Gastrointestinal stromal tumors, Liver metastases, Imatinib
Gastrointestinal Stromal Tumors (GISTs) are rare tumors of the gastrointestinal tract, with an estimated incidence of 1.5/100000/year. GISTs are nonepithelial tumors originating in the interstitial Cajal's cells (cells of the autonomic nervous system). These cells express antigens for CD 177 and/or CD 34 [1]. More than half of GISTs start in the stomach but they can start anywhere along the gastrointestinal tract. We report the case of liver metastases as a first manifestation of GIST.
A 77-year-old female patient suffered persistent gastrointestinal symptoms including abdominal pain, eructation, nausea and early satiety. The duration these symptoms were six weeks. The patient did not notice any blood in her stools. The patient regularly saw a physician because of hypertension. At the clinical examination we observed enlarged abdomen due to adipose tissue, hepatomegaly hard in consistency and slight sensitivity at liver palpation. Laboratory test showed mild hepatocytolisis (ALT = 42 U/l, AST 89 U/l) and cholestasis (ALP = 178, LDH = 873 U/l and GGT = 206 U/l). The rest of the laboratory tests (coagulation, kidney) were normal. The level of CEA, CA 19-9 and AFP were normal. Chest and abdominal radiography was normal.
We performed abdominal ultrasound and we observed numerous focal hepatic lesions with cystic appearance. Computed Tomography (CT) showed multiple hepatic cysts with thick wall and weak iodocaptation and a weak mass at the fornix level (Figure 1). The endoscopic ultrasound established the existence of a polylobate submucous mass of 30/30 mm, originating in the muscular layer. Pathological examination of biopsy specimens of the liver showed a tumoral mass, non-encapsulated, with dense tumoral cellular proliferation, medium size tumoral cells and frequent mitoses. The immunophenotyping and the immunohistochemical profile showed positivity for C kit (CD 117) and vimentine, as well as negativity for desmine, S100 and keratine. The final diagnosis was gastric GIST with hepatic metastases, stage IV. The patient was treated with imatinib (400 mg/day). Four months after the beginning of the treatment CT scan showed hepatic tumors mostly cystic and the gastric tumor was significantly reduced in size (18/22 mm).
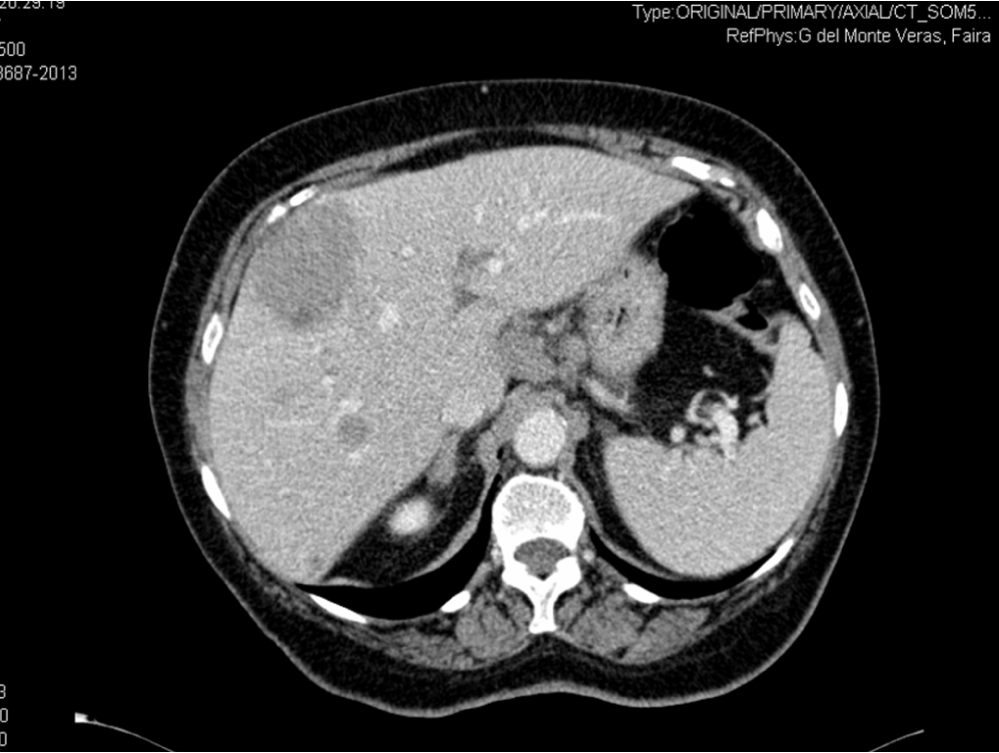 Figure 1: Computed Tomography (CT) showed multiple hepatic cysts with thick wall and weak iodocaptation and a weak mass at the fornix level. View Figure 1
Figure 1: Computed Tomography (CT) showed multiple hepatic cysts with thick wall and weak iodocaptation and a weak mass at the fornix level. View Figure 1
The term GIST was first used in 1983 by Mazur and Clark, in the past, these tumors were classified as leiomyomas, leiomyosarcomas and leiomyoblastomas [1,2]. GISTs are rare before the age of 40 years and very rare in children, with a median age at diagnosis of 50-60 years. Some data show a slight male predominance.
Most GISTs are sporadic and have no established risk factors. The association of gastric GIST, paraganglioma, and pulmonary chondroma is known as Carney's triad.
The symptoms of GISTs are non-specific and depend on the size and location of the lesion. The most common symptom at presentation is bleeding (50%), but the patients may also have various other symptoms (abdominal pain or discomfort, early satiety, bloating, obstructive jaundice, dysphagia, fever and anaemia-related symptoms such as fatigue and palpitations) or they may present with an abdominal tumor with no symptoms [2,3]. The symptoms may mimic those of functional gastrointestinal disorders as in our patient. 10-25% of patients present with metastatic disease. The most common location of a GIST seems to be the stomach (50-60%) and the small intestine (30-40%) and elsewhere in the gastrointestinal tract (10%) [3]. Metastases from GISTs are often found in the liver and peritoneum. Rarely they metastasise to other sites such as the lungs or bone.
The type of imaging used initially will depend on the mode of presentation and local availability. If a small sub-mucosal mass is seen as an incidental finding at the time of endoscopy, then endoscopic ultrasound should be performed first. If this type of imaging is not available computed tomography is an alternative. For larger palpable masses, or where the patients present with hemorrhage, abdominal pain or obstruction, computed tomography is usually the initial investigation. This type of imaging is widely available to assess both primary tumor extension and the presence of metastases. Positron emission tomography has also been introduced for the additional functional information it can provide.
The diagnosis is based on histologic and immunohistochemical criteria, the most important of which is the expression of transmembrane tyrosine kinase receptor protein derived from the activated c-kit gene. GISTs are composed of spindle (70%) and epithelioid cells (30%).
Treatment options involve: Surgical resection, tyrosine-kinase inhibitors administration, radiotherapy and chemotherapy [1]. All GISTs 2 cm in size or greater should be respected, the management of incidentally encountered GISTs less than 2 cm in size remains controversial. Surgery is the principle treatment for GISTs and suitability for resection should be explored by an appropriate sub-specialist surgeon. The treatment depends on the size and location of the tumor [4]. Most patients with metastatic disease ultimately cease to respond to imatinib [3,4]. Imatinib mesylate is a selective, potent, small molecule inhibitor of a family of structurally related tyrosine kinase. The recommended starting dose of imatinib is 400 mg/day which can be escalated, if necessary, to 800 mg/day.
The most important independent prognostic factor for GIST recurrence after surgery is a high tumor mitotic rate [1,3]. Another important risk factor is the location of the tumor. In general, GIST not exceeding 2 cm behave biologically in a non-aggressive manner (unless located in the duodenum or rectum), whereas tumors larger than 2 cm have an increased risk of recurrence.