Although mortality after pancreaticoduodenectomy (PD) in high volume centers is less than 5%, morbidity is still as high as 30 - 50%. Hemorrhage from ruptured pseudoaneurysm is a rapidly progressing and potentially fatal complication after PD.Visceral pseudoaneurysm after pancreatic surgery is well known by surgeons. Postpancreatectomy hemorrhage is a life threatening entity, and must be managed urgently. Here we report two cases, late massive bleeding after pancreaticoduodenectomy. First case is a 69-year-old male with a ruptured dorsal pancreatic artery pseudoaneurysm which was successfully treated with endovascular arterial coil embolization. Second case is a 52-year-old male patient with a ruptured gastroduodenal artery pseudoaneurysm which was treated with laparotomy. Upper gastrointestinal bleeding in the late postoperative period following PD should alert the surgeon to the possibility of a ruptured celiac vessel pseudoaneurysm.
Hemorrhage, Pseudoaneurysm, Pancreatic surgery
PD: Pancreaticoduodenectomy; ISGP: An International Study Group of Pancreatic Surgery; CT: Computerized Tomography
Thanks to the developments in diagnostic modalities, improved intensive care possibilities and modern surgical techniques, PD operation (Whipple operation) can be performed with a low mortality rate of 5% in experienced hands. However, complication rate is still high and could not be reduced to figures below 30 - 50% [1,2].
A rare and serious complication is post-pancreatectomy hemorrhage. According to the classification of ISGP in 2007, post-PD bleeding is divided into two groups as "early" and "late" [2]. In the early period of first 24 hours, the bleeding is usually due to some technical or hematological issues.
Late bleeding can occur even after several weeks. Main causes of late bleeding are intraabdominal abscesses and pseudoaneurysms which have developed in arteries by deleterious effects of pancreatic exocrine secretion [2-6].
Visceral artery pseudoaneurysm that develops after PD operations is a serious and life-threatening complication [7,8]. However, improvement in diagnostic modalities and treatment with radiological methods have changed the management and outcome of this dangerous complication [9,10].
Visceral artery pseudoaneurysms are rare pathologies. Therefore, large series are not common in the literature. However relevant material can be obtained from case reports.
In this presentation, we report two cases of visceral artery pseudoaneurysm; one of whom was succesfully treated by interventional radiology, while the other died secondary to severe sepsis originating in the abdomen.
A Standard Whipple operation was performed in a 69-year-old male patient for duodenal tumor. On the fourth day of the operation, mild tenderness occurred in epigastrium, followed by an increased amount of drainage through the abdominal drains. On the seventh day, amilase level was found to be very high (1855 u/l). At the same time, a cholangiogram showed leakage from the hepaticojejunal anastomosis. However, the amount of fistula fluid gradually decreased; abdominal tenderness diminished and the patient was discharged from the hospital on the 14th day while the drains were left in situ. On the 45th day he was re-admitted to the hospital with the complaints of fatigue and bloody stool with defecation. Physical examination was normal. Blood pressure was also 110/70 mmHg within normal limits. Laboratory tests showed anemia (Hemoglobine was 6.3 g/dl) which necessitated infusion of blood products. Upper gastrointestinal endoscopy was attempted in emergency situation, fresh blood was seen in the lumen of the afferent loop but it was not possible to make a thorough localization. CT-angiogram displayed pseudoaneurysm and extravasation in the vicinity of pancreatoduodenostomy anastomosis (Figure 1) An angiography was performed (Figure 2) Extravasation of contrast material from the dorsal pancreatic artery, a branch of the splenic artery , was observed and selectively cannulated (Figure 3). Then dorsal pancreatic artery was embolized with two 2.5 mm microcoils (Figure 4). After the procedure was completed, the patient showed a progressive improvement. After a- five day observation he was discharged without any problems.
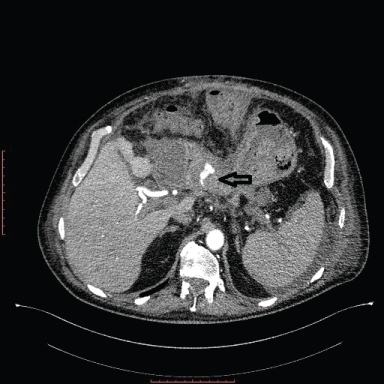 Figure 1: CT-angiogram displayed pseudoaneurysm and extravasation in the vicinity of pancreatoduodenostomy anastomosis. View Figure 1
Figure 1: CT-angiogram displayed pseudoaneurysm and extravasation in the vicinity of pancreatoduodenostomy anastomosis. View Figure 1
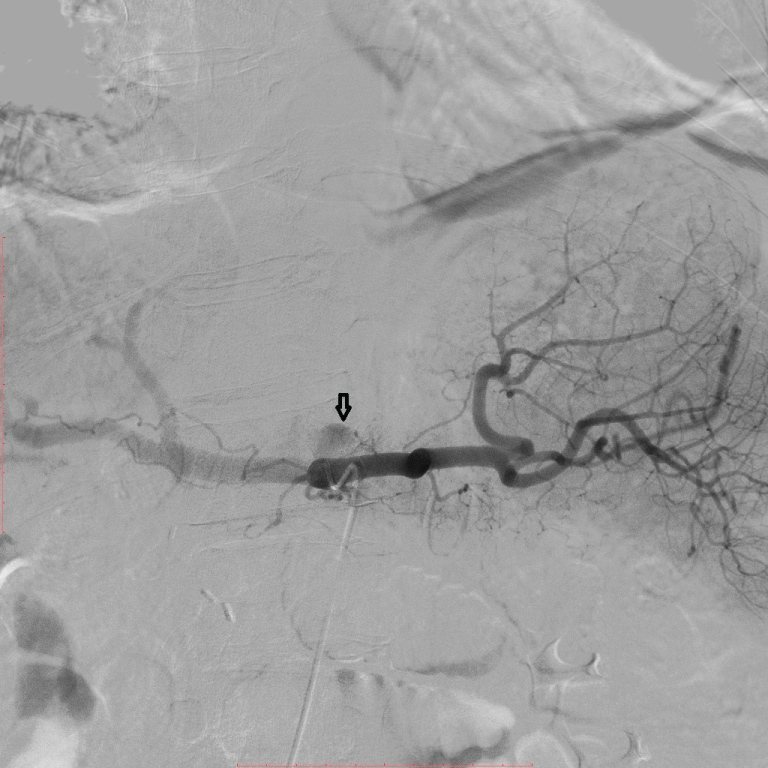 Figure 2: Visceral artery angiography. View Figure 2
Figure 2: Visceral artery angiography. View Figure 2
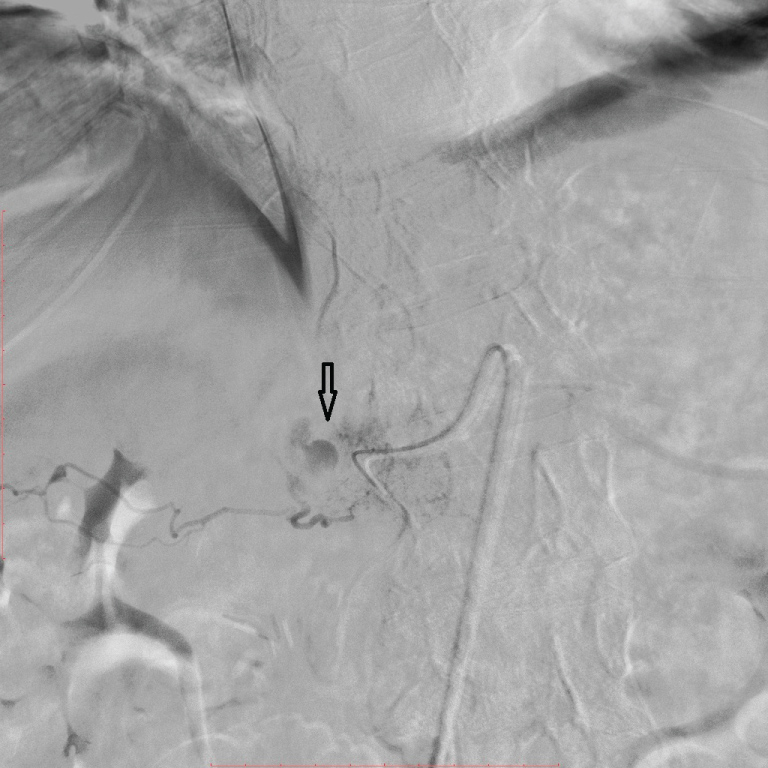 Figure 3: Extravasation of contrast material from the dorsal pancreatic artery. View Figure 3
Figure 3: Extravasation of contrast material from the dorsal pancreatic artery. View Figure 3
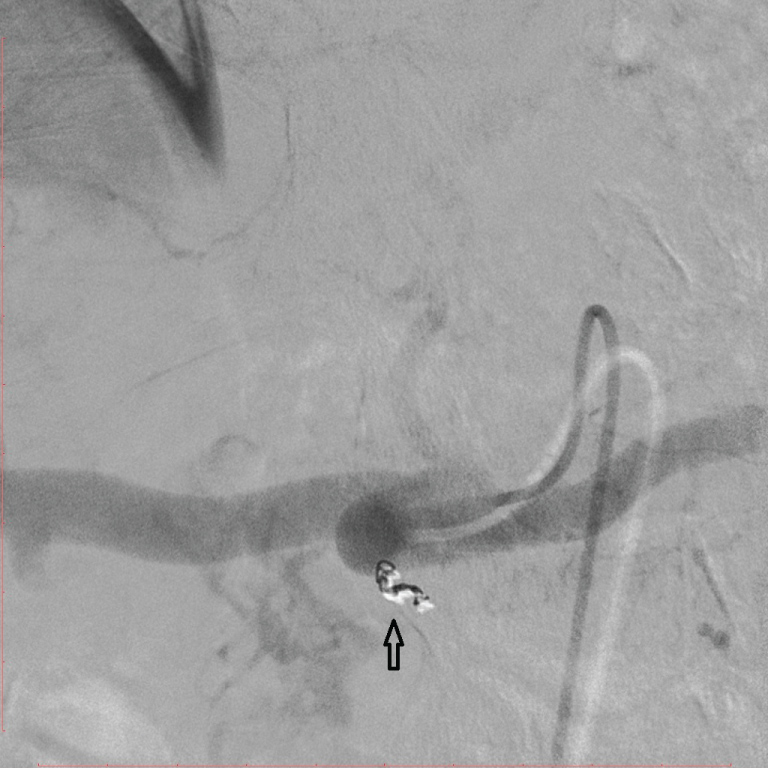 Figure 4: Dorsal pancreatic artery was embolized with two 2.5 mm microcoils. View Figure 4
Figure 4: Dorsal pancreatic artery was embolized with two 2.5 mm microcoils. View Figure 4
A 52-year-old male was operated on with the diagnosis of pancreatic head carcinoma and standard PD was performed. High fever, leucocytosis and signs of peritonitis developed at the 7th day of the operation concomittent with a fistula discharge of 350 ml per day. A reoperation was planned. At surgery, leakage from pancreaticojejunostomy anastomosis and local peritonitis were found. The peritoneal cavity was lavaged with copious amounts of saline. On the fifteenth day of the operation, massive hematemesis and melena occurred. An endoscopy showed massive bleeding from afferent loop. Emergency laparotomy revealed bleeding from pseudoaneurysm located at the gastroduodenal artery stump. Hepatic artery ligation, completion pancreatectomy and and splenectomy were performed. On the third day of the surgery he died of multiple organ failure.
Pancreaticojejunostomy is the most complicated phase of Whipple operation. Leakage of pancreatic anastomosis occurs in 6 to 24% of the patients and leads to a mortality rate of 40% [11]. In many of the cases, however, anastomotic fistula closes spontaneously. The frequency of complications still remains high despite the improvements in intensive care units and surgical technique. Both of the patients we presented here were in sepsis or showed a tendency to sepsis caused by postoperative leakage. In the second case, procedures like abdominal lavage, reoperation, and drainage were not effective. Surgery certainly plays a role, but in a case with severe sepsis, ileus, numerious and dense adhesions in peritoneal cavity, it has not been beneficial.
Doppler ultrasonography which is a noninvasive method for early diagnosis is particularly valuable if pulsatile hematoma is observed [12].
Endoscopic diagnosis is difficult. If it is observed during endoscopic intervention that bleeding has stopped, this could be merely due to the intermittent character of hemorrhage; alternatively, it could be attributed falsely to bleeding of mucosal erosions. If the clots in the afferent loop are completely evacuated , and active bleeding or a pulsatile mass is seen, the diagnosis is precise. Immediate surgical intervention is indicated in this situation. However, the incidence of mortality (16 - 50%) and morbidity (5 - 25%) are high [10,13]. Surgical exploration is quite difficult due to the anatomical distortion caused by the first operation. Probable rate of rebleeding is not low (63%) [14,15]. Moreover, the individual ligation of the hepatic artery cannot be effective. A patient in this situation should be treated only by a completion pancreatectomy.
Thanks to the modern radiological proceedings in recent years, there has been a significant progress in the treatment of post-pancreatectomy pseudoaneurysms. CT-angiography can be preferred for diagnosis. However it is a noninvasive method. Angiography is the best method for diagnosis. It has the superiority of proceeding to transarterial embolization in experienced hands. In transarterial embolization, success rate is 83 - 100%, mortality is 0 - 1% [15-20]. However, even after a successful intervention , it might not be possible to stop the bleeding. In these patients, covered stents may be useful [21].
Transarterial embolization, in our opinion, should be at the top of the list in the treatment of pseudoaneurysms. Exploratory laparotomy , hepatic artery ligation and surgical intervention for completion pancreatectomy should be attempted in case of failed transarterial embolisation.
Written informed consent was obtained from the first patient for publication of this Case Report and any accompanying images. A copy of the written consent is available for review by the Editor-in-Chief of this journal.
Written informed consent was obtained from the second patient's son for publication of this Case Report and any accompanying images. A copy of the written consent is available for review by the Editor-in-Chief of this journal.
The authors declare that they have no competing interests.
TA conceived of the study and participated in its design and coordination and helped to draft the manuscript.
SC participated in the design of the study
IR conceived of the study
ASA conceived of the study and participated in its design and coordination and helped to draft the manuscript.