Avoidable hospital readmissions and medical errors are costly and dangerous. Many hospital systems have invested in various transitions of care models, health information systems and now increasingly, in telehealth, to help improve care after hospitalization. Although many models and strategies exist to improve care transitions, very few guidelines address the role of health technology, data analytics and health information exchanges within this process. Few studies have described an optimal workflow for physicians performing virtual clinical surveillance using telehealth. Furthermore, although many published studies have conducted telehealth transition of care interventions for patients with specific disease pathologies, few studies evaluate interventions using multi-modal remote patient monitoring for patients with mixed-chronic conditions. This appears to be an ideal target audience for telehealth interventions given that, the factors affecting patient risks for readmission are often complex and multifactorial. Our study aims to evaluate a new workflow for addressing comprehensive transition of care, using risk stratification, telehealth remote patient monitoring, and patient-centered virtual visits. We also introduce a new communication tool for relaying tele-communication.
To describe current study protocol and demonstrate the steps and stakeholders involved to ensure proper integration and scalability to other practices.
The study is a feasibility study with a randomized controlled trial design, in which an anticipated 180 patients will participate. The treatment group receives technology driven clinical surveillance with a dedicated transition of care physician, along with weekly virtual visits using a telehealth kit, in addition to standard transition of care services. The control group receives the standard of care and follow up within 30 days of hospital discharge. All patients are enrolled in the Health Information Exchange (HIE) and undergo risk stratification. Risk stratification is performed for all patients using two different modalities: An Electronic Medical Record (EMR) based prognostic tool and a validated machine learning algorithm from our biomedical informatics team. The endpoint is 30 day hospital readmission. Patient data is collected on hospital and ED utilization, patient self-management, perceived care coordination and patient experience.
Our study goals are to identify the optimal clinical workflows needed to incorporate telehealth technologies into patient care, and incorporate risk stratification to target patients most at risk for readmission. The specific aim of the study is to determine the generalization and scalability of implementing telehealth services in the post hospital period to improve transitions of care and reduce hospital readmissions. To accomplish our study goals and aim we will provide services in the post-acute period following hospital discharge to evaluate the impact of telehealth on care coordination, patient satisfaction, patient self-management and hospital readmission.
Telehealth, Telemedicine, Readmissions, Telecare, Bioinformatics
HIE: Health Information Exchanges; EMR: Electronic Medical Record; IRB: Institutional Review Board; PCP: Primary Care Physician; AHRQ: Agency of Health Care Research and Quality
As healthcare reform matures, policy makers, administrators, payers and healthcare providers are all looking to achieve the Triple Aim objectives of providing improved health care at a lower cost [1]. Preventable hospital readmissions remains an important issue as a marker of quality in healthcare delivery. In the legacy of the Health Information Technology for Economic and Clinical Health (HITECH) Act of 2009, there have been many incentives for meaningful use of electronic data and of the Health Information Exchanges (HIE), resulting in reduced 30 day readmissions [2].
It is known that the period following a hospitalization can be the most dangerous time for a patient. In fact, as many as one in five patients will suffer adverse events after hospital discharge [3]. Many of these adverse events are potentially preventable by addressing medication and clinical errors, patient behaviours, gaps in education and communication during this transition period. As new technologies evolve, there are increased demands and opportunities in modernizing healthcare delivery; while harnessing telemedicine to address these complex readmission factors. However, understanding how to incorporate telehealth into current clinical workflows has been a considerable barrier to the adoption of telemedicine [4-6]. Telemedicine, shows great potential in reducing hospital readmission, to date study findings have been inconsistent [7-12]. This technology, offers an opportunity to virtually connect patients to providers through the high risk readmission period. Multifunctional telehealth interventions may provide the greatest benefit to patients and that complex patient-centered models have been shown most effective in reducing readmissions [11,13]. Thus, an integrated multidisciplinary telehealth intervention has the greatest promise to effectively deliver post-hospital transitional care and decrease readmissions.
The aim of this paper is to share our methodologic experience with the goal of developing a clinical workflow which integrates traditional clinical practice with advanced technology, data analytics and new data sources (HIE) for high quality transitional care. By clarifying the methodology of clinical processes involved in telemedicine interventions, we hope to promote the adoption of telemedicine [4] and offer a scalable approach to integration.
Our objective is to evaluate the effectiveness of the protocol created for the current patient centered, physician led, transition of care, telemedicine intervention. According to the current model of care, each patient upon discharge is provided with a discharge summary, containing next steps to follow-up, scheduled appointments and instructions to further care. Patient's responsibility is to coordinate their followup care, ensure proper management of their health and medication adherence until their next primary or specialist consultation. Aforementioned list of actions is the "standard of care" available post-discharge. The intervention begins at the bedside and involves remote patient monitoring of daily vitals, weekly virtual visits, detailed Electronic Medical Record (EMR) documentation and use of risk stratification as well as data from the HIE. We hypothesize that in comparison to the "standard care" that:
1. Preventable hospital readmissions will be reduced through patient centered virtual visits, daily biometric surveillance, and increased data access.
2. Patient satisfaction during the transition of care period will be improved.
3. Adverse healthcare outcomes will be reduced.
The primary goal of the study is to determine the effect of telehealth on unplanned hospital readmissions within 30 days of the index hospitalization discharge. In addition, we have collected data in order to provide secondary analyses on the effect of telehealth on emergency department utilization, patient satisfaction, qualitative patient experience, patient self-management and self-efficacy attitudes. In accordance with our Patient Centered Medical Home quality improvement initiative, transitions of care must be performed within 7-14 days of discharge for any and all patients receiving inpatient care. This study has also led to successful integration of patient data into the traditional clinician evaluation from the data warehouse which provides data from a variety of sources including the HIE, community pharmacies, and claims data. We use this data to apply validated risk stratification measures [14,15] to patient evaluation, to attempt to understand readmission risk better. We also have identified a clinical workflow model for remote patient monitoring in transitions of care and introduce a communications hand-off tool for telehealth encounters.
This study is being performed at Stony Brook Medicine, which is a 603-bed teaching institution in the North part of Long Island, New York. Servicing mostly population of Suffolk County with yearly admission rate of 31,715 patients, with a range of 10.812.8 percent readmission rate. Lest than one percent of all admissions are uninsured.
Study data is collected and managed using RED Cap [16] electronic data capture tools hosted at Stony Brook Medicine. RED Cap (Research Electronic Data Capture) is a secure, web-based application designed to support data capture for research studies, providing: 1) An intuitive interface for validated data entry; 2) Audit trails for tracking data manipulation and export procedures; 3) Automated export procedures for seamless data downloads to common statistical packages; and 4) Procedures for importing data from external sources. RED Cap software allows the team to incorporate a randomization schema to include it in the process of enrollment seamlessly. After meeting inclusion criteria, the software follows a schema unknown to the researchers to randomly select consented participants into appropriate arms of trial.
Patient security has been of utmost importance to secure patient data due to potential risks of utilizing audio-visual technology for performing medical interventions. Data collection, transmission and storage have been tested and approved by institution's specialists in Information Technologies and Biomedical Informatics. Furthermore, the Stony Brook University School of Medicine Institutional Review Board (IRB) reviewed and approved this study (970227) to ensure protection of human subjects in this study. The data is stored and secured in the EMR, and a HIPAA compliant database provided by the telehealth vendor, as well as in RED Cap. All smart phones are password protected, allowing only the patients and their caregivers to access the phone. Transmitted data includes only study identifiers, and all documentation is conducted in the EMR. All data security measures are outlined in all recruitment and consent materials. As mentioned earlier, less than one percent of the patients admitted into the hospital are uninsured. Due to the potential lack of significant ability to link to care and alter the study, uninsured patients are currently excluded from the trial. Additionally, healthcare costs for readmission of uninsured patients can pose a challenge for the hospital, which could be prohibitive for reproducibility and generalizability of the study.
Patients in accordance to the inclusion/exclusion criteria (Table 1) are identified using EMR data and are approached by a licensed clinician to determine eligibility and enrollment through survey, medical history, and physical exam. 60 patients will be randomized to receive telehealth services, 60 patients will be randomized to receive the usual discharge planning after hospital discharge. The study will be over 10 months, with approximately twelve patients enrolled monthly. The Telehealth patient will be provided with a smart phone device and Bluetooth-enabled blood pressure monitoring cuff, weighing scale, and pulse oximeter (Figure 1). These Telehealth patients will measure their vitals daily using the equipment and have weekly virtual visits with a transition of care physician (teledoc). Patient agrees upon consent to participate in the trial for the length of thirty (30) days. The teledoc in this trial, is a senior resident physician of the primary care medical division. There are seventeen providers at the outpatient practice overseeing the care of already established patients by the resident performing the virtual encounters. It is important to note that enrollment, virtual visits and remote monitoring is performed by the resident who, in turn, reports to the patient's PCP in the practice. The role of the teledoc can be fulfilled by a trained resident, fellow, nurse-practitioner or a primary care physician. Further virtual visits may be arranged at the discretion of the teledoc/PCP based on the clinical determination of the patient.
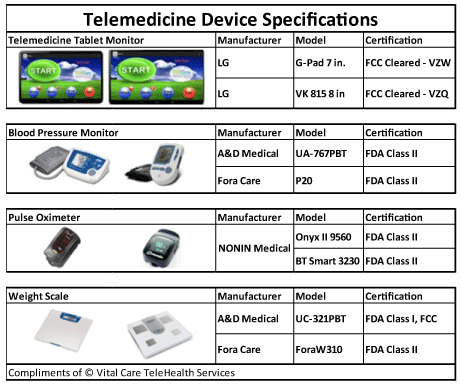 Figure 1: TeleKit. View Figure 1
Figure 1: TeleKit. View Figure 1
Table 1: Inclusion and Exclusion Criteria for evaluating Potential Family Medicine Patients Hospitalized at Stony Brook Medicine. View Table 1
Patient enrollment and randomization occurs at the bedside. All patients are consented for the HIE in addition to the trial, and are risk stratified though an EMR data based validated algorithm. The care management team is notified of all study participants in order to notify the telehealth team of hospital discharge. A physical exam is performed on patients randomized to the treatment arm, to allow for the teledoc to evaluate the patient in person prior to virtual visits. Upon hospital discharge the patient receives the telehealth equipment by a vendor service to their home within 48 hours.
The bedside risk stratification is done by an internally and externally validated High Risk Readmission Tool across many different hospital systems. This tool will identify patients at High Risk for Readmission via a risk score grouped as high, moderate, and low. Normalizing the readmission risk score converts it into a more universally used scale (0-100 scale) that it easier for clinicians to understand and use. The scores are calculated by using a proprietary algorithm by Cerner© that includes about 40+ data points from groups, based on the patient history and admitting physical exam, diagnosis related group codes, patient demographics, procedures, utilization, lab tests, medications, and exploratory variables. The tool was validated by a public academic center, Advocate Health Care [15].
Further risk stratification, will be conducted using a validated machine learning algorithm [14] by our Biomedical Informatics team. This will be a useful comparison to the Cerner© tool in predicting future readmission risk after 30 days.
The patient follows prompts from the smart phone to register vitals daily, using a blood pressure cuff, pulse oximeter and digital scale (Figure 1). The teledoc determines the parameters of the vitals depending on the patient clinical history and status. The telehealth vendor, notifies the teledoc of any abnormal values.
The weekly virtual visit technique is based on the theoretical framework of the Coleman Transition of Care Model [17], and best practices of "Whole-Person" transitional care from the Agency of HealthCare Research and Quality (AHRQ) [18]. The Coleman model focuses on timely follow up with a primary care provider, medication self-management, use of a dynamic patient-centered record, and knowledge and monitoring of red flags that could indicate clinical decompensation of a patient [17]. The "Whole-Person" transition of care focuses on comprehensive assessments of the patient, incorporating potential social determinants of adverse health outcomes and interdisciplinary care coordination. These models are incorporated into the content of the virtual visits that allow for thorough assessments and identification of potential factors.
Prior to the virtual visit, the Primary Care Physician (PCP) is alerted of the dates of scheduled virtual visits as to be available for hand-off afterwards. The teledoc begins evaluation of recorded vitals obtained from daily patient values, review of clinical orders, medications, radiology, labs, and previous clinical notes, including the automated readmission risk score from the internal EMR prior to the encounter. The patient then verifies no further hospitalizations or emergency room visits are present in the HIE. After the review of the objective EMR and HIE data, the teledoc then begins synchronous two way audio-video conferencing with the patient, which mirrors the interaction of an in-person interaction (Figure 2). The teledoc then performs a detailed medicine reconciliation focusing on prevention of medication errors, ensuring adequate review of potential barriers for medicine adherence. The patient is coached on self-management, and instructed to recite the indication for each medication. A joint- preliminary patient centered plan is agreed upon by the telehealth provider and the patient. The visit is then completed with data collection survey using RED Cap. Thorough documentation is recorded in the EMR using a modified Situation-Background-Assessment-Recommendation (SBAR) framework [19] (Figure 3 and Figure 4). In this structure, communication is effectively conveyed through an Assessment/Plan section organized in a severity stratified problem based format. A short Action List (Figure 4) is then created for telephone communication to the PCP. A clinical plan is then offered to the primary care doctor for consideration, the primary care doctor authorizes all final medication changes or treatment plans. The patient is then notified of the finalized medical plan.
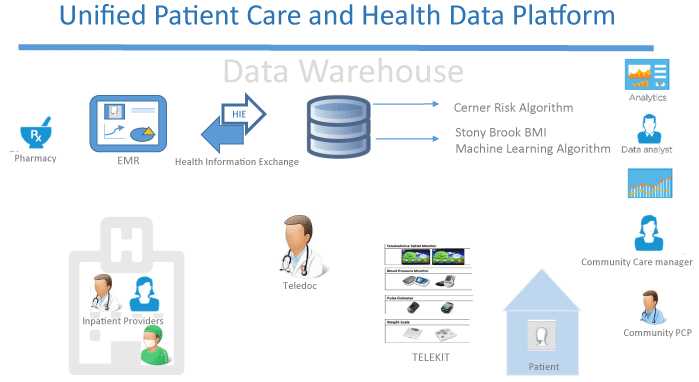 Figure 2: Unified Patient care and Data Platform. View Figure 2
Figure 2: Unified Patient care and Data Platform. View Figure 2
 Figure 3: EMR Note. View Figure 3
Figure 3: EMR Note. View Figure 3
 Figure 4: TELE Acronym and Short Action List. View Figure 4
Figure 4: TELE Acronym and Short Action List. View Figure 4
This feasibility study introduces a novel physician led, patient-centered telehealth intervention using the latest available data at Stony Brook Medicine. There are several limitations to the study methodologies employed that should be considered. Generaliz ability must be taken into account when evaluating our design, given that Stony Brook Medicine is a large academic center with advanced biomedical informatics and Information Technology resources. The time dedicated and level of clinical training or expertise for the role of the teledoc should be taken into account. Larger well powered, multi-institutional trials are required to make definitive conclusions regarding the ability of the intervention to reduce hospital readmissions.
However, despite these limitations, we believe the methods discussed are valuable to researchers evaluating telehealth utilization.
Telehealth offers promising opportunities to address patient needs in the community after a hospitalization. Understanding the role of telehealth incorporating data analytics in this period is an important goal of this study. Regular virtual evaluations incorporating all available patient data, may further improve healthcare delivery, reduce medical error, and improve patient self-management post hospital discharge.
Proving patients with a service that improves access to medical care, transitions of care, access to their established medical provider is invaluable to ensure care during a vulnerable time post-discharge. Concurrent with the aim of the study, we hope to introduce an innovative way to perform medicine in the community using telemedicine. The interdisciplinary collaboration of biomedical informatics, information technology, care management, private industry and medicine has allowed for a truly thorough and comprehensive evaluation of patients as they transition healthcare environments. The ability to incorporate HIE, EMR and patient generated data, will continue to create personalized and unique care plans for patients after hospitalization. Many lessons of effective transitions of care are shared in this model through engagement of high-acuity post-discharge patients. This feasibility trial began enrolling patients in June 2017. The trial is currently ongoing. All final results will be disseminated through peer-reviewed publications as well as at scientific conferences. Lay summaries will be provided to the study participants and clinical and administrative stakeholders of the trial.
Our study and all of its components were approved by the Stony Brook University Institutional Review Board.
None.
All authors listed above have contributed to this work equally.
The authors declare to possess no conflict of interest. All of the collected data analysed is under the full control of the research team.