The global healthcare has been challenged to provide adequate care during COVID 19 pandemic [1]. There is increased public anxiety and knowledge gaps that have created major dilemmas in health care delivery. In this situation a "don't miss" diagnosis of Covid-19 is unacceptable and there is a trend to suspect respiratory illness as COVID disease unless proved otherwise. We present one of mimics of Covid pneumonia. EVALI (E- cigarettes and vaping associated acute lung injury) is caused by aerosolization of content of E- cigarettes e.g. vitamin E acetate, coconut oil and limonene [2]. COVID-19 is transmitted through respiratory droplets and Aerosols [3]. It is unknown if vaping puts patients at higher risk of respiratory failure if co-infected with COVID-19. Therefore, exposure history in patients with clinical findings of pneumonia-like syndrome is important.
EVALI, COVID-19
31-year-old male with history of Crohn's disease presented with fever, fatigue, dry cough and dyspnea at rest for 4 days. Medications included infliximab every 6 weeks with last dose one month prior to admission. He had temperature of 102 F, tachycardia with Spo2 of 86% on room air. Auscultation revealed bilateral basal crepitation on auscultation. Arterial blood gas showed PO2 of 48 on room air, wide A-a gradient and respiratory alkalosis. Chest radiograph (Figure 1) demonstrated faint bilateral pulmonary interstitial opacities. Transthoracic echo was normal. Contrasted CT chest (Figure 2 and Figure 3) showed diffuse ground glass opacities. Patient was suspected to have COVID 19 pneumonia and placed in negative pressure isolation. Influenza A and B antigen, sputum and blood cultures, urine legionella and streptococcus, serum histoplasma and cryptococcal antigens were negative. Reverse transcriptase PCR testing for COVID-19 was negative on day 1 and day 3. He remained on high flow oxygen. Further workup was initiated. Serum beta-D- glucan was negative. Serum ACE was 35 (N 16-85 U/L). Serum BNP was 30 pg/ml (N 6-100 pg/ml). Serum LDH was 366 U/L (N 140- 271 U/L). HIV 1 and 2 antibody screen was negative. Rheumatoid factor, anti-dsDNA, anti Jo-1, anti Scl-70, anti-Smith, SSA 52 and 60, SSB, anti-chromatin antibodies were negative. Procalcitonin was < 0.10 ng/ml (N ≤ 0.15 ng/ml).
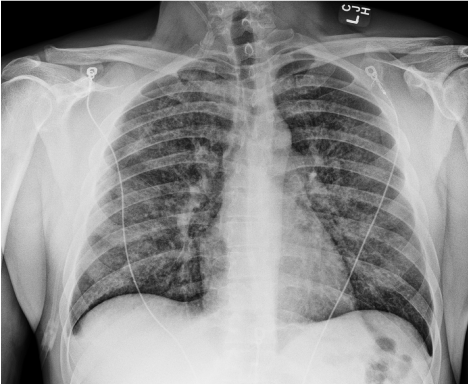 Figure 1: Chest x-ray showing faint bilateral pulmonary interstitial opacities.
View Figure 1
Figure 1: Chest x-ray showing faint bilateral pulmonary interstitial opacities.
View Figure 1
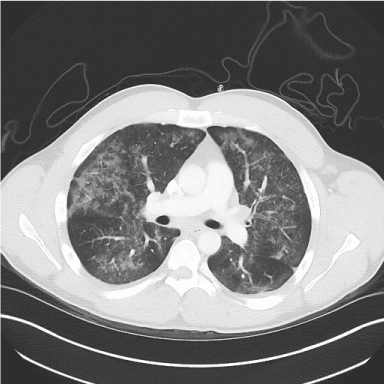 Figure 2: Axial and coronal CT scan of the chest demonstrate diffuse pattern of ground glass opacities without Consolidation or interlobular septal thickening.
View Figure 2
Figure 2: Axial and coronal CT scan of the chest demonstrate diffuse pattern of ground glass opacities without Consolidation or interlobular septal thickening.
View Figure 2
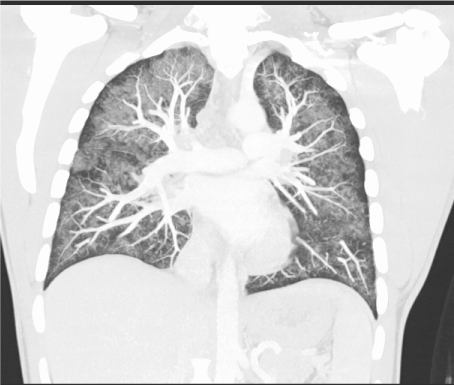 Figure 3: No pleural effusion.
View Figure 3
Figure 3: No pleural effusion.
View Figure 3
On further exploration, patient reported binging disposable Juul pods, vaping nicotine (40-50 hits/day), tetrahydrocannabinol (140-150 hits/day), and cannabidiol. He attributed this to anxiety from stay-at-home orders. A diagnosis of EVALI was made. Patient developed significant clinical and radiographic improvement (CXR, Figure 4) in one week as he stopped vaping and finished one week course of oral steroids.
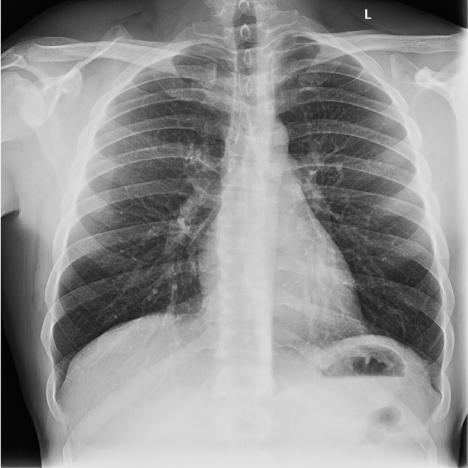 Figure 4: Chest x-ray frontal view showing improvement in hazy ground glass opacities in both lungs.
View Figure 1
Figure 4: Chest x-ray frontal view showing improvement in hazy ground glass opacities in both lungs.
View Figure 1
COVID 19 pneumonia and EVALI are aerosol associated acute lung injuries with similar respiratory symptoms and radiographic findings. Covid pneumonia is an infectious disease where as EVALI is non-infectious agents that can cause acute respiratory failure and acute lung injury. These and some striking difference between the two illnesses (Table 1). Electronic cigarettes (E-CIGs) and Electronic nicotine delivery systems (ENDS) gained popularity in young adults to the point of reaching epidemic levels in 2018-2019 [4]. Since February 2020, CDC has reported a total of 2807 hospitalized cases/deaths by EVALI [5,6]. COVID-19 pandemic as of 5th May 2020, has infected 1,171,510 cases in U.S.A with 68,279 deaths [7]. There are reports of progression to Covid pneumonia in smokers [8], but there is paucity of data on association between vaping rates and COVID-19 rates. Although, there is a decline in incidence of EVALI, but to eradicate the disease Public health awareness is needed.
Table 1: Comparison between EVALI and COVID-19. View Table 1
EVALI is a diagnosis of exclusion and does not have a single confirmatory test. In EVALI, lab findings include nonspecific elevation of Leukocyte count, Erythrocyte sedimentation rate and Liver enzymes [9]. Elevated liver enzymes and inflammatory markers can also be seen in COVID-19. However, lymphopenia is more common in COVID-19 than EVALI [3]. COVID-19 is diagnosed by reverse transcription polymerase chain reaction on respiratory tract specimens [3].
EVALI presents with patterns of basilar- predominant consolidation and ground-glass opacity with areas of lobular or subpleural sparing on CT scan. Sometimes there may be findings of rapidly developing acute lung injuries including acute eosinophilic pneumonia and diffuse alveolar damage [2]. In contrast, COVID-19 has varied imaging findings. In early disease, inflammatory infiltrates may be found in subpleural or peribronchovascular regions. With advanced illness, ground glass opacities, crazy paving pattern and consolidation in bilateral lobes are common findings can be seen [2,10]. Histopathologic findings in EVALI may include Foamy Macrophages, Acute Fibrinous Pneumonitis, Diffuse alveolar injury, or Organizing Pneumonia [11]. Histopathologic characteristics in COVID- 19 disease on nonspecific and include Inflammatory changes, vascular congestion, proteinaceous exudates and findings of diffuse alveolar damage [12]. Microscopic findings may include viral infection changes multinucleated enlarged pneumocytes with large nuclei, amphophilic cytoplasm and prominent nucleoli in alveolar spaces [13].
There is significant overlap in acute lung injury presentation due to COVID-19 and EVALI ranging from completely asymptomatic, radiographic abnormalities to severe respiratory failure and multiorgan dysfunction. EVALI is a diagnosis of exclusion. High suspicion of index and an eye for detail in history taking is crucial in prompt recognition and timely management.
Informed consent from patient was obtained; No Conflicts of Interests; All 4 authors contributed equally in case report.