The proximal hamstring complex is frequently injured in athletes, traditionally occurring in waterskiing, sprinting and hurdles. However, more recently it is increasingly being reported in a variety of different sports. The hip and knee joint are stabilized by the hamstring muscles due to eccentric contractions, which occur when a muscle contracts whilst passively stretched. This happens to the hamstring muscle during hip flexion and knee extension. Injuries are much more common during eccentric contractions, 12% of hamstring injuries are proximal and of these 9% are complete. The current literature advocates surgical intervention of complete proximal hamstring avulsion injuries with early surgical management associated with better clinical outcomes in terms of pain, function and return to sport. The diagnosis of this type of injury can be challenging due to the complexity of the surrounding anatomy. Injury classifications have been produced in order to understand, diagnose and manage these injuries appropriately. We present a rare variant of a proximal hamstring injury; with plastic deformation of the proximal tendons with the insertions at the ischial tuberosity intact. This type of injury has not previously described or classified in the literature.
Hamstring injuries are common in athletes of all levels. It is important to differentiate between mid-substance muscle and muscular-tendinous injuries, which respond well to non-operative management and more proximal avulsion injuries, which require surgical intervention. Prompt and accurate diagnosis of these injuries allows for earlier surgical treatment, which is crucial in avoiding more complex surgery, post-operative complications, a longer rehabilitation program and thus a delay in the return to play.
We present a case with an unusual finding of a proximal hamstring avulsion injury on MRI imaging. The proximal tendons remain intact but have been stretched past the point of Young's modulus of elasticity, leading to plastic deformation. This results in weakness in the hamstring complex clinically, requiring surgical intervention to improve the overall function of the hamstring muscles. This particular finding has not previously been described in the literature. Informed consent was obtained by the patient. No ethics approval was required.
A 37-year-old male previously fit and healthy presented with left posterior thigh pain after practicing diving from a diving board into a swimming pool. The patient had been performing a range of dives before moving onto the 1-meter springboard. While attempting to dive of this, the desired position to enter the water was not achieved resulting in the left leg being kicked forward. When impact with the water was made the left hip was hyperflexes with the knee in full extension, the trunk was flexed with the right leg underneath, a quasi-hurdling position. The patient immediately complained of a sharp pain, feeling something had snapped and “gone”. He was unable to weight bear at the time of injury.
On examination, no obvious deformity was seen with only minimal bruising present in the posterior thigh. There was pain in the postero-medial aspect of his left thigh with extensive adductor spasm and no sciatic nerve symptoms or signs and no neurovascular deficit. There was no palpable tenderness over the ischial tuberosity. Both hip extension and knee flexion were reduced with a score of 2/5 for overall hamstring power. Spinal movements were normal although flexion was limited by posterior left thigh pain. An MRI scan was requested for further investigations and initially reported as a full thickness tear and disruption of the medial portion of the proximal hamstring common tendon with retraction and 12 cm gap between the two segments. The working diagnosis at this stage was a complete proximal hamstring avulsion injury. The decision to treat this surgically was made where the uniqueness of this injury became apparent. The time to surgery from initial injury and diagnosis was 16 days.
The normal hamstring complex consists of three muscles; biceps femrois BF, semimembranosus SM and semitendinosus ST. The adductor magnus muscle has a tendinous slip originating from the inferno-medial aspect of the ischial tuberosity and is sometimes referred to as the hamstring component. The general consensus is to view the hamstring complex as the three muscles of BF, ST and SM.
This is considered as a double muscle, having a long and short head. The long head arises from the medial facet of the ischial tuberosity and the short head from the lateral supracondylar ridge of the linea aspera of the femur. The origin of the biceps on the femur has been used as a landmark to distinguish between proximal and distal injuries [1] and both the proximal distal tendons span the entire length of the muscle. There is dual innervation with the long head innervated by the tibial and the short by the peroneal. This may lead to asynchrony in co-ordination and intensity of stimulation and has been put forward as a reason for this muscle having the highest frequency of tears [2].
This is a single muscle arising from the inferomedial aspect of the ischial tuberosity. It is thought to form a conjoint tendon with the long head of BF. The great length of this muscle has been thought to pre-dispose it to rupture [3]. It is innervated by the tibial nerve.
This originates on the superolateral aspect of the ischial tuberosity beneath the proximal half of ST. The SM tendon runs medially and anteriorly to the other hamstring tendons. As with BF the proximal and distal tendons span the entire length of the muscle. The innervation is from the tibal nerve.
The procedure was carried out under general anesthetic with the patient in the prone position. A longitudinal midline incision in the posterior thigh was used and diathermy hemostasis was obtained. The hamstring complex was accessed without any difficulty with very little hematoma formation. The sciatic nerve was identified and protected throughout. The biceps femoris was intact. The ischial tuberosity was identified, and the hamstring insertions appeared viable and stable. The entire tendon of semimembranosus was almost denuded for 20 cm and the muscular portion had retracted distally. This was identified and mobilized. It was then brought back up and overlapped to shorten it backup and bring tension into it and into the muscle and then repaired on itself with No5 Ethibond Kessler sutures soft tissue to soft tissue, bringing the muscle back up under tension. It was reinforced with 1.0 Vicryl, muscle to tendon sutures. A good repair was obtained, and a thorough washout performed.
This is a most unusual injury in that the muscle off the tendon of semimembranosus had been stripped off and de-functioned the semitendinosus, which had plastically deformed and retracted; this is illustrated in Figure 1a, Figure 1b. The rehabilitation program is outlined in Table 1. At present the patient is progressing well through the rehabilitation program and is expected to make a full recovery returning to pre-injury activity levels. A full return to sport is generally predicted at 24-28 weeks.
 Figure 1: (a) MRI scans illustrate high signal at ischial tuberosity extending down the entire tendon of the medial portion; (b) This correlates with surgical findings of an intact proximal tendon origin with plastic deformation and defunctioning semi-tendonosis.
View Figure 1
Figure 1: (a) MRI scans illustrate high signal at ischial tuberosity extending down the entire tendon of the medial portion; (b) This correlates with surgical findings of an intact proximal tendon origin with plastic deformation and defunctioning semi-tendonosis.
View Figure 1
Table 1: Rehabilitation Protocol Used. View Table 1
Proximal hamstring avulsion injuries are increasingly being recognized and the frequency is increasing amongst athletes in a variety of sports [4,5]. The current literature advocates surgical intervention for complete hamstring avulsions with better functional outcomes recorded and a faster return to sports in those patients being operated on acutely within 4-6 weeks of the original injury [6]. Magnetic resonance imaging, MRI remains the modality of choice for diagnosis [1,7]. Despite advances in radiographic imaging techniques, the diagnosis of proximal avulsions remains challenging in part due to the complex anatomy in this region. A specific MRI classification for proximal avulsion injuries has been described based on the anatomical location and amount of retraction of the proximal complex [8]. This is shown in Table 2. Typically Type 5 injuries are delayed presentations, indicating that the tendons may retract with time [8].
Table 2: Classification of Proximal Hamstring Injuries. View Table 2
Despite the classical history and mechanism of injury described in this particular case, with the hip hyperflexes and knee extended [7], the type of proximal hamstring injury described in this case is a rare variant of those previously documented. The proximal tendon structure remains at its insertion on the ischial tuberosity but loses its functional elastic recoil properties as it the tendons are stretched beyond the point of Young's modulus. After this point is reached plastic deformation occurs where the tendon does not return to original shape once load is removed. This is shown in Figure 2 below. Clinically, this leads to weakness and overall decreased function in the hamstring complex, affecting the patient's ability to participate in sporting activities. This should be considered when interpreting MRI images in conjunction with the clinical history and examination findings. Surgical intervention is recommended as the treatment for this type of injury.
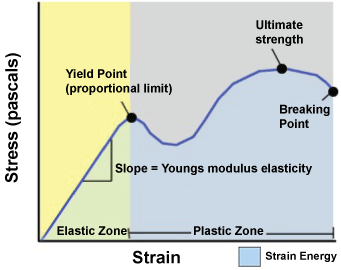 Figure 2: This graph illustrates the stress/strain relationship and Youngs Modulus of elasticity, beyond which plastic deformation will occur.
View Figure 2
Figure 2: This graph illustrates the stress/strain relationship and Youngs Modulus of elasticity, beyond which plastic deformation will occur.
View Figure 2
Diagnosis of these injuries should be made early to facilitate surgery and allow for a more efficient rehabilitation program and quicker return to sport. MRI remains the imaging modality of choice and the clinician should be aware of the variations associated with proximal hamstring avulsion injuries. We present a further variant of this specific injury, which responds well to surgical management and should be considered when interpreting MRI images.