocol, a patient was allowed to start sleeping in his/her preferred position during the diagnostic PSG. The patients were not informed about the need to sleep in the supine position prior to the sleep study. However, if the patient had been sleeping entirely in the nonsupine (lateral or prone) position and had not exhibited any abnormal respiratory events during the first half of the night, the PSG technologists would enter the patient's the room and would gently encourage him/her to sleep in the supine position. If by 3 am the patient's AHI was at least 20/hr based on at least 2 hours of sleep, the sleep study was split, and a CPAP therapeutic trial was conducted. Sleep studies were scored by registered PSG technologists and reviewed and rescored by board-certified sleep medicine specialists as appropriate.
The exposure variable was the absence or presence of supine sleep during the diagnostic PSG. Absence of supine sleep was defined as time spent in the supine sleep = 0 while presence of supine sleep was defined as any supine sleep time > 0. The time spent in supine sleep was measured both in duration (minutes) and as a percentage of total sleep time. The outcome variable was the diagnosis of OSA based on the AHI. Since all of the patients referred to our institution were clinically suspected of having OSA by their referring physicians based on neurocognitive dysfunction (e.g., sleepiness, fatigue, insomnia etc.), mood disorders (e.g., depression), cardiovascular disorders [i.e., systemic hypertension, congestive heart failure, coronary heart disease (CHD), stroke, etc.], the diagnostic cut-off for OSA was set at an AHI ≥ 5 events per hour of sleep based on at least 2 hours of PSG-recorded sleep. Potential confounding variables were based on known risk factors for OSA, including age, body mass index (BMI), and cardiovascular comorbidity [3,20,21]. The age, BMI, and history of systemic hypertension, CHD, stroke, etc. were abstracted from medical records, including the most recent sleep disorders clinic visit note prior to the sleep study. Although other cardiovascular disorders such as systemic hypertension and stroke were ascertained in this study, only CHD was selected as the marker for cardiovascular comorbidity in order to avoid collinearity.
Continuous or interval baseline demographic, anthropometric, clinical, and polysomnographic variables were compared between the exposure groups (i.e., supine sleep absent vs. present) using t-tests. The association between baseline categorical independent variables and the absence/presence of supine sleep was analyzed using Pearson Chi-square test. Binary logistic regression analysis was performed to estimate the odds ratio (OR) and the corresponding 95% Confidence intervals (95% CI) for the association between the absence of supine sleep and the diagnosis of OSA, after adjusting for potential confounders including age, BMI, and CHD. The best fitting binary logistic regression model was selected based on the -2 log likelihood differences or deviance χ2 statistic. Given our two-tailed hypothesis, we chose an α < 0.05 as cut-off for statistical significance.
The cohort had a mean age of 48.7 ± 13.2 years and were predominantly male (56%), Caucasian (53%) or African-American (40%), and overweight or obese (mean BMI = 35.4 ± 8.2) (Table 1). OSA symptoms were common including snoring (79%), witnessed breathing pauses during sleep (43%), sleepiness (mean Epworth Sleepiness Scale Score = 16.2 ± 1.8), and fatigue (38.3 ± 14.4) (Table 1). Given that the participants were recruited from a clinical population, there was a high prevalence of cardiovascular and pulmonary comorbidities and recreational substance use (Table 1). The cohort had a mean AHI of 17.0 ± 21.5 per hour of sleep, predominantly obstructive, with an average minimum oxygen saturation (minSpO2) of 83.6 ± 7.5%. The 47 patients who underwent split-night PSG had an AHI of 39.1 ± 26.5 per hour during the diagnostic portion of the study while the 186 patients who underwent a full-night diagnostic PSG had an AHI of 10.4 ± 14.2 per hour. Sleep position as a percentage of total sleep time during PSG was predominantly lateral (56.1 ± 27.9%), followed by supine (41.0 ± 28.0%) and prone (2.5 ± 8.9%) (Table 2).
Table 1: Demographic, anthropometric, and clinical characteristics of all participants. View Table 1
Table 2: Diagnostic polysomnographic characteristics of participants (N = 243). View Table 2
As expected per our protocol, the vast majority (94.6%) of our patients achieved supine sleep while 5.4% did not. There were no statistically significant differences in the age, gender or race distribution, BMI, neck circumference, prevalence of snoring, and Epworth Sleepiness Scale or Fatigue Severity Scale scores between participants who had no supine sleep and those who did (Table 3). Aside from the percentage of time spent in the supine and lateral positions, there were also no statistically significant differences in sleep architecture, frequency of sleep-disordered breathing events, and SpO2 between the 2 groups (Table 4).
Table 3: Demographic, anthropometric, and clinical characteristics based on occurrence of supine sleep. View Table 3
Table 4: Diagnostic polysomnographic characteristics of participants categorized based on occurrence of supine sleep. View Table 4
The absence of supine sleep during a PSG was associated with a reduced prevalence of an OSA diagnosis when compared to having any supine sleep. OSA was present in 46% (6/13) of patients who had no supine sleep compared to 76% (176/230) of patients who had supine sleep during a PSG. In patients diagnosed with OSA, bivariate analysis revealed a statistically significant negative association between the absence of supine sleep and the diagnosis of OSA [odds ratio (OR) = 0.26, 95%CI: 0.08, 0.81]. This unadjusted model means that the absence of supine sleep during a diagnostic PSG decreased the odds of detecting OSA by 74% when compared to having any supine sleep during PSG. Several multivariable logistic regression models were fitted, starting with a full model predicting OSA based on the absence of supine sleep and adjusting for potential confounders (i.e., age, BMI, and presence of CHD). Based on the analysis of the -2 log likelihood or deviance differences, the binary logistic regression model which includes absence/presence of supine sleep, age, and BMI, but not CHD, as covariates was the best fitting model (Table 5). The presence of CHD was not a confounder since excluding it from the full model did not result in a statistically significant -2 log likelihood or deviance difference statistic and its Wald χ2 statistic was also not statistically significant (β = -0.268, Wald χ2 = 0.315, df = 1, p = 0.574). This means that the absence of supine sleep during PSG is associated with an 86.3% reduction in the odds of having OSA when compared to having any supine sleep after controlling for age and BMI (Table 5). Age (β = 0.035, Wald χ2 = 7.347, df = 1, p = 0.007) and BMI (β = 0.068, Wald χ2 = 10.151, df = 1, p = 0.001) were statistically significant covariates based on the Wald statistics (Table 5).
Table 5: Multivariable binary logistic regression model predicting obstructive sleep apnea based on absence of supine sleep. View Table 5
This prospective cross-sectional study found a statistically significant relationship between the absence/presence of supine sleep during PSG and the diagnosis of OSA. In patients diagnosed with OSA, bivariate analysis revealed a statistically significant inverse association between the absence of supine sleep and the diagnosis of OSA [OR = 0.26, 95%CI: 0.08, 0.81]. Conversely, adult patients suspected of OSA who achieved supine sleep during their diagnostic PSG, as opposed to none, increased the crude odds of being diagnosed with OSA diagnosis 3.8-fold. This association remained robust despite adjusting for known confounders such as age and BMI in binary logistic regression models. Our finding that supine sleep increased the crude and adjusted odds of diagnosing OSA supports our sleep laboratory policy of requiring technologists to encourage patient to achieve some supine sleep during PSG. In fact, an overwhelming majority (95%) of our patients achieved some supine sleep due to this policy. Our findings also corroborate Sunnergren's concern that the absence of supine sleep may underdiagnose the presence of OSA [18]. On the other hand, supine sleep has also been shown to increase risk for central sleep apnea-Cheyne Stokes respiration [22] and treatment-emergent central sleep apnea (TECSA) [23]. A higher baseline central apnea index, especially during NREM supine sleep during the diagnostic study, increased the likelihood for the appearance of TECSA during a subsequent CPAP therapeutic titration [23]. Since we were unable to analyze the association between the different supine sleep duration cut-offs (e.g., 0, 5, 10, 15, 30 minutes) and OSA diagnosis due to sample size limitations, future studies should determine the optimal supine sleep duration required for accurate OSA diagnosis. Although our findings may still require confirmation with larger studies, it is prudent to recommend that sleep laboratory policies should include a protocol for encouraging patients to achieve supine sleep during PSG in order to enhance diagnostic efficiency and facilitate the subsequent treatment of OSA.
Age and BMI were statistically significant covariates in our best fitting multivariate logistic regression, but the presence of CHD was not. The Sleep Heart Health Study published in 2002 was the largest population-based US study that described the linear relationship between BMI and OSA severity [3]. Since then multiple randomized controlled trials employing medical and surgical weight loss strategies have confirmed this linear relationship between BMI and OSA [24,25]. Age, a known risk factor for OSA, can promote airway collapse by reducing the oropharyngeal dilator muscle tone. Several experimental studies have demonstrated the effect of aging on upper airway collapsibility [26-31]. Ray and colleagues studied Fischer 344 rats and reported that aging-related upper airway collapsibility was likely related to alteration in neural control rather than muscular function [26]. Seebart, et al. reported reduced serotonin (5HT) levels with compensatory upregulation of serotonin 2A receptors in the hypoglossal nucleus of aging rats [27]. On the other hand, Kaneko and his group demonstrated a reduction in myosin heavy chain mRNA expression and a transition from fast to slow myofiber phenotype in the genioglossus muscles of aging rats [28]. Hodges, et al. also described remodeling of the genioglossus myoneural junctions in aging rats [29]. Aging appeared to reduce the oxidative capacity of the upper airway muscles in aging Wistar rats [30]. A study of age-related upper airway muscle function in human subjects demonstrated a greater reduction in electromyographic activity of the genioglossus and tensor palatine muscles in older vs. younger men [31]. A study of 10 healthy human subjects also found a reduced hypoxia response of the genioglossus muscles in the older subjects [31]. Despite controlling for these strong confounders, BMI and age, our multivariate logistic regression model still found a robust association between the absence/presence of supine sleep and OSA diagnosis. We suspect that this robust association between the supine body position may be related to the significant pull of gravity on the soft palate and tongue in the recumbent position, resulting in retropalatal and/or retrolingual space obliteration independent of the effects of advanced age and obesity on the upper airway muscle tone and caliber.
The strengths of our study include the collection of objective PSG parameters for our exposure and outcome variables and the inclusion of clinically significant confounders in our logistic models. On the other hand, despite the statistically significant results, the main limitation of our study is the potential for information bias resulting from our sleep laboratory protocol requiring our technologist to ensure that supine sleep occur during PSG. Although the patients were allowed to sleep in their preferred position initially, our PSG technologists had been instructed to encourage patients to switch to the supine position if the patients had been sleeping entirely in the lateral position, particularly if the AHI was still within normal limits (i.e., AHI < 5/hr) during the first half of the night. This policy of encouraging supine sleep would have reduced the number of patients in our sample with no supine sleep and would have altered the expected distribution and variability of the duration of supine sleep. The application of this policy might also have varied depending on the patient's OSA severity and caused a differential misclassification of exposure based on disease severity, a type of information or measurement bias. For example, patients with severe OSA might not have been encouraged to sleep on their backs since they already had an elevated AHI even when sleeping on their side, thereby attenuating their disease severity. On the other hand, patients with only positional or mild OSA might have been encouraged to sleep in the supine position, thereby augmenting their AHI. Allowing patients to choose their preferred sleep position/s during a full-night sleep PSG would have eliminated this concern but this would be contrary to optimizing the diagnostic efficiency of PSG in clinical practice. Home sleep apnea testing (HSAT), which allows patients to sleep in their preferred position/s, might be an alternative approach to addressing this research question. Another limitation of our study is selection bias, since we recruited our participants from a clinical population rather than from a community-based population, which may limit the generalizability of our findings. We suspect that our sample of middle-aged, obese adults with a high prevalence of comorbid cardiopulmonary diseases and a high likelihood of OSA would have overestimated the association between supine sleep and OSA diagnosis. Although our findings cannot be applied to the general population, they may still be applicable to similar clinical populations with comorbidities and risk factors for OSA. Since the occurrence of supine sleep and the diagnosis of OSA were ascertained at the time during PSG, we cannot establish a causal relationship between the exposure and the outcome (temporal bias). Our arbitrary cut-off time 3 am for splitting the PSG might have influenced the sleep architecture, i.e., the percentage of REM sleep, as well as the success of a CPAP titration, particularly in older adults with advanced sleep phase syndrome who might not have been able to sleep later than this time. Tailoring the cut-off time for splitting based on patient-related circadian rhythm patterns may prove to be more appropriate in ensuring all sleep stages are achieved by the patient during both the diagnostic and therapeutic portions of the split-night PSG. And finally, although we tried to control for confounders, residual confounding is very likely since we were only able to explain approximately 15% of the variance of the outcome. Potential confounders not measured in this retrospective study may include alcohol consumption, tobacco smoking, previous upper airway surgery, neck position and head/trunk elevation during PSG. A prospective, randomized, cross-over study will help address the above limitations through the ascertainment of unmeasured potential confounders and the comparison of the likelihood of an OSA diagnosis between supine present vs. absent polysomnographic conditions in the same cohort of patients.
In clinically referred patients suspected of OSA, the absence of supine sleep during PSG significantly reduced the odds of an OSA diagnosis, even after adjusting for age, BMI, and CHD. Sleep laboratory policies should consider incorporating protocols that encourage patients to achieve some supine sleep during polysomnography in order to facilitate OSA diagnosis.