Dyslipidemia is considered as the major risk factor for cardiovascular disease (CVD) and may contribute to the higher mortality in chronic obstructive pulmonary disease (COPD). However, the prevalence and consequences of dyslipidemia in COPD is still unclear.
We studied comprehensive lipid profile panel including serum total cholesterol (TC), triglyceride (TG), low density lipoproteins (LDL), very low-density lipoproteins (VLDL) and high-density lipoproteins (HDL) in COPD patients to study the relationship of dyslipidemia with severity of disease.
Serum TC, TG, LDFL, VLDL and HDL were measured at baseline patients with COPD. Anthropometry including BMI, mid upper arm circumference (MUAC), sum of four skin fold thickness and six-minute walk test (6MWT) were done in all the patients.
Of 125 recruited patients, 35 had moderate, 52 severe & 38 very severe COPD. Total cholesterol in moderate, severe and very severe COPD was 178.5 ± 34.5 mg/dl, 174.2 ± 36.4 and 169.4 ± 34.1 mg/dl respectively. Level of LDL in moderate, severe and very severe COPD was 107.5 ± 34.5 mg/dl, 103.0 ± 33.7 & 103.1 ± 35.6 mg/dl respectively. HDL levels in moderate, severe & very severe COPD were 43.2 ± 5.3, 44.9 ± 8.4, 43.1 ± 9.5 mg/dl. VLDL levels in moderate, severe and very severe COPD were 21.0 (11.0-112.0), 21.9 (2.0-177.0), 21.0 (10.0-80.0) mg/dl. TG levels in moderate, severe & very severe COPD was 106.0 (55.0-418.0), 106.0 (36.0-353.0), 103.0 (52.0-295.00 mg/dl respectively. 6MWT, BMI & MUAC decreased with severity of COPD. There was no significant difference in smoking index and waist hip ratio in the 3 groups.
We did not find any correlation between COPD disease severity and lipoproteins.
COPD, Dyslipidemia, Lipid profile
COPD often co-exists with other comorbidities that may impact prognosis of the disease [1-8]. Among these, Cardio-vascular events are the leading cause of morbidity and mortality in COPD. A greater than twofold risk is reported for cardiovascular-related hospitalization and mortality in patients with COPD compared with those without COPD [9].
Dyslipidemia is considered as the major risk factor for cardiovascular disease (CVD) and may contribute to the higher mortality rates in COPD associated with CVD [10-12].
However, the prevalence and consequences of dyslipidemia in COPD is still unclear. Some, but not all studies have demonstrated altered lipid levels in COPD. Significantly higher levels of TG, cholesterol, LDL and lower levels of HDL have been reported in COPD patients; however, their impact on disease outcomes has not been uniformly demonstrated [13].
Hence an attempt was made here to explore and document the extent of dyslipidemia in an Indian cohort of COPD patients.
The aim of this study was to study a comprehensive lipid profile panel by evaluating the serum levels of total cholesterol (TC), triglyceride (TG), low density lipoproteins (LDL), very low-density lipoproteins (VLDL) and high-density lipoproteins (HDL) in chronic obstructive pulmonary disease (COPD) patients and to study the relationship of dyslipidemia with severity of disease.
We conducted a prospective cross-sectional study in the Department of Pulmonary Medicine and Sleep Disorders, AIIMS, New Delhi, India.
One hundred and twenty-five (125) patients with a known diagnosis of COPD were recruited from the outpatient of the pulmonary medicine department between 2009 and 2013. The diagnosis of COPD was based on the presence of a compatible history plus spirometric demonstration of non-reversible airflow limitation as determined by FEV1/FVC ratio < 0.7. Spirometry was performed as per the ATS/ERS criteria (2005). All patients were required to be clinically stable for at least three months prior to study and free of clinical signs of exacerbation, such as infection or heart failure. Patients with a clinical history of asthma, bronchiectasis, pneumonia, tuberculosis or other inflammatory diseases such as malignancy, arthritis, inflammatory bowel diseases, liver, cirrhosis, end stage renal failure or connective tissue disorders were excluded. At the time of recruitment, patients were asked to complete a questionnaire containing demographic characteristics and history of cigarette smoking. The details of spirometric results, severity of disease based on GOLD's criteria, severity of dyspnea based on Modified Medical Research Council (mMRC) scale, exacerbation episodes of disease during the past years and history of inhaled steroid use were noted. Smoking habits of COPD patients were classified into three categories: 55 active smokers, 25 nonsmokers and 45 ex-smokers (withdrawal from tobacco > 6 months). The study was approved by the ethics committee of the Institute. Written informed consent was obtained from all the subjects.
Height was measured to the nearest cm and weight to the nearest 100 gm using standardized technique [14]. Body mass index (BMI) was calculated weight in kg and height in meters. Sum of skin fold thickness (in the biceps, triceps, sub scapular and suprailliac regions) were measured using Holtain calipers (Crymych U.K.).
Pulmonary function test was measured with a computer-assisted spirometery (Flow handy Zan100 USB, Oberthulba).
Forced expiratory volume in 1 second (FEV1), forced vital capacity (FVC), and Inspiratory capacity (IVC) were calculated from the flow-volume curve and expressed as a percentage of reference values. The highest value of at least three measurements was used. The reversibility of airway obstruction assessed according to GOLD guidelines using 400 micrograms inhalation of salbutamol [15,16]. Severity of disease was staged by mean FEV1 (L) and percentage of predicted FEV1.
Venous blood sample (5 ml) was drawn from all the patients in the fasting state of at least 14 hrs. The blood sample was centrifuged at 3000 rpm for 15 min; sera separated and stored at -80 ℃ until assayed. Total cholesterol, High density lipoprotein (HDL) and triglyceride (TG) levels were determined with Konelab auto analyzer using Randox test reagents. Low density lipoprotein (LDL) concentration was calculated using the Friedewald Equation (LDL = Total cholesterol-HDL-TG/5). Very low-density lipoprotein (VLDL) concentration was calculated using triglyceride/5 formula.
Besides descriptive statistics the analysis was done with the help of SPSS version 15. One-way anova/Kruskal-wallis test was applied to see the significance between three groups followed by multiple range tests. Pearson's correlation was used to measure the dependence between different variables. P value less than 0.05 is considered as significant.
Detailed baseline demographic and clinical characteristics of the study population are presented in Table 1. The study was carried out in 125 stable patients diagnosed with COPD. Based on FEV1, patients were characterized as moderately severe (FEV1 50-80%), severe (FEV1 30- 50%) and very severe (FEV1 < 30%). PFT variables of recruited subjects are shown in Table 2. Mean levels of mid upper arm circumference and sum of four skin fold thickness were increasing significantly with the severity of COPD.
Table 1: Demographics and clinical characteristics of the study population. View Table 1
Table 2: Spirometry variables in subjects recruited in the study. View Table 2
Concentration of total cholesterol (TC), LDL, HDL, VLDL and TG in moderate, severe and very severe COPD patients are shown in Table 3. None of the lipid was found significantly different among three groups of COPD patients. These are depicted in Figure 1 and Figure 2.
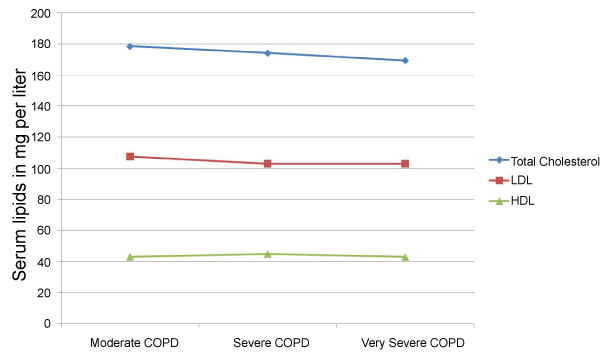 Figure 1: Distribution of total cholesterol, LDL and HDL levels amongst patients with respect to severity of COPD. View Figure 1
Figure 1: Distribution of total cholesterol, LDL and HDL levels amongst patients with respect to severity of COPD. View Figure 1
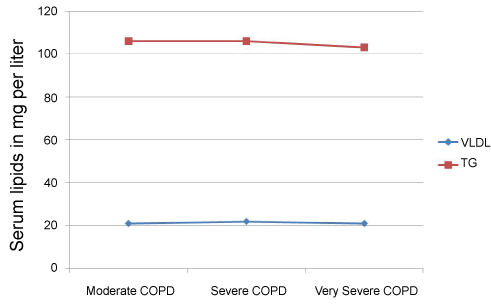 Figure 2: Distribution of VLDL and TG levels amongst patients with respect to severity of COPD. View Figure 2
Figure 2: Distribution of VLDL and TG levels amongst patients with respect to severity of COPD. View Figure 2
Table 3: Lipid profile in study population. View Table 3
Total cholesterol (TC), LDL, HDL, VLDL and TG levels were correlated with anthropometric measurements in all COPD patients. No component of the lipoproteins except Triglyceride was significantly correlated with anthropometric measures (Table 4).
Table 4: Anthropometric Correlation with serum Triglycerides. View Table 4
The triglyceride levels were significantly correlated with BMI (p = 0.003), sum of 4 skinfold thickness (P = 0.06) and mid upper arm circumference (p = 0.003). No significant correlation was found between triglyceride level and waist hip ratio.
In this cross-sectional observational study, we analyzed the lipid profile in COPD patients with varying degree of severity. It was observed that all components of lipid profile were within the normal predicted upper level. In addition, we did not find any statistical difference in total cholesterol (TC), LDL, VLDL, HDL and TG between mild, moderate and severe COPD. However, Triglyceride levels were significantly correlated with Body Mass Index (BMI) and Mid Upper Arm Circumference (MUAC). Increase in BMI and MUAC may increase triglyceride levels in COPD patients.
Patients with COPD generally encounter cardiovascular complications. Lipid profile is usually acknowledged as a good predictor for cardiovascular disease. Mitra, et al. found significantly high serum levels of all lipoproteins TC, TG, LDL in COPD cases than controls. HDL levels were also significantly decreased in cases than controls [13]. Our findings were compatible with a number of previously held studies. Attaran D, et al. evaluated the serum lipid profile in chemical warfare patients with COPD and found statistical difference in cholesterol and triglyceride levels between patients and controls but none of the lipid parameter showed any correlation with severity of airflow limitation assessed by FEV1 [17]. Similar results were reported in other studies [18,19]. Conversely, Beti Zafirova-Ivanovska and colleagues reported that hypercholesterolemia in COPD patients significantly increases with disease severity [20]. Overall, a definitive demonstration of dyslipidemia in COPD and its association with disease severity remains uncertain.
It is notable, however, that most previous reports show lipid profile within normal range. However, lipid levels were elevated in COPD compared to controls but were not abnormally high. These observations enforced us to think that etiological factors for COPD might contribute for cardiovascular complications in patients with COPD. Cigarette smoking is markedly the most important etiological factor for COPD [21] accordingly we found considerably high smoking index in very severe COPD patients. A number of studies have also been reported discussing role of smoking in causing dyslipidemia [22]. Smoking is a contributor for the development of COPD as well as for dyslipidemia.
The 6MWT is easy to administer, better tolerated, and more reflective of activities of daily living than the other walk tests [23]. Similar to previous studies, we found that the 6MWD of our subjects reduced significantly with worsening disease severity. This may have important implications on activities of daily living.
Anthropometric measurements are very useful to understand any disease so that role of nutrition can be ascertained in disease etiology and its management. Malnutrition is common in COPD and associated with poor exercise tolerance and higher morbidity and mortality. Sum of four skin fold thickness (SUM) and Mid Upper Arm Circumference (MUAC) are significantly lower in very severe COPD patients. COPD patients with lung deficit function require more energy to compensate their reduced lung function. Majority of their total energy expenditure is attributed to lungs for its efficient working. Body fat equally participates in energy production leading to lesser fat accumulation.
To conclude, our study suggests cardiovascular problems are not enhanced with disease worsening. We did not find any correlation between COPD disease severity and lipoproteins, but more comprehensive studies are required to get accurate results. As statin treatment in COPD patients reduced mortality rates [24], there must be integrated pathway linking COPD with cardiovascular problems. More work is needed to uncover the causative mechanism of cardiovascular disease in COPD. Major drawback of our study is that we did not include any healthy controls for case comparison.
The authors thank Mr. Ajit Kumar for technical assistance throughout the study.