We are an established pleural centre offering medical thoracoscopy and indwelling pleural catheters. Our infection rates with prophylactic antibiotics were lower than the national average and given the era of antibiotic stewardship and lack of evidence to support the administration, we stopped giving them. We then noticed a large jump in infection rates and hence, in this paper, we reviewed our practice.
Physician led invasive pleural procedures such as Indwelling Pleural Catheters (IPCs) and Medical Thoracoscopy (MT) are becoming well established in everyday respiratory practice in the management of both malignant and non-malignant pleural effusions [1-5].
Anecdotally, in the United Kingdom, practice varies enormously amongst hospitals as to who does the procedures, where they are done and what follow up services are set up. We have previously called for a national database in the hope that standardisation of practice can occur [6].
Complications of these procedures do occur and can carry significant morbidity and mortality. Infection rates have been studied extensively and range between 3 to 7 percent [1,3,5]. As such, there is an ongoing debate as to how to reduce this complications and one of the aspects of this is whether antibiotics should be given pre-procedurally.
There is a scant body of evidence on the foregoing. The current British Thoracic Society guidelines only suggest routine prophylaxis only in patients with risk factors such as asplenia, prosthetic heart valves and previous endocarditis and this is based on expert opinion only [1]. Nuttal et al. [7] have presented that prophylactic doxycycline following IPC insertion for malignant pleural effusions probably reduced their infection rate. More recently, Dhooria, et al. [8] randomised 100 patients to receive either cefazolin or intravenous saline. The infection rate in the antibiotic group did not reduce, even after all the variables were controlled for. This is the only randomised controlled trial to date.
We run a well established, safe and streamlined pleural service, serving over 500,000 patients across 3 different sites. We have previously published our low infection and high sensitivity rates of IPCs and MT respectively following a review of all procedures done from 2010 to 2015 [6]. We then did all our procedures in theatre under strict aseptic conditions, and recommended a pre-op single dose of prophylactic antibiotics.
In 168 cases of MT, we had three pleural space infections (1.7%) and two wound infections (1%). Our diagnostic sensitivity was 97%, which is higher than other quoted figures. In 70 patients with IPCs, 96% had prophylactic antibiotics pre-procedure and three (4%) developed late pleural space infections. All three required intravenous antibiotics. One had cellulitis around the insertion site and required drain removal and the others received intrapleural fibrinolytics according to the MIST 2 protocol to clear their pleural space.
As such, in January 2015, we stopped giving prophylactic antibiotics prior to such procedures. There are no national guidelines for this, so this was agreed locally between the pleural consultants.
For clinical governance, we then reviewed our infection rates from Jan 2015 to Jan 2016. All our procedures are done aseptically in theatre. All the pleural consultants and trainees doing the procedures are trained in surgical scrubbing techniques.
During that time, 28 IPCs were performed, and there were 5 infections (18%), 2 within 4 weeks of the procedure. 1 was an empyema requiring intrapleural fibribolytics and drain removal, 2 had superficial cellulitis and 2 insertion site abscesses, with 1 IPC removed from each group.
40 MTs were performed, and there were 2 empyemas (4%) both requiring intrapleural drugs. 1 of them was within 4 weeks of procedure. Figure 1 shows one such instance of infection.
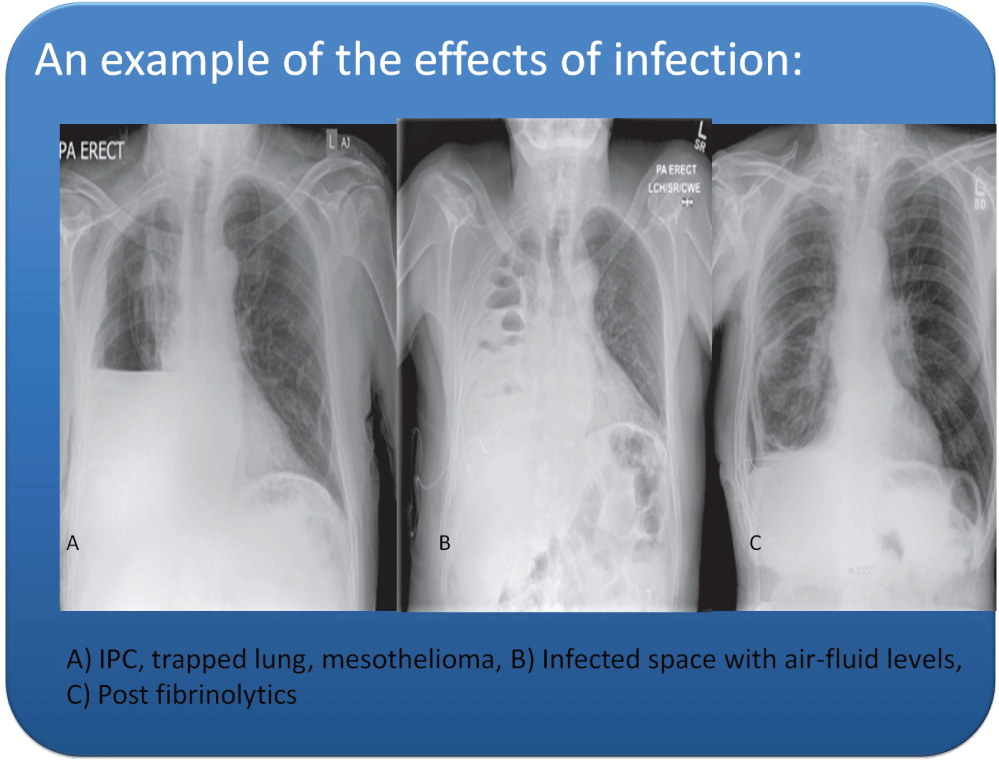 Figure 1: A) Shows the chest x-ray of a mesothelioma patient with a trapped lung and an IPC in situ; B) Shows a loculated pleural effusion with multiple air fluid levels and; C) shows clearance of the pleural space after the administration of fibrinolytics. View Figure 1
Figure 1: A) Shows the chest x-ray of a mesothelioma patient with a trapped lung and an IPC in situ; B) Shows a loculated pleural effusion with multiple air fluid levels and; C) shows clearance of the pleural space after the administration of fibrinolytics. View Figure 1
All required admission and 6 required treatment with intravenous antibiotics. Length of stay was between 1 and 36 days. There was no associated mortality.
Bacteria grown were Corynebacterium jeikeirum, Streptococcus anginosis and Coagulase negative staphylococcus.
Table 1 show the infection rates which have clearly increased. This is a small sample and our previous data was based on review of 70 IPCs and 173 thoracoscopies. However, we could not ignore the increasing rate of infections and so we have opted to start giving 2 grams of flucloxacillin pre and postoperatively.
Table 1: Shows a clear rise in the incidence of infection with no prophylactic antibiotics. View Table 1
Further work will determine if that is correct, but we would welcome data from more pleural centres on this topic. We recognise the importance of antibiotic stewardship and that in the era of growing antibiotic resistance, we should not be giving antibiotics without proper evidence available. This is urgently needed given the increasing popularity of these physician led invasive pleural procedures.