Dengue virus infection in pregnancy has been associated with miscarriage, intrauterine fetal death, and secondary neonatal impairment, including prematurity and vertical transmission of the virus.
This study reports a fatal outcome due to confirmed dengue, resulting in maternal and fetal death. Dengue should be included in the differential diagnosis of HELLP syndrome in hyperendemic areas such as Brazil, and RT-PCR in paraffin-embedded tissue used to confirm the diagnostic, especially when these samples are the only available material.
Dengue, Maternal death, Pregnancy, Pathology
Dengue Virus (DENV) is an arthropod-borne virus belonging to the Flaviviridae family, genus Flavivirus and has four antigenically distinct serotypes (DENV 1-4). Brazil is considered hyperendemic for dengue, and all serotypes have been identified. The occurrence of dengue infection in pregnancy has been reported in the literature since 1948 and a recent systematic review [1] reported several cases of antenatal complications associated with dengue, including miscarriage, stillbirth, and premature deliveries. In 2013, seven laboratory confirmed cases (serology, RT-PCR, and immunohistochemistry) of vertical transmission were reported in Rio de Janeiro [2].
We report evidences of vertical transmission resulting in maternal and fetal death, in a dengue infected pregnant woman diagnosed after death.
Since 2009, after the reporting of 13 pregnant women with dengue in the state of Rio de Janeiro [3] an intensified surveillance of dengue in pregnant women had been recommended, and a guideline to the care and monitoring of infected pregnant women by healthcare workers was created along to the recommendation to the placenta pathological examinations of all suspected cases in the reference maternities of the state. In November 2010, a 23-year-old pregnant woman was admitted to a maternity in Rio de Janeiro, complaining of lower abdomen pain, vomiting and diarrhea. The symptoms had started at the same day and fever has not been reported. The fetal heartbeat was audible at the admission, but after lipothymy and maternal hypotension (BP = 120 × 80 mmHg at the moment of admission, at 1:30 pm; BP = inaudible during lipothymy at 5:20 pm; BP = 70 × 50 mmHg after 500 mL of Ringer’s lactate administered; BP = 70 × 50 mmHg at 6:33 pm), the obstetric evaluation revealed inaudible fetal heartbeat. The ultra-sound showed a single 32-33-week-old apparently dead fetus’, with no active movements; oligohydramnios and a reduced detached premature placenta with no flow at color Doppler and free fluid in the abdominal cavity. Hemogram data is found in Table 1. The woman evolved into shock and a cesarean section was performed. During the intervention, a large blood extravasation into the abdominal cavity occurred. Splenectomy was performed as well as hemostasis of the liver surface due to rupture of the Glisson's capsule. An overall deterioration of clinical status characterized by hypothermia, anuria, hemodynamic instability followed by mydriasis, absence of other cranial reflexes and subsequent death was reported. Spleen tissue, placenta and umbilical cord were paraffin-embedded for histopathological analysis. During the death investigation process DENV infection was tested with these materials.
Table 1: Complete blood count. View Table 1
Tissues samples from the patient were paraffin-embedded and subjected to microscopic examination after fixation in a 10% formalin solution. Placental weight and disk measurements and some of the characteristics of the fetal membranes, including color and transparency, were evaluated. The distribution and size of the chorionic vessels were evaluated in the fetus. The color and appearance of the placental lobes and tissue sections were examined. The color and thickness of the funicular vessels and Wharton’s jelly were evaluated in the umbilical cord and the abnormalities recorded. After examination, the placental tissues were excised, and seven sections were obtained: from the umbilical cord, two cross-sections at opposite ends and a longitudinal section in the median region; from the membrane, a cross-section of the membrane roll; and from the placental disk, a sample of the cord insertion site and a sample from the middle and outer disks as well as of any other sites considered relevant. All the tissues sections were stained with Hematoxylin-Eosin (HE).
The fetal membranes, umbilical cord, chorionic plate, villi, intervillous space, and decidua basalis were examined under a light microscope.
For immunohistochemistry, the primary antibody MAB 8705 (Merck Chemicals) was used according to the manufacturer's instructions, and the Novolink™ Polymer Detection System and SIGMA FAST™3,3 kits were used in the staining reactions. Paraffin-embedded tissue sections from the livers of patients with a confirmed diagnosis of dengue virus infection who progressed to death as well as paraffin-embedded fetal tissues of the products of conception from infected patients were used as the positive controls for immunohistochemistry. For the negative controls for immunohistochemistry, paraffin-embedded tissue sections from the livers of patients who died due to dengue in which the primary monoclonal antibody used in the incubation step was omitted and only the diluent solution of Bovine Serum Albumin (BSA) were used together with paraffin-embedded placental samples from uninfected patients in which the primary monoclonal antibody was included.
For molecular diagnosis, the viral RNA was extracted from paraffin-embedded tissues using the PureLink FFPE RNA Isolation Kit (Invitrogen, Carlsbad, California, USA). The qualitative Reverse-Transcriptase Polymerase Chain Reaction (RT-PCR) described by Lanciotti [4] was performed for DENV detection and typing. This protocol detects the four serotypes in a semi-nested procedure, generating amplified products with specific molecular sizes (in bp) for each DENV serotype.
The histopathological analysis of the placenta showed areas of corioangiosis (abundance of blood vessels), edema of the villous stroma, and increase in the number of syncytial knots and reduced intervillous space (Figure 1). The immunostaining was positive in decidual cells (Figure 2). The infecting dengue serotype, DENV-2, was identified by RT-PCR detected virus only in the umbilical cord.
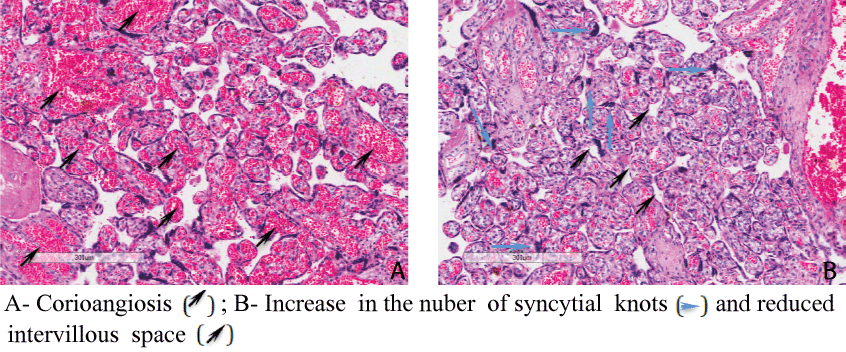 Figure 1: Histopathological findings in the placenta.
View Figure 1
Figure 1: Histopathological findings in the placenta.
View Figure 1
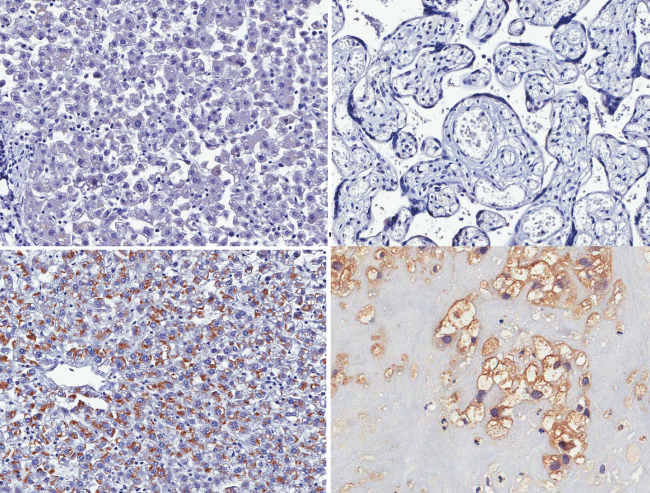 Figure 2: Immunostaining positive in decidual cells. A) Negative control (liver) 20x; B) Negative control (placenta) 20x; C) Positive control (liver); D) Immunostaining positive in decidual cells.
View Figure 2
Figure 2: Immunostaining positive in decidual cells. A) Negative control (liver) 20x; B) Negative control (placenta) 20x; C) Positive control (liver); D) Immunostaining positive in decidual cells.
View Figure 2
Maternal mortality is considered a serious public health problem worldwide, so that the etiological diagnosis for the cause of death is indispensable. Some diseases, specific to pregnancy such as HELLP syndrome, sepsis and bleeding syndromes can cause confounding to complication of Dengue disease. There have been descriptions of thrombocytopenia, liver insufficiency and hemorrhagic complications after childbirth in pregnant women with dengue infection, evidencing the importance of diagnosis distinction from the diseases that are common to pregnancy, such as the HELLP Syndrome in hyperendemic country [5].
Mother’s and fetus death were probably associated to shock, the most severe form of Dengue and which mimicked a usual obstetric complication. The abdominal pain, a “warning sign” may also be useful for monitoring severity in DENV infected pregnant woman, and should be released in specific vulnerability centers as the maternities of hyperendemic countries. The positive immunostaining in placental samples opens a new perspective for the diagnosis of dengue in pregnant women, considering that these samples are easily available, especially when these samples are the only material available [6].
In countries where DENV infection is endemic, serology testing, ELISA IgM and paired IgG or NS1 or RT-PCR should be added to the differential diagnosis of pregnant women whose clinical manifestations are compatible to sepsis or HELLP syndrome [5]. In the event of maternal death, we suggest that immunohistochemistry and/or RT-PCR should be used to test placental tissue, especially in the absence of other materials, to elucidate the cause of death [6].
The hemodynamic changes experienced by the mother due to capillary leak syndrome as well as the vertical transmission of the virus would be responsible for the fetal morbidity.
The placenta proved to be an organ that reflects well the inflammatory response, virus presence and the maternal hemodynamic alterations.
The presented case illustrates the histopathological alterations of placenta due to DENV infection and demonstrates DENV perinatal transmission by the presence of positive RT-PCR in the fetus umbilical cord and reinforces the importance of including DENV infections in differential diagnosis of syndromes occurring in pregnant women such as HELLP and sepsis.
We acknowledge FAPERJ (Fundação de Amparo à Pesquisa do Estado do Rio de Janeiro) for funding the laboratory diagnosis.