55-year-old para 2 woman was brought to the emergency department following insertion of a tension-free vaginal tape complaining of lower abdominal pain and vertigo. The subsequent angiography localized a significant bleeding from the right obturator artery and a retropubic hematoma 17.5 cm × 10.0 cm in size. The patient was successfully treated by arterial embolization; however, the postoperative course was greatly protracted due to persistent subfebrilia and eventually the hematoma was removed by laparoscopy. This case illustrates that embolization should be considered an important alternative for management of arterial bleeding following synthetic midurethral slings. However, removal by laparoscopy or laparotomy may be necessary in large hematomas subsequently to embolization.
Arterial bleeding, Tension-Free vaginal tape, Retropubic hemorrhage, Embolization
The Tension-Free Vaginal Tape (TVT) was introduced in 1996 and is now widely used in surgical treatment of urinary incontinence due its low risk of surgical complications and high long-term cure rate [1]. Surgical complications may however occur as the blind passage of a sharp instrument through the retropubic space carries the risk of visceral or vascular injury [1,2]. The Transobturator Tapes (TVT-O, TOT) were introduced later to minimize the risk of TVT. However, vascular and nerve injuries due to these procedures have also been reported [1].
Venous injuries resulting in a vulval-vaginal or retropubic hematoma are not uncommon [1,3]. An arterial injury is rare but potentially life-threatening due to the risk of blood loss and hemodynamic instability. Commonly, it has been managed through an open abdominal incision [1,3]. In the last decade; embolization has gained favor for the treatment of acute hemorrhage in different anatomical areas within several surgical specialisms for the treatment of acute hemorrhage [4]. Case reports have shown favorable outcomes of arterial embolization following insertion of a synthetic Midurethral Sling (MUS) complicated by arterial hemorrhage [5-13].
This case report describes an injury to the right obturator artery following a TVT procedure complicated by arterial hemorrhage successfully treated by embolization, but with a protracted postoperative course. The present case is discussed with reference to a brief systematic review of the literature.
Seven hours after undergoing an uneventful TVT insertion under local anesthesia a 55-year-old non-obese para 2 woman was brought to the emergency department complaining of lower abdominal pain and vertigo. On physical examination, she was alert and aware, but pale, peripherally cold and hypotensive (blood pressure was 80/30 and pulse = 55/minute). Apart from medical treatment for hypertension, she was healthy. Prior surgical history included an appendectomy only. On suspicion of intraperitoneal bleeding, laparoscopic evaluation was performed showing a large hematoma retropubically and on the posterior abdominal wall and after conferral with a vascular surgeon, the decision was made to perform arterial embolization. The subsequent angiography localized significant bleeding from the right obturator artery; an anterior branch of the internal iliac vessel (Figure 1) and a retropubic hematoma 17.5 cm × 10.0 cm in size (Figure 2). The patient was treated by selective embolization with coils of the right obturator artery (Figure 3) and her vital signs remained stable after the procedure. Five days postoperatively, the patients presented with fever of 38.9 ºC and diffuse lower abdominal pain. She received intravenous broad-spectrum antibiotics, the pain abated and an enhanced Computed Tomography (CT) scan revealed a reduced hematoma sized 11 cm × 6 cm. To prevent formation of an abscess and due to ongoing fever (temperature up to 38.9 ºC) laparoscopic evacuation of the hematoma was performed with a total blood loss of 1000 ml on postoperative day 10. Because the upper part of the tape had loosened from the tissue and was visible intraperitoneally, this part had to be removed.
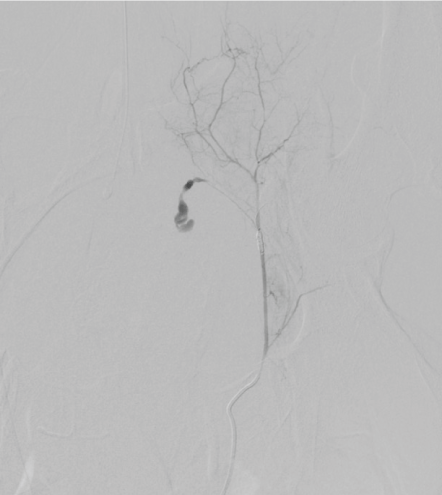 Figure 1: Pelvic arteriography before embolization of the right obturator artery. View Figure 1
Figure 1: Pelvic arteriography before embolization of the right obturator artery. View Figure 1
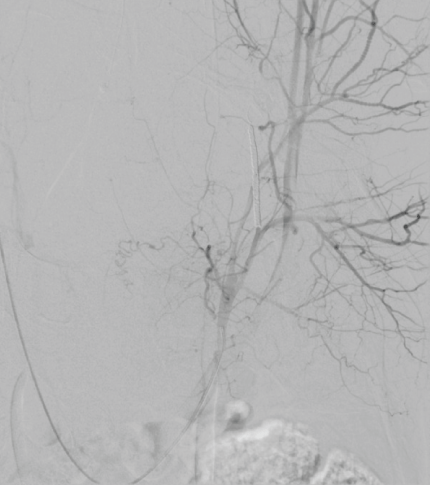 Figure 2: Enhanced computed tomography shows a major retropubic hematoma (17.5 cm × 10 cm) following tension-free vaginal tape. View Figure 2
Figure 2: Enhanced computed tomography shows a major retropubic hematoma (17.5 cm × 10 cm) following tension-free vaginal tape. View Figure 2
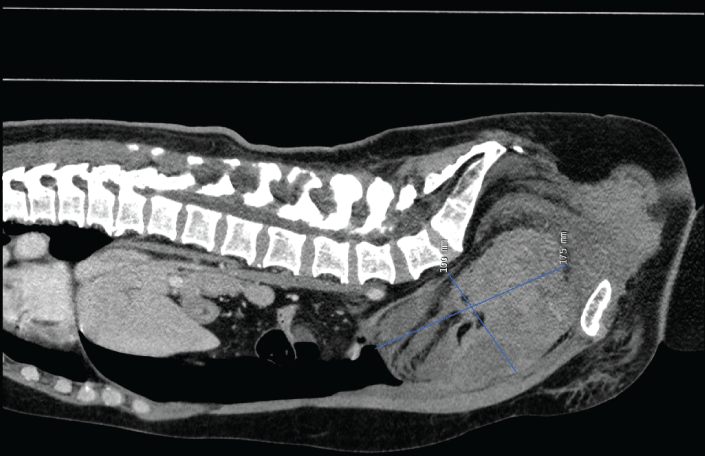 Figure 3: Pelvic arteriography after embolization of the right obturator artery. View Figure 3
Figure 3: Pelvic arteriography after embolization of the right obturator artery. View Figure 3
The patient was in fair general health postoperatively, but due to low-grade fever, she received intravenous antibiotics for nine days in total. On postoperative day 14, the patient was discharged on oral antibiotics. Due to persistent low-grade fever on postoperative day 21, an enhanced CT scan was performed excluding injury to the urinary tract, however showing a 1.4 cm × 6 cm pelvic mass representing either a small abscess or a residual hematoma. No further treatment was initiated. Two months postoperatively, the patient was well-being and reported no stress urinary incontinence.
To decrease the risk of vascular injury it is imperative that the surgeon employs the correct technique [6,14] and ensures there no bleeding occurs from the vaginal incisions perioperatively [1]. However, since it is not uncommon for the pelvic arteries to follow an aberrant course [14], hemorrhage is not always possible to prevent. Rarely, hemorrhage results from an occult bleeding diathesis [6]. In the present case, while there was no explanation for the hemorrhage, as it was unlikely to have been due to surgical technique, the passage of the trocars through the retropubic space was inevitably a blind procedure [1] and vessel damage was hence more likely to have been a chance adverse event.
The incidence of retropubic hematomas following MUS sling procedure using TVT has been reported as 2 - 4% and the consequent need for surgical intervention as 0.3 - 1.2% [2].
The majority of retropubic hematomas is due to venous bleeding and can often be managed expectantly [1]. Arterial bleeding, however, is a rare event and even though immediate and adequate treatment is imperative, no standard for its management has been established. Commonly, it has been managed through an open abdominal incision [1,3].
To date, eleven cases have described arterial bleeding following synthetic MUS managed by arterial embolization [5-13] (Table 1). The present case, in agreement with the other studies, illustrates the usefulness of angiography to locate the bleeding and to obtain hemostasis in arterial injuries following synthetic MUSs [5-13]. Unlike previous cases, the present postoperative course was greatly protracted due to persistent infection, multiple assessments and ultimately, removal of the hematoma. There are several further possible explanations for the protracted course: Firstly, unlike in the majority of reported cases, the patient underwent laparoscopy prior to angiography [5,7-12] which may have increased the risk of infection. Secondly, an obvious disadvantage of leaving the hematoma in situ is that the stagnant blood provides an ideal environment for bacterial infection to develop [1]. The risk in the present case might conceivably have been reduced had the patient been given prophylactic antibiotics, as recommended in some earlier case reports [1,3].
Table 1: Literature on arterial injury following synthetic midurethral slings and embolization. View Table 1
Thirdly, the size of the hematoma might also be a limiting factor, as this is the largest hematoma (10 cm × 17.5 cm) reported following a synthetic MUS, for which management has been attempted by embolization without subsequent removal [6-8,12,13]. In the literature, hematomas up to 13 - 16 cm following synthetic MUSs have been managed with embolization without the need for subsequent removal [6,7]. Normally, small hematomas (< 5 cm) do not require any surgical intervention [1], but hematomas up to 10 cm have in stable patients been managed expectantly [3], which suggests that the maximum size for embolization also lies within this range.
The present case report, in agreement with existing literature, illustrates that embolization should be considered an important alternative treatment for management of arterial bleeding following synthetic MUSs; as the minimal approach of the TVT is preserved while managing a potentially life-threatening condition. However, the size of the hematoma might be a limiting factor for leaving it in situ, which necessitates removal by laparoscopy or laparotomy subsequently to embolization.
Lack of access to intervention radiology and awareness of the treatment among uro-gynecologists may reduce this surgical practice.
No potential conflict of interest relevant to this article was reported.
None.
Written informed content was obtained from the patient for publication of this case and any accompanying images.