The case study of a non-small cell lung carcinoma confirmed by complete necropsy study is reported in an old man with apathetic hyperthyroidism, atrial fibrillation and heart failure. The authors emphasize diagnostic challenges related to effects of hyperthyroidism on nutritional status versus under nutrition caused by unsuspected development of a coexistent malignancy. Moreover, main features and diagnostic pitfalls of apathetic hyperthyroidism are commented. The aim of this report is to enhance the suspicion index of primary health care workers about the possibility of concomitant benign and malignant conditions with similar manifestations.
Apathetic hyperthyroidism, Autopsy, Lung cancer, Toxic adenoma
Apathetic hyperthyroidism is an uncommon condition described by Lahey FH (1931), which may evolve as heart failure or clinically undetected, easily mistaken by malignant disease [1-5]. The prevalence of hyperthyroidism ranges from 0.5 to 2.3% after the age of 60 years, whereas apathetic hyperthyroidism may be found in up to 15% of older people with thyrotoxicosis [5]. Clinical detection of hyperthyroidism in the elderly is often delayed if manifested by fatigue, weakness, weight loss, insomnia, depression, mental confusion and variable apathy [1-6]. Episodes of atrial fibrillation and heart failure in this scenery should raise the suspicion [3,4,6]. Hyperthyroidism coexistent with thyroid cancer is a scarcely reported entity (1.2-13.3%), more often related to cases of Graves' disease, toxic multinodular goiter or toxic adenoma [7]. Herein is reported a non-small cell pulmonary carcinoma diagnosed by complete necropsy performed in an old male with apathetic hyperthyroidism, atrial fibrillation and heart failure. Paraneoplastic hyperthyroidism due to lung carcinoma or germ-cell tumor is also commented.
A 68-year-old heavy smoker was admitted with heart failure diagnosed nine months before. He was in regular use of digoxin and diuretic, low-sodium diet and potassium supplementation. In the last four weeks, he evolved with apathy and fatigue, palpitation, hyperhidrosis, and weight loss (5 kg) in spite of normal appetite. Physical examination revealed BMI: 17 kg/m2; PA: 150/70 mmHg; heart rate: 100 bpm and rhythm of atrial fibrillation; palpable elastic node (± 1.0 cm) in the right thyroid lobe; moderate hypotrophy of scapular girdle, and muscular weakness in lower extremities; and lack of moist and warm skin, fine tremor in extremities, conjunctival congestion, eyelid retraction, or deficit of convergence in the eyes. Worthy of note, this patient had never utilized amiodarone either before or during his hospitalization. The hypothesis of hyperthyroidism was confirmed by laboratory tests showing reduced level of TSH (< 0.01 µU/l), and elevated levels of free T4 (3.8 ng/dL) and free T3 (5.0 pg/ml). The ultrasonography of the neck showed a solitary nodule (0.8 cm) in the right thyroid lobe. Furthermore, hot image of the nodule with decreased uptake in the remaining parenchyma by the scintigraphy study with Tc-99m pertechnetate was consistent with case of toxic adenoma. Except for weight loss, he had significant improvement with radioactive iodine-131 ablation. After discharge that occurred on D23 he was followed in Endocrinology outpatient service. Ten months later, he was admitted in poor general clinical status, progressive breathlessness, productive cough, cyanosis, bilateral jugular vein distention, bilateral pleural effusion (more voluminous at the left side), PA: 170/90 mmHg; heart rate: 120 bpm, rhythm of atrial fibrillation, hepatomegaly, absence of signs of ascites, and mild bilateral lower limb edema. The chest radiography showed opacity in the upper left lobe and elevation of the ipsilateral lung hilum, suggestive of partial atelectasis with mediastinal enlargement (Figure 1A, Figure 1B and Figure 1C). The routine laboratory determinations on admission did not reveal remarkable alterations. Anti-thyroid autoantibodies were negative; human chorionic gonadotrophin (HCG), alpha-fetoprotein, lactate dehydrogenase, serum magnesium and calcium were in normal values. During hospitalization, there was gradual severity of heart failure (Figure 1D and Figure 1E), that was unresponsive to intensive care management, and his death occurred 11 days after admission. The authorized autopsy study confirmed the diagnoses of thyroid benign disease; pulmonary congestion and bilateral pleural effusion due to hypertensive heart failure; in addition to atelectasis of the left upper lobe due to a pulmonary epidermoid carcinoma (Figure 2).
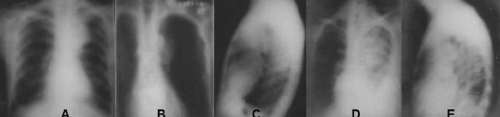 Figure 1: (Chest radiographs) A to C: Opacity in the upper left lobe and elevation of the ipsilateral lung hilum, suggestive image of atelectasis with mediastinal enlargement; D and E: Gradual increase of parenchymal opacity volume, cardiomegaly, and bilateral pleural effusion.
View Figure 1
Figure 1: (Chest radiographs) A to C: Opacity in the upper left lobe and elevation of the ipsilateral lung hilum, suggestive image of atelectasis with mediastinal enlargement; D and E: Gradual increase of parenchymal opacity volume, cardiomegaly, and bilateral pleural effusion.
View Figure 1
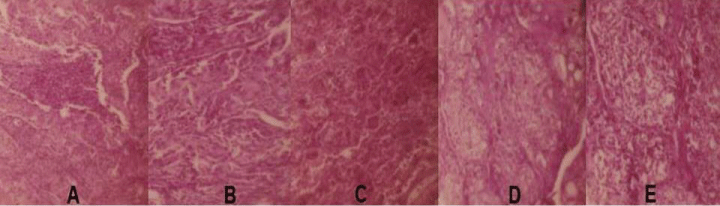 Figure 2: (Photomicrographs; H&E stain, ×100) A: Features of the epidermoid pulmonary carcinoma with a central area of necrosis; B: Detail of tumor cells showing images of anaplasia and cornification; C: Aspects of the pulmonary area with atelectasis and congestion; D and E: Hyperplasia of thyroid acini with high cubic and columnar cells of clear cytoplasm and peripheral nuclei, in addition to almost total absence of colloid within the smallest acini.
View Figure 2
Figure 2: (Photomicrographs; H&E stain, ×100) A: Features of the epidermoid pulmonary carcinoma with a central area of necrosis; B: Detail of tumor cells showing images of anaplasia and cornification; C: Aspects of the pulmonary area with atelectasis and congestion; D and E: Hyperplasia of thyroid acini with high cubic and columnar cells of clear cytoplasm and peripheral nuclei, in addition to almost total absence of colloid within the smallest acini.
View Figure 2
The patient herein reported had apathetic hyperthyroidism due to a toxic adenoma, coexistent with non-small cell pulmonary carcinoma, as well as obstructive atelectasis, and heart failure. Because thyroid nodules with subnormal TSH do not exclude the possibility of malignancy, the amplitude of differential diagnosis had to be widened to avoid misdiagnosis of cancer [6]. The main differential diagnoses were discarded, including toxic multinodular goiter, Graves' disease, Hashimoto's thyroiditis with thyrotoxicosis, amiodarone-induced thyrotoxicosis, excessive intake of thyroid hormones, increased secretion of TSH, and thyroid cancer [3,6,7]. Additional concerns were about rare hypotheses as ingestion of thyroid-contaminated food [8], and paraneoplastic hyperthyroidism due to mediastinal germ-cell tumor or lung malignancy [9,10].
In The Netherlands, Oosting SF, et al. (2010) evaluated occurrences of paraneoplastic hyperthyroidism in 144 patients presenting metastatic non-seminomatous germ-cell tumors. The authors detected five patients (3.5%) with hyperthyroidism and elevated levels of HCG [10]. van Kooten MJ, et al. described transient thyrotoxicosis soon after starting nivolumab to treat non-small-cell lung carcinoma, followed by a rapid transition to hypothyroidism [11]; phenomena that enhance the diagnostic challenges involving this cancer and thyroid function.
In Denmark, Miret M, et al. reviewed paraneoplastic syndromes in a cohort of 33,755 patients with non-small cell lung carcinomas and reported that the most prevalent (3.0%) potential syndromes in the group were endocrine and metabolic conditions. The incidence rate difference per 1000 persons-years, and the adjusted hazard ratio (95% CI) in comparison with general population were 16.1 (14.7-17.5) and 3.4 (3.1-3.6), respectively; and adjusted hazard ratio of 146 cases in subcategory of thyroid condition was 2.3 (1.9-2.8) [12].
Sato K, et al. (2018) studied 38 patients in Japan, with non-small cell lung carcinomas (26% squamous) treated by nivolumab, median age 68.5 years, 74% male, and 68% heavy smokers; hypothyroidism and hyperthyroidism were usual immune-related adverse effects [13]. The above-mentioned findings indicate that novel cancer therapies utilized in the growing population of elderly can origin endocrine adverse-effects, which increase diagnostic pitfalls. Precocious manifestations of thyrotoxicosis may evolve unsuspected in elderly individuals, whereas atrial fibrillation and cardiac failure are very frequent findings in this condition. Early diagnosis of apathetic hyperthyroidism allows due treatment and lower morbidity and mortality; however, the progressive weight loss with muscular weakness can mimic malignant entities. Hyperthyroidism can also occur associated with thyroid malignancy, or cancer of other origin. Therefore, one must highlight the importance of broad differential diagnoses, in special in the elderly patients presenting with unspecific clinical manifestations.
Other major concern should be about hyposkillia, a novel term that refers to insufficient clinical skill in procedures of medical practice. In fact, up to 20% of clinical misdiagnoses are related to inaccurate anamnesis and physical examination, in addition to equivocal interpretations of the complementary investigations [14]. Finally, but not the least, the authors highlight the role of autopsy studies to better clear some causes of death.
This patient with apathetic hyperthyroidism also had a pulmonary cancer diagnosed during the autopsy. The main purpose of this case report of about an elderly patient with a constellation of symptoms herein described is to emphasize the possibility of benign and unsuspected malignant conditions developing in concomitance. Case reports may enhance the suspicion index about less common diagnostic conundrums.
The authors would like to thank Almir José Batista, the official photographer of the Armed Forces Hospital, in Brasília-DF, Brazil for the images that illustrate the present case study.
The authors of this manuscript declare that had substantial contributions to the conception and design of the work; in the acquisition, analysis, and interpretation of clinical and laboratory data; in drafting and revising it critically for important intellectual content; in final approval of the version to be published; and in agreement to be accountable for all aspects, ensuring that questions related to the accuracy and integrity of any part of the manuscript were appropriately investigated and resolved. They also declare that do not have any potential conflict of interest to disclose, and there was no financial support for this work.