Acute lymphoblastic leukemia (ALL) is an unusual diagnosis in the adult population. These cases are rarely reported in combination with ischemic stroke and endocarditis. We present a case of an elderly female patient presenting with acute hyperleukocytosis and new diagnosis of ALL, border-zone ischemic stroke and nonbacterial thrombotic endocarditis.
81-year-old female presented to an outside emergency room with subacute onset of left facial weakness and right hemiparesis for 12 hours. A non-contrast CT scan of the head and CTA head and neck showed no acute findings. Laboratory results were remarkable for a leukocyte count of 245.75 k/uL. She was diagnosed with acute leukemia and transferred to a comprehensive stroke center where she was treated with leukapheresis and hydroxyurea. The patients focal deficits somewhat improved, but in the following days, became confused and aphasic. Brain MRI showed bilateral acute border-zone ischemic infarcts (Figure 1). Echocardiogram was also ordered as part of the routine stroke work up. It detected a mobile mass on the ventricular side of the mitral valve leaflet concerning for nonbacterial thrombotic endocarditis. The patient was a febrile and blood cultures were negative on four repeated occasions, seven days apart. The family chose not to pursue any further invasive work up given her aforementioned wishes, and she was eventually discharged to home hospice with comfort care with palliative care team consultation.
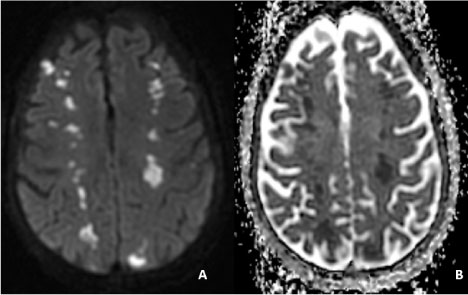 Figure 1: Brain MRI without contrast.
Figure 1: Brain MRI without contrast.
These images demonstrate a hyperintensity in the diffusion weighted image (A) and hypointensity in the apparent diffusion coefficient image (B) in bilateral hemispheres consistent with acute ischemic infarction. These lesions are located in the frontal lobes at the border zones of the MCA-ACA territories and parieto-occipital region at the limits of the MCA-PCA territories. View Figure 1
To the best of our knowledge, this case illustrates the first report of an adult patient diagnosed with ALL in combination with an acute border-zone ischemic stroke and nonbacterial thrombotic endocarditis. It is important to recognize that acute leukemia scan have an effect on cerebral perfusion and may present with hyper-viscosity leading to ischemic cerebrovascular and cardiac events.