Blastomycoses dermatitidis is a fungal organism endemic to the eastern United States. This organism is thought to grow in soil and decaying wood, and exposure with inhalation of the spores can result in blastomycosis, a potentially life-threatening disseminated infection. We present a case of an 11-year-old female who presented to our institution with headaches and left-sided facial swelling, who was ultimately found to have blastomycosisof her left zygomatic bone.
Skin and soft tissue infections (SSTIs) are one of the most common reasons for hospital presentation in the pediatric population. Within the past decade, there has been an increase in the number of SSTIs. Common pathogens include Streptococcus, Staphylococcus aureus (both MRSA and MSSA), as well as gram-negative and mixed infections [1]. Fungal infections are far less common, however, their incidence is also increasing. Common fungal pathogens include Candida albicans and Aspergillus species. Such infections are typically seen in immunocompromised hosts, and fungal infections often occur in an opportunistic fashion [2]. Blastomycosis typically presents as a primary lung infection, which can progress to a disseminated phase. In the disseminated phase, the yeast cells become trapped in capillary beds which lead to damage in various areas, including the skin, genitourinary tract, the central nervous system, as well as the bone marrow [3]. We present a case where a child was found to have isolated blastomycosis of her left zygomatic bone.
An 11-year-old female presented to Comer Children's Hospital of University of Chicago Emergency Department (ED) in April 2019 after 1 month of headache and left-sided facial swelling that was present for 2 weeks. She was initially treated at an outside facility for both a nasal polyp as well as left acute otitis media. She was given Amoxicillin and Zyrtec but had no improvement in her symptoms. She then developed left orbital pain with both medial and lateral gaze and woke up on the morning of her presentation with her left eye completely shut. In our ED she had normal vital signs and induration over her left zygomatic arch with left upper lateral and lower lateral eyelid edema. She had laboratory studies drawn that demonstrated a normal white blood cell count of 7 K/μL and an elevated sedimentation rate (ESR) 61 mm/hr, and C reactive protein (CRP) 32 mg/dL. A CT maxillofacial without contrast was performed and demonstrated an abscess in the left facial soft tissues with suggestion of osteomyelitis of the underlying zygoma and zygomatic arch, as well as fluid in the left maxillary sinus (Figure 1). An MRI of the orbits was completed which demonstrated a loculated fluid collection of the left facial soft tissues over the zygomatic arch with inflammatory changes that extended to the preseptal soft tissues and retromasticator space (Figure 2). There was also edema and abnormal signal replacement of the fatty marrow of the adjacent zygomatic arch, zygoma, and orbit. Of note, there was mucosal thickening of bilateral maxillary and left frontal sinuses. She was then admitted and started on Clindamycin and Ceftriaxone. The Ophthalmology and Infectious Disease teams were also consulted at that time. The Ophthalmology exam did not demonstrate any ocular involvement. Over the next 48 hours the patient had improvement in her induration as well as pain. There were no signs of any periorbital swelling and no difficulty with eye movement; her CRP was downtrending as well. She was discharged home with Clindamycin and instructed to follow-up in one week.
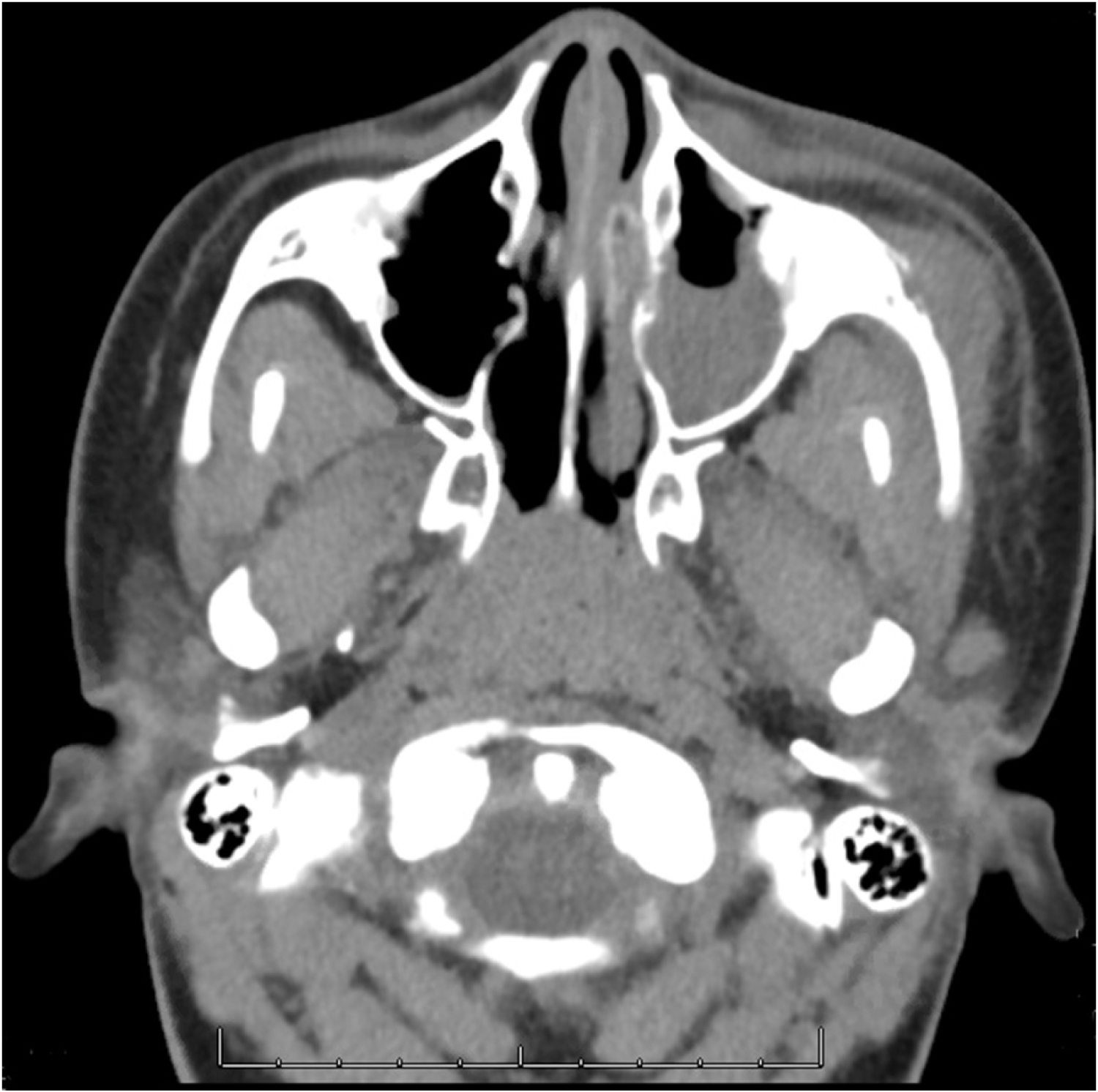 Figure 1: CT maxillofacial without contrast on initial presentation demonstrating a soft tissue density with surrounding fat stranding in the left facial soft tissues measuring 2.7 × 1.3 × 3.8 cm, consistent with abscess. There is also lucency, permeated texture, and a periosteal reaction of the leftzygoma and zygomatic arch adjacent to this region suggestive of osteomyelitis.
View Figure 1
Figure 1: CT maxillofacial without contrast on initial presentation demonstrating a soft tissue density with surrounding fat stranding in the left facial soft tissues measuring 2.7 × 1.3 × 3.8 cm, consistent with abscess. There is also lucency, permeated texture, and a periosteal reaction of the leftzygoma and zygomatic arch adjacent to this region suggestive of osteomyelitis.
View Figure 1
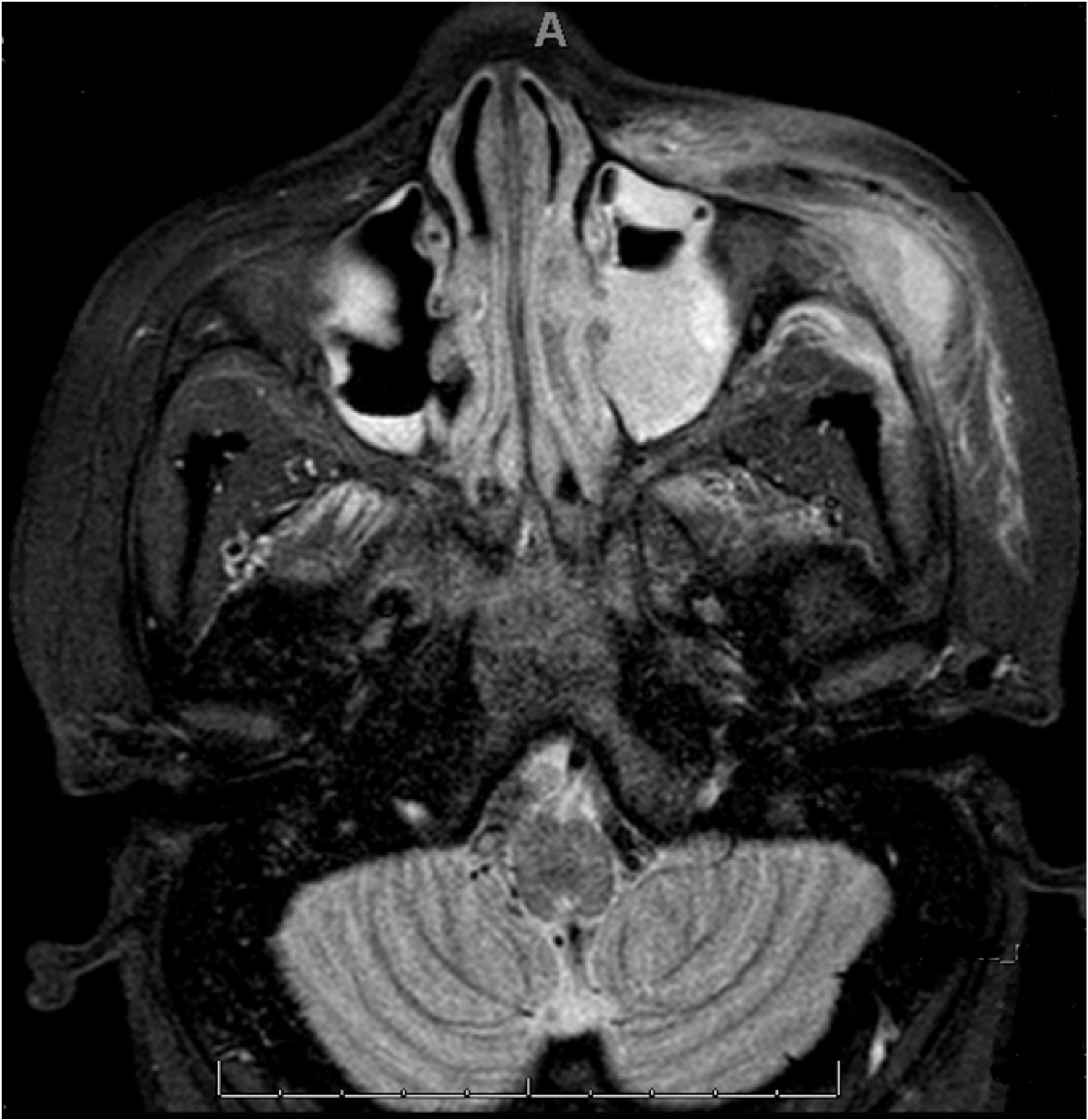 Figure 2: MRI orbits with and without contrast demonstrating a 2.0 × 1.4 × 1.6 cm loculated fluid collection in the left facial soft tissues with soft tissue swelling, edema, and fat stranding suggestive of infection extending to the left cheek and left preseptal and periorbital soft tissues. There is also pathologic replacement of the normal fatty marrow of the adjacent left zygomatic arch, left zygoma, and lateral wall of the left orbit suggestive of osteomyelitis. There is bilateral maxillary sinusitis noted, left more severe than right.
View Figure 2
Figure 2: MRI orbits with and without contrast demonstrating a 2.0 × 1.4 × 1.6 cm loculated fluid collection in the left facial soft tissues with soft tissue swelling, edema, and fat stranding suggestive of infection extending to the left cheek and left preseptal and periorbital soft tissues. There is also pathologic replacement of the normal fatty marrow of the adjacent left zygomatic arch, left zygoma, and lateral wall of the left orbit suggestive of osteomyelitis. There is bilateral maxillary sinusitis noted, left more severe than right.
View Figure 2
At her follow-up appointment, her left facial edema had returned, and it was decided to have her undergo repeat imaging. A CT neck with contrast was completed, which demonstrated enlargement of the previously described fluid collection overlying the left zygoma and an increase in osteolysis of the left zygomatic bone (Figure 3). She underwent an incision and drainage of the fluid collection and debridement of the tissue. This was then sent for aerobe/anaerobe culture, AFB, and fungal culture and she was started on Unasyn due to the concern for osteomyelitis. On post-operative day 1, her fungal smear was positive for yeast resembling Blastomyces dermatitidis. Infectious disease was again involved in her care and she was started on oral Itraconazole and a chest X-ray, urine Histoplasma antigen, and Histoplasma Ab were checked and were all unremarkable. She was discharged home on post-operative day 2 with a one week follow-up and a one year prescription of Itraconazole.
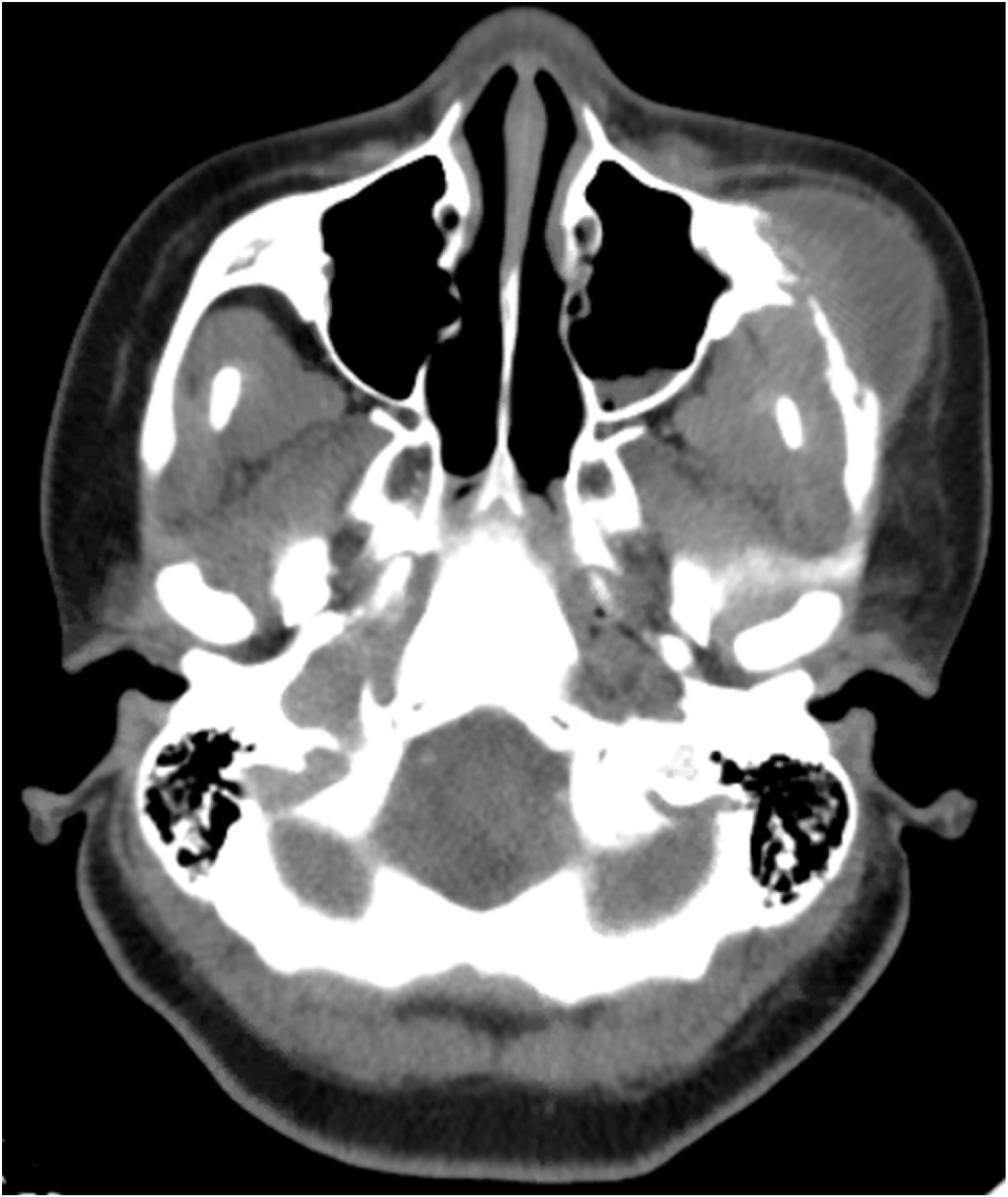 Figure 3: CT neck with contrast performed at follow-up demonstrating progression of findings related to osteomyelitis of the left zygoma with inflammation of the left subperiosteal inferotemporal orbit and left anterior masticator space, as well as left maxillary sinusitis and left parotid lymphadenopathy.
View Figure 3
Figure 3: CT neck with contrast performed at follow-up demonstrating progression of findings related to osteomyelitis of the left zygoma with inflammation of the left subperiosteal inferotemporal orbit and left anterior masticator space, as well as left maxillary sinusitis and left parotid lymphadenopathy.
View Figure 3
Blastomycosis dermatitidisis a dimorphic fungus that is endemic to the Midwest, specifically to the Mississippi and Ohio River valleys as well as the Great Lake Regions [3]. Infection is acquired by inhalation of organisms that occur as molds in the environment, which then convert to yeast once in the lungs [4,5]. This dimorphic fungus has been found in soil, decaying vegetation and pigeon manure, however it is hard to isolate it in the environment [6]. The infection is most commonly seen in middle-aged males, which can possibly be explained by an increased exposure in the environment through work or activities [6]. Blastomycosis most commonly infects the lungs, and symptoms appear after a 2 to 6 week incubation period [5].
Blastomycosis in children represents 3-10% of all reported cases [7,8]. The diagnosis of Blastomycosisis often delayed in pediatric patients, which may explain why disseminated disease is more common at the time of diagnosis [9].
Disseminated extrapulmonary Blastomycosis most commonly involves the skin, bones, GU tract, and central nervous system and disseminates via hematogenous spread [10]. Dissemination to osteoarticular structures occurs in approximately 25% of extrapulmonary infections, with the most common sites including long bones, lower limbs and axial skeleton, followed by vertebrae [10,11]. The most common presenting signs and symptoms of osteoarticular spread are bone pain, erythema or warmth, and possibly a draining sinus.
Bone is the second most common site for disseminated Blastomyces infection, and has been seen in ~5-25% of patients. The organism infects the metaphyseal and epiphyseal portions of the bone [12]. Osseous infections can occur at any bony site in the body. The facial bones are very rarely involved. Thomas, et al. found Blastomyces in the hard palate of an immunocompromised host. In a survey covering three decades of Blastomyces cases, skull and facial bone involvement made up 23% of the osseous involvement [12,13]. Albarillo, et al. reported a case of mandibular Blastomycosis occurring in an immunocompetent patient in Illinois without pulmonary involvement, which ultimately required right hemimandibulectomy [14]. Our particular case is unusual in that the patient presented with osseous Blastomycosis without pulmonary complaints. To our knowledge, there has not been a report of Blastomycosis involving the zygomatic bone in the literature.
All patients with Blastomycosis should receive antifungal therapy regardless of the clinical presentation due to the high likelihood of progression or recurrence if left untreated [15]. This is further guided by the severity of disease, presence of CNS involvement, and the host immune status. Itraconazole is first line for mild to moderate Blastomycosis, with a treatment duration of 6-12 months [16].
Pediatric soft tissue infections of the head and neck are a relatively common occurrence. Pathogens typically include Streptococcus, Staphylococcus aureus, as well as gram-negative, and mixed infections. However, fungal sources are a rare possibility and should remain on the differential in the setting of a patient who fails to improve on traditional antibiotics. A multidisciplinary approach can be beneficial when treating patients with uncommon infections, and long-term treatment and follow-up is often warranted.