Despite recent research focus on the association between Helicobacter pylori (H. pylori) infection and epilepsy there is no consensus about the findings. To obtain a more comprehensive estimate of the association we conducted a meta-analysis to determine the prevalence of H. pylori infection in epilepsy patients and healthy controls. PubMed, EMBASE, Cochrane Library, Web of Science, Google Scholar and CINAHL were searched to identify eligible studies. Four studies were selected for inclusion, involving 418 cases (232 patients with epilepsy and 186 controls). Overall, the prevalence of H. pylori infection in patients with epilepsy was higher than that in control groups. (46.98% vs. 26.34%, OR = 2.58, 95% CI: 1.15-5.82, P = 0.02). Subgroup analysis revealed that the levels of H. pylori infection in epilepsy patients was greater than that in control group by using ELISA (OR = 5.36, 95% CI: 2.62-10.95, P < 0.00001), but it was not statistically significant difference when using 13C urea breath test (OR = 1.36, 95% CI: 0.75-2.46, P = 0.32). Our analysis demonstrated that the association between H. pylori infection and epilepsy is a significant positive correlation. Whether H. pylori infection is a risk factor for epilepsy should thus be addressed in large-scale and prospective studies.
Epilepsy, Helicobacter pylori, Prevalence, Meta-analysis
Helicobacter pylori (H. pylori) is a gram-negative bacterium and mainly associated with chronic gastritis, peptic ulcer disease, gastric cancer and gastric mucosa-associated lymphoid tissue lymphoma [1,2]. Furthermore, some reports have discerned a relationship between H. pylori infection and extra-gastrointestinal diseases such as cirrhosis, pancreatic cancer, coronary heart disease, stroke, migraine, Alzheimer's disease and Multiple sclerosis [3-8]. As these results remain controversial, the interactions between H. pylori and humans are suggested to be extremely sophisticated [9].
Recently, there has been some research interest in the association between H. pylori infection and epilepsy. Several studies evaluating the possible association between H. pylori infection and epilepsy have been published [10-15]. Some studies have reported a significant positive correlation between H. pylori infection and epilepsy [11,12]. However, others have failed to determine any association between H. pylori infection and epilepsy [10,13]. In 2011, Asadi-Pooya et al [14] reported that treating H. pylori infection in patients with refractory epilepsy did not significantly change the seizure frequency. To obtain a more comprehensive estimate of the association we conducted a meta-analysis to determine the prevalence of H. pylori infection in patients with epilepsy and controls.
A systematic search of PubMed, EMBASE, Cochrane Library, Web of Science, Google Scholar and CINAHL was performed to identify potentially relevant publications from the date of database origination through August 2016. They were searched for abstracts using the terms ("Helicobacter pylori" [Mesh] OR "Campylobacter pylori" [Title/Abstract] OR "Campylobacter pyloridis" [Title/Abstract] OR "Campylobacter pyloris" [Title/Abstract] OR "Helicobacter nemestrinae" [Title/Abstract]) AND ("Epilepsy" [Mesh] OR "Epilepsies" [Title/Abstract] OR "Seizure Disorder" [Title/Abstract] OR "Seizure Disorders" [Title/Abstract] OR "Seizures, Epileptic" [Title/Abstract] OR "Epileptic Seizures" [Title/Abstract] OR "Epileptic Seizure" [Title/Abstract] OR "Seizure, Epileptic" [Title/Abstract] OR "Single Seizure" [Title/Abstract] OR "Seizure, Single" [Title/Abstract] OR "Seizures, Single" [Title/Abstract] OR "Single Seizures" [Title/Abstract] OR "Epilepsy, Cryptogenic" [Title/Abstract] OR "Cryptogenic Epilepsies" [Title/Abstract] OR "Cryptogenic Epilepsy" [Title/Abstract] OR "Epilepsies, Cryptogenic" [Title/Abstract] OR "Status epilepticus" [Title/Abstract] OR "Aura" [Title/Abstract] OR "Auras" [Title/Abstract] OR "Awakening Epilepsy" [Title/Abstract] OR "Epilepsy, Awakening" [Title/Abstract]). There was no language restriction. Two investigators independently selected all titles and abstracts identified by the initial search.
The inclusion criteria were as follows: (1) The studies had to be case-control, cross-sectional or case-cohort in design; (2) studies that provided the raw data on H. pylori infection in both the epilepsy group and the control group. Studies were excluded if: (1) The studies had no control groups; (2) The articles were review articles, laboratory studies, or studies of animals. To ensure homogeneity in data the two investigators performed the data extraction independently.
Calculation of dichotomous variables was conducted using the odds ratio (OR) with the 95% confidence interval (CI) as the summary estimates to measure the strength of the association of H. pylori infection and Epilepsy. Heterogeneity was tested using the I2 statistic test, which is a quantitative measure of inconsistency across studies. I2 values of above 25%, 50% and 75% being considered to indicate low, medium, and high heterogeneity, respectively. Heterogeneity was also determined by Q-test, and it was considered indicative of significant heterogeneity when P values were less than 0.1. When the effects were assumed to be homogeneous (I2 < 50%) a fixed-effects model was used; otherwise, the random-effects model was more appropriate [16]. Statistical significance was set at P values of less than 0.05. The meta-analysis was performed using Review Manager 5.3 software.
We identified 54 articles from PubMed, EMBASE, Cochrane Library, Web of Science, Google Scholar and CINAHL. Of these articles most were excluded after reading the titles and abstracts, mainly because they were reviews or were not relevant to the meta-analysis, leaving 11 that appeared to fulfill the inclusion criteria. Following more thorough scrutiny, an additional 7 articles were excluded. Finally, a total of 4 prospective articles including 232 cases of Epilepsy and 186 participants were included in the meta-analysis [10-13]. A detailed flowchart of the selection process is presented in figure 1.
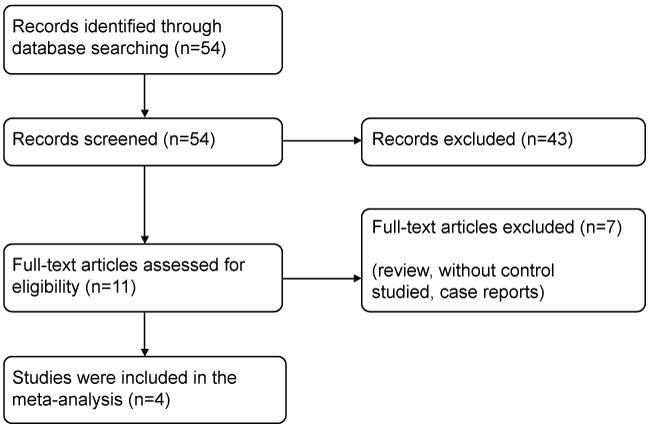 Figure 1: Flow diagram of the study selection process.
View Figure 1
Figure 1: Flow diagram of the study selection process.
View Figure 1
The main characteristics of the 4 included studies are presented in table 1. Four studies involved 232 patients with epilepsy, with a total H. pylori infection rate of 46.98% (109/232). The sample size of the control groups was 186, of which 49 were H. pylori-positive (26.34%). Concerning the H. pylori measure methods, two studies used ELISA, and two studies used the 13C urea breath test (13C-UBT). Okuda, et al. [11] divided the epilepsy subjects into two subgroups: idiopathic generalized epilepsy (IGE) and idiopathic localization-related epilepsy (ILE). Ozturk, et al. [12] separated the Epilepsy patients into poor prognosis and good prognosis groups. Asadi-Pooya, et al. [10] determined the frequency of infection with H. pylori among two groups of patients with epilepsy: patients with idiopathic generalized epilepsy (IGE) and patients with temporal lobe epilepsy (TLE) due to mesial temporal sclerosis. Razak, et al. [13] investigated the association of H. pylori infection with generalised epilepsy and partial epilepsy.
Table 1: Characteristics of the 4 included studies. View Table 1
Overall, the prevalence of H. pylori infection in patients with epilepsy was higher than that in control groups. (46.98% vs. 26.34%, OR = 2.58, 95% CI: 1.15-5.82, P = 0.02) (Figure 2). The heterogeneity was high (P = 0.03, I2 = 68%). We performed a subgroup analysis to further investigate the factors impacting the overall results.
 Figure 2: Overall meta-analysis of the prevalence of H. pylori infection in the epilepsy group compared with the control group.
View Figure 2
Figure 2: Overall meta-analysis of the prevalence of H. pylori infection in the epilepsy group compared with the control group.
View Figure 2
Using stratified analysis based on different methods, the data revealed that the prevalence of H. pylori infection in epilepsy patients was greater than that in control group by using ELISA in two studies (OR = 5.36, 95% CI: 2.62-10.95, P < 0.00001), but it was not statistically significant difference when using 13C urea breath test in other two studies (OR = 1.36, 95% CI: 0.75-2.46, P = 0.32) (Figure 3).
 Figure 3: Subgroup analysis according to different detection methods for the association of H.pylori infection with Epilepsy.
View Figure 3
Figure 3: Subgroup analysis according to different detection methods for the association of H.pylori infection with Epilepsy.
View Figure 3
The association between epilepsy and H. pylori infection is controversial [10-15]. In this meta-analysis we provide an overview of the relationship between H. pylori positiveity and epilepsy with a total of 418 subjects from four eligible studies. Overall the prevalence of H. pylori infection in epilepsy patients (46.98%, 109/232) was higher than in control individuals (26.34%, 49/186) (P = 0.02), indicating that H. pylori infection may be a risk factor for epilepsy.
Epilepsy may be triggered by immunological mechanisms as a result of H. pylori infections. Autoimmunity was recently suggested to be involved in the pathology of epilepsies [17]. Bartolomei, et al. [18] found that detection of anti-GM1 antibodies could allow identification of patients with partial epilepsy associated with an autoimmune response. H. pylori could indirectly influence the brain function due to the release of multiple cytokines such as IL-1,IL-6,TNF-α,which involved in the blood–brain barrier (BBB) disruption and pathogenesis of neuronal inflammatory damage in epilepsy [19,20]. Kountouras, et al. [20] have hypothesized that H. pylori might be a potential therapeutic target in epilepsy.
We conducted a further analysis based on different detection methods, the results showed that the prevalence of H. pylori infection in epilepsy patients was higher than that in control groups by using ELISA [11,12], but it was not statistically significant difference using 13C-UBT [10,13]. The anti-H. pylori IgG-ELISA is a common method for detecting H. pylori seropositivity in clinics. It is well suitable for large-scale population surveys [21]. 13C-UBT is a detection method based on the carbon dioxide and ammonia produced by H. pylori converting urea and has high specificity and sensitivity [21]. 13C-UBT reveals the active (present) infection, whereas the serology can reveal the past infection. However, it may be impossible to directly compare the 13C-UBT results due to the difference in UBT protocols across different clinical centers generated differences in breath sample collection times and intervals, as well as influences on delaying gastric emptying [21,22].
There are some limitations in our study. First, the analysis was conducted on a small number of case-control studies, and the cases included in these studies are also limited and lack of high-quality data. Second, the lack of individual data has limited further subgroup analyses of gender and epilepsy sub-type. Finally, some articles published in non-English languages might be missed.
In summary, the present study showed that the association between epilepsy and H. pylori infection is a significant positive correlation. Whether H. pylori infection is a risk factor for epilepsy should thus be addressed in large-scale and prospective studies.
This study was supported by National Natural Science Foundation of China (Grant No. 81500953), The Program of Jilin Provincial Science & Technology Department (Grant No. 20150520143JH), Jilin Provincial Development and Reform Commission Project (2014N151), and Norman Bethune Program of Jilin University (Grant No. 2015215).