A 21-year-old active duty soldier presented with skin lesions distributed on his face, arms, and hands. Two weeks prior to presentation he characterizes the development of lower lip herpetic lesion. He was otherwise well. Three days prior to presentation he was given Valtrex 1000 mg BID. He describes expressing fluid from lesions located bilaterally on his mandibular surface. Later that day, the lesions spread to his arms bilaterally. Throughout the day his hands started progressively swelling. He denies fevers. His past medical history is only significant for oral HSV.
Examination revealed scattered skin-colored papules with an erythematous base on the face and arms. Lesions on the chin and submental area were present and had an overlying crust. The inferior vermillion was notable for significant crusting, while two small skin colored plaques were present on the superior vermillion (Figure 1). The patient's palms were a beefy red color bilaterally with central clearing on the left and a small focal clearing on the right hand. The proximal hands had small erythematous papules that coalesced to form a large continuous plaque on the distal aspect of the hands and fingers. The dorsal aspect of the hands and fingers contained erythemic papules and plaques (Figure 2). Initially, there were no vesicles, ulcers, hyperkeratosis, bullae, drainage, or warmth associated with any of the lesions. Bullae developed later.
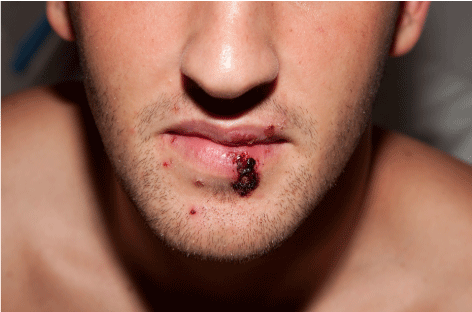 Figure 1: Skin colored papules with an erythematous base and overlying crust.
View Figure 1
Figure 1: Skin colored papules with an erythematous base and overlying crust.
View Figure 1
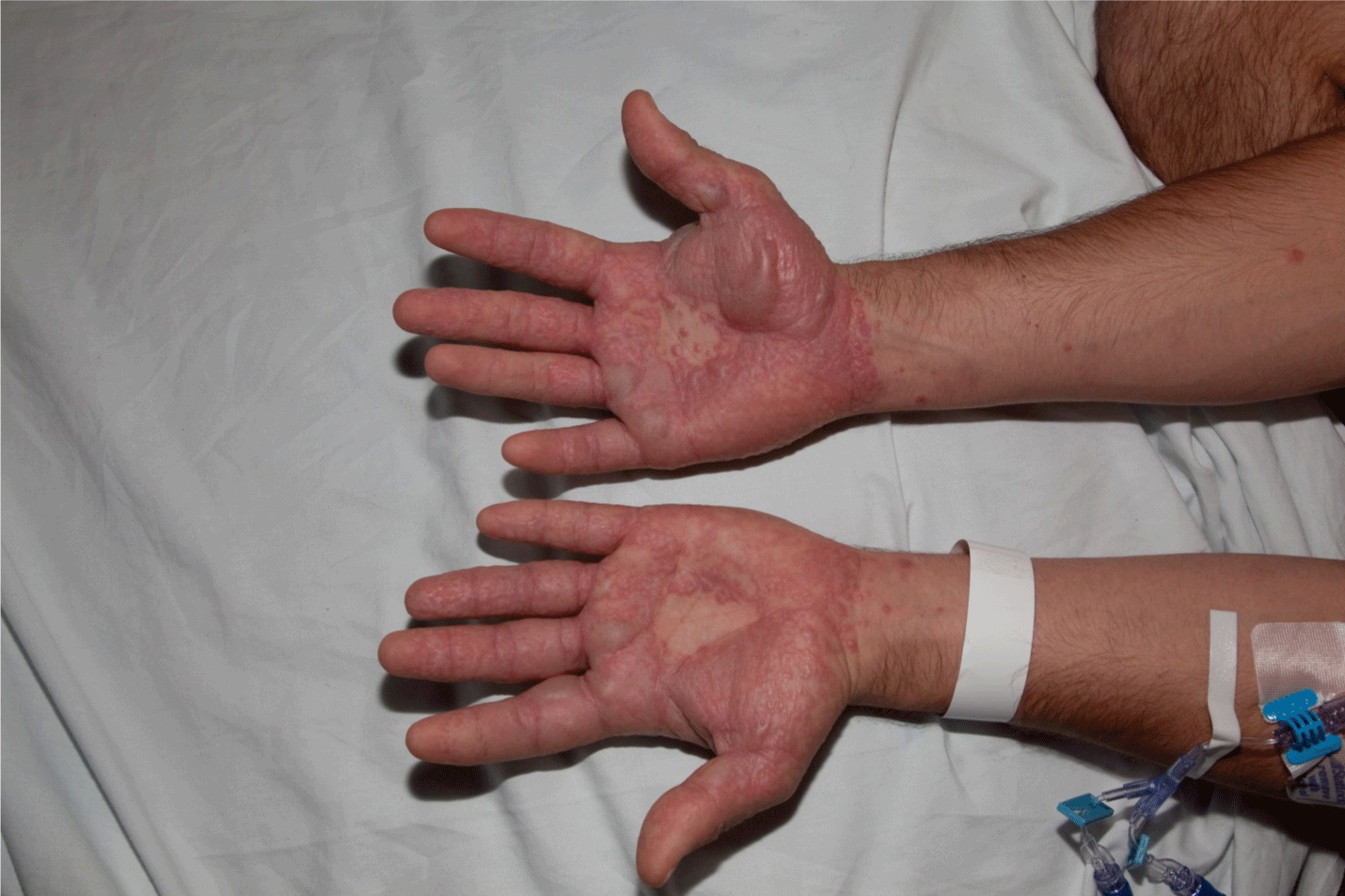 Figure 2: Erythematous papules and plaques with bullous formation.
View Figure 2
Figure 2: Erythematous papules and plaques with bullous formation.
View Figure 2
Based on the patient's history and physical examination, which one of the following is most likely?
A. Urticaria
B. Fixed drug eruption
C. Stevens-Johnson Syndrome
D. Erythema Multiforme
E. Bullous pemphigoid
See the following page for discussion.
The answer is D. Erythema multiforme (EM) was first described by Ferdinand von Hebra in 1866 [1] and is distinct process from Stevens-Johnson syndrome. EM is most frequently secondary to the herpes simplex virus (HSV) [1,2] which causes an immune mediated reaction [2] with cutaneous manifestations. After HSV, the next two most common causes of EM are Mycoplasma pneumonia infection and drugs; with non-steroidal anti-inflammatories (NSAIDS) and sulfa medications being the most common [1,2]. There are a number of other medications that have been implemented in causing EM. There are a few case reports of vaccinations leading to EM [3] as well as certain malignancies [2].
Classically, the lesions of EM are symmetric on the extremities, particularly on the acral extensor surfaces. The palms or plantar surfaces are often involved [1,2]. The "target" lesion is characteristic. Additional morphologies include: Erythemic macules, papules, lesions resembling urticaria, vesicles, and bullae [4].
EM is a self-limiting process. The lesions often develop over a few days and resolve within one to four weeks. Itching, burning, swelling, pain, and post-inflammatory hyperpigmentation [2] are also described as part of the sequelae of EM. Recurrent EM (greater than six times per year) and persistent [1,5,6] EM have been described. EM is a clinical diagnosis for which there is no lab test. Treatment of EM consists of stopping all new medications if there is concern for a drug induced source. Current evidence suggests that antiviral drugs do not change the course of EM; however, these medications are often prescribed. Symptomatic treatment using antihistamines and topical steroids is warranted [2]. Treatment with antibiotics and possibly hospital admission are recommended if the underlying source is Mycoplasma pneumoniae infection [1,2,6]. A brief description EM as well as the other answer choices can be found in Table 1.
Table 1: Clinical description of dermatologic changes. View Table 1
Urticaria is a generalized pruritic skin reaction due to histamine release, causing areas of edematous plaques surrounded by an area of erythema (wheals) [4,7] These lesions are typically pink to skin-colored and vary in size and shape [4]. Urticarial lesions may also present with burning or pain. The lesions suddenly appear and can continue to reoccur [7]. Acutely, urticaria can last for up to six weeks, while chronic urticaria is defined as lasting longer than 6 weeks [7]. Treatment consists of removing the offending agent and treating with antihistamines. Initially a single antihistamine (H1 blocker) may be given. If this is not effective, a second agent can be added. Alternatively, the initial medication can be given at a higher dose. Hot water can worsen the lesions, thus should be avoided. Topical steroids are not indicated. Prednisone can be used in acute urticaria but is not indicated for chronic urticaria [4].
A fixed drug eruption is a cutaneous drug reaction marked by solitary, round, well demarcated, bright red to dusky erythemic macules or plaques that can also form bullous lesions [4,7]. The lesions from a fixed drug eruption will continue to form in the same location with each additional drug exposure [4]. These lesions typically blister, crust and/or desquamate, and are associated with pruritis and burning. Fixed drug eruptions are most often found on the genitalia and perianal area [7] but can occur anywhere. Fixed drug eruptions are associated with a refractory period in which the agent does not activate new lesions. Often a challenge test confirms the diagnosis [4].
Patients with Stevens-Johnson Syndrome (SJS) present after reacting to initial medication ingestion. A prodrome may precede the mucocutaneous lesions by a few days [7]. Those affected are usually children or young adults [4] presenting with widespread atypical target lesions [2] or macular purpuric lesions associated with skin tenderness and burning; erosions and bullous lesions may also be evident on the mucosal surfaces [4]. The skin lesions of SJS are centrally distributed on the face, trunk, and proximally on the upper extremities [7]. Lesions on the oral mucosa may be covered with a thick crust; and conjunctivitis, corneal ulcerations, and uveitis may affect the eyes [4]. Lesions spread distally, and patients will have multiple systemic findings [2] Stevens-Johnson syndrome can involve between 10-30% total body surface area (TBSA) desquamation. When the desquamation exceeds 30% TBSA, the disease is termed toxic epidermal necrolysis (TEN) [8]. Differentiating SJS from EM is important as SJS/TEN is life threatening, and the course of treatment is substantially different.
Bullous pemphigoid is an autoimmune, inflammatory, subepidermal blistering disease that is associated with pruritic urticarial, erythemic plaques and tense bullae [2,4], typically in patients over 60 [7] years of age. Bullous pemphigoid lesions are typically found in skin folds, skin flexures and dependent areas [4]. Bullous pemphigoid lesions are sporadic, and patients initially present with findings consistent with urticarial and subsequently develop bullous lesions. Bullous pemphigoid can be triggered by drugs and UV light. Bullous pemphigoid does not produce a Nikolsky sign [7]. The diagnosis is made via histology and direct immunofluorescence [4]. Localized lesions are treated with topical corticosteroids and prednisone is used in widespread presentations [7].