Pyogenic granuloma, or lobular capillary haemangioma is common in skin and mucosal surface such as oral cavity. It hardly occurs in tracheal mucosal, and even more rare to cause life threatening tracheal obstruction. Surgical excision is the mainstay of treatment with multidisciplinary support.
A 56-year-old man presented with chronic cough and wheeze for 5 months, which was initially treated for Chronic Obstructive Pulmonary Disease (COPD). Worsening of symptoms with haemoptysis alerted for further imaging workup which revealed lobulated mass at distal trachea. Bronchoscopic excision of mass was performed successfully with Extracorporeal Membrane Oxygenation (ECMO) as the mass occluded almost entire trachea that made ventilation almost impossible.
Pyogenic granuloma is a benign disease, but it can be life threatening if occurs at airway mucosa. ECMO is always an option to buy time for definitive surgical treatment.
Pyogenic granuloma, Lobular capillary haemangioma, ECMO
Pyogenic granuloma is a relatively common benign vascular lesion that occurs on skin and mucosal surfaces. It is a misnomer since it is neither caused by bacterial infection nor it is a true granuloma. Besides skin, mucosal lesion frequently happens on oral cavity especially gingiva, nose and tongue. It is extremely rare to be present in tracheal mucosa [1]. To date, there are less than 15 reported cases of tracheal pyogenic granuloma from literature search.
A 56-year-old man, presented to casualty with a week history of worsening cough and wheezing. Cough was productive and there was frank haemoptysis. Otherwise, he had no fever, dysphagia, odynophagia, neck swelling or constitutional symptoms. He was a chronic smoker for 20 years and had hypertension as the only medical comorbidity. There was no significant surgical and family history. However, he has background history of chronic cough and wheezing for 5 months and was treated for Chronic Obstructive Pulmonary Disease (COPD) with bronchodilators and inhaled steroid but symptoms persisted.
On arrival to hospital, he was alert but tachypnoic. There was audible wheeze. His respiratory rate was 30 breaths per minute and saturation was 93% on high flow mask. There was no neck node or mass felt. Lung examination revealed prolonged expiratory phase with rhonchi. Air entry was equal but reduced bilaterally. A full ENT examination found no abnormalities in the nose, oral cavity, neck, pharynx until vocal cords. Blood and sputum workup for infectious causes were initiated and results were later found out to be negative. His PCO2 was 46 mmHg while PO2 was 94 mmHg. Chest X ray showed hyperinflated lung field. High resolution computed tomography of the thorax showed large pedunculated mass at right anterolateral wall of tracheal at the level of T1/2 vertebrae (Figure 1 and Figure 2).
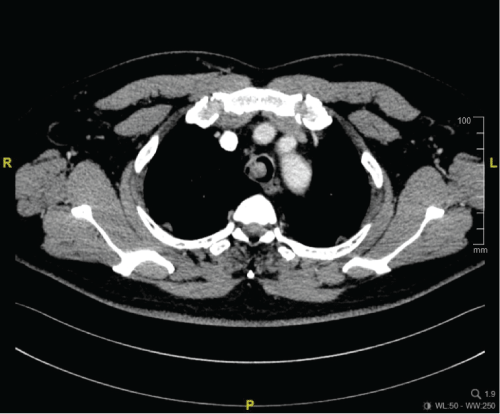 Figure 1: Axial cut of HRCT thorax showing pedunculated lobulated homogenous mass arises from right anterolateral tracheal wall. View Figure 1
Figure 1: Axial cut of HRCT thorax showing pedunculated lobulated homogenous mass arises from right anterolateral tracheal wall. View Figure 1
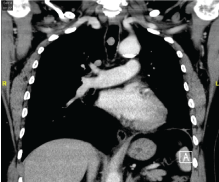 Figure 2: Coronal cut of HRCT thorax showing pedunculated lobulated homogenous mass arises from right tracheal wall. View Figure 2
Figure 2: Coronal cut of HRCT thorax showing pedunculated lobulated homogenous mass arises from right tracheal wall. View Figure 2
Emergency orotracheal intubation was accomplished promptly due to worsening respiratory distress but ventilation was deemed difficult. He needed high Positive End Expiratory Pressure (PEEP) at 10 cm H2O, pressure support at 14 and fraction of inspired oxygen at 80%, and yet tidal volume for a 70 kg man achieved was only 260 mls. Due to difficulty to maintain oxygenation, Emergency Extracorporeal Membrane Oxygenation (ECMO) was performed by cardiothoracic unit via veno-venous route.
Bronchoscopic excision of the mass was done with ECMO ongoing. The tissue mass was removed with biopsy forceps with the help of rigid suction tube endoscopically by 2 surgeons. Firstly, the attachment of the mass was identified and few drops of 1:100000 epinephrine were applied. The mass was then dissected away from base with suction tube and removed from trachea with optical forceps. It was a globular mass that occluded almost 90% of the distal trachea (Figure 3). The mass measured about 8 mm × 5 mm.
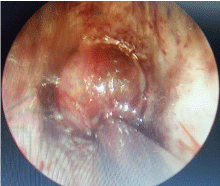 Figure 3: Bronchoscopic view of mass that occlude almost the entire distal trachea. View Figure 3
Figure 3: Bronchoscopic view of mass that occlude almost the entire distal trachea. View Figure 3
Histopathological result from specimen revealed lobular arrangement of capillaries within edematous fibroblastic stroma which was suggestive of pyogenic granuloma (Figure 4). He was extubated one day later and was discharged home well a week after the procedure. He is asymptomatic so far three years postoperatively and was planned for yearly follow up. No further scans were performed as the patient was asymptomatic and because of financial constraint.
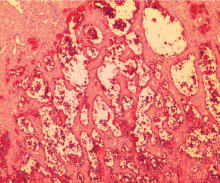 Figure 4: Low power view of the lesion. Respiratory epithelium with underlying tissue composed of numerous closely packed blood vessels. Haematoxylin & Eosin. (Magnification x40). View Figure 4
Figure 4: Low power view of the lesion. Respiratory epithelium with underlying tissue composed of numerous closely packed blood vessels. Haematoxylin & Eosin. (Magnification x40). View Figure 4
Pyogenic Granuloma (PG) is a common vascular hyperplasia of skin and mucous membrane. It usually occurs among young adults with its peak incidence in second and third decade of life. Higher incidence is recorded among female at their pregnancy interval due to its hormonal association. Mucosal lesions at oral cavity, nasal cavity, tongue, larynx, trachea, colon, duodenum have been reported [2]. However, there are only very limited cases on tracheal site lesion and it is extremely rare. Therefore, incidence at this site is still unknown. The aetiology of this lesion is not well understood. Possible predisposing factors include previous trauma, chronic irritation, viral oncogenes, and increased level of female sex hormones. Although trauma is reported as a triggering factor, only 7 to 23% of patients reported a previous injury at the site. As for hormonal association, there is a 5% reported association between pyogenic granuloma and pregnancy [3].
Recently, the term 'Lobular Capillary Haemangioma' (LCH) has been suggested due to its histological appearance of the lesion. It has distinctive lobular arrangement of capillaries of various sizes in a fibro myxoid matrix. Often, there is ulceration of surface epithelium with surrounding inflammation. Macroscopically, it always appears as a polypoidal tissue, either pedunculated or sessile [4]. It may bleed easily if ulceration is present. There is no risk of malignant transformation. Any lesion with such appearance must be excised or biopsied to rule out malignancy. In general, tracheal tumours account for less than 2% of all upper respiratory tract growth. Malignancy must be ruled out from biopsy or excision especially among adult populations. Differentials could include adenoma, lipoma, papilloma, fibroma, chondroma and cancer [5].
Previous reported cases of tracheal PG shared same symptoms of cough and haemoptysis. Prakash, et al. reported a similar case of tracheal PG in a pregnant young lady with airway obstruction, whom was initially thought of asthmatic attack [6]. The severity of obstruction was almost the same until the extent of ECMO needed.
Diagnosis of tracheal PG is actually via direct bronchoscopic examination and excision or biopsy of the lesion. Imaging study such as HRCT thorax may give clues on the extent of the lesion and degree of obstruction. However, it is not as sensitive as direct bronchoscopic examination as small tracheal PG maybe missed from the scan [7].
Surgical excision is the mainstay of treatment for PG. Various methods have been described. Endoscopic excision was first described in a 64-year-old man by Xu, et al. [8] Chawla, et al. successfully used combined endoscopic and laser technique to remove a distal tracheal PG in an elderly man as well [9]. Other modalities included cryotherapy and electrocautery loop snare were demonstrated by Udoji, et al. and Kalanjeri, et al. respectively [10,11]. In our report, technique performed was a conventional method with the use of cold instruments such as bronchoscopy and biopsy forceps, which was similar to the case described by Irani, et al. [2]. Excision of PG at tracheal carries risks of aspiration pneumonia, pneumothorax, oesophageal injury and sudden complete airway obstruction in severe bleeding. Methods of hemostasis that had been been described includes adrenaline drops, electrocauterization, brachytherapy and photocoagulation [12]. In our report, bleeding was minimal and was able to be secured with drops of adrenaline.
Therefore, proper planning of management is of extreme importance to prevent such disaster. Multidisciplinary approach that involves experienced ENT surgeons, anaesthetists, cardiothoracic and pulmonary teams is required for the challenge from the 'difficult airway'. Total tracheal obstruction in our case made us no choice but to opt for ECMO as a temporary method to maintain oxygen saturation and to buy time for complete surgical excision. This method has been successful in many cases of severe tracheal obstruction by any causes such as foreign bodies, and most frequently malignant tumours from trachea or mediastinum [13]. In such cases, invasive means to provide airway, such as endotracheal intubation and tracheostomy are not suitable as obstruction could not be bypassed. Another adjunct frequently used in difficult airway is Heliox. It is a mixture of helium and oxygen. It has lower density than room air and helps reduce airflow resistance by increasing laminar flow [14].
In summary, acute tracheal obstruction especially at the distal trachea is very rare, but it is extremely challenging for managing clinicians. It is a situation where the airway is equivalent to 'cannot bag, intubate or tracheotomise'. Other means to maintain oxygenation must be bore in mind such as ECMO if facilities and specialties are available.
Besides, in our report, because of patient's chronic smoking behaviour, symptoms of chronic cough and wheezing misled us to the diagnosis of COPD in the initial phase of treatment. Therefore, besides cough and wheeze, symptoms of haemoptysis could give extra clue that the airway must be further examined bronchoscopically or radiologically to rule out any sinister pathology in the trachea.
|
• Chronic wheezing and cough unresponsive to medical therapy should warrant further investigation of the airway. HRCT provides valuable information about airway disease. • PG of tracheal mucosa is a very rare benign disease with no risk of malignant transformation. It could lead to tracheal obstruction. Bronchoscopy is both diagnostic (biopsy) and therapeutic (endoscopic excision). |
None declared.