Psychiatric training consists of core psychiatry training for three years during which trainees has to pass the College membership examination MRCPsych before they enter the Old Age Psychiatry specialty training for further 3 years. The curriculum for specialist training in Old Age Psychiatry is being reviewed by the Old Age Faculty of the Royal College of Psychiatrists.
To gather information from Postgraduate Deaneries (Old Age Psychiatry Senior Specialty Trainees and their Trainers) about the current training in old age psychiatry and related specialties such as Geriatric Medicine, Neurology, Palliative Care and Neuropsychiatry. E-mails with a link to the survey were sent by the Faculty of Old Age Psychiatry manager to 16 Deaneries across the UK. The surveys were open for 6 weeks and closed on 31st January 2017.
Old Age Psychiatry Trainers (n = 55 responded from 16 deaneries) reported that ad hoc training in 53% of geriatric medicine, neurology (49%) and palliative care (54%). 95% of trainers thought the old age curriculum should reflect the need for geriatric medicine, neurology, palliative care, and neuropsychiatry training. 44 Trainees responded to the survey from 15 deaneries (28% were ST4, 38% ST5 and 34% ST6). Of those responded, 39% felt confident in managing physical problems and common long-term conditions such as falls, incontinence and delirium, 50% felt slightly confident, 11% felt not confident.
The results of this survey suggest there is general agreement that these specialties are important and relevant to Old Age Psychiatry. Training should be mandatory as part of the curriculum.
Curriculum, Competency, Trainee, Trainer, Medical education, Geriatric medicine, Neurology, Palliative care
Trainees enter Old Age Psychiatry Specialty Training after successfully completing both the Foundation Training Programme (and having evidence of equivalence) and the Core Psychiatry Training Programme. The advanced curriculum for practice provides the framework to train Consultant Psychiatrists in the UK. The current Curriculum for specialist training in Old Age Psychiatry was developed in 2010 and updated in 2016. Within the curriculum there is no link with geriatric medicine, palliative medicine, neurology or neuropsychiatry. The curriculum is currently being reviewed by the Royal College of Psychiatrists. It is therefore timely to consider what changes might be appropriate [1].
The General Medical Council (GMC) in 2010 [2] produced guidance on "Treatment and care towards the end of life: Good practice in decision making" and in 2012 "Leadership and management for all doctors" [3]. In 2015, [4] the Old Age Faculty produced its new criteria that was approved by the College and the GMC after extensive consultations. In 2016, the GMC approved the new Liaison Curriculum in both Adult and Old Age psychiatry. In 2016, the GMC asked the College to map all curricula to the GMC "Good Medical Practice". From 1st July to 27th September 2015, the GMC and the Academy of Medical Royal Colleges consulted jointly on a draft framework for generic professional capabilities (GPCs) [5]. The nine-domain framework aims to identify, simplify and clarify the important core professional capabilities doctors should possess at specialist registration. In 2016, the Royal College of Psychiatrist set up the Gatsby/Wellcome Neuroscience Project Implementation Group to ensure that neuroscience is reflected in the curriculum and examination syllabus. Also, in 2016, OP100 [6] report "Improving the physical health of adults with severe mental illness: Essential actions" was published by the Academy of Medical Royal Colleges and the Royal Colleges of General Practitioners, Nursing, Pathologists, Psychiatrists, Physicians, the Royal Pharmaceutical Society and Public Health England. The report highlighted that there should be the same level of physical healthcare available to people with severe mental illness as is available to members of the general population. The Old Age Faculty has been working closely with the British Geriatric Society and the joint working highlighted the need for more integrated curriculum to reflect the new NHS. The Faculty in 2016 produced a report [7] on Integrated Care that highlighted the need for more training in integrated services. As old age psychiatrists work closely with neurologists and neuropsychiatrists, there is a need for our higher trainees to understand neuroscience. Increasing focus and developments in this area may also potentially increase recruitment of old age psychiatrists.
The next 10 years will see substantial increases in the number of older people and in the percentage of the population that they represent. There will be an increase in those over 60 from 14.9 (2014) to 21.9 million by 2039. This is likely to be accompanied by an increase in the prevalence of recognised mental illness amongst an ageing cohort who are more attuned to mental health issues and are more demanding good services than previous generations. As a result of these two trends the number of older people with identified mental illnesses is expected to triple over the next 25 years. Maintaining the status quo is untenable because the need is rapidly increasing. The only solution is a radical change in how old age psychiatry is organised and delivered. The rarefied skill pool must be deployed to manage older people with physical health problems, functional mental illness and those with behavioural and psychological symptoms of dementia.
In an editorial, Fisher and Teodorczuk [8] reported that the co-occurrence of physical and mental ill health means there is considerable overlap between the patients that geriatric medicine and old age psychiatry service. The authors also reported that both specialties face an identity crisis and recruitment challenges. The editorial highlighted the greater demand and contribution of the psychiatry for older people to the care of older people.
People and services are changing and the field of Old Age Psychiatry is no exception. People are ageing and co-morbidities are becoming more common. According to a Department of Health document [9] 'Comorbidity is one of the most important issues facing health systems in the developed world today and the single disease approach is unable to address this problem appropriately'. That statement is completely understandable considering 'around 25% of hospital inpatients have a diagnosis of dementia' [10]. Services are constantly changing form. In recent times, there have been discussion and plans for ageless services, GPs taking responsibility for cholinesterase inhibitors and it is likely other changes will be considered and implemented in the future [11]. The current Old Age Psychiatry trainees will provide the consultants of the future and will need to be able to respond to these changing demands. It is therefore important Old Age Psychiatry training and the guiding curriculum are relevant to the challenges that will face trainees in their future carers.
Trainees should have two sessions a week devoted to special interest sessions which allow personal development in a 'clinical or clinically related area of service which cannot be provided within the training post, but which is of direct relevance to the prospective career pathway of the trainee' [1]. There is not a clear consensus on how this special interest is used and if all trainees should gain experience in areas such as geriatric medicine, neurology, palliative care and neurology.
The aim of this survey was to gather information from Old Age Psychiatry trainees (ST4-ST6) and trainers about the current training in old age psychiatry and related specialties such as Geriatric Medicine, Neurology, Palliative Care and Neuropsychiatry. This survey will enable a review of the current curriculum and submission of a new old age psychiatry curriculum to GMC in 2017.
The survey was developed for both Old Age Psychiatry trainees and trainers. E-mails with a link to the survey were sent by the faculty of old age psychiatry manager to 16 Postgraduate Deaneries across the UK. The survey was distributed in a survey monkey format. The survey did not collect demographic data such as age, and gender as the focus was on capturing the training experience and to encourage response rate; however, the survey collected data such as year of training and deanery as well as factual information on time spent in the above four areas and the training arrangements for these e.g. formal, outpatients or ad hoc. Ad hoc training could be opportunistic, temporary, provisional, no-systematic, non-generalizable, and inadequate planned.
After consultation with the Cardiff Local Ethical committee by telephone, we were advised that no Ethical Approval was warranted as the survey is considered as service evaluation, is anonymous and is about training experience. The survey was open for 6 weeks and closed on 31st January 2017. Both trainees and trainers were asked to give their consent for their comments to be used as part of the publication e.g. by taking part in this survey, you consent for publication.
Statistical analyses were used when relevant e.g. Figures were done using excel, and Chi-square test were used to assess level of significance of non-parametric data. We looked at the survey responses, added comments and the results were interpreted using a summative content analysis to interpret meaning from the content of text data and, hence, adhere to the naturalistic paradigm (Table 1 and Table 2 used to summarise qualitative content) and focus was on themes such as the confidence in dealing with physical health problems, the training experience in dealing with physical health and end of life care issues, training arrangement for the related specialties, good examples of joint training and any recommendations suggested.
Table 1: Examples of good training opportunities. View Table 1
Table 2: Additional comments. View Table 2
55 Old Age Psychiatry Trainers responded from 16 deaneries. During the higher old age psychiatry training period (Figure 1), ad hoc training was evident in 53% of geriatric medicine, neurology (49%) and palliative care (54%). In neuropsychiatry, the largest proportion was available as outpatients (35%). Only 9% of geriatric training, 12% of neurology training, 11% of palliative care training and 26% of neuropsychiatry training was formal.
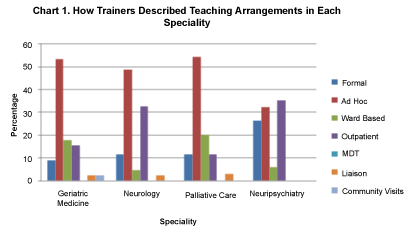 Figure 1: How trainers described teaching arrangements in each speciality. View Figure 1
Figure 1: How trainers described teaching arrangements in each speciality. View Figure 1
Figure 2 shows the largest proportion of trainers estimated that during the whole higher training in old age psychiatry trainees spent 6-10 hours in geriatric medicine (24%) and 1-5 hours in neurology (26%). 46% of trainers estimated 0 hours are spent in palliative care and 41% estimated 0 hours are spent in neuropsychiatry.
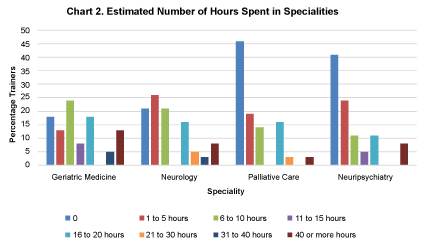 Figure 2: Estimated number of hours spent in specialities. View Figure 2
Figure 2: Estimated number of hours spent in specialities. View Figure 2
95% of the responding trainers thought the old age curriculum should reflect the need for geriatric medicine, neurology, palliative care, and neuropsychiatry training. 51% of respondents made suggestions of improvement to the current curriculum such as the curriculum should include the above specialties. For example, make them explicit areas to be checked in Annual Review of Competence Progression and there needs to be formal placements in neurology. However, we need to ensure that there is time and resource to ensure these opportunities. There was a requirement for more opportunities in other areas such as neuroimaging, biomarkers and it would be far more useful to have some neuropsychiatry and geriatric medicine competencies.
44 Trainees responded to the survey from 15 deaneries (28% were ST4, 38% ST5 and 34% ST6). Of those responded, 39% felt confident in managing physical problems and common long-term conditions such as falls, incontinence and delirium, 50% felt slightly confident, 11% felt not confident. Currently, trainees have one day a week to develop psychotherapy, research and special interest skills. However, the links with other related specialties tends to rely on special relationships with "friendly" colleagues rather than be structured part of training and development. Trainees reported that there should be some minimum requirements in terms of trainees understanding and experience with medicine, palliative medicine, neurology and neuropsychiatry. 100% had an allocated day a week for research/special interest in their speciality training.
Figure 3 shows that 98% were currently conducting research or doing a special interest. Only one respondent (2%) said there was a recognised cross speciality programme in their region for training events, 43% did not know. Only 5% (2) of respondents said there was a shared care ward in their hospital, 14% did not know, 82% said there was not a shared care ward. 57% said there was an opportunity for shared CPD events, lunchtime teaching or shared teaching by trainees to medical students in their hospital, 14% did not know if there were such opportunities and 30% said there were no such opportunities. 50% were aware of the British Geriatrics Society (BGS) and their meetings, 84% would be interested in attending a BGS meeting. 37% intend to do research or special interest in the area of geriatric medicine, 33% in liaison psychiatry, 24% in neurology, 16% in neuropsychiatry, 14% in palliative care, 14% in movement disorder clinic, 5% in frailty assessment clinics by geriatricians and 51% in another area.
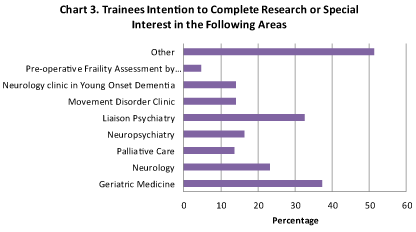 Figure 3: Trainees intention to complete research or special interest in the following areas. View Figure 3
Figure 3: Trainees intention to complete research or special interest in the following areas. View Figure 3
Chi-square showed that neurology was more available than neuropsychiatry (yes/no), X2 = 20.333 (2, N = 54), P = 0.000; however, neuropsychiatry was more available than palliative and geriatric medicine, X2 = 46.286 (1, N = 54), P = 0.000. Also, geriatric medicine training was more available than palliative medicine, X2 = 10.111 (2, N = 54), P = 0.006.
Figure 4 demonstrates that during the whole higher old age psychiatry training programme most respondents had spent 5 hours or less attached to the following specialities. 62% spent 5 hours or less in geriatric medicine, 79% spent 5 hours or less in neurology, 87% spent 5 hours or less in palliative care, 90% spent 5 hours or less in neuropsychiatry. Chi-square showed that trainees spent more time in general in geriatric medicine compared with neurology, X2 = 83.053 (4, N = 38), P = 0.000, neuropsychiatry, X2 = 56.000 (2, N = 39), P = 0.000 and palliative medicine, X2 = 51.231 (2, N = 39), P = 0.000.
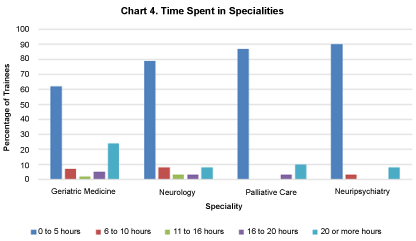 Figure 4: Time spent in specialities. View Figure 4
Figure 4: Time spent in specialities. View Figure 4
55% organised the above attachment themselves, 41% said this was not applicable. Most of these training opportunities were ad hoc (Figure 5). In geriatric medicine, 39% was ad hoc and 26% in inpatient setting. In neurology 47% were ad hoc and 33% in outpatients. In palliative care 47% were ad hoc and 27% formal. In neuropsychiatry 50% was ad hoc and 19% in the inpatient setting.
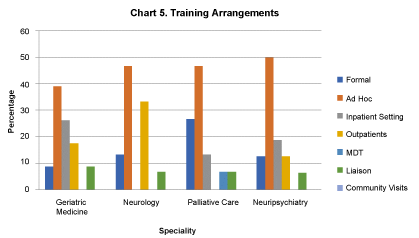 Figure 5: Training arrangements. View Figure 5
Figure 5: Training arrangements. View Figure 5
Trainees were asked about the time spent (in hours) with different members of the multidisciplinary team such as consultant, SpRs, Core Trainees, Foundation Doctors, and other members of the MDT. During their attachment, more trainees spent time with the consultant than SPRs, X2 = 13.000 (2, N = 24), P = 0.002; Core trainees, X2 = 8.273 (2, N = 22), P = 0.016; FY1 & FY2 doctors, X2 = 11.636 (1, N = 22), P = 0.001; and members of the multidisciplinary teams, X2 = 10.333 (3, N = 24), P = 0.016.
Formal teaching during the attachments in the above specialties was reported by 68% of trainees as did not include formal teaching on core topics, 3% said there was formal teaching on core topics and 24% said they did not know. Some of the reasons identified for the lack of such training future planning as a special interest, lack of availability or hard to organise due to clinical work. One respondent said it was not on the curriculum. 54% that did not have such attachments did intend to have them in the future, 11% were unsure, only 3% said they did not intend to have such attachments in the future.
79% (N = 43) of trainees thought that the Old Age Curriculum should reflect the need for geriatric medicine/neurology/palliative care/neuropsychiatry training. The final question asked respondents for any additional comments (Table 2).
This survey is important in gathering the general views of trainers and trainees about what to include in the future curriculum. The majority of responses reflected the need to include geriatric medicine, neurology, palliative care, and neuropsychiatry training. Whilst 95% of trainers and 79% of trainees thought the old age curriculum should reflect the need for the above specialities in training the availability of these opportunities varied, with 81% of trainers reporting available opportunities in geriatric medicine, 67% in neurology, 57% in neuropsychiatry, 54% in palliative care and only 22% in preoperative frailty clinic by geriatricians.
100% of trainees have an allocated day a week for research or special interest. However, results suggested that the majority of trainees are not spending time in the main 4 speciality areas and the majority reported less than 5 hours experience in each area. Most of these training opportunities were ad hoc, although some had formal attachments.
A number of trainees and trainers named specific places where such attachments were being done well, however, caution was also given about the availability of these options and the difficulty of meeting competencies.
The Old Age Faculty has been working closely with the British Geriatric Society and the joint working highlighted the need for more integrated curriculum to reflect the new NHS. There is a need for our higher trainees to understand neuroscience and an increasing focus and developments in this area may lead to increase potential recruitment and luring potential old age psychiatrists into being neuropsychiatrists.
This survey supports the proposal made by Fisher and Teodorczuk [3] for shared training pathway where experience is gained in geriatric medicine and the psychiatry for older people. However, the authors recommend that within the first year of psychiatry for older people higher training to be more structured and include a three-monthly rotation in the above specialties. The transferred skills will improve the clinical care of the patient and will also improve understanding and working relationships with other specialties. Integrated care is vital for the future of older people care. Watmough, et al. [12] found that 5 years post-qualification the majority of trainees felt their career choice was primarily dictated by their postgraduate experience. A continuum of improving curricula between undergraduate and postgraduate training in the psychiatry for older people is needed. Bennett, et al. [13] reported that medical school undergraduate curricula for old age psychiatry advance in line with future demographic needs and more curriculum space needs to be given to old age psychiatry. The survey also supports the views of the Faculty of Old Age psychiatry in its integration report that recommended the workforce for physical and mental health services needs to be fit for purpose and have appropriate skills to deliver integrated care [7]. Greater collaboration and establishing working relationship between disciplines are important to arrange mutually beneficial training experiences, buddy system between specialities, and encourage trainees to attend joint conference and teaching events. There is also a need for better online resources that include transferrable knowledge and skills.
It is also important to recognise that we need to rekindle the passion, cohesion and vision and to change our idea of what old age is and evolve into different service structures [11].
Finally, to improve recruitment and workforce in old age psychiatry it is important that we develop our curriculum to attract more trainees, to reflect the changing demographics and shape of old age psychiatry. We need to be adaptable and integrated in our approach to the care and training.
This is a timely survey that will help inform curriculum changes. Despite the low response rate given the population of trainees and trainers in Old Age Psychiatry, the spread of respondents across deaneries and the four devolved countries means the sample is likely to be representative, although it is also necessary to recognise respondents probably had an interest in the curriculum which is why they participated. It may be purely that they need to abide by the curriculum, but it may also be that they have particular issues with the curriculum.
One limitation in relying on trainers to estimate time spent by trainees in certain specialities may be considered unreliable. In the trainee survey time spent in each speciality may be impacted upon year of training, ST4 trainees are understandably going to have spent less time in each speciality and this could skew the results. Another limitation is that the survey did not assess training needs based on prevalence of specific problems in the elderly population as the survey aimed at gathering basic information about the current training in old age psychiatry and related specialties such as Geriatric Medicine, Neurology, Palliative Care and Neuropsychiatry.
Nevertheless, this survey provides a timely look at opinions on the Old Age Psychiatry Curriculum and as some respondents highlighted any changes need to be achievable and therefore gathering opinion from those it might affect is of paramount importance. It will be interesting to find out how this survey relates to curricula across the world and whether a worldwide generic curriculum can be achieved.
Aziz had the idea and did statistical analyses. All authors developed the survey, analysed the data and contributed to the paper writing.
None.
None.