Some social and demographic factors in the population may contribute to the practice of Breast Self-Examination (BSE) allowing timely detection of cancer in the early stages.
To determine the socio-demographic factors associated with breast self-examination in women attending primary care.
Analytical, observational, cross-sectional study in women aged 20-59, entitled to a primary care unit in Cancún, Quintana Roo, Mexico. Sociodemographic data were recorded: age, occupation, schooling, marital status, religion, socioeconomic status. Risk factors: Family history with breast cancer and body mass index. We performed bivariate analysis and logistic regression with BSE as a dependent variable.
We surveyed 380 women, mean age 38 ± 10.5 years, 22% performed BSE. There is a significant difference (p < 0.05), for primary education or less, single civil status, socioeconomic worker level, Jehovah's Witness religion; Without difference for the occupation between the groups of BSE and those that do not realize BSE. There is a risk of not carrying out BSE in women of socio-economic workers RP (Prevalence Ratio) = 2.06, with primary or less PR = 1.27, Jehovah's Witnesses PR = 3.34, single marital status RP 1.29, common PR = 1.49.
Eight out of ten women do not have BSE. In primary care centers, it is necessary to strengthen BSE programs in health service providers. Despite the diffusion for the prevention of breast cancer in health institutions, sociodemographic factors limit BSE in urban women.
Breast cancer, Breast self-examination, Social demographic factors
Worldwide, more than one million cases of Breast Cancer (BC) are diagnosed annually, this is equivalent to 411,000 deaths from this cause, accounting for 14% of cancer deaths worldwide. Approximately 60% of BC deaths occur in developing countries [1].
According to the World Health Organization (WHO), its incidence is expected to increase by 50% by 2020 [2]. In Latin America and the Caribbean, breast cancer is the most prevalent among women according to the Pan American Health Organization (OPS). In 2012, this neoplasm was detected in more than 408,000 women, and by the year 2030, it is estimated that there is a 46% increase [3]. In particular, Colombia, Costa Rica, Ecuador, Mexico, and Venezuela, which previously had relatively low rates, An increase in mortality rates [4-6].
In Mexico, more than 75% of cases of BC are diagnosed in advanced stages (II, III, IV) according to data from the Histopathological Registry of Malignant Neoplasms [4-8]; and the occurrence of BC is 10 years earlier compared to that reported for European and Anglo-Saxon women, in the United States the average age of onset is 60 years, while in Mexico it is 50 years [5].
Studies have been carried out in Latin American countries on the coverage of the clinical breast examination, identifying in a descriptive way the main characteristics that influence the performance of this procedure, however, few studies have explored the factors that are associated to Breast Self-Examination (BSE) and their knowledge [6,7].
The periodic practice of BSE can lead us to an early diagnosis of breast cancer, therefore, to a better prognosis for those who suffer from this disease. Evidence shows that breast cancer control depends to a large extent on sociodemographic, cultural, economic and health services organization, however, little is known about the weight of these variables in the detection of this disease [8-12].
The purpose of this study is to analyze sociodemographic variables related to the practice of breast self-examination and risk factors for breast self-examination.
An analytical, observational, transversal study was carried out; 380 women between the ages of 20 and 59, entitled and assigned to the Mexican Social Security Institute (IMSS), participated in a family medicine unit in Cancún, Quintana Roo, in 2016.
The family medicine unit No. 16 of Cancún, Quintana Roo, was selected, with a population of 32,050 beneficiaries; Women between the ages of 20 and 59 who attended the outpatient clinic and who agreed to participate in the study were excluded, those with a previous diagnosis of breast cancer were excluded, and those with a comorbidity that prevented them from answering the survey, Incomplete questionnaires were deleted.
In the areas of external consultation of the unit, the patients belonging to 20 family medicine clinics were identified, they were randomly invited to participate in the study; In an area reserved to preserve confidentiality, was given the informed consent for authorization and then the study survey to respond.
The variables of the study were: age, schooling, occupation, religion, socioeconomic level and marital status, body mass index, and antecedent of the direct relative with breast cancer. Once the surveys were obtained, two groups were formed according to the outcome variable (BSE positive) to perform the determination of prevalence reasons.
As of bias control methods, it was considered that the patient answered the survey in a self-administered way. To avoid information, bias the statistical analysis was performed by an independent analyst. To avoid the measurement, bias the weight and height variable was obtained by integrated preventive care nurse (API) standardized in detections.
The sample size was determined using the statistical program Stats, for a finite sample with an estimated proportion of 50% confidence level (1 α): 95%, maximum acceptable error: 5%. The extraction of the subjects was carried out in a random way in the totality of the offices of the medical unit.
Descriptive statistics were used as measures of central tendency and dispersion for the quantitative variables; Frequencies and percentages and 95% confidence intervals [95% CI:] for the qualitative variables. Inferential statistics on qualitative variables using Pearson's Chi square test was considered a statistical significance of at least 0.05 (p-value). In order to carry out the risk measurement, prevalence ratios (SBE positive vs. SBE negative) were determined.
A binary logistic regression model was used to eliminate spurious associations, considering the entry of variables with a minimum p value of 0.10.
The data was entered into a database in the statistical program SPSS version 21.0 for Windows 8.
Of a total of 32,050 women in the Primary Healthcare Unit No. 16, 380 women aged 20 to 59 years were randomly enrolled, 22% (n = 80) reported performing Breast Self-Examination (BSE +) vs. 78% (n = 300) that do not perform it (BSE -) (Figure 1).
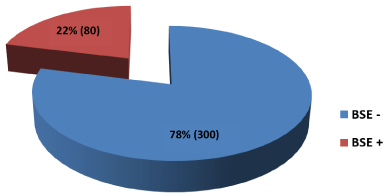 Figure 1: Breast Self-Examination.
Figure 1: Breast Self-Examination.
N = 380. BSE (-): Negative Breast self-examination, BSE (+): Positive Breast self-examination. View Figure 1
The frequency of self-examining women (BSE +) was: 50% (n = 40) performed every six months, 35% (n = 28) monthly, 15% (n = 12) once a year (Figure 2).
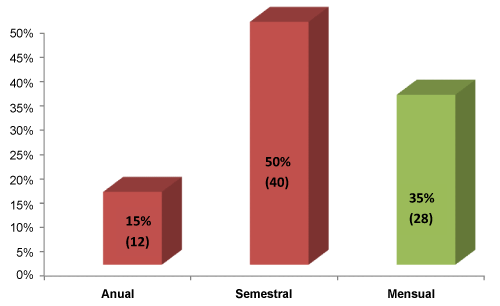 Figure 2: Breast Self-Examination Frequency.
Figure 2: Breast Self-Examination Frequency.
N = 80. BSE (+): Positive Breast self-examination. View Figure 2
The differences in variables between BSE and non-BSE groups are shown in Table 1, the following results stand out: The mean age of women who performed BSE was 37.38 years ± 11.09 and for women who did not perform BSE was 39 ± 10.18, mean weight for both groups was similar, 66.31 kg ± 8.6 in the group with BSE + and 66.35 kg ± 8.62 for the group with BSE -. For BMI, a mean of 27.55 kg/m2 ± 3.57 was reported for the group of women with BSE + and 27.73 kg/m2 ± 3.41 in the group of women who did not perform BSE. The most frequent occupation was housewife with 154 cases (40.52%) in the group of women who do not practice BSE.
Table 1: Sociodemographic characteristics. View Table 1
The highest level of schooling in the group of women who did not self-explore was secondary or higher, with 258 cases (67.8%). Regarding religion, women with a non-BSE religion were reported to predominate with 159 cases (41.9%), and of the different religions studied, Jehovah's Witness women were the least performing BSE with 12 (3.15%) cases. The civil status Free union was the one that predominated in the group of women who do not perform BSE with 172 cases (45.26%). Regarding the socioeconomic level, it was found that the low average level was the one that predominated with 138 cases (36.31%) in those women who did not perform BSE, there were no patients with high stratum nor marginal stratum. The family history of breast cancer was reported in 39 women in total, 34 (8.94%) who had BSE and 5 women (0.13%) who did not. As for nutritional status, overweight predominated in 182 women (47.89%) who did not practice BSE. The determinants of risk of prevalence (Table 2); Reported RP 1.27 for primary or lower schooling, 3.34 for practicing Jehovah's Witness Religion, 1.89 for no partner, 2.06 for socio-economic workers. In contrast to the antecedent of Relatives with Breast Cancer who reported a PR of 0.02. All with p < 0.05.
Table 2: Determinants of prevalence risk. View Table 2
The logistic regression model for civil status, socioeconomic status, religion, and schooling is shown in Table 3, confirming the risk for all variables except for schooling Exp (B) = 0.93 [95% CI: 0.41-206].
Table 3: Logistic regression model for risk estimation. View Table 3
Breast cancer is currently a relevant public health problem requiring priority attention [2,3,10]. In most regions of the world, it is the leading cause of female mortality due to malignant tumors and has already surpassed cervical cancer [3,11]. In Mexico, there are studies that associate breast cancer control to a large extent with socio-demographic, cultural, economic and health organization factors [5].
National and international health institutions recommend prevention activities such as breast cancer education [12]. Breast self-examination is a simple and effective method, which can be carried out periodically, within the reach of all women and recommended as the first method to be used for the early detection of breast cancer, so that the woman knows the shape and texture of her breasts and thus can make an early detection of any change or presence of breast lumps [8,9,11-14].
The Mexican Official Standard NOM-041-SSA2_2011 [14] for the prevention, diagnosis, treatment, control and epidemiological surveillance of breast cancer recommend performing breast self-examination for all women from the age of 20 monthly. A detection Precocious may be the most important link in the chain of care, since if it is done in time there is a high probability that women will prolong their life [8], increase the chances of survival in women and keep the breast [11]. The diagnosis in most young women is performed by detecting a lump in breast self-examination [15].
In this study, it was found that breast self-exploration is infrequent, since only 22% were performed, of which only 35% performed with the periodicity recommended by the health institutions. Similar to that reported by Tesfaye Hailu, et al. [16]. In a study carried out in Ethiopia in 2014, in a population of 760 women, of whom 41% reported self-exploration, and only 17.7% knew the recommended frequency for their practice [16]. Alwan, et al. [17] reported that the practice of breast self-exploration in Iraq in their study with 387 participants (302 women and 85 men) was 48% [17]. A higher frequency is reported by Mary Atanga Bi Such, et al. [18]. In their study carried out in Cameroon in 120 women, 60% of whom did self-exploration, but only 35% performed it monthly [18]. In the city of León, Guanajuato, Mexico, 73.7% of women performed BSE Periodical, however, the quality of the same reported reaches only 27.2%.
As for the association between BSE and age, it was found that women who self-explored most corresponded to the stratum between 20 and 29-years-old with 33% and the least self-explored were the group of 40 to 49 years with 5%, like the study by Tesfay Hailu, et al. [16] Who reported a self-exploration practice in 97% of women under 25-years-old and 3% in those older than 25 years, 15 in contrast to Lidiana Martínez Muñoz, et al. [19] Who concluded in their study of 80 women in Bernardo Posse, Cuba, that women older than 40 had greater knowledge and adherence to the practice of breast self-exploration than the group of women aged 25 to 39; However, the mean age of BSE practice in both groups did not report a statistically significant difference (p = 0.22) [19].
With regard to the relationship between breast self-examination and schooling, uneducated and primary women are scanned in 3%, and women in high school in 9.47% (p = 0.03), that is, at a higher level of schooling increased breast self-exploration practice in accordance with what was commented by Fred Gustavo Manríque Abril, et al. [20] Who in a study of 810 women in Tunga Colombia reported adequate completion of breast examination in 128 women with completed secondary education and 16 women without completed secondary education [20] differing in results of Yépez Ramírez D, et al. [4] in their study with 350 women over 20-years-old in a family medicine unit in León, Guanajuato, Mexico, found no association between the practice of breast self-exploration and schooling.
The association between BSE and sociodemographic variables, marital status, religion, schooling and socioeconomic status were statistically significant in this study (p < 0.05), unlike the study by Khaled Abdulla, et al. [21]. Conducted in 2016 in the Republic of Yemen, which found no relationship between low frequency of breast self-examination and sociodemographic factors [21].
International and national health institutions recommend prevention activities, such as breast cancer education, aimed at sensitizing women about the importance of knowing the normal characteristics of their breasts and requesting medical attention if they discover any abnormality [8].
Among the weaknesses of this study is the non-determination of costs and verification of the correct BSE technique in the women evaluated, as well as the competencies of health service providers in primary care units, as the first link in the chain of prevention of BC [22].
The contribution of this research is evidence of the low practice of BSE in women in a primary care unit of a public health institution in Mexico, and although it is a minimal sample, it is part of the 85% of primary care institutions that offer prevention services and health education to the Mexican population.
This is the result of an incipient line of research to carry out educational, training and impact interventions in breast cancer care in the state of Quintana Roo, Mexico.