Leukocyte apheresis is a therapeutic option for moderate-to-severe active ulcerative colitis in Japan. It causes fewer complications, however, leukocyte apheresis requires the use of a relatively large caliber of peripheral venous line for hemodialysis. We reluctantly used a large caliber catheter with a double-lumen into the central vein. Catheter-related thrombosis and infection cases were occasionally observed during leukocyte apheresis. The impact of the catheter size and the thrombosis complication has been not fully elucidated. This was a retrospective study of 15 ulcerative colitis patients using the central vein catheters for the leukocyte apheresis.
We examined data derived from patients receiving leukocyte apheresis over 2 years. Leukocyte apheresis was performed through the peripheral vein in 9 patients, and for 6 patients placed a double-lumen central vein catheter.
Three of 6 patients who used dialysis catheters developed catheter-related thrombosis and sepsis. Another 3 patients who underwent a double-lumen central vein catheter and 9 patients who underwent apheresis through the peripheral vein did not develop obvious infection or thrombosis.
It is important to select as small a caliber of catheter as possible to prevent thrombosis, when we place a central vein catheter in patients in the active phase of ulcerative colitis, as caliber of catheter is associated with thrombus formation. Especially the risk of hypercoagulability increases in the active phase of ulcerative colitis.
Ulcerative colitis, Central vein catheter, Thrombosis, Hypercoagulability, Leukocyte apheresis
UC: Ulcerative Colitis; LA: Leukocyte Apheresis; CV: Central Vein
Ulcerative colitis (UC) is an idiopathic colonic inflammatory disease. In addition to corticosteroids, 5-aminosalicylic acid and conventional immunosuppressive agents, more recent effective drugs such as infliximab, adalimumab, and tacrolimus, have been introduced to the remission induction therapy of UC. However, achieving remission induction therapy is difficult in some cases when inflammation flares up. Leukocyte apheresis (LA) is a therapeutic option for steroid-dependent or steroid-resistant UC patients with moderate-to-severe active steroid UC as described in 'Guidelines for the Management of Ulcerative Colitis in Japan' [1]. The infiltration of leukocytes into the intestinal mucosa plays an important role in the formation of mucosal lesions via the increased production of cytokines and inflammatory mediators [2]. LA is an excellent therapy that removes peripherally circulating activated leukocytes or granulocytes in the blood by the extracorporeal circulation technique of filtration using a leukocyte removal column [3]. In addition, it has fewer complications compared to other drug therapies. Furthermore, it does not require the measurement of blood concentrations of the administrated agent [4,5]. However, LA requires a relatively large caliber peripheral venous line for hemodialysis over several weeks. Sometimes it is difficult to maintain the peripheral venous line in patients with veins in a poor condition. In this situation, we reluctantly place a large caliber catheter with a double- or triple-lumen into the central vein (CV) via the internal jugular vein or the femoral vein for LA. We have occasionally experienced severe catheter-related thrombosis and infection cases with central vein catheters. The impact of the catheter size and the thrombosis complication has been not fully elucidated. We retrospectively collected data derived from patients who received LA over 2 years in our hospital.
Fifteen patients received LA over 2 years in our hospital. LA was performed through the peripheral vein in 9 patients. Six patients received dialysis catheters into the CV. We used a double-lumen catheter (GamCath Dolphin catheter, 11Fr, double lumen, Baxter, Deerfield, IL, USA) for LA in 5 adult patients and a double-lumen catheter (6.5Fr) for 1 pediatric patient. Patient characteristics are shown in Table 1. All catheters were managed in accordance with the Centers for Disease Control and Prevention Guidelines [6]. LA was preformed twice a week, and total parenteral nutrition was administered daily.
Table 1: Characteristics of ulcerative colitis cases associated with leukocyte apheresis. View Table 1
LA was performed safely without complication in 15 patients. Three of 6 patients who received dialysis catheters showed catheter-related thrombosis and sepsis and one patient had catheter occlusion (Table 2). Another 3 patients who underwent a double-lumen central vein catheter and 9 patients who underwent apheresis through the peripheral vein did not develop obvious infection or thrombosis. Seven of 9 patients with apheresis through the peripheral vein underwent single lumen central vein catheter for intravenous alimentation.
Table 2: Complications of ulcerative colitis cases when a catheter was placed into the central vein. View Table 2
Patient case 1 was placed a right inguinal catheter and had swelling and flares on her right lower extremity after 12 days of catheter placement. Computed-tomography scans revealed a wide range of thrombus formation over the right femoral vein to inferior vena cava (Figure 1). We immediately placed an inferior vena cava filter (Figure 2) via the jugular vein and initiated thrombolytic therapy. Patient case 3 was placed a right jugular catheter and showed signs of sepsis; therefore, we removed the catheter on the third day. A thrombus was found on the catheter tip. Acinetobacter was also detected by culture of patient blood and the catheter tip. The patient's fever was improved after catheter withdrawal. Patient case 5 was placed a right jugular catheter and developed remittent fever after the initial LA. We administrated antibiotics and removed the catheter. Thrombus was observed on the tip of catheter. Blood culture and culturing the catheter tip were negative. However, remittent fever was improved after catheter removal. All patients recovered without any after effects.
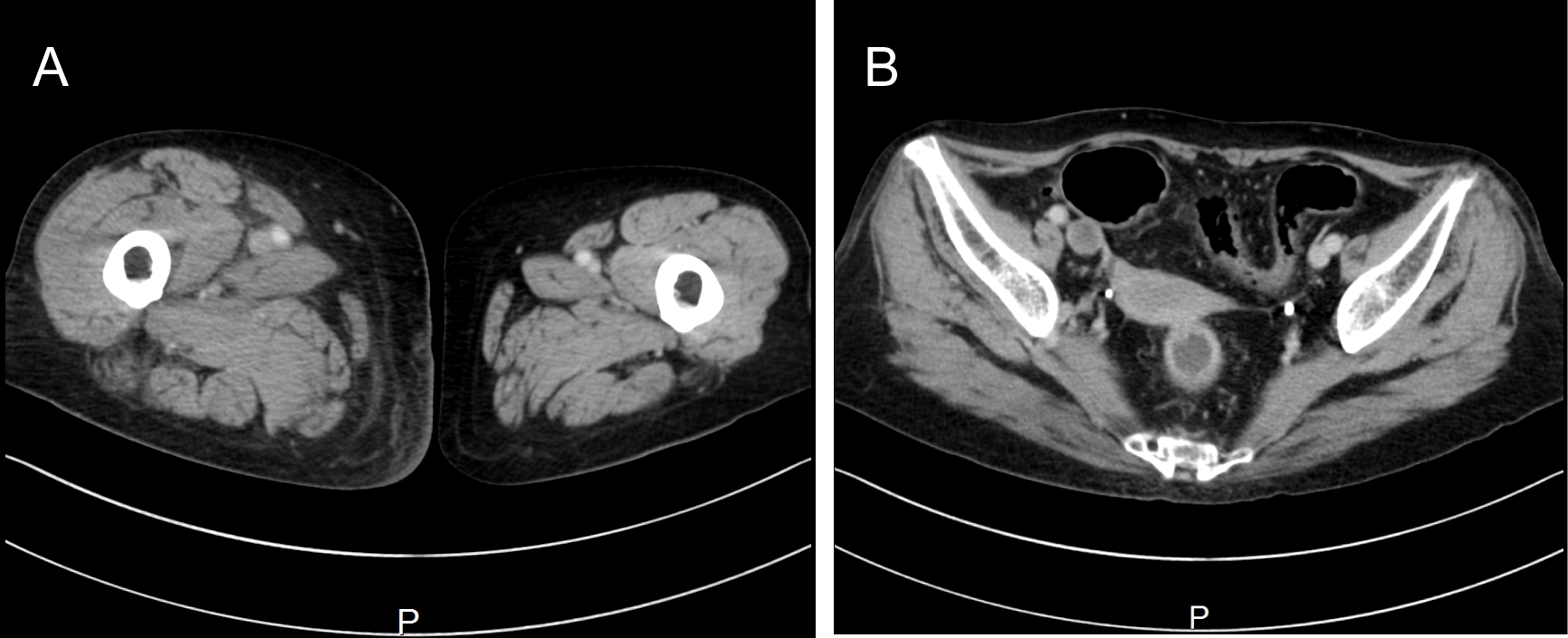 Figure 1: CT scan reveals a swollen right lower extremity (1-a) and filling defect showed thrombosis in the right iliac vein (1-b). View Figure 1
Figure 1: CT scan reveals a swollen right lower extremity (1-a) and filling defect showed thrombosis in the right iliac vein (1-b). View Figure 1
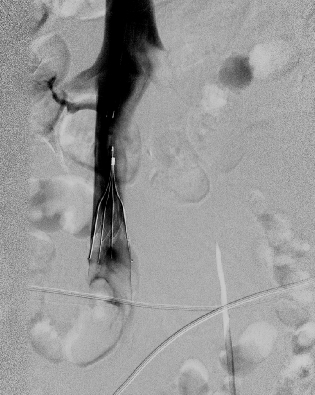 Figure 2: Venography shows a blood clot and the inferior vena cava filter. View Figure 2
Figure 2: Venography shows a blood clot and the inferior vena cava filter. View Figure 2
LA, as stated in 'Guidelines for the Management of Ulcerative Colitis in Japan', is an effective treatment for patients with severe refractory UC. LA was reported to induce remission in 60 -75% of active-staged UC patients [4,5]. However, to perform hemodialysis a relatively large caliber of peripheral venous line is required. Our hospital performs steroid intensive intravenous therapy and LA for patients with refractory UC. In cases where maintaining the intravenous line is difficult because of the poor quality of the peripheral vein, LA is performed by using a CV catheter. It is important to note that we complied with the Maximal Sterile Barrier Precautions in accordance with the Centers for Disease Control and Prevention Guidelines [6] for CV placement.
It is rare to observe thrombosis and infection over such a short period in diseases other than UC. Fifteen cases received LA of which six were performed using dialysis catheters. Complications such as catheter-related thrombosis and sepsis occurred in 3 cases and occlusion in 1 case.
In general, venous thromboembolism is a serious complication of UC [7]. Hypercoagulability has also been shown to increase in the active phase of UC [8,9], and might be caused by a mechanism involving increasing platelet counts and enhancement of the coagulation system [7]. However, in the case of severe UC, we may use a CV catheter for intravenous alimentation in fasted cases, but we do not often experience severe complications such as thrombosis and sepsis with catheter use over a short period. In the present study, a CV catheter (16G, single lumen) was used for intravenous alimentation in 7 patients; however, obvious infection or thrombosis was not detected. The diameter of a 16 G catheter is 1.6 mm; in contrast, the diameter of an 11 Fr catheter for LA is 3.5 mm. An association between thrombus formation and catheter caliber was previously reported [10,11]. In the cases described here, we considered the use of a large caliber catheter the cause of thrombosis and subsequent sepsis.
The Centers for Disease Control and Prevention Guidelines also describe a relationship between thrombosis and catheter infection [6]. In the present cases, catheter-related infections had evolved from the catheter thrombosis. The possible reasons why a large caliber catheter causes thrombosis might be a relative stenosis of the vein into which the catheter is inserted, blood flow stasis and turbulence.
When the active phase of UC shows hypercoagulability, a high risk of catheter-related thrombosis must be considered. The placement of a large caliber catheter into the CV has a high risk of causing thrombosis. Therefore, when we place a CV catheter into patients in the active phase of UC, it is necessary to select as small a caliber of catheter as possible to prevent thrombosis. In conclusion, it is important to pay attention to catheter-related thrombosis for cases when a CV catheter is used in the active phase of UC.
There is no Conflict of Interest about this manuscript for all authors.
Funding: This study was not funded by any grant.
Ethical approval: All procedures performed in studies involving human participants were in accordance with the ethical standards of the institutional and national research committee and with the 1964 Helsinki declaration and its later amendments or comparable ethical standards.
Informed consent: Informed consent was obtained from all individual participants included in the study.
Statement of equal authors' contribution: No coauthor applicable.