Obesity is considered an increasing problem in the worldwide population, reaching epidemic proportions of about 400 million obese people in the world. The accumulation of adipose tissue leads to chronic oxidative stress, since its excess is associated with the development of inflammation, increasing the probability of developing comorbidities due to weight gain. This research aimed to evaluate the changes in inflammatory and antioxidants biomarkers after bariatric surgery in patients with morbid obesity. The study was executed with a population of 63 people with morbid obesity, composed of 77% of women and 23% of men, analyzing their food consumption, antioxidant level, oxidative stress, anthropometric and biochemical data. It was observed that after 6 months of surgical procedure, in addition to weight loss, there was a significant improvement in antioxidant biomarkers and oxidative stress.
Obesity, Bariatric surgery, Oxidative stress, Antioxidants
Obesity is characterized by the excessive accumulation of fat in the body, constituting a complex and multifactorial disease with severe social, psychological and clinical consequences, affecting all ages and social groups. Its prevalence has grown sharply in the last decades, being one of the most serious problems of public health. Overweight may be linked to an individual's genetic patrimony, poor eating habits, lifestyle, emotional factors or endocrine disorders, being a risk factor for a number of diseases [1].
The storage of adipose tissue is associated with the development of oxidative stress and inflammation, which can trigger comorbidities associated with this overweight, leading to risks in the development of chronic noncommunicable diseases (NCDs) such as type 2 diabetes and cardiovascular diseases which, if untreated, can lead to premature death or reduced quality of life. Visceral fat is an endocrine organ of hormonal storage and producer of inflammatory adipokines, causing the obese person to present chronic inflammation. Increased levels of IL-6 (interleukin-6) and TNF-alpha (tumor necrosis factor), multifunctional cytokines, are associated with morbidity and mortality [2].
Yet, the enzymes that act as markers of oxidative stress, CAT, SOD and NADPH, act by means of prevention mechanisms, preventing and/or controlling the formation of free radicals and non-radical species involved in the initiation of chain reactions that culminate in the propagation and amplification of the process and, consequently, the occurrence of oxidative damages [3].
Obesity can be treated through conservative, non-invasive therapies, aimed at modifying eating habits, with the follow-up of a nutritionist, followed by the stimulation of the practice of physical activity, in order to change the lifestyle. Also, in conjunction with these practices, the use of medications, which will be considered if there is failure associated with non-pharmacological treatment, if the patients have grade 2 and 3 obesity, or if they have any other obesity-related pathology [4].
Another therapy that has become increasingly frequent is non-conservative and invasive bariatric surgery (BS), and it has been shown to be efficient in reducing comorbidities associated with obesity, in weight loss, besides contributing to the improvement in quality of life. Surgical techniques differentiate according to the mechanism of action, being able to be restrictive, disabsorptive or mixed [5].
The technique of bariatric surgery discussed in the present study is the mixed one. It promotes a gastric reduction associated with malabsorption, especially the Roux-en-Y Gastric Bypass operation, or Fobi-Capella, which reduces stomach volume to 30 ml [5].
Bariatric surgery is considered one of the most effective ways to treat severe obesity because, in addition to leading individuals to lose weight and possibly treat obesity-related comorbidities, it also enables a change in lifestyle and promotes new post-surgical habits [5].
Studies indicate that the reduction of obesity markers, which are the proinflammatory IL-6 (interleukin-6) and TNF-alpha (tumor necrosis factor), and those of oxidative stress, NADPH (nicotinamide adenine dinucleotide phosphate), CAT (catalase) and SOD (superoxide dismutase), bariatric surgery exerts a protective effect on the damage caused by oxidative stress [6].
Thus, the present study had as objective to evaluate the alterations of inflammatory and antioxidant biomarkers after bariatric surgery in patients with morbid obesity.
After approval by the research ethics committee, a clinical cohort study was applied, with sample selection by convenience. All patients underwent Fobi-Capella surgery and were invited to participate in the study; it was explained to them how the study would be performed and, after acceptance, the patient signed the TCLE (Informed Consent Form) (Appendix A). The study was conducted at a private bariatric surgery clinic in the city of Natal-RN, Brazil.
The sample was freely demanded according to the flow of surgeries in the clinic, in which the patients were in the pre-surgical phase and in the sixth postoperative month. The patients were submitted to Fobi-Capella technique, considered a mixed technique of surgery (restrictive and disabsorptive). The exclusion criteria considered were: smokers, alcoholics, use of antioxidants and patients with severe renal and hepatic diseases.
In addition to chart analysis, patients were asked to fill in questionnaires containing cadastral data (name, age, gender, family per capita income, educational level, occupation) and clinical data (comorbidities, use of medications and/or supplements, consumption of antioxidant foods and the practice of physical activity) (Appendix B).
Dietary intake was assessed by retrospective use, a 24-hour food recall (Appendix C), which was performed in the consultation before the surgical procedure and at the consultation 6 months after surgery. The quantities of food referred to by the patients, in a home measure, were converted to grams (g) or milliliters (ml) using a home measurement table (Appendix C). The consumption data were calculated by the TACO table (Tabela Brasileira de Composição de Alimentos - Brazilian Table of Food Composition). In order to evaluate the adequacy, the reference values of the Dietary Reference Intakes-DRI were used [7].
The anthropometric evaluation was performed before and after bariatric surgery, and the patients were weighed in a scale with the least possible clothing, barefoot, and in an erect position. The height was obtained by a stadiometer, the patient standing upright with the arms extended along the body, with his/her back to the wall, in the Frankfurt plane (Appendix B).
The BMI (Body Mass Index) was obtained according to the World Health Organization [8] for adults and Lipschitz [9] for the elderly.
CB measurement (arm circumference) was performed using an inelastic tape measure at the midpoint between the acromion and the olecranon. The TSF (triceps skinfold thickness) was measured by the adipometer at the back of the arm, also at the midpoint between the acromion and the olecranon. From the BS and TSF measurements, arm muscle circumference (AMC) was calculated, which is classified according to Frisancho [10].
For the measurement of AMP (adductor muscle thickness of the thumb), the patient maintained the hand relaxed, with the arm resting on the thigh, with the thumb away from the rest of the fingers, forming a 90º angle with the index finger, so that the muscle could be pinched by the adipometer.
Three measurements of each variable were performed to obtain the average, as a final result.
Approximately 5 ml of blood was collected from the antecubital region of the forearm for analysis of the concentration of IL-6 (interleukin 6), TNF-alpha (tumor necrosis factor), SOD (superoxide dismutase) (16190SOD), CAT (catalase) (CAT100) and enzymatic cofactor NADP/NADPH (nicotinamide adenine dinucleotide phosphate) (MAK038-1KT). The collections were performed by qualified individuals, and all biosafety procedures were considered. After the necessary preparations for each technique, the samples were frozen in an ultra-freezer at a negative temperature of 80 ℃ degrees. Biochemical techniques were performed in the potiguar laboratory of Natal-RN, Brazil, and the dosage method used was Elisa (SIGMA-ALDRICHE, St. Louis-MO, USA).
Patients underwent routine biochemical exams and their results were taken from the medical records. Considering their importance, they are performed monthly, so that there is control in the levels of fasting glycemia, Total Cholesterol, HDL and Triglycerides.
All results were expressed as mean and standard deviation, structured and analyzed using descriptive analysis with the statistical package (PRISMA, 2017) version 7.0 for MacBook. Descriptive analysis of the general characteristics of the study population (sex, gender, weight, height, BMI, oxidative stress biomarkers and biochemical tests) and dietary parameters (24 h recall) were performed, and data were presented as mean ± standard deviation (M ± SD). Student's t-test was performed. Statistical significance was defined as p < 0.05.
The study included 63 individuals who met the inclusion and exclusion criteria. The mean age was 37.4 (± 10.61) years, being composed predominantly by women (77%). The most frequent comorbidities were systemic arterial hypertension (48.3%) and diabetes mellitus (35%), as shown in Table 1.
Table 1: Profile of age and comorbidities of individuals undergoing bariatric surgery at a private clinic. N = 63 individuals. View Table 1
Regarding the anthropometric parameters, the individuals presented a reduction of 127 kg (kilogram) (± 12.73) to 84.3 kg (± 12.93) in body weight (p < 0.05). As for fat mass and lean mass, a reduction of 51.4 kg (45-75) to 29.5 kg (21.5-49.5) was obtained with (p < 0.05), and a reduction of 56.4 kg (47-89.4) to 40.4 kg (31.8-82.2), respectively (p < 0.05). The initial BMI of 42.1 Kg/m2 (38.6-53.5) significantly reduced to 29.9Kg/m2 (26.4-39.8) (p < 0.001). A significant reduction in waist circumference variables was also observed in relation to the preoperative period (Table 2).
Table 2: Anthropometric profile of individuals undergoing bariatric surgery at a private clinic. N = 63 individuals. View Table 2
After 6 months of obesity surgery, subjects had a reduction in biochemical tests (glycemia, cholesterol and triglycerides) and had an increase in HDL parameters, as shown in Table 3.
Table 3: Biochemical parameters of individuals undergoing bariatric surgery at a private clinic. View Table 3
Figure 1, shows the data of inflammatory markers. In the six-month period after obesity surgery, significant differences were obtained in inflammatory parameters (p < 0.0001), IL-6 with 268.6 pg/mL (± 18.5) and TNF-alfa with 200.4 pg/mL (± 16.4). The results suggest that patients undergoing bariatric surgery significantly decreased inflammatory mediators after 6 months.
 Figure 1: Evaluation of inflammatory markers of individuals undergoing bariatric surgery at a private clinic. BS: before surgery; AS: 6 months after surgery. View Figure 1
Figure 1: Evaluation of inflammatory markers of individuals undergoing bariatric surgery at a private clinic. BS: before surgery; AS: 6 months after surgery. View Figure 1
In Figure 2, oxidative stress was evaluated by the enzyme NADP/NADPH (nicotinamide adenine dinucleotide phosphate) that decreased after 6 months of bariatric surgery from 359.4 RLU/mg (± 53.5) before surgery to 249.3 RLU/mg (± 41.4) with significant difference (p < 0.0001).
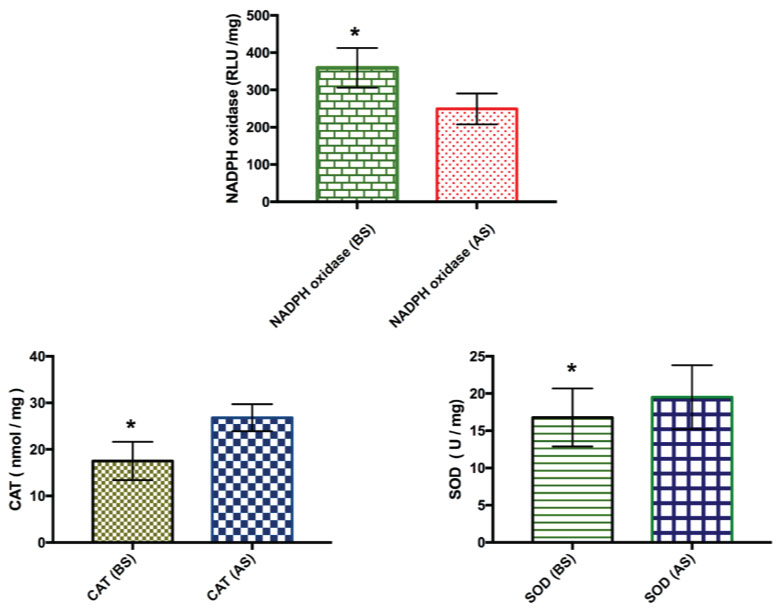 Figure 2: Evaluation of oxidative stress markers of individuals submitted to bariatric surgery at a private clinic. BS: before surgery; AS: 6 months after surgery. View Figure 2
Figure 2: Evaluation of oxidative stress markers of individuals submitted to bariatric surgery at a private clinic. BS: before surgery; AS: 6 months after surgery. View Figure 2
As it can be observed in Figure 2, the CAT activities were significantly different between the groups (p < 0.05). Throughout the study, the activity of the CAT enzyme had an increase in the 6 months after the surgical procedure, showing its antioxidant potential, in relation to the basal moment. Regarding the SOD, the results were similar to those of CAT, for which 6 months after the surgical procedure there was a significant increase of the SOD enzyme (p < 0.05).
In Table 4, the correlations between IL-6 and TNF-alpha with the waist circumference were evaluated. The results suggest a positive correlation between the parameters evaluated; the decrease in waist circumference (Table 2) decreases the inflammatory cytokines (Figure 1) in the individual after 6 months of bariatric surgery.
Table 4: Correlation between IL-6 and TNF-alpha and the waist circumference. View Table 4
Being overweight today is a global crisis. Today, 40% of the world's population is overweight, three times more than 40 years ago (World Health Organization) [11]. In Brazil, one in two adults, and one in three children, is in the same condition (Brazilian Institute of Geography and Statistics - IBGE, 2010). Obesity increases the risk of deadly diseases like diabetes, heart disease and at least 13 types of cancers, according to the National Cancer Institute (INCA) [12]. All these diseases are among the main causes of death in Brazil [13].
According to the Ministry of Health, in Brazil, at least 17% of the population is obese due to sedentary lifestyle and high consumption of industrialized products [14].
Due to the great increase in obesity indexes, there are currently several ways to fight it. Among the treatments, bariatric surgery stands out, which is an invasive procedure for individuals with class III obesity. This procedure has been developing technologically, and its advance is in accordance to the increase of the global epidemic of obesity. To date, only 1% of the patients undergoing this surgery have the effects of reversed weight loss [15].
According to the data described above, related to obesity and the performance of bariatric surgeries, the present study presents the benefits of this procedure, showing that individuals in the range of 37 years of age present significant changes in weight, with associated comorbidities, and that women are predominant in the number of bariatric surgeries. One possible explanation for this fact, perhaps, is because women are more concerned about beauty and health care [16].
The study points out that, of the 63 individuals who participated in the study, 48.3% were hypertensive and 35% were diabetic (Table 1), being these the most prevalent diseases due to obesity among patients. In a large cohort study carried out by Dra. Gunn Signe Jakobsen, doctor at morbid obesity center of the Sykehuset i Vestfold in Tønsberg (Norway), it was seen that, in addition to weight loss, bariatric surgery also reduced the risk of hypertension and other obesity-related comorbidities [17].
Table 2 of the present study shows that there was a very significant reduction of p < 0.001 in body weight, in BMI and in the fat mass index of the patients, as well as a significant loss of p < 0.05 of lean mass after 6 months of bariatric surgery; it was notorious that results related to weight loss associated with a change in body fat distribution allowed a considerable improvement in biochemical tests (Table 3), with a significant improvement in the markers of Glycemia, Total Cholesterol, HDL and Triglycerides, thus reducing the risk of diseases associated with obesity.
The possible explanation for this fact must be due to the significant decrease in the number of adipose tissue (Table 2), since the amount of fat is directly related to the increase in insulin resistance. The indicators of body composition are strongly associated with metabolic alterations, and it is important to verify their relation with the components of metabolic syndrome and insulin resistance [18], increase in blood pressure, since the excessive fat accumulation in the abdominal region and the deposition of adipose tissue in the viscera are strongly related to the cardiovascular risk factors [19].
Adipose tissue has the capacity to produce adipocytokines, substances that participate in the inflammatory response. These adipocytokines may present pro- or anti-inflammatory actions, such as TNF-α, IL-6 and adiponectin, respectively. Obese individuals have reduced levels of adiponectin [20].
Figure 1 shows the evaluation of inflammatory markers of patients undergoing bariatric surgery. Results were obtained with significant differences in the parameters of the proinflammatory cytokines IL-6 (interleukin) and TNF-α (tumor necrosis factor) after 6 months of surgery, showing that the reduction of adipose tissue has a great impact on these biomarkers. In an article that addresses the inflammatory processes of obesity, it has been seen that adipose tissue is not just a stock organ. It also plays the role of producer of certain bioactive substances as IL-6, with inflammatory functions. As the amount of adipose cells increases, there is a change in the production of inflammatory adipokines, that is, the greater the amount of adipose tissue, the greater the secretion of these adipokines, such as TNF-α and IL-6. They are adipokines with immune function, and are produced by adipocytes in response to infectious or inflammatory stimuli. The authors concluded that reducing body mass through bariatric surgery is a safe method to decrease the inflammatory state of these biomarkers [21].
Thus, according to the benefits derived from the surgical intervention for the control and reversal of obesity, the evaluation of antioxidant biomarkers and oxidative stress in patients after Fobi Capella type bariatric surgery was exposed in Figure 2.
For a better understanding, it remains to be known that free radicals are reactive molecules containing a number of unpaired electrons, which are produced in the normal course of energy metabolism. According to this theory, toxic effects of these radicals are introduced into the cellular interior, triggering deleterious reactions called oxidative stress [22].
The installation of the process of oxidative stress arises from the existence of an imbalance between oxidant and antioxidants compounds, in favor of excessive generation of free radicals or to the detriment of their speed of removal. Such a process leads to the oxidation of biomolecules with consequent loss of their biological functions and/or homeostatic imbalance; the manifestation of which is potential oxidative damage against cells and tissues [3].
Obesity and associated comorbidities are one of the causes of this homeostatic imbalance, giving rise to oxidative damage [23].
In Figure 2, the results of oxidative stress biomarkers can be observed by the enzymes cofactor NADP/NADPH (nicotinamide adenine dinucleotide phosphate), CAT (catalase) and SOD (superoxide dismutase), which are natural enzyme defenses. It was observed that there was extreme significance (p < 0.001) in the biomarkers of NADPH, which is a pro-oxidant enzyme, and a reduction after 6 months of surgery was observed. With the CAT and SOD antioxidant enzymes, it was observed that there was a significant increase (p < 0.05) in biomarkers after 6 months of surgery, in relation to basal moment, leading to the belief in the benefits of bariatric surgery, and that fat reduction improved the picture of chronic diseases associated with obesity, in view of the balance between pro-oxidant and antioxidant enzymes.
In the present study, the results suggest that the surgical procedure promoted weight loss accompanied by the decrease of body fat, improving inflammation parameters.
The results also suggest that the decrease of the inflammatory cytokines has a relation with the decrease of visceral fat, as shown in Table 3 and in Figure 1. In the study by [24], it was demonstrated the body mass and the subsequent improvement of biochemical, metabolic and anthropometric parameters in patients undergoing bariatric surgery. This may contribute to the reduction of patient oxidation and, consequently, reduce the risks of development and multiple comorbidities associated with obesity.
Therefore, the results show that the surgical procedure promoted an improvement of the defense system (Figure 2), allowing the increase of the CAT and SOD enzymes, which constitute the first line of antioxidant defense and the largest defense system of the organism, as well as the decrease of NADPH, showing the reduction of oxidative stress [25].
In analyzes performed in the data collections of the present study, a significant improvement was observed in all aspects after 6 months of bariatric surgery, such as weight reduction, improvement in biochemical tests, and a decrease in fasting glycemia, in total cholesterol, in HDL and in triglycerides, in inflammatory markers (IL-6 and TNF-alpha), as well as in oxidative stress markers (NADPH, CAT and SOD). This leads us to believe that bariatric surgery was of total relevance for an improvement in the quality of life of these patients. However, this is still a topic that needs to be discussed and studied, analyzing genetic and external factors, lifestyle, among others, since its prevention and final resolution are extremely important for the well-being of the population affected by obesity.