To review the long-term outcomes after a vaginal native tissue repair, High Midline Levator Myorrhaphy (HMLM), for symptomatic vault prolapse.
Following IRB-approval, a prospectively maintained database of women who underwent HMLM for symptomatic vault prolapse (VP) alone or associated with other POP was reviewed for demographic data, history of prior POP, physical examination, hospital stay length, and long-term outcomes. Patients with < 6 months follow up and no retrievable operative notes were excluded. Data was reviewed by a third-party investigator. Failure was defined as same compartment POP ≥ stage 2 or POP reoperation. Descriptive statistics and Kaplan-Meier curves were obtained.
Between 1996 and 2014, 94 women met all criteria. Mean follow-up time was 7.7 (0.6 - 18.4) years, mean age was 69.6 (36 - 91), and 89% were Caucasian. Patients were grouped by POP indications: VP (6), vault and anterior (26), vault and posterior (35), and all 3 compartments (27). No intra-operative complications were reported. Ten (11%) early complications (< 30 days) were noted (Clavien I/II). Sixty-seven (71%) women were cured of VP. Ten (11%) had failure in a non-apical compartment and 17 (18%) had apical failure. Reoperation rate was 14% (13/94) and 5% (5/94) for vault and non-vault recurrences, respectively. VP recurrence-free probability between women with ≤ 2 versus 3 POP compartments was statistically significant (p = 0.0128).
At a mean follow-up of 7-8 years, HMLM was successful in two thirds of women. Best outcome was noted in women with VP and one associated compartment prolapse.
Pelvic organ prolapses (POP) is widely prevalent and leads to more than 300,000 surgeries in the United States costing more than $1 billion annually [1]. Vaginal vault prolapses (VP), prolapse of the vaginal apex, can be a result of cardinal and utero-sacral ligaments laxity and/or damage [2]. The risk of VP increases with advancing age and number of vaginal deliveries [3]. VP has a prevalence of 0.2% to 43% in various studies, with a recurrent prolapse rate of 5 to 34% and reoperation rate of 5-26% depending on repair technique [4-6]. Vaginal techniques have faster recovery rates and lower morbidity than abdominal procedures, especially for women > 65 years [7]. Techniques involving transvaginal mesh are under scrutiny after the recent 2008 and 2011 FDA notifications with concerns for post-operative mesh erosion, pelvic pain, and/or dyspareunia [8,9].
Recent literature on native tissue repair for vault prolapse include an OPTIMAL randomized trial by Barber, et al. that compared utero-sacral ligament vault suspension (ULS) and sacrospinous ligament fixation (SSLF). ULS suspends the vaginal apex to the utero-sacral ligaments intraperitoneally, and SSLF to the sacrospinous ligament extraperitoneally. At 2 years follow up, the study found no statistically significant difference in surgical success between the two procedures. Surgical failure rate was 36% for ULS and 37% for SSLF, with surgical repair for POP recurrence at 3.1% and 2.6%, respectively [10].
High midline levator myorrhaphy (HMLM), first described in 1988, is a vaginal surgery for VP that does not rely on mesh interposition, avoids the inherent difficulties associated with sacrospinous fixation involving nearby vascular and neural structures, and is well-suited for middle-aged to older women [11]. Unlike SSLF, HMLM keeps the vagina midline, and unlike ULS, HMLM can be done many years after hysterectomy when the utero-sacral ligaments are no longer readily identifiable. Since its original report, there has been few published series on surgical outcomes, none of which included long-term data. Therefore, the objective of this retrospective study from a prospectively maintained, IRB-approved, database was to review HMLM long-term outcomes in women with symptomatic VP at a tertiary care center.
An institutional review board approved, prolapse database of women who underwent HMLM for symptomatic stages II/III VP alone or associated with other POP was reviewed for: Demographic data, history of prior POP, physical examination findings, one global quality of life index (QoL) ranging from 0 (pleased) to 10 (terrible), operative notes, peri-operative complications (Clavien), length of hospital stay, and long-term outcomes based on last office visit information (examination, questionnaire). Of note, baseline and follow-up examinations were performed by a variety of clinicians over time including faculty, fellows and trained physician assistants. For examination, the Baden-Walker half-way scoring system [12] was used at baseline because the study was started before the POP-Q [13] classification system was implemented in our database at our institution. However, all examination findings at the last visit used the POP-Q classification system. Early complications (< 30 days) were classified according to the Clavien-Dindo classification of surgical complications [14]. Patients with less than 6 months follow-up and no retrievable operative notes to confirm that an HMLM was performed were excluded. Data was acquired through an electronic medical record system (EPIC) by a reviewer (YW) not related to patient care. Women with no secondary POP in any compartment after HMLM procedure were defined as cured. This strict success definition was chosen because rather than being an isolated process, VP is commonly associated with one or more other compartment prolapses. Failure was defined as any compartment prolapse ≥ stage 2 on physical examination, or reoperation for POP.
All surgeries were performed by one surgeon (PZ) at a single institution. The surgical technique has been described previously in detail [11]. A rectal pack, soaked with Betadine™, is inserted to allow recognition of the rectum throughout the procedure. Then, with the patient in Trendelenburg position, a Scott retractor to expose the vagina and a urethral catheter to drain the bladder are placed. Two sutures are placed at each vaginal vault fornix to confirm location of the vaginal apex for later repositioning (Figure 1A). The dimensions of the vagina are measured. A midline incision is made overlying the bulging prolapse, extending anteriorly and/or posteriorly as far distally as needed based on associated compartment prolapses when present. Vaginal flaps are raised on each side of the original incision. After opening the enterocele sac, a pack is placed to reduce the bowels. The pack in the rectum can now be palpated, as well as the medial edge of the levator muscle bordering the rectum on each side. A No. 1 absorbable suture is then placed into the levator musculature on the right side, then passed over the rectum and secured to the medial edge of the levator muscle on the other side. The suture is left on a stay clamp. A second suture is then placed in a similar fashion 1 cm proximal to the last suture. After this is done, the closure of the enterocele sac is accomplished. A No. 1 polypropylene purse-string suture is placed circumferentially to close the peritoneal cavity. After the peritoneal packs are removed and the purse-string suture cinched down, indigo carmine (or fluorescein nowadays) is administered intravenously and cystoscopy is done to confirm ureteral jets bilaterally. The 2 preplaced levator sutures are then tied sequentially across the midline. These 2 levator sutures (proximal and distal) are then tagged with a hemostat. The ends of each suture are threaded on a No. 6 curved Mayo needle and then transfixed at the new restored site of the vaginal apex from inside out approximately 1 cm apart from each other (Figure 1B). The proximal and distal end of each levator sutures are then tied to each other bringing the vaginal vault down over the rebuilt levator plate just underneath with direct tissue apposition (Figure 1C and Figure 1D). If an anterior repair or anti-incontinence procedure is required, it can now be carried out, followed by a rectocele repair with perineorrhaphy, if indicated. Figure 2A, Figure 2B, Figure 2C and Figure 2D illustrate the tying and tagging of the levator muscles after enterocele closure as well as the final anatomical position of the vagina over the rebuilt levator shelf. While HMLM started out as an intra-peritoneal procedure, it can also be performed as an extra-peritoneal procedure, thus decreasing the potential for ureteral injury.
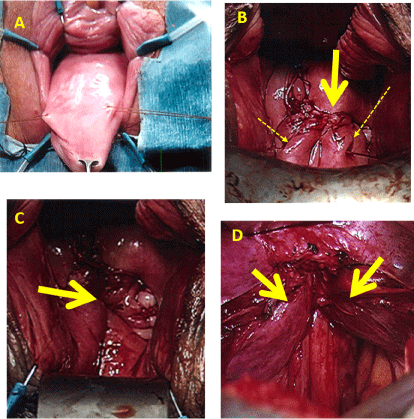 Figure 1: Intraoperative views: (A) Vault prolapse with sutures marking site of vaginal apex; (B) HMLM suspension sutures have been tied already and the vaginal cuff has been closed (large arrow). The end of the HMLM suspension sutures have been transfixed from inside out at each side of the apex (dashed arrows); (C) Final appearance of the vaginal vault anchored back over the rebuilt levator plate underneath; (D) Midline approximation of levator muscle edges as seen by lapararoscopy on same patient at end of HMLM procedure. View Figure 1
Figure 1: Intraoperative views: (A) Vault prolapse with sutures marking site of vaginal apex; (B) HMLM suspension sutures have been tied already and the vaginal cuff has been closed (large arrow). The end of the HMLM suspension sutures have been transfixed from inside out at each side of the apex (dashed arrows); (C) Final appearance of the vaginal vault anchored back over the rebuilt levator plate underneath; (D) Midline approximation of levator muscle edges as seen by lapararoscopy on same patient at end of HMLM procedure. View Figure 1
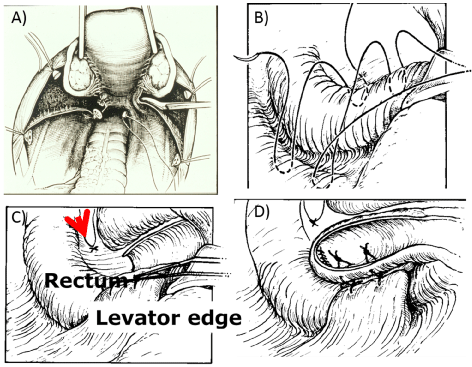 Figure 2: Schematic of (A) Abdominal view of the utero-sacral ligaments pre-hysterectomy; (B) Levator sutures tied across the midline and tagged; (C) Sagittal view of upper vagina and closed enterocele sac; (D) Levator sutures transfixed at apex to reposition upper vagina over the recreated levator plate at the conclusion of the procedure [11]. View Figure 2
Figure 2: Schematic of (A) Abdominal view of the utero-sacral ligaments pre-hysterectomy; (B) Levator sutures tied across the midline and tagged; (C) Sagittal view of upper vagina and closed enterocele sac; (D) Levator sutures transfixed at apex to reposition upper vagina over the recreated levator plate at the conclusion of the procedure [11]. View Figure 2
Patients were divided into four indication groups for analysis: (1) Only vault prolapse, (2) Vault and anterior compartment (cystocele) prolapse, (3) Vault and posterior compartment (enterocele and rectocele) prolapse, and (4) Prolapse of all three compartments. It was hypothesized that women with multiple compartment POP, older age, multiparity, and/or post-hysterectomy would fare worse.
Descriptive statistics were calculated using means and standard deviations for continuous measures, and frequencies and percentages for categorical measures. ANOVA and unpaired Student t-tests were used to test for differences in continuous measures, and Fisher's Exact test in categorical measures. A Kaplan-Meier curve was used to test for differences in survival distributions of HMLM by indication group. All analyses were performed using SAS 9.4 (SAS Institute Inc., Cary, NC). All tests were performed at the p = 0.05 significance level.
Between May 1996 and September 2014, 94 of 109 women who underwent HMLM met inclusion criteria (< 6 months follow up (6), operative notes not retrievable (9)) (See study flow chart on Figure 3). Baseline demographic characteristics are summarized in Table 1. Based on Baden-Walker, all symptomatic patients who underwent HMLM had vault descent stages II or III. Mean follow-up time was 7.7 years (standard deviation 4.6 and range 0.6 to 18.4).
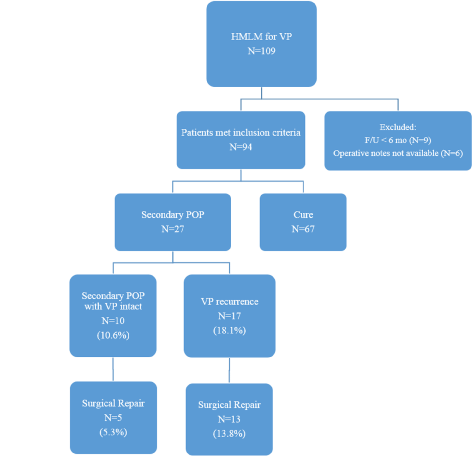 Figure 3: Study population flow chart. View Figure 3
Figure 3: Study population flow chart. View Figure 3
Table 1: Baseline patient characteristics by indication categories. View Table 1
Ninety-four percent had at least one other concurrent vaginal prolapse repair. Six patients had vault only (V), 26 vaults and anterior (V + A), 35 vault and posterior (V + P), and 27 all three compartments (V + A + P). Ninety-two women had intraperitoneal HMLM and 2 extraperitoneal HMLM. Neither women in the extraperitoneal group had intraoperative, perioperative complications, or POP recurrence in any compartment.
A total of 24.5% (14 V + A, 2 V + P, and 7 V + A + P) had concurrent hysterectomy for associated uterine descent. No intraoperative complications were reported. Ten (10.6%) Clavien I/II early complications (< 30 days) were noted: Urinary retention/prolonged catheter (4), urinary tract infection (2), incontinence (2), bladder spasms (1), bleeding without transfusion (1). These 10 early complications were divided among the 4 surgical groups with 2 in each, except 4 in the V + A + P group (p = 0.5278).
Preoperatively the V + P, V + A, and V + A + P indication groups had no statistical differences in demographic data for age, race, BMI, number of follow up years, smoking status, number of vaginal deliveries, presence of systemic HRT, or reported vaginal sensation of bulge/pressure. Variables that were statistically different (confidence level of 95%) between at least two groups include: Prior hysterectomy (p = 0.0050), concurrent hysterectomy (p = 0.0001), and prior POP surgery (p = 0.0280). Difference in length of hospital stay was significant (p = 0.0220). Baseline patient characteristics by indication categories are summarized in Table 2. Due to limited sample size in the vault only indication group, analyses of overall differences were carried out only for the three other categories. No baseline patient characteristics were statistically different between patients who were cured of POP and those with secondary vault failure (data not shown).
Table 2: Secondary POP repair by indication group. View Table 2
Overall 67/94 (71.3%) women were cured of VP. Ten women (11%) had failure in a compartment other than the apex and 17/94 patients (18%) had failure at the apex. All 10 of the non-apex failures were recurrent cystoceles. Time to diagnosis of POP recurrence, time to reoperation, and type of reoperation are reported in Table 3. Reoperation rate was 13.8% (13/94) and 5.3% (5/94) for vault and non-vault recurrences, respectively. Apical recurrence with surgical repair was borderline significant between indication groups (p = 0.0494).
Table 3: Post-HMLM POPQ points and QoL scores by indication group. View Table 3
No statistical difference was found in length of hospital stay, perioperative, and early complications between patients with and without POP recurrence. The probability of recurrence-free patients over time for each indication group revealed no statistical difference (p = 0.0849) (data not shown). When the recurrence-free probability between patients with two or less compartments POP and three compartment POP were compared, a statistically significant difference was observed (p = 0.0128, Figure 4). Post-operative POPQ points and QoL score by indication group are summarized in Table 3. Aa, Ba, TVL and QoL score were not statistically different between indication groups. Post-HMLM POPQ points that differed significantly between indication groups included Ap (p = 0.0483), Bp (p = 0.0063), and C (p = 0.0382).
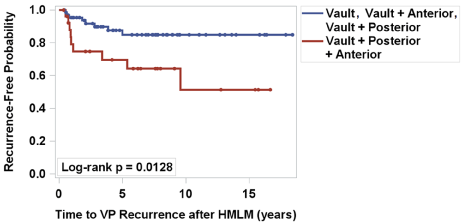 Figure 4: Kaplan-Meier curve for VP recurrence-free status after HMLM procedure by indication groups. View Figure 4
Figure 4: Kaplan-Meier curve for VP recurrence-free status after HMLM procedure by indication groups. View Figure 4
We reviewed the long-term outcomes for patients that received HMLM for vault prolapse between 1996 and 2014. With a mean follow up of 7.7 years, we found an overall recurrence rate of 28%. Non-vault recurrence rate was 11% and vault recurrence rate was 17%. Of the women who had vault failure, 33.3% were in the V +A + P indication group where all three compartments required repair. Twenty-six percent of women who had vault failure and underwent corrective surgery were in the V + A + P group, 15.4% V + A, and 2.9% V + P (p = 0.494). Smoking status, parity, hysterectomy status, presence of systemic HRT, vaginal bulge sensation/pressure, and prior POP surgery were not statistically different between women with or without recurrence. Based on these findings, it seems HMLM is not the best choice for complicated prolapse cases involving all three compartments, especially those that have complete eversion of the vagina. For patients that had vault-only prolapse or vault and one other compartment prolapse, HMLM had an 88% success rate.
Overall the operation was well tolerated, and the majority of patients had minimal peri-operative events. HMLM overall surgical success rate was on par with other VP repair procedures that have long-term outcomes data, such as sacrospinous ligament fixation, uterosacral ligament vaginal vault suspension, and McCall Culdoplasty. Moreover, the low rate of serious perioperative complications was consistent with other vaginal native tissue repairs [15]. One other long-term outcome study on a variant of HMLM was done by Natale, et al. in 2008, with a mean follow-up time at 5 years [16]. These authors found 3.3% vault recurrence and 26.8% cystocele recurrence. Although our 17% vault recurrence rate is higher, our follow-up time is also significantly longer, with over 60% of our patients followed past 5 years. Our cystocele recurrence rate at 18% is consistent with Natale group's findings. Sexual function was evaluated in prior studies [11,16] but the data was not tallied in this series due its sparsity. Few women were sexually active at baseline with their symptomatic POP; and, based on self-reporting, a few were active post-operatively (population mean age nearing 70-years-old).
This study's strengths include: Long-term follow-up in the majority of patients operated with HMLM, patients' relative homogeneity of age and associated conditions, and continuity of surgical technique by one surgeon at a single institution, thus reducing clinical practice variability. Limitations include the change in clinical outcome assessment from Baden-Walker at baseline to POP-Q at last visit, the Caucasian ethnicity predominance, and the limited number of patients in the VP only indication group.
Based on our results, HMLM is an acceptable option for women with VP and one other compartment prolapse wishing a native tissue repair. Those with complete vaginal eversion who require surgical repair of the anterior, posterior and apical compartments might achieve better long-term outcomes with an alternative procedure.