This article presents a case of an 88-year-old man who shows blue-violaceous discoloration on his fingers and toes, with a greater intensity on the third finger of right hand and the first, second and third toe of his right foot. The patient had been recently diagnosed with atrial fibrillation and met the criteria for oral anticoagulation with acenocoumarol, which had started two weeks earlier. When the treatment was discontinued, the bluish color of his fingers disappeared, for which reason the patient was concluded to present a rare adverse effect to treatment with dicumarin, making it necessary to replace it for another anticoagulant with a different mechanism of action.
Anticoagulants, Acenocoumarol, Adverse effects, Skin pigmentation, Skin manifestations
Due to the increase of the quality and quantity of life in our population, there are more and more frequent pathologies associated with age, such as the appearance of arrhythmias and, among them, the most common of all, atrial fibrillation. In relation to this increase in the survival of our patients, we consider the treatment of possible complications associated with this pathology. Oral anticoagulants are therefore drugs that we use more and more frequently in primary care consultations in the elderly patients.
In our environment, vitamin K antagonists are the most used, specifically in Spain, acenocoumarol (Sintrom® in 1 and 4 mg tablets). In the Anglo-Saxon country's warfarin sodium (Aldocumar® in tablets of 1, 3, 5 and 10 mg) is used more and it is with this drug that most studies and clinical trials have been carried out.
Both drugs have good oral absorption, high plasma protein binding and hepatic metabolism, being excreted through the kidneys. The fundamental differences are pharmacokinetics, with a shorter half-life span and duration of action for acenocoumarol in comparison with warfarin (5-9 hours versus 36-48 hours and 2-3 days versus 2-5 days, respectively).
It is important to notice that there is a great individual variability in response to the treatment due to multiple factors, both pharmacokinetics (absorption, metabolic clearance) and pharmacodynamics (different concentration/effect ratio), and others such as noncompliance, dietary variations, pharmacological interactions, intercurrent processes, etc [1].
Next, we present the case of an elderly patient with a blue or purple finger syndrome due to the initiation of oral anticoagulant therapy with vitamin K antagonists.
An 88-year-old man with personal history of hypertension, hyperuricemia, seronegative polyarthritis, complete atrio-ventricular block for which a definitive pacemaker was implanted in VVIR mode and as for previous surgical interventions with appendectomy and laparoscopic cholecystectomy. By chance, two weeks earlier, he had been diagnosed with atrial fibrillation that met criteria for oral anticoagulation with acenocoumarol.
The patient went to his Family Doctor's office because of the appearance of blue-violaceous tint on his fingers and toes, with a greater intensity on the third finger of his right hand and the first, second and third toes of his right foot. He presents discrete edema and sensation of paresthesia's (Figure 1 and Figure 2). Denies local pain or other symptoms through electric appliances. The arterial pulses were present and were symmetrical in both upper and lower extremities, the findings in the rest of the physical examination with devices are not worth mentioning.
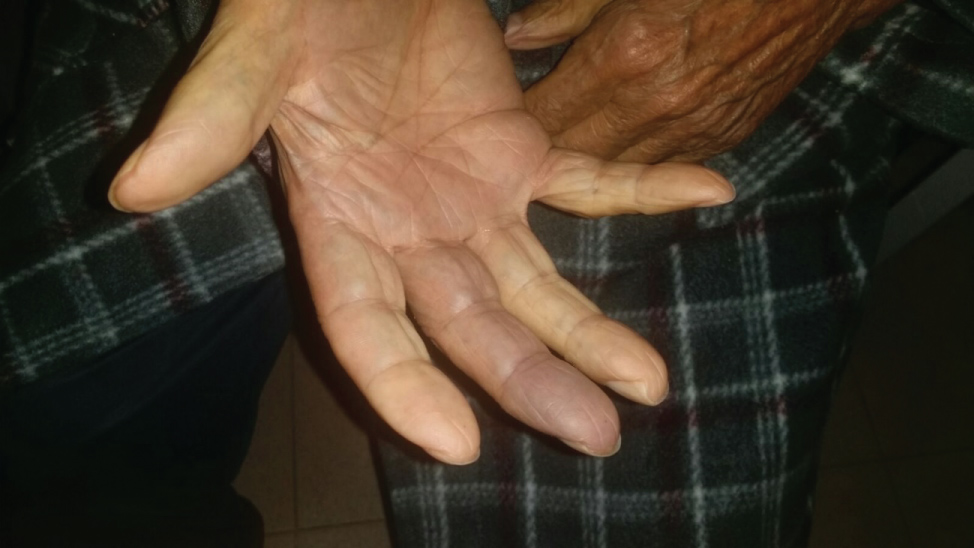 Figure 1: Blue purple color evident on the third finger of the right hand. Oblique plane. View Figure 1
Figure 1: Blue purple color evident on the third finger of the right hand. Oblique plane. View Figure 1
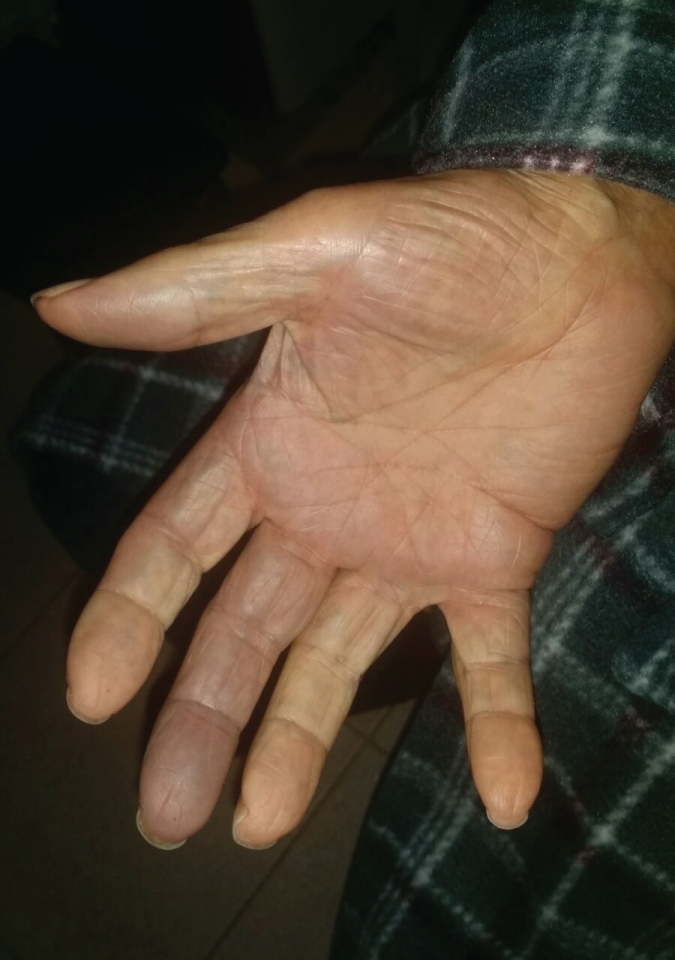 Figure 2: Ventral plane of the blue coloration shown in Figure No. 1. View Figure 2
Figure 2: Ventral plane of the blue coloration shown in Figure No. 1. View Figure 2
He presented a control of INR (International Normalized Ratio) in therapeutic range [2], being in treatment with 7 mg a week. Upon the suspicion of his primary care physician that he could present an adverse effect of the vitamin K antagonist drugs, telematic interconsultation was performed with the Hematology service of the reference hospital for assessment of the case.
Then, treatment with acenocoumarol was withdrawn and replaced for low molecular weight heparin, after which the symptoms subsided in a few days. Determinations of protein C and S were made, resulting in figures within normality.
For all these facts we conclude that the patient had, as a collateral effect of the treatment with dicumarinics, a "blue finger syndrome" for which reason his treatment has been replaced for a direct-acting anticoagulant drug: Apixaban 2.5 mg each 12 hours, but not before performing an echocardiography in which the absence of valvular disease that contraindicated the new prescribed medication was observed.
Acenocoumarol is an oral anticoagulant whose effect is mediated by the inhibition in the liver of vitamin K factors dependent on gamma-carboxylation (II, VII, IX and X), which results in the synthesis of coagulation proteins that may be immunologically detectable, though they lack biological activity. However, in addition, it also inhibits the C and S proteins dependent on gamma-carboxylation, these have anticoagulant properties through the inactivation of two cofactors of coagulation, activated factor V and VIII.
It is because of these competitive effects that coumarins create a biochemical paradox: they produce an anticoagulant effect (by inhibition of factors II, VII, IX and X) and a potentially thrombogenic effect by altering the synthesis of natural anticoagulants (protein C and S).
Multiple adverse effects have been associated with the use of warfarin and acenocoumarol. Bleeding is the main risk of such therapy. Although infrequent, however, non-hemorrhagic complications can also play a considerable role [2]: priapism, hepatitis, alopecia, pruritic macular and popular rash, blue finger syndrome (cholesterol microembolization) and cutaneous necrosis. Unfractionated and low molecular weight heparin can also induce to skin necrosis, but the latter is usually at the injection site [3].
Purple finger syndrome is a rare side effect of warfarin therapy that affects 1 in 5,000 patients; however, this risk increases to 3% if the patient also has a protein C deficiency [4]. It was thought that the pathogenesis was due to a direct and toxic insult to the capillaries, which increased the dilatation and permeability of the vasculature [2]. More recent theories describe cholesterol microelements [5] that are formed as a consequence of the anticoagulation injury itself, or indirectly due to bleeding at the atherosclerotic plaques.
It is a diagnosis of exclusion; there must be an absence of obvious trauma, severe cold-induced injury, or generalized cyanosis. Other causes of ischemia should be ruled out, for example, decreased arterial flow, deterioration of venous flow and other prothrombotic states. Most of the time it is documented that it occurs 3 to 8 weeks after starting anticoagulation, but it has been observed that it occurs between 8 hours and a year after starting therapy.
If it is recognized early, a complete resolution can be achieved simply by substituting warfarin, acenocumarol in our case, for a different anticoagulant. This has been done in previous cases documented with other anticoagulants. Apixaban was used in other similar cases with resolution of symptoms [6]. It started treatment with low doses of apixaban by the advanced age of the patient with the idea of preserving security [7].
The identification and control of this adverse drug reaction with such low incidence is an expression of the diagnostic capacity of the family doctor for rare clinical entities [8,9].
None Declared.
None Declared.