Tracheostomy is a common procedure in long-term ventilated patients and frequent in those with severe stroke. Decannulation not only involves removal of the tracheostomy cannula, but also evaluation of upper airway protection. The predictors of success provide an objective guide to minimize the time of permanence of the same. Currently there are no studies on predictors of decannulation success in neurocritical patients.
To analyze clinical and demographic data in a cohort of tracheostomized neurocritical adults in the Intensive Care Unit over a period of 9 months. Secondarily, to compare decannulated and non-decannulated patients to identify variables associated with decannulation success.
We have analyzed the data of adult neurocritical tracheostomized patients during a stay in the Intensive Care Unit.
≥ 18 years, neurocritical tracheostomized patients.
Epidemiological data and personal antecedents, clinical follow-up variables: tracheostomy indication, tracheostomy timing, success of weaning, days of mechanical ventilation, success of decannulation, stay in Intensive Care Unit and ward, condition to discharge.
Prospective cohort study. Many of 32 patients were analyzed. Most frequent reason for admission was subarachnoid hemorrhage. The suspicion of prolonged weaning was the main criteria to perform a tracheostomy. Decannulation rate was 25%.
When comparing decannulated/non-decannulated patients, statistically significant differences were found in age (p = 0.037), tracheostomy timing (p = 0.001), tracheostomy motive: suspicion of prolonged weaning (p = 0.004) and prolonged mechanical ventilation (p = 0.009); Successful weaning (100% vs. 54% respectively p = 0.029) and discharge condition.
When analyzing clinical and demographic data, a greater percentage of females and subarachnoid hemorrhage was observed as a reason for more frequent admission. Both the suspicion of prolonged weaning and the prolonged mechanical ventilation were predominant causes of tracheostomy. The 66% of the tracheostomies were successfully removed; Decannulation rate was of 25%. When comparing decannulated and non-decannulated patients, significant differences were found in age, timing and reasons for tracheostomy, success in weaning, and condition at discharge. In those patients with successful decannulation, younger age, greater timing of tracheostomy and prolonged mechanical ventilation were observed as a reason for predominant tracheostomy.
Stroke, Aneurysmal subarachnoid hemorrhage, Decannulation, Weaning, Tracheostomy, Critical care
Patients with acute and pre-existing neurological disorders may develop altered consciousness or acute respiratory failure requiring orotracheal intubation (OTI) and mechanical ventilation in neurocritical care units. In those with acute vascular disease requiring intubation, in-hospital mortality is approximately 50% [1,2]. In neurocritical units, an increase in reintubation rates, pneumonia, tracheostomy (TQT) and prolonged mechanical ventilation (PMV) was reported [3,4]. The rate of failure of extubation varies from 5 to 20%, depending on the population studied, and has been associated with a prolonged stay in the intensive care unit (ICU) and hospital, as well as higher rates of TQT and mortality. In patients with traumatic brain injury, the failure of extubation lengthens hospital stay, increases the frequency of TQT, pulmonary complications and increases morbidity and mortality [5]. Cerebral dysfunction can contribute to the failure of extubation for various reasons, such as decreased patient's ability to protect the airway and eliminate secretions [2]. Both delay and early extubation increase the rate of complications, the need for TQT, the stay in the ICU and mortality [6].
One of the challenges in the management of the neurocritical patient in mechanical ventilatory assistance (MVA) continues to be the identification of those patients who are more likely to require long-term ventilatory support, and the determination of the optimal moment to perform TQT [2]. Mayor, et al. [7] suggest the use of objective scales such as the glasgow coma scale (GCS) daily assessment, among others; scores less than 7 had a high positive predictive value on the fourth day to identify patients who required TQT for airway protection. Similarly, Namen, et al. [4] found that a GCS score less than 8 was associated with a higher probability of extubation failure in neurosurgical patients. Coplin, et al. [8], however, found no relationship between the failure of the extubation and the GCS score [2].
Although TQT is a common procedure in long-term ventilated patients in the ICU and frequent in patients with severe cerebrovascular accident (CVA), the optimal timing of TQT is still unknown, and the impact of its realization is controversial [9]. The obstruction of the upper airway, the failure in the release of the MVA and the debilitating neurological conditions are only one of the few indications for the realization of the TQT. A percutaneous approach offers a lower number of surgical site infections and postoperative bleeding than a surgical approach. Late complications for both procedures are stenosis, tracheomalacia, followed by tracheo-esophageal, tracheo-innominate and tracheo-cutaneous fistula [10].
The prognosis of patients with CVA who require a stay in the ICU and MVA is generally poor, with reported mortality rates ranging between 40 and 80%. It is not clear whether patients ventilated with ischemic or hemorrhagic stroke should be tracheostomized. Although the benefits of early TQT, such as reduction of hospital stay, reduction of duration of MVA, and eventual reduction of mortality, have been demonstrated by small randomized trials in certain subgroups of non-neurological patients, this It has not yet been systematically investigated in patients with CVA in neurocritical care [9].
Early TQT in patients with CVA ventilated in ICU is feasible and safe, and presumably reduces the need for sedation, the incidence of pneumonia associated with mechanical ventilation, hospital stay and costs. The benefits in mortality should be determined by a large multicenter clinical trial [11,12].
The removal of the tracheal cannula is also an important objective in the rehabilitation of tracheostomized patients to achieve the progressive independence of mechanical ventilatory support and reduce the risk of respiratory complications [13]. Decannulation not only involves removal of the TQT cannula, but also evaluation of permeability and protection of the upper airway [14]. Several predictors of decannulation success have been described, such as the amount of secretions, the ability to produce vigorous cough [15], maximum expiratory pressure (Pemax) > 40 cm H2O [16], peak expiratory flow (PEF) < 160 L/min [17] and the state of consciousness [8,14] among others. These predictors provide an objective guide to minimize the length of stay of the TQT.
The relationship between PEF and the result of decannulation was studied by Bach and Saporito [17] in 1996. These authors determined that the cut-off point of decannulation success was 160 L/min. This study was developed in a population of patients with neuromuscular alterations, with maximal insufflation maneuver and with cough help techniques. On the other hand, Chan, et al. [18] evaluated the PEF induced as decannulation success, measured by TQT with deflated balloon, and described as a cutoff point a value > 29 L/min. The state of consciousness is considered a predictive factor for both extubation and decannulation success [4,8,14,19,20].
Currently, there are no studies on decannulation predictors in neurocritical patients available in the available literature, so the objective of this study is to analyze the clinical and demographic data in a cohort of adult neurocritical tracheostomized patients in the Intensive Care Unit for a period of 9 months and, secondarily, to compare decanulated and non-decanulated patients to identify variables associated with decannulation success.
Prospective cohort study.
We recruited prospectively and consecutively the data of adult neurocritical tracheostomized patients during the stay in the ICU of a center specialized in neurovascular patients in a period of 9 months (June 2014 - February 2015). Inclusion criteria: patients ≥ 18 years old, neurocritical, tracheostomized during the stay in our ICU. Those patients who had a disease that affects the central nervous system and that requires intensive care of high complexity were considered as neurocritical patients.
Patients with known swallowing disorders, neuromuscular and/or neurodegenerative diseases prior to admission were excluded. The data of patients who died within 48 hours were eliminated for the analysis. of the TQT. After the recruitment, the patients were followed up for a period of 4 months and then the data were analyzed.
The analyzed variables were: epidemiological data (gender, age, date of admission, reason for admission, Charlson Score, admission GCS), and pathological antecedents prior to admission. Clinical follow-up variables: TQT reason, OTI days until TQT, successful MVA disengagement, MVA days, decannulation success, ICU stay, nosocomial stay and discharge condition. In decannulated patients, GCS was also analyzed prior to decannulation, PEF, Pemax, days of TQT, and decannulation failure.
The informed consent was signed by the family member in charge and the study was approved by the Teaching and Research Committee of our institution.
In the patients who were included in the study, the epidemiological data were recorded, antecedents to the hospitalization, the Charlson Score 21 was scored from 0 to ≥ 8, granting zero to the absence of comorbidities (Appendix 1), the GCS of admission was scored on 15 (6 motor, 5 verbal, 4 ocular).
The success of MVA decoupling was recorded, considered in those patients who did not require ventilatory support for at least 48 hours. and the days of MVA were quantified from the OTI until the last night with MVA.
The reason for TQT was classified into 5 categories: suspicion of prolonged weaning (those patients whose clinical condition suggests that they may have prolonged weaning), prolonged weaning (more than 3 attempts and/or more than 7 days from the first test), 22 prolonged MVA (more than 21 days of MVA), failed extubation (need for reintubation within 48 hours of extubation), suspicion of prolonged MVA (those patients whose clinical condition, such as vasospasm or convulsive status, among others) infers that they will continue in MVA for a long time). The timing of TQT was also recorded by quantifying the days elapsed from the OTI to the TQT procedure.
In the patients who were in clinical conditions, the decannulation protocol of the institution was implemented (Appendix 2). And in those who achieved decannulation, the same day of the procedure, the GCS was measured (considering its score over 15 and giving 1 point for verbal), the PEF (the patient was measured 90 degrees spontaneously, after carrying out an air-stacking maneuver and with air stacking plus the assistance maneuver of the cough with thoracoabdominal compression, registering the highest value) [17], and the Pemax was measured by mouth with a unidirectional valve for 40 seconds and were taken 3 measurements registering the highest value.
The days of TQT were also recorded, considered as the time in days elapsed from the TQT procedure until the time of decannulation.
To patients who presented, after the procedure of removal of the TQT cannula, respiratory rate > 35 rpm, thoraco-abdominal paradox, poor management of secretions (requirement of nasotracheal aspiration more than 3 times per day), agitation, diaphoresis, signs of obstruction of upper airway and/or by medical decision, the re-cannulation was carried out consigning the data and reason for the failure. The decannulation success considered in those patients who did not require re-cannulation within 72 hours of withdrawal the TQT was also recorded.
The condition of discharge was recorded: death, domicile, rehabilitation center or continued hospitalization upon completion of the months of follow-up. The number of days from the admission to the ICU up to the discharge/death was quantified for the nosocomial stay. And for the stay in ICU, the number of days from admission to the ICU until the transfer to another sector, referral or death.
The qualitative variables were expressed as absolute values, percentages and 95% confidence intervals for the entire sample. The distribution of the continuous variables was analyzed with the Kolmogorov-Smirnov test, and they were expressed as medians and percentiles of 25 and 75%. The comparison of the categorical variables was performed with the chi2 test or Fisher's exact probability test, as appropriate. For the categorical data, the relative risk (RR) and its corresponding 95% confidence interval (95% CI) were also calculated. To compare the continuous variables, the nonparametric Mann-Whitney U test was used. All tests were performed for two tails, and a significance threshold of 0.05 was considered. The statistical package SPSS Statistics 17.0MR and the StatCalc function of Epi Info 7MR were used.
Out of a total of 38 patients, 35 patients were included; 3 patients were eliminated from the analysis due to death within the first 48 hours. of performed the tracheostomy. Data from 32 patients were analyzed (Figure 1). In the patients analyzed, the median age was 70 years old, and 66% were women. The most frequent reason for admission was subarachnoid hemorrhage (SAH) (47%) followed by ischemic stroke (38%). The median GCS of admission was 7 points.
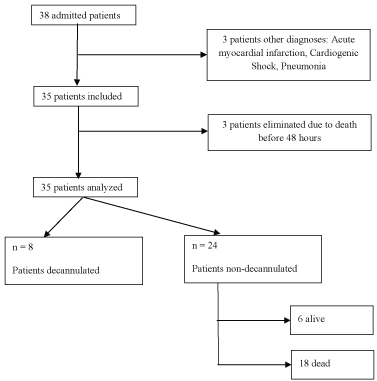 Figure 1: Flow chart.
View Figure 1
Figure 1: Flow chart.
View Figure 1
Among the reasons for tracheostomy the most frequent was the suspicion of prolonged weaning (41%), followed by suspicion of prolonged MVA (22%). 66% of neurocritical tracheostomized patients were successfully disengaged and the decannulation rate was 25% (Table 1).
Table 1: Clinical and demographic characteristics of the general population (n = 32). View Table 1
When comparing decannulated patients with non-decannulated patients, statistically significant differences were found in median age (71.5 years not decannulated versus 61.5 years cannulated (p = 0.037)); no statistically significant differences were found for pathological antecedents as well as for the reason for admission. The most frequent reason for admission among decannulated patients was subarachnoid hemorrhage (Fisher III or IV) while among the non-decannulated was ischemic stroke. Both the Charlson score and the GCS of admission were similar in both groups (median of 3 and 7 points respectively). Statistically significant differences were found in the median timing of TQT (20 days of cannulated vs. 12 non-decannulated days, p = 0.001).
When carrying out the p-joint analysis, statistically significant differences were observed in the TQT criteria and when performing the analysis individually, in suspicion of prolonged weaning (57% not decannulated versus 0% decannulated p = 0.004) and prolonged MVA (50% decannulated versus 4% not decannulated p = 0.009, RR = 12.00).
Statistically significant differences were also found in the success of decoupling was 100% in decannulated patients and 54% in non-decannulated patients (p = 0.029, RR = 1.85), without differences in hospital and nosocomial stay (the median nosocomial stay was 105 days in decannulated patients versus 47 days in non-decannulated patients). On the other hand, the number of non-decannulated patients alive was 108 days. With respect to the condition of discharge in the group of non-decannulated deaths predominated while among the patients decannulates was more frequent home delivery (57%) followed by rehabilitation center (43%). None of the decannulated patients died during the follow-up period. Statistically significant differences were found in the condition of discharge for both home discharge in favor of decannulated patients (p = 0.0003) and death for non-decannulated patients (p = 0.0003). (Table 2).
Table 2: Comparison of clinical and demographic variables: Decannulated/non-decannulated. View Table 2
In decannulated patients, the median GCS prior to decannulation was 14.5 points with a median PFT of 210 L/min. The decannulation success was 100% (Table 3).
Table 3: Clinical data prior to decannulation (n = 8). View Table 3
TQT is a frequent procedure in neurocritical patients with the purpose of facilitating the adequate management of the airway. The optimal time to perform the TQT is not yet clear, but its practice is common in critical care either percutaneously or surgically, after 2 to 3 weeks of the OTI after the failure of weaning or failed attempts of extubation [21,22]. Regarding neurocritical patients, there are some studies of subgroups in mixed populations or in patients with head trauma, many of them in favor of early TQT. But it has never been approached prospectively in patients with non-traumatic brain diseases, mainly stroke [9].
Gandía-Martínez, et al. [23] have analyzed the early TQT (≤ 9 days) versus late TQT (> 9 days) in neurocritical patients. They have found that those neurocritics admitted to the ICU requiring TQT (subarachnoid hemorrhage and ischemic stroke) in the first 9 days of OTI shortened the MVA time and the consequent need for sedation, decreases the frequency of pneumonia by shortening the antimicrobial treatments, and decreases the stay in the ICU without modifying the duration of the hospital stay or the mortality in ICU or hospital.
Rizk, et al. [24] have reported the effects of TQT timing after severe brain injury, suggesting that an early TQT strategy (< 7 days), particularly when performed in patients with a reasonable chance of survival, gives a better overall clinical result (fewer adverse events), shortens the stay, and a greater probability of functional independence) than when the TQT is performed late (> 7 days). These results are also influenced by the severity of the injury.
In contrast to the results of other authors [7,25,26], in our series, the tracheostomized neurocritical patients were preferably women (66%). The nosocomial mortality was 58%, higher than expected in neurocritics, possibly due to the predominance of non-traumatic cerebral pathology, to the acute or subacute state of the same and, on the other hand, to the advanced age of the sample (median of 70 years), which was considerably greater than that found in the available literature.
The median timing of TQT was 15 days, finding statistically significant differences between decannulated and non-decannulated patients, this being greater in the first group possibly influenced by the patient's clinical condition that allowed to infer the possibility of extubation, so that extended the term of MVA. Despite the prolonged timing of TQT of the decannulated patients, no major complications were observed.
At present, there are no definitive data or recommendations to determine the optimal time to perform TQT in different groups of patients with ventilatory assistance, including the neurocritical population.
The patients who could not be decannulated were older, the ischemic stroke was the main reason for admission, and the suspicion of prolonged weaning was the reason for TQT. Half of the patients could not be dissociated from AVM. Possibly these results were obtained in the patients who continued with a TQT cannula because of the severity of the lesion, its extension and location, although we did not consider these variables for the analysis.
We consider as limitations of the present study the fact of having been performed in a single institution, with a small number of patients included, so many of the variables did not yield conclusive results, and not including variables in relation to the patient's functional status at nosocomial discharge.
In spite of the relevance and importance of decannulation, there is no universally accepted protocol for its performance. Variability in existing algorithms [16], non-randomized study design [27] and ambiguity in the screening, technique and monitoring of decannulation limits our understanding in this important area of care. Singh, et al. [28], have recently performed a systematic review of the process of decannulation. From 1995 until 2016 they have finally included 18 studies. There were no randomized controlled studies. All were single centre studies and only a few were performed in neurological ill patients. Decannulation process was more often individualized than protocolized. Singh, et al. conclusion is that universally accepted protocol is needed for better standardization.
When analyzing the clinical and demographic data in a cohort of adult neurocritical patients tracheostomized in the ICU, a higher percentage of females was observed, and the subarachnoid hemorrhage was the most frequent reason for admission. Both the suspicion of prolonged weaning and that of prolonged MVA were the predominant reasons for TQT. 66% of tracheostomized patients were successfully dissociated, with a decannulation rate of 25%.
When comparing decannulated and non-decannulated, significant differences were found in age, timing and reasons for TQT (suspicion of prolonged weaning and prolonged MVA), the success of disengagement, and condition at discharge. In those patients with successful decannulation, a younger age, a greater timing of TQT and prolonged MVA were observed as a reason for predominant TQT.
The analysis of these associated variables could be considered in a future study, to identify predictors of decannulation success. Randomized controlled studies in this aspect of tracheostomy care can make it more evidence based.
All authors declare not to have any conflict of interest related to the content of this manuscript.