D.T. a 42-year-old male with no significant past medical history underwent circumcision for recurrent Balanitis using the sleeve technique. The procedure was uncomplicated, however a few adhesions with hyper-vascularity were found between the foreskin and the glans. No antibiotic prophylaxis was given intraoperatively. Good haemostasis was achieved with bipolar diathermy.
The patient was due to be discharged the same day but remained in hospital overnight due to a single vasovagal event. He was discharged day 1 postoperatively with no routine urology follow up, as per guidelines.
Day 2 postoperatively, the patient noticed penile swelling for which he visited GP and was prescribed oral antibiotics. He continued to have increasing pain over the next 2 days, and day 4 postoperatively he was referred back to Hospital under the care of Urology. On review in A&E he had signs of a superficial skin infection [cellulitis] likely secondary to a penile haematoma, and he was admitted for treatment with IV antibiotics. Bloods cultures taken previously were negative for significant growth.
Day 5 postoperatively, during ward-round, the patient was noted to have a necrotic patch on the penile/scrotal area and he was taken for urgent debridement where surgical findings were a 5-7 cm gangrenous patch on right hemiscrotum. There was subcutaneous involvement of the scrotum and also the left side of penile shaft with a small pocket of pus distally, near the glans. Wide debridement of the scrotal and penile skin needed to be performed (Figure 1). A diagnosis Fournier's gangrene was confirmed with tissue histopathology.
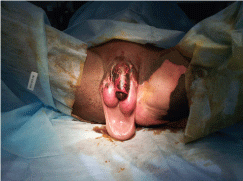 Figure 1: Example of primary debridement for Fournier Gangrene.
View Figure 1
Figure 1: Example of primary debridement for Fournier Gangrene.
View Figure 1
The patient then underwent a second debridement the day after, requiring debridement of 2/3rd of the penile shaft and anterior scrotal sac. The patient was admitted for HDU care following this, and blood cultures taken on admission came back positive for Group A Streptococci.
A third debridement was needed for a small necrotic region at the base of the scrotum day 8 post initial operation and the patient was referred to University College London Hospital, under the care of the reconstructive Urology team. Prior to graft surgery reconstruction to the penis and scrotum at day 15, a fourth debridement was needed after day 11 post the initial procedure. The patient was eventually discharged 20 days post initial procedure (Figure 2).
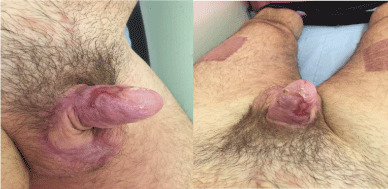 Figure 2: Surgical site 5 months post discharge at clinic follow up.
View Figure 2
Figure 2: Surgical site 5 months post discharge at clinic follow up.
View Figure 2
Necrotising Fasciitis [Fournier Gangrene] forms part of a group of soft tissue destructive infections that are characterised by local and systemic manifestations and which require urgent surgical intervention with debridement of the affected area and surrounding tissue. There are two classifications of Fournier's [1]:
Type I infections- Polymicrobial infections, typically comprising both anaerobic and aerobic pathogens.
Type II infection- Group A [haemolytic] Streptococcal gangrene.
The typical histological appearance of Fournier's is necrosis of the epidermis and underlying dermis with visualisation of polymorphs and micro-abscesses.
There is a known association with Necrotising Fasciitis and recent surgery, although the literature on this infection following circumcision is very limited. Case reports reviewed in the literature report cases of Fournier's being associated with diabetes, obesity, intravenous drug use, traumatic wound [2]. Fournier's was also found following mass voluntary medical male circumcision in Uganda [3]. There has been some postulation regarding NSAIDs having a role in the clinical progression of Fournier's, this is however founded in anecdotal reports and not supported by evidence-based review [4]. Neither the aforementioned associated risk factors, or NSAID use were present in this patient.
There are a number of discussion points arising from this case: The patient was low surgical risk and he had no associated risk factors for Fournier's Gangrene, although surgery is a risk factor for any infection. Could here have been an aetiological factor that was not identified in this patient [2]? Standard surgical practice was applied to this case, and there was no concern at the time of surgery for contraction of a post-surgical infection. Should the presence of foreskin adhesions and hyper-vascularity requiring diathermy control have been considered an indication for high infection risk? And if so, should the patient have been given intravenous antibiotics, despite this not being trust protocol at the time [5].
As for all patients undergoing this procedure, consent is gained for all possible complication, including bleeding, swelling, pain, infection and possible dissatisfaction with the cosmetic outcome [6]. In this case the primary presenting complaint was of pain during intercourse secondary to balanitis, however the final outcome in this case of Fournier's Gangrene, was not factored into the pre-surgical discussion. The GMC references the case of Chester vs. Afshar [2004] as a precedent for consenting patients for all possible complications of surgery. Cases such as Chester vs. Afshar demonstrate that the paternal principle of care no longer prevails, nor does the Bolam defence [7]. Given the rarity of this complication, should it become routine for the risk of Fournier's to be discussed during consenting for this procedure?
This case highlights a very uncommon, yet serious and life-threatening complication post circumcision. The patient, deemed low risk for any intra or post-operative surgical complications, had no associated risk factors for developing Fournier's Gangrene [2]. Were there unidentified risk factors that could have led to the eventual outcome? Did the need for diathermy to control bleeding of the foreskin adhesions contribute to developing the infection, and therefore should antibiotic prophylaxis have been given? Guidelines did not indicate the uses of antibiotics in such circumstances. The important question therefore is should this case change our practice; Should all patients undergoing circumcisions be given prophylactic antibiotics, and prior to surgery should we be consenting for such complications?
No funding was required.
No conflict of interest was seen.
Not required as not part of any research.
Informed consent was obtained from all individual participant included in the study.