Cambodian Ministry of Health (MoH) is working towards the elimination of mother-to-child transmission (eMTCT) of HIV by 2025. According to national policy, following the antiretroviral therapy for HIV-positive pregnant women (PW), HIV-exposed infants (HEI) are given antiretroviral prophylaxis for six weeks (PMTCT Guideline 2011), followed by a first PCR test (PCR1) and cotrimoxazole (CTX) prophylaxis at six weeks of age, and later followed with an HIV-antibody test (AB-Test) at 18 months. Based on the Cambodia MOH national report in 2017, 75.0% of HEIs received ARV Prophylaxis, 35.0% received PCR1 and 41.3% obtained CTX within two months of age. Therefore, we aimed to assess the knowledge and practice of HIV-positive PW and providers' perception about low service uptake for HEIs.
We conducted a sequential mixed method study to quantitatively analyze national data on 1,118 HIV-positive PW and infants pairs registered between 2014 and 2016, supplemented by qualitative study through in-depth interviews with 38 HIV-positive PW and post-delivery women and 9 providers who worked at local antenatal and antiretroviral clinics in four referral hospital in Cambodia. Frequencies and factors associated with low uptake of HEI services were analyzed using STATA 14; qualitative conventional content was analyzed using NVivo 10. We excluded abortions and stillbirths and neonatal deaths from analysis.
We found that among 1,037 HEIs, 72.0% received NVP, 47.0% received PCR1, 50.3% received CTX within two months of age and 7.0% received AB-Test. Three supportive reasons discovered from qualitative study were: a lack of knowledge by women, a lack of clear education and misunderstanding by ART and ANC providers, and inadequate care seeking behavior by women driving to low use of HEI service.
We conclude that HIV-positive PW and providers in all four referral hospitals commonly misunderstand the service delivery needs of HEI. This report is the first describing gaps in knowledge and practices among HIV-positive PW and providers and has uncovered significant barriers to the use of HEI service that can be used to make the necessary changes needed to Cambodian MOH national eMTCT goal.
Cambodia, Elimination, HIV-Exposed Infants, HIV-positive pregnant women, Mother-to-child transmission of HIV
AB-Test: Antibody Test; AIDS: Acquired Immune Deficiency Syndrome; B-IACM: Boosted-Integrated Active Case Management; CTX: Cotrimoxazole; HEI: HIV-exposed Infant; HIV: Human Immunodeficiency Virus; eMTCT: elimination of Mother-to-Child Transmission; LTFU: Lost-to-Follow-up; NVP: Nevirapine; PCR: Polymerase Chain Reaction; PW: Pregnant Women
Cambodian Ministry of Health set a goal to eliminate mother-to-child transmission (eMTCT) of HIV by 2025, defined as a target MTCT rate of less than 5% among breastfed HIV-exposed infants (HEI) [1]. Cambodia has made substantial progress in the field of HIV prevention and care, including prevention of MTCT over the last 10 years. HIV prevalence among pregnant women (PW) has fallen from 2.9% in 1999 to 0.28% in 2014 [2] and to 0.18% in 2018 with the number of HEIs born in 2014-666 cases, 2015-699 cases and 2017-537 cases [3]. The predicted HIV-MTCT rate at two months of age has declined from an estimated 37.0% in 2007 to 6.2% of in 2015. Despite a high coverage of PW knowing their HIV status and a high proportion of HIV-positive PW receiving ART (93.0% and 77.0%) respectively [3], the coverage of services for HEIs remains low: In 2017 75.0% received ARV prophylaxis (nevirapine, NVP), 35.0% received first polymerase chain reaction test (PCR1) and 41.3% had cotrimoxazole (CTX) prophylaxis within two months of age [1].
HEI is defined as an infant or child less than 24 months of age who was born to an HIV-positive mother until HIV-positive diagnose is made. HEI services in this study refers to the package of care for early infant diagnosis, ARV-prophylaxis (NVP) and OI-prophylaxis (CTX) and PCR1, HIV-antibody test (AB-Test). In 2014-16, in Cambodia, HIV-positive PW were offered lifelong antiretroviral therapy (ART) following the WHO's Option B+ policy and HEIs were given NVP at birth, followed by PCR1 test and CTX at six weeks of age. All HEIs were given AB-Test when HEIs reached 18 months of age [4].
Globally, a number of studies have identified reasons that could influence the low uptake of HEI Service. A lack of knowledge and poor practices by HIV-positive PW, specifically the fact that some women are not aware of how a mother can transmit HIV to her child after birth [5]. Some mothers do not give NVP to their newborns because they deliver at home [6]. Loss-to-follow-up of children can occur throughout the PMTCT cascade: For example, 16.0% are lost prior to the first infant visit and from 4.1% to 75.0% are lost by the age of 3 months, and from 20.8% to 66.1% by the age of 18 months [7]. Confirmed MTCT rates can be low, but due to poor retention, it is estimated that only about half of HIV-positive children are diagnosed [8] and there are missed opportunities for pediatric diagnosis also failure to collect child HIV test results [9,10]. Finally, poor management, service location and follow-up care can contribute to low outcomes for HEI. These can include a lack of funds for transportation [9,11]. Late enrolment of the HEI in follow-up clinics can also be due to home delivery [9,11,12].
Despite low levels of service uptake, there are limited studies investigating reasons for underutilization of pediatric services for HEIs in Cambodia. Therefore, we conducted this study to assess the knowledge and practices of HIV-positive PW and providers' perception about the low uptake of HEI services.
The quantitative study was carried out on the Cambodian national follow-up database obtained from the National Center for Dermatology and STI (NCHADS) on PW-HEI pairs registered between 2014 and 2016 covered 9 of 25 highest HIV-prevalence provinces in Cambodia. Subsequently, we purposely choose three provinces to conduct interviews, including Battambang, Phnom Penh Municipality and Siem Reap (SRP) due to the HIV outbreak, HIV-positive PW mobility, hidden HIV-positive PW and free delivery service with formula milk from private clinic (Kanthakbopha) respectively. The qualitative study was conducted in four referral hospitals (RH) of three provinces including Roka (ROKA) and Sampov Loun (SPL), Social Health Clinic (SHC), Siem Reap (SRP).
A sequential mixed method was conducted to explain the low service uptake for HEIs found from the quantitative data among 1,118 HIV-positive PW and infants pairs registered in the national follow-up database. Our design may be more complete than the national database as it included additional data found in the 5 provincial PMTCT records and data from national laboratory unit (EID database).
The qualitative component consisted of in-depth-interviews (IDI) with 38 HIV-positive women and 9 providers. The qualitative replies from women pregnant now reflect those that delivered in 2014-16. Because all HIV-positive PW have bi-monthly visits at ART clinics, we randomly selected HIV-positive women from the four RHs' list stratified by current pregnancy, post-delivery or/and abortion who did or did not have antenatal care (ANC) or/and antiretroviral therapy (ART). We also recruited providers from ANC, delivery, ART services to see the differences of service provision.
Data obtained from NCHADS was verified through comparison with the provincial PMTCT and EID database for complementation, de-duplication and correction. We used STATA 14 to analyze the frequency and factors association such as women's age group, rural-urban, provinces and delivery status with the use of NVP, PCR1, CTX and AB-Test. We excluded 81 cases from HEI service analysis (58 abortions, 23 stillbirths/neonatal deaths). We analyzed the use of NVP, PCR1, CTX within 8 weeks of age and AB-Test within 24 months of age.
Two sets of question guides (in-depth-interview for HIV-positive women; in-depth-interview for providers) were developed for the qualitative study and pre-tested with women and providers to check for simplicity, consistency and acceptability. The interviews were carried out in quiet discreet locations in the hospital's ART clinics. Audio-player was used in the local language; transcribed verbatim in Khmer and then back-translated into English. Because we intended to learn more factors related to the low use of HEI service, the questions were mostly open-ended to the participant's comments rather focus on behavior. We approached the text by making notes of participants' first impressions, thoughts, and initial analysis which become initial coding scheme. Codes then sorted into categories based on how different codes are related and linked. Conventional content analysis was done through NVivo 10. Quantitative and qualitative results were merged to triangulate the findings for divergence or convergence.
For binary or categorical outcome variables, the Chi-square (χ2) test was used. Variables at the p-Value < 0.05 were considered statistically significant.
This study was approved by the National Ethic Committee for Health Research of Cambodia (NECHR). Permissions to perform the study was obtained from NCHADS and the National Maternal Child Health Center. Informed consent was obtained from every respondent.
There were 1,118 PW registered in NCHADS' follow-up database, collected from 9 highest HIV-prevalence represented 25 provinces in Cambodia. The majority of women were aged between 26 and 35 (55.3%), followed by those 36 years and above (26.3%). Delivery data were analyzed for 1,060 cases (58 abortions); 72.2% of women had actual delivery from referral hospitals (RH), health centers (HC), private clinics, home delivery, in which 63.6% of women delivered at RHs. HEI services were analyzed among 1,037 cases (23 stillbirths/ neonatal deaths) (Table 1 and Figure 1).
Table 1: Characteristic of HIV-positive PW registered in follow-up database 2014-2016 (n = 1,118). View Table 1
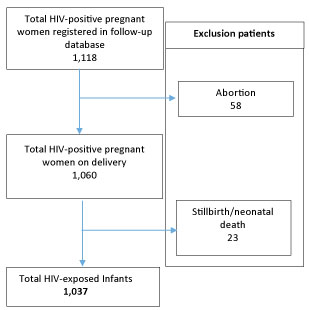 Figure 1: Schematic representation of quantitative study population and exclusion. View Figure 1
Figure 1: Schematic representation of quantitative study population and exclusion. View Figure 1
Our study revealed a low percentage of HEI services uses among the 1,037 HEIs (Figure 2).
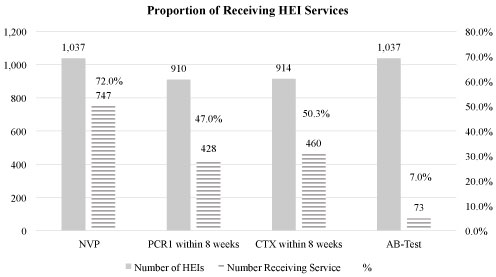 Figure 2: Proportion of receiving HEI services. View Figure 2
Figure 2: Proportion of receiving HEI services. View Figure 2
Table 2, Chis-square shows there is no statistical significant difference for the use of NVP, PCR1, CTX and AB-Test by women's age group and for the use of NVP and AB-Test by rural-urban status (p > 0.05).
Table 2: Proportion of receiving NVP, PCR1, CTX, AB-Test by selected variables, 2014-2016 (n = 1,037). View Table 2
In total, 72.0% had NVP. Among provinces, the proportion of having NVP are higher in Pursat, 91.7% followed by Siem Reap, 84.8% and the lowest is in Phnom Penh, 14.1%. Chi-square shows the percentage of using NVP is statistical significance at p < 0.001 across provinces (Chi-square = 181.98). The proportion of using NVP is high among those that had actual delivery, 95.0% and only 13.1% among unknown status. Chi-square shows the percentage of having NVP is statistical significance at p < 0.001 across delivery status (Chi-square = 690.85).
In total, 47.0% had PCR1. Among rural-urban, in rural, 50.7%, in urban, 43.4%. Chi-square reveals the percentage of having PCR1 is statistical significance at p < 0.05 across rural-urban status (Chi-square = 2.27). Among provinces, the higher percentage is in Siem Reap, 65.5% followed by Pailin, 60.0%, and the lowest uptake is in Phnom Penh, 7.6%. Chi-square shows the percentage of having PCR1 is statistical significance at p < 0.001 across provinces (Chi-square = 92.28). The proportion using PCR1 occurred only among actual delivery, 69.6%. Chi-square shows the percentage of having PCR1 is statistical significance at p < 0.001 across delivery status (Chi-square = 387.60).
Only 50.3% of HEIs received CTX. Among rural-urban, in rural, 54.6%, in urban, 46.1%. Chi-square indicates the percentage of having CTX is statistical significance at p < 0.05% across rural-urban status (Chi-square = 6.65). Among provinces, the higher percentage are in Kampong Cham, 69.7% followed by Siem Reap, 60.2% and Pailin, 60.0% and the lowest is in Phnom Penh, 8.9%. Chi-square shows the percentage of having CTX is statistical significance at p < 0.001 across provinces (Chi-square = 86.73). The proportion of having CTX is higher among actual delivery, 67.8%, among unknown status, 13.6%. Chi-square demonstrates the percentage of having CTX is statistical significance at p < 0.001 across delivery status (Chi-square = 235.56).
Only 7.0% of HEIs had AB-Test. Among provinces, there is no uptake in Kampong Cham and Phnom Penh. The higher percentage are in Pailin, 19.4% followed by Siem Reap, 18.2%. The lowest is in Kampong Som, 2.7%. Chi-square indicates the percentage of having AB-Test is statistical significance at p < 0.001 across provinces (Chi-square = 51.49). Among delivery status, the AB-Test utilization occurs only among actual delivery, 9.7%. Chi-square shows the percentage of having CTX is statistical significance at p < 0.001 across delivery status (Chi-square = 31.22).
Twelve HIV-positive PW and 26 HIV-positive post-delivery women were interviewed. Most of them were registered in the NCHADS's follow-up database in 2014-16. The majority of HIV-positive PW (86.8%) were 26 years old and over and all of them were on ART. The majority of women were housewives (34.2%) followed by workers (29%) and the rest (31.7%) were sellers, famers, entertainment workers or others. The majority of the women (66.0%) had up to a grade 6 level education and 34% of women had no formal education and could not read or write (Table 3).
Table 3: Characteristics of HIV-infected women (n = 38) in In-depth Interview. View Table 3
Of the nine providers, two were ANC counselors (midwives), one ANC/Maternity clinician (medical doctor) and six ART counselors (four medical doctors, one medical assistant, and two nurses). Two of the before mentioned providers were from three RHs, however, Siem Reap RH had three providers (Table 4).
Table 4: Characteristics of providers (n = 9) in In-depth Interview. View Table 4
The knowledge among HIV-positive women is inconsistent. Some women were aware of ways to prevent HIV-infection and that the infection from MTCT was not 100%. It was known by many women that ARV can prevent the transmission of HIV from MTCT.
"HIV can be prevented by using condom every time we have sexual intercourse; the infection of mother-to-child is not 100%", W33.
Most women expressed their treatment commitment because of their desire to have a child free of HIV. One of HIV-positive PW describes her efforts and side effects of ARV she felt.
"I am told that my child can be prevented if I take medicine regularly and consistently. I have tried hard through serious side effect in my first one month initiation", W37.
HIV-positive women have different levels of knowledge about the comprehensive package of HEI related services. Only among post-delivery women could describe what type of service are provided for HEIs. Some women could give correct information such as given NVP for about one month and a half and the final diagnostic HIV test done at 18 months that is consistent with the national policy. They failed to mention details about the schedule for receiving PCR test and CTX within two months of age. Some women described the way to follow-up their HEIs until they reached one year and above.
"to prevent HIV transmission from mother-to-child, first, give medicine [NVP] for about one month and a half to newborn baby, then bring the baby to see provider until the baby reached 18 months for HIV testing", W17.
"Give cotrimoxazole [CTX] until the baby had 3 times of negative HIV-tests", W9.
Some women could not describe clearly what services were needed for their unborn children when they were pregnant. They perspective on providers' messages about HEI services. Though some women could describe the need for services, the message they understood were not consistent with national policy particularly delivery mode and feeding option.
"I don't know what kind of services my child should receive; I think after birth I will ask to provider…but what I could recall I must deliver through cesarean section and feed by child formula milk", W38.
"I have not been told what services to give to my unborn child, I want to know" W2
One third of women provided NVP to their child for about one month and a half and then attended the PAC clinic on a monthly basis for one year and a half, which is consistent with national schedule policy.
"I give medicine to my child for about one month and a half and bring her to see provider monthly until she reached one year and a half as I had done with my previous one; my older child is negative, now is 2 years and a half", W17.
"My child was given syrup and drawn blood for testing. I was given two bottles of cotrimoxazole syrup that are used for 40 days. When I came next time they will give cotrimoxazole tablets", W29.
Some HIV-positive women did not bring their infants for HEI services based on the incorrect messages they receive from providers. Those messages are inconsistent with the national recommendation for the final HIV test.
"Test a child once again at one month and a half for the final test", W15
"My child was given medicine [NVP] at delivery, and I was not told about further service for my child", W13.
Some women expressed their challenges for bringing their children to receive HEI services as the lack of transportation and poor interaction with providers. Some women expressed their disappointment towards the attitudes of their healthcare providers.
"I am sick but I don't have money to travel to hospital; I owe Mototaxi 3000 Baht [90.8USD] up to now", W13.
"My husband threaten me to never bring my children to hospital because he hates providers. Once I gave birth in the car without help when I was referred to RH", W7 "I will never bring my kids to see providers due to the loud providers stared angrily at me, blaming me…no…unless they call for", W6.
All providers including ANC, maternity and ART counselors/clinicians were aware of the availability of PMTCT services and they were able to explain that all women identified HIV-positive should be given Option B+ immediately regardless of CD4 results.
"If the result is positive and she is still not on ART, we give her immediately the ARVs, Option B+", ART3.
Most ANC providers gave very limited information, or, did not explain how to use HEI services because they assumed women would not remember.
"We told HIV-positive women a few key messages. We did not explain the utilization of HEI services because we do not provide delivery service here [HC] and we could not remember well what service their HEI should receive; we expect the maternity staff would explain more", ANC2.
Most ART providers assumed that the messages should be explained well to all HIV-positive PW and it should be the role of ANC providers.
"Most cases, women were not aware of services [for HEIs]. It should be responsible by ANC [staff]. I doubt if women be given or they forgot the message, if they understand the importance of services their infants' needs, they will follow", ART8.
One maternity provider describes the process and services they routinely provide to HIV-positive women to transfer their infants for HEI service.
"At our site [maternity] we trained staff to provide service for HEI following the national guideline. We fill out the referral slip describing the mode and time of delivery event and name of drugs the HEI has received and then we give syrup [NVP] to HEI. We explain women how the drug use and we monitor them and send them to PAC service [Koma Angkor RH] through our networking", MAT7.
The information on HEI services was not explained clearly by ANC, maternity and ART providers. Some information was inconsistent with the national policy.
"What I remember…give [NVP] more; I told women to take CTX daily... baby tests once and again at 7 and half months. If HEI received PCR1 then I ask to bring HEI for antibody at one year and half, but I lost a lot of children for final test", ART3.
Some providers were able to explain the reasons that prevent women from bringing their children to clinics.
"Lost HEIs, most cases occurred among women who do not have married certificate, factory workers and did not disclose their HIV-status. We want ANC and maternity to cooperate with our clinic [ART clinic] and use one message", ART3.
Our study indicated a low use HEI services in Cambodia. Of all HEIs, 72.0% received NVP, 47.0% had PCR1, 50.3% received CTX and 7.0% had AB-Test. These data suggest three important findings:
First, the HEI service utilization in our analysis was higher to that seen nationally, except the uptake of NVP (72.0% versus 75.0%), the utilization of PCR1 (47.0% versus 35.0%) and CTX (50.3% versus 41.3%). Our finding may provide more accurate results than the national database as the analysis included additional data from 5 provinces and EID database. Of note, for AB-Testing there was very limited reports from the national program, but it was available in the provincial PMTCT database. AB-Testing are important for monitoring the final diagnosis of HEIs; unfortunately only 7.0% of HEIs had undergone a final HIV test. There was a great lost-to-follow-up (LTFU) and/or missing of HEI services particularly for PCR, CTX usage and AB-Test that remains a significant barrier to achieving eMTCT program outcomes. LTFU at each stage of the cascade should be improved even our data showed higher performance than some countries that have similar challenges. For example, Thailand 9% [13], Ethiopia 22.2% of HEIs were lost in care and treatment and 53.3% of those infants born at facilities did not receive any prophylaxis [14]. Loss of HEIs occurred at all stages of PMTCT cascade in a Malawi's study, where 12.2% of HEIs were not yet enrolled into care by the age of 6 months and only 3.8% enrolled after the age of 12 months. A study in Nigeria indicated that the greatest loss occurred prior to delivery care (21.0%), with a further 16.0% lost prior to first infant visit and lost for PCR1 47.0% [15]. Our findings shows the use and loss HEI service were statistical significance among provinces at p < 0.001. The higher uptake of NVP are in Pursat and Siem Reap while the higher uptake of PCR1 are in Siem Reap and Pailin. The highest use of CTX are in Kampong Cham and Siem Reap while the highest utilization of AB-Test are in Pailin and Siem Reap. The lowest use of HEI service are in Kampong Som and Phnom Penh. This finding is important for the national program to further target for successful intervention as the common use of HEI serivces has occurred in Pursat, Siem Reap, Pailin provinces. These findings were consistent with our qualitative findings.
Second, the lack of mother's knowledge about HEI services is clear from the interviews and resulted in low uptake HEI service suggested by the quantitative analysis. Our qualitative study found some HIV-positive women were aware of HIV transmission and prevention from MTCT and the understood that likely in some African settings, the transmission rate was not 100% [5]. Most women believed that ARV could prevent MTCT transmission as supported by the fact all women were on ART. However, only a few women had an awareness of HEI service and those were described only by post-delivery women who received education from maternity wards or they have had experiences from their own previously exposed children. Information and counseling from ANC and ART providers were inconstant and confusing. This confusion could possibly be due to the unclear messages from ANC providers. Some women were not aware of HEI services but they would do what they were told. They had a low level of understanding, or, it because of the fear to talk to providers. In some countries, a negative perception of HEI service by women may prevent HEIs from receiving services [12]. Counseling should be improved to empower HIV-positive women to closely care for their children as found in Cote d'lvoire and inter-personal communication and confidentiality can significantly improve health service delivery in all facilities [14]. Some women described the way to follow-up their children until their children reached one year and above. Most women could not explain what kind of services their children should receive when they were pregnant. This may be related to confusion about roles and responsibilities among ANC, maternity and ART providers in distribution and promotion of HEI services. ANC providers perceived that women are easy to forget messages; they expected the message should be done at maternity whereas ART providers thought the message should be done at ANC setting. Our quantitative study indicates only 63.6% of HIV-positive PW had actual delivery at referral hospitals, the rest of women give birth at home, HCs, or private clinics would have missed the opportunity bringing their children for HEI services. The HEI information dissemination might mostly done at maternity settings which is concur with quantitative study, the percentage of having NVP, PCR1, CTX, AB-Test are high and had statistical significance at p < 0.001 across delivery status by Chi-square test. Among actual delivery, 95.0% had NVP, 69.6% had PCR1, 67.8% had CTX and 9.7% had AB-Test. The best approach is to access all HIV-positive PW to deliver at referral hospitals and improve delivery documentation.
Finally, the practice of having HEI services were poor among HIV-positive women. Some women who hide their HIV-positive status would have missed HEI service. Those included women that do not have married certificate and factory workers. Majority of women did not receive message from providers did not bring their HEIs to services. There were also women who wanted to bring their HEIs for services but threatened by their husbands to not bring the child for care due to they perceived poor interaction between providers. This practice could result in negative consequences for HEIs to receive important services [15]. A portion of HIV-positive PW did not show up at RHs for delivery; this may represent a lack of transportation or fear of disclosure of HIV-status which is similar to findings in several published literature reviews [16].
This is a first report showing gaps in knowledge of services for HEIs identified for both providers and women in Cambodia, which may have contributed to a low uptake of ARV-prophylaxis, PCR1, CTX and AB-Testing. Strengthening data and information systems is needed to better understand service delivery and prevent LTFU. To minimize the ambiguity of information passed from the providers to the HIV-positive PW, feedback mechanisms and routinely checking of patients' awareness and satisfaction should also be monitored and improved. The benefits to all HEIs in receiving services according to the national policy should be strongly promoted. HIV-positive women should be empowered to disclose their status. Clear and consistent messages of HEI services should be done repeatedly at ANC, delivery and ART settings.
The authors would like to thank the HIV-positive women who involved in the study in ROKA, Sompov Loun, Social Health Clinic, Siem Reap Referral Hospitals for their enthusiastic participation. We also deeply thanks to Dr. Therese Delvaux, Dr. Jennifer Bohl for the review and edition, International University, NCHADS, NMCHC for their strong supports.
No conflict of interest.