Double J stent is a routine procedure in urology. Today, it is used for a wide range of indications. Their use is not without consequences. Complications may be frequent or rare, minor or serious. Perforation of the renal parenchyma, with or without the formation of a hematoma, is a serious complication that is considered very rare. In this report, we report the case of a 70-year-old patient who underwent bilateral double-J ureteral stent for obstructive renal failure due to prostate cancer. He presented to our center 20 days later with low back pain, diuresis failure and renal insufficiency on the laboratory work-up. Further work-up, mainly imaging (ultrasound and CT scan), revealed a lateral perforation of the renal parenchyma, complicated on the left by the formation of a hematoma. Management consisted in changing the double J probes. The outcome was favorable, with improvement in clinical signs and biological parameters. This routine procedure can be unexpectedly complicated by exceptional situations. On the basis of this case and existing literature, the various aspects will be analyzed and discussed.
Double J ureteral stent, Complication, Parenchymal perforation, Hematoma, Renal
The double J ureteral stent is commonly used in endo-urological practices. However, certain complications may arise [1]. The most frequently reported are urinary tract infections, hematuria, irritative signs and flank pain secondary to vesicoureteral reflux [2]. Serious complications such as renal-colic fistula or vascular migration have been reported [3,4]. Another serious complication is parenchymal perforation, which has been reported sporadically. This is a rare complication, first described by Dündar, et al. in 2008 [1]. In 2015, Altay, et al. [2] reported the 4 th case in the literature. In all the previous cases reported, the perforation involved a kidney. One case of parenchymal perforation in a single kidney has already been reported [5]. In the present article, we report an original case of bilateral renal parenchymal perforation with unilateral hematoma formation induced by placement of a double J ureteral stent in a patient undergoing prostate cancer treatment.
Mr. A, aged 70, had been treated for prostate cancer (undergoing hormone therapy) at another center, and had been fitted with bilateral double-J ureteral stents for bilateral low back pain associated with obstructive renal failure. He presented to our center 20 days later with bilateral low back pain and diuresis failure. Biological work-up showed an increase in creatinine (52 versus 29 mg/ml at the last work-up reported by the patient). Clinically, he was stable and had lumbar tenderness to palpation. Biologically, the rest of the work-up was correct, apart from elevated plasma creatinine. Emergency ultrasound (Figure 1) revealed bilateral dilatation of the renal cavities, with the proximal tips of the JJ probes located in the renal parenchyma. The right kidney showed a hematoma.
 Figure 1: Ultrasound images showing dilatation of the renal cavities with the proximal ends of the JJ probes in the renal parenchyma and a haematoma.
View Figure 1
Figure 1: Ultrasound images showing dilatation of the renal cavities with the proximal ends of the JJ probes in the renal parenchyma and a haematoma.
View Figure 1
Additional scans (Figure 2) showed that both JJ probes were extra-renal, crossing the renal parenchyma and forming a subcapsular haematoma on the upper pole of the right kidney, measuring 45 × 40 mm.
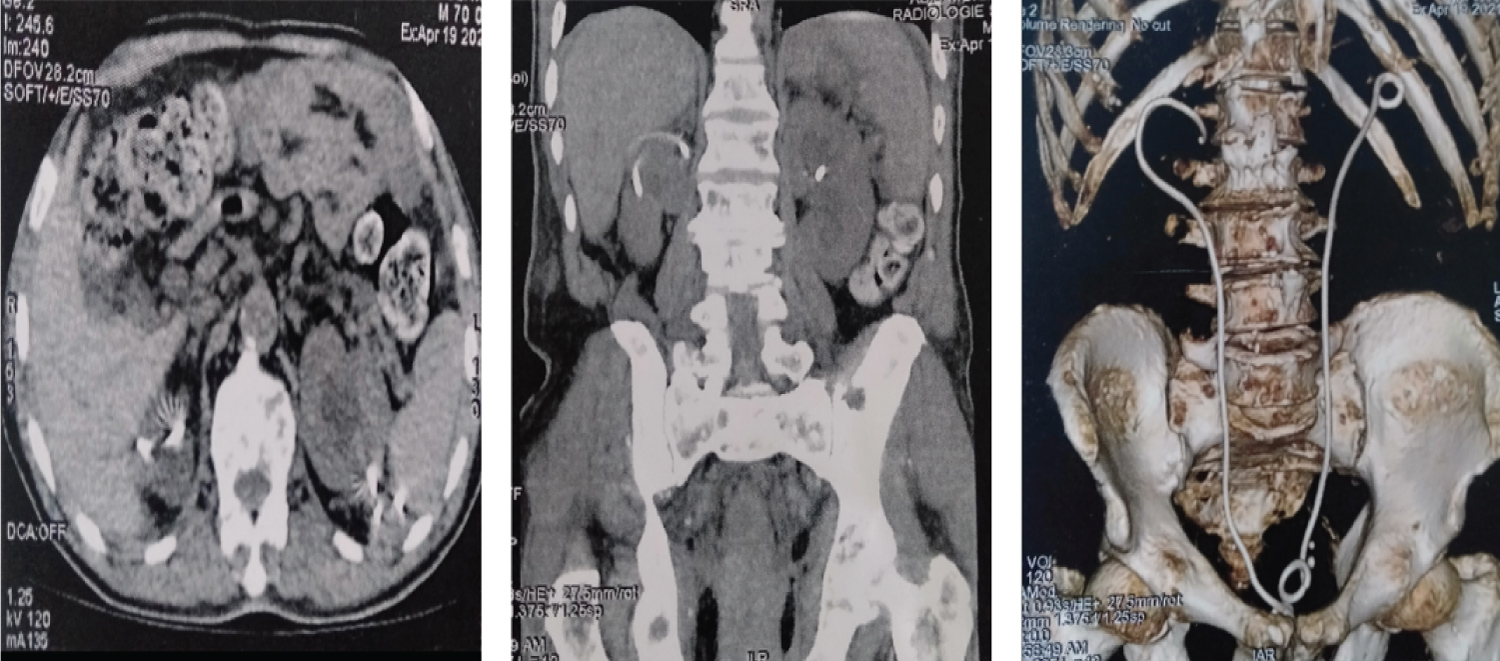 Figure 2: Scans showing two JJ probes are extra-renal, perforating the renal parenchyma bilaterally, with haematoma of the upper right pole.
View Figure 2
Figure 2: Scans showing two JJ probes are extra-renal, perforating the renal parenchyma bilaterally, with haematoma of the upper right pole.
View Figure 2
After conditioning, the patient was taken to the OR, where JJ ureteral probes were changed without incident. Removal of the old stents was easy. At the end of the procedure, a bladder stent was placed. Urine was not hematic. He was discharged from hospital on D3 post-op, after improvement in his clinical and biological condition, and sent home with a letter to his former center.
The insertion of double-J ureteral stents is a common urological procedure. The indications are manifold, and may or may not be performed in an emergency [6]. Their first use dates back to 1967, described by Zimskind [7]. Since then, their use has become increasingly widespread, in line with the growing number of complications associated with them [1]. Among the multitude of complications, Liao, et al. [8] considered perforation of the renal parenchyma caused by double-J stent insertion to be a very rare occurrence. Apart from Gönülalan, et al. [5], who reported the occurrence of this complication in a patient with a single kidney, all previous studies have reported cases of unilateral involvement. To our knowledge, our case is the first with bilateral involvement.
Some authors [6,8] have put forward hypotheses concerning the mechanism of occurrence. Their hypothesis consists in explaining the occurrence of this complication by injury to the renal parenchyma caused by the guide wire. Risk factors have been identified, such as the risk of infection and the fact that the procedure is performed without a fluoroscope. This complication occurred even in cases where the fluoroscope was used [2,6]. In addition to the risk factors identified, we report the occurrence of a case in a patient with pelvic cancer.
This perforation of the renal parenchyma may or may not be accompanied by the formation of a hematoma [9]. Hematoma formation is secondary to vessel bleeding after parenchymal injury. The most plausible explanation for the development of a hematoma is vessel bleeding after parenchymal injury, which collects subcapsularly and forms the hematoma [6] (Table 1).
Table 1: Below presents the main features of the studies cited [2,5,6,8,9], together with their epidemiological, clinical and therapeutic data. View Table 1
Based on the data in this table, the sex ratio is in favor of women (3/2), and age varies, with an average of 60.5 years. Indications for JJ placement vary, and are mainly dominated by lithiasis. In our case, the patient was suffering from prostate cancer. The symptomatology is atypical: Irritative signs, lumbar pain of variable intensity, vomiting, hematuria. Liao, et al. [8] have reported signs of hemodynamic instability (hypoxia and hypotension). This complication may be discovered in the immediate postoperative period, or after a few weeks, as in the case of this report. Diagnosis is based on imaging: ultrasound, X-ray and CT scan. The CT scan is the confirmatory investigation.
Justifications for early percutaneous drainage could include cases where patients suffer unbearable pain, present infectious complications related to the hematoma itself, as well as situations involving renal compression and ischemia, particularly when the hematoma is sub capsular and exerts pressure on the kidney. In the event of uncontrolled bleeding or rapid evolution of the hematoma, conventional drainage by open surgery may be opted for [10]. Therapeutic approaches vary in the literature, and may include stent repositioning [2,5,6], replacement [9] or removal [8]. Management of iatrogenic kidney injury depends on the severity of the injury. Minor injuries are usually treated conservatively, including careful monitoring of the patient's vital signs, blood transfusions and follow-up imaging. Conversely, large or persistent lesions require immediate intervention with angio-embolization, and possibly further surgery if necessary [8]. Our patient benefited from a stent change.
Sabnis, et al. [11] have given recommendations to avoid this type of complication: Do not force the guide wire when it is difficult to pass, perform the procedure under fluoroscopic control, and alert the operator to any unusual situation (intense pain, severe hematuria). For early detection, other authors recommend urinary tract radiography or renal ultrasound immediately after the procedure, if the patient presents with disturbed vital signs. An abdominal CT scan should be considered if perforation with haematoma formation is suspected. In the event of hematoma formation, the patient's prognosis may be life-threatening, and treatment must be urgent [8].
The insertion of a J stent is a regular procedure in urology and should not be regarded as trivial. Whatever the procedure and the precautions taken, it is important to ensure that the stent is in place. Follow-up and clinical monitoring are important. Any atypical symptomatology must be investigated and a complication, such as perforation, must be ruled out. This and other serious complications must be taken into account by urologists who insert DJ stents. In the event of insertion due to cancer, the urologist must take care to maximize vigilance (intra- and post-operatively). Exceptions can occur at any time, even during routine procedures.
Not applicable.
Not applicable.
The datasets used and/or analyzed during the current study available from the corresponding author on reasonable request.
No competing interests.
None.
All the authors have contributed to the elaboration of the paper; and this from the conception to the final version.
None.