On January 2020, in Wuhan was officially identified an outbreak of a novel-coronavirus related pneumonia. On February 11th, 2020, WHO named the disease COVID-19 and the virus SARS-CoV-2 [1].
In Europe the outbreak due to SARS-CoV-2 took place in Lombardia and Veneto regions which are located in northern Italy. As April 30th, in Italy there were a total of 205,463 SARS-CoV-2 positive cases, with 18,149 in-hospital patients and 27,967 COVID-19 related deaths [2].
Patients with COVID-19 have a wide range of symptoms: Fever, dry cough and dyspnea being the most common; other symptoms can include myalgia or fatigue, runny nose, diarrhea and vomiting. Some patients might experience anosmia and ageusia [3].
Currently published reports on skin manifestations in patients with laboratory confirmed COVID-19 are scarce [3,4]. A study from Recalcati, et al. highlighted that cutaneous manifestations were detected in 20.4% of COVID-19 patients admitted to hospital in Italy, some of them were present at the onset of the disease or alternatively after the hospitalization when medical treatment has been initiated [5].
A more recent study from France reports a case of urticarial eruption appearance in a COVID-19 patient before the onset of any fever or respiratory symptoms. 48 hours later patient was tested positive for SARS-CoV-2 and treated with paracetamol and antihistamines [6].
Herein we present a unique case of cutaneous manifestation in a patient with SARS-CoV-2 infection which occurred during the high symptomatic phase (symptoms storm) of COVID-19 when the patient was not assuming any drugs which could elicit an allergic reaction unlike those reported by Recalcati who were in-hospital patients under medical treatment. Of note, about twenty days after recovery from COVID-19 the patient also underwent to neutralizing antibody assay.
An asymptomatic 62-years-old man was tested positive for SARS-CoV-2 after unprotected direct contact with a symptomatic COVID-19 patient. He had no comorbidity and he was isolated at home. On the basis of current guidelines he didn't take any drugs [7,8].
Seven days after being positive at swab test, he presented malaise, high fever (39 °C), dry cough without dyspnea. On physical exam he had no pleural friction rubs or lung crackling noise. No laboratory data were collected because of his home quarantine.
On day 10th after the positive swab test, during "symptoms-storm", he presented a no itching erythematous rash localized only at the trunk resembling chicken-pox. Patient was not assuming any medication.
He had fever and cough for the following five days and on day 14th he underwent swab test control which resulted yet positive. At this time cutaneous manifestations were still present (Figure 1).
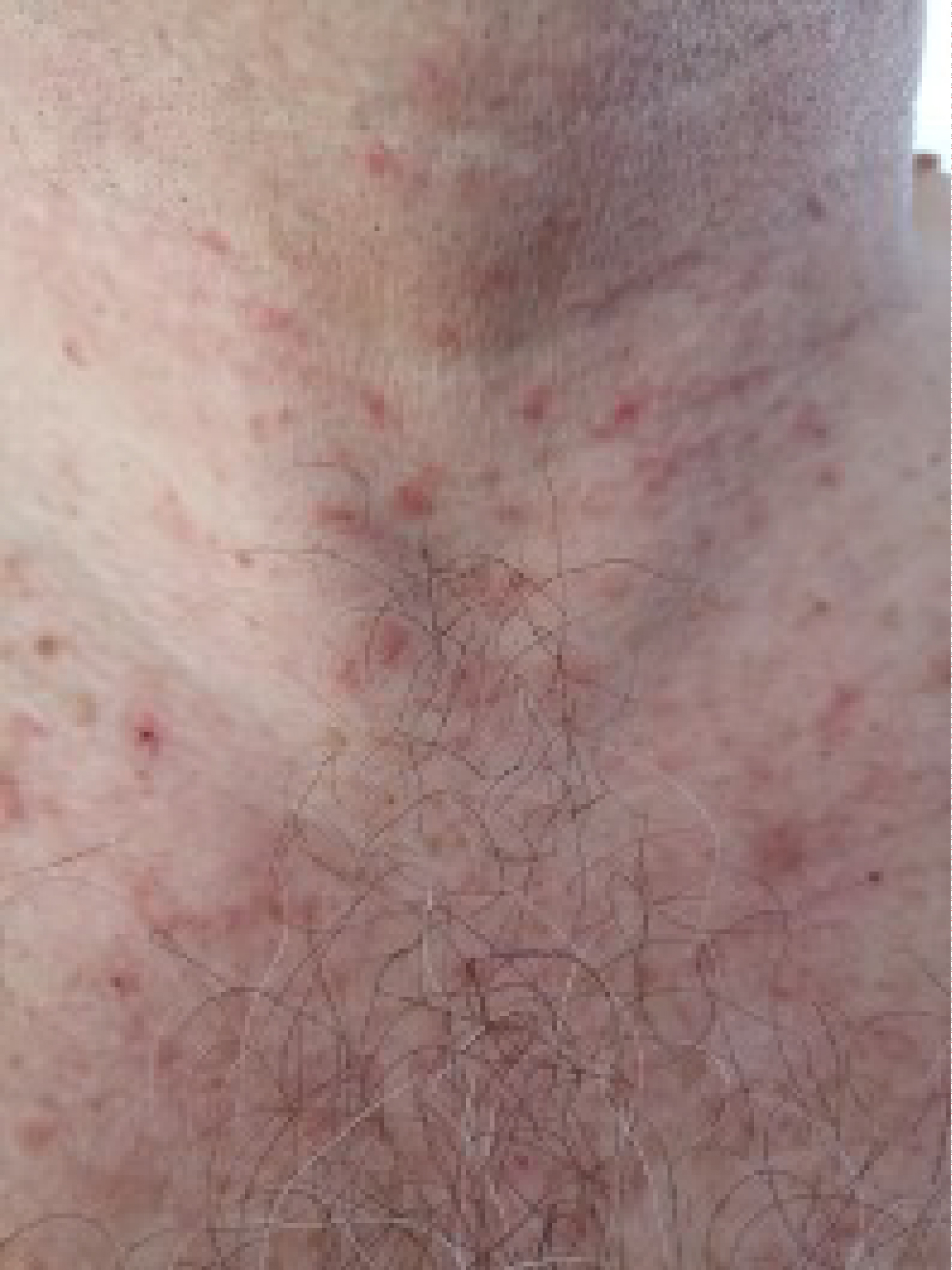 Figure 1: Skin lesions on day 14th.
View Figure 1
Figure 1: Skin lesions on day 14th.
View Figure 1
Twenty days after the onset of symptoms he resulted negative on two swab samples collected at 24 hours apart but skin lesions were only attenuated.
The patient experienced complete recovery of cutaneous manifestations 30 days after diagnosis of SARS-CoV-2 infection (Figure 2).
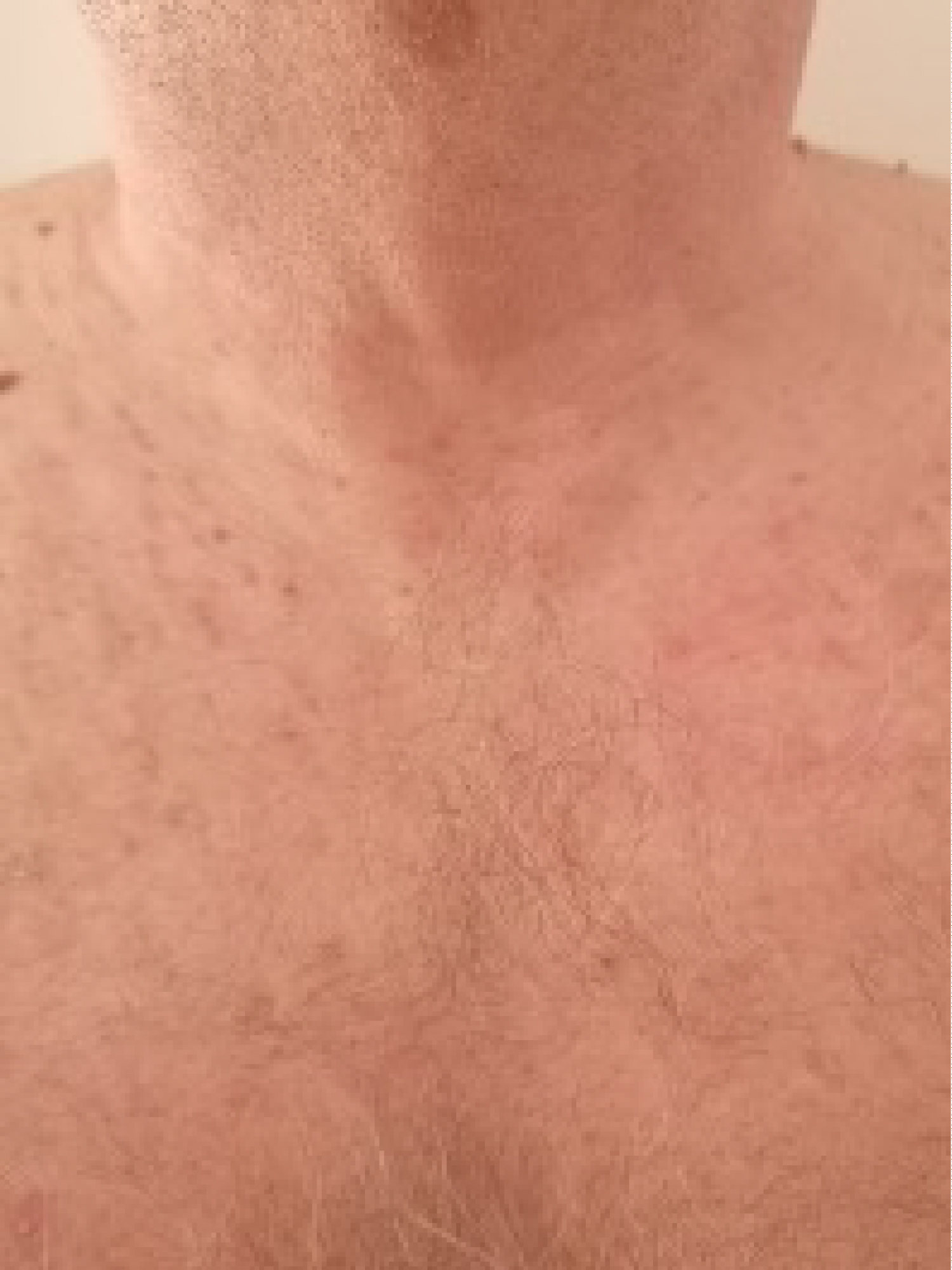 Figure 2: Skin lesions after recovery on day 30th.
View Figure 2
Figure 2: Skin lesions after recovery on day 30th.
View Figure 2
The anti-SARS-CoV-2 antibody assay was performed nineteen days after the second negative nasopharyngeal swab test control. The antibody titer was 1:80. We highlight that the test was performed with a viral neutralization method: This assay detects antibody capable of inhibiting virus replication (i.e., neutralize virus infection) testing scalar dilutions of the serum with fixed quantities of virus [9].
The association between urticaria and general viral infections is common either in children and adults but the real role of viruses in the pathogenesis of skin lesions still needs to be clarified [10]. According to Shipley [11], 0.16% of in-hospital patients experience drug-induced urticaria, commonly due to antibiotics (penicillin and sulfonamides) or nonsteroidal anti-inflammatory drugs. SARS-CoV-2 infection is preferably associated with respiratory symptoms and less is known about cutaneous, cerebral or cardiovascular manifestations. No specific treatment is available. In symptomatic cases it is based on empiric antimicrobials, antipyretics and, in selected cases, on antiviral and chloroquine or hydroxychloroquine. These drugs could cause skin manifestations and their role on SARS-CoV-2 related skin lesions should be evaluated.
Particularly interesting in this case is the natural course of the COVID-19 related skin manifestations completely unrelated to pharmacological-induced interactions. Such manifestations did not require any additional therapy such antihistamines and steroids.
Moreover unlike previous reports, the skin manifestations became evident only during the "symptoms-storm" phase and disappeared several days after swab test became negative.
In conclusion according to this case report:
1) Skin manifestations during SARS-CoV-2 infection might become evident during the "symptoms-storm" phase
2) They are unrelated to COVID-19 drugs treatment
3) They do not require any specific drug treatment
4) They will disappear very late even after swab test became negative.