Pyoderma gangrenosum (PG) is a rare entity belonging to the neutrophilic dermatoses. It is an inflammatory dermatosis with a chronic evolution by relapses, often revealing an associated underlying disease. The location to the breast represents is unusual, poorly documented in the literature and whose diagnosis remains difficult to establish.
We report the case of a 51-year-old female patient, with no particular pathological history, who presented for 4 months a painful ulceration of the left breast, of centrifugal extension measuring 9 cm of the great axis, with a hemorrhagic base, well limited by an inflammatory violaceous border with no other localisations and no notion of trauma. A skin biopsy revealed a dermal neutropilic infiltrate.
The patient was given oral corticosteroid therapy at a dose of 0.5 mg/Kg/day coupled with topical corticosteroids. The results were satisfying: The ulcer gradually healed and the pain reduced.
Pyoderma gangrenosum is a poorly understood clinical entity, classically presenting with inflammatory and painful skin ulcerations. It may occur in a post-surgical or post-traumatic context defining the phenomenon of pathergy described in neutrophilic dermatoses. Treatment is mainly based on topical corticosteroids or in severe cases oral immunosuppressants and the treatment of the underlying pathology.
Neutrophilic dermatoses are considered as inflammatory diseases characterized by cutaneous, epidermal, dermal or hypodermal infiltration by normal neutrophils, with no signs of infection. However, those dermatoses are currently considered rather cutaneous signs of neutrophilic diseases with the possibility of visceral neutrophilic localisations, and are frequently associated with systemic diseases, mainly malignant blood disorders and inflammatory bowl diseases [1].
Pyoderma gangrenosum occurs as nodular lesion which evolves towards a cutaneous painful ulceration of centrifugal extension, with a bleu well- defined, blue, dusky, erythematous borders [2].
The positive diagnosis is clinical; however it remains difficult to establish since there are no precise diagnostic criteria and many other diseases can have the same clinical aspect. Pyoderma gangrenosum usually involves lower limbs, the localization to the breast is uncommon, described in some cases as a complication to surgical procedure or minor trauma.
A 51-year-old patient with a free medical history, presented to our department with a painful breast ulcer that has been evolving for one month in a febrile context. The patient reported noticing a subcutaneous inflammatory nodule on the left breast (Figure 1), which evolved rapidly into a painful ulceration. On examination, the patient was in good general condition; she presented with an ulcerated skin lesion taking up almost the entirety of the left breast measuring 9 cm of the major axis, with a fibrino-hemorrhagic background, well limited by an inflammatory violaceous border (Figure 2).
The lymph node examination did not reveal any peripheral adenopathy, the abdominal and pleuropulmonary examinations were normal. The patient had initially consulted the department of gynecology, an ultrasound coupled with mammography were classified BIRADS 3 of the ACR, a breast biopsy revealed a benign mastopathy. The patient was then transferred to our department where we performed a 3-part biopsy for histological, bacteriological and mycological study. The bacteriological and mycological samples were negative, the skin biopsy was in favor of pyoderma gangrenosum; it showed an ulcerated and necrotic epidermis, a fibrous dermis infiltrated by inflammatory neutrophilic polynucleated cells. Serum protein electrophoresis, thyroid and glycemic assessment were normal. The tumor markers were negative. The abdominal ultrasound and chest tomography were normal and the blood count did not show any hematological disorders.
The patient was given oral corticosteroid therapy: prednisone at a dose of 0.5 mg/day coupled with High-potency topical steroids, fifteen days after the treatment we noticed that the lesion was stable and started to reduce in size, at one month the inflammatory signs and the size of the ulcer reduced significantly (Figure 3).
Pyoderma gangrenosum is a rare neutrophililc dermatosis ; it was first described by the French dermatologist Louis-Anne-Jean Brocq , in 1908 as a fast spreading ulceration of soft tissue [2]. It's incidence is estimated at 6.3 cases per year and per million inhabitants [3], a recent cross-sectional study from the USA found that the prevalence of PG is 58 cases per million adults; the average age of diagnosis is 60 years and it seems to be a slight female predominance [4,5].
This dermatosis usually appears on the limbs, often after a trauma or surgery reflecting the phenomenon of pathergy, the localization to the breast is rare, only few observations were described in literature most of them following breast surgery, however our patient had no history of surgery nor trauma, the lesion appeared spontaneously as an inflammatory nodule (Figure 1) and progressed into the ulceration (Figure 2) [6].
 Figure 1: Image taken by the patient when the lesion was first noticed.
View Figure 1
Figure 1: Image taken by the patient when the lesion was first noticed.
View Figure 1
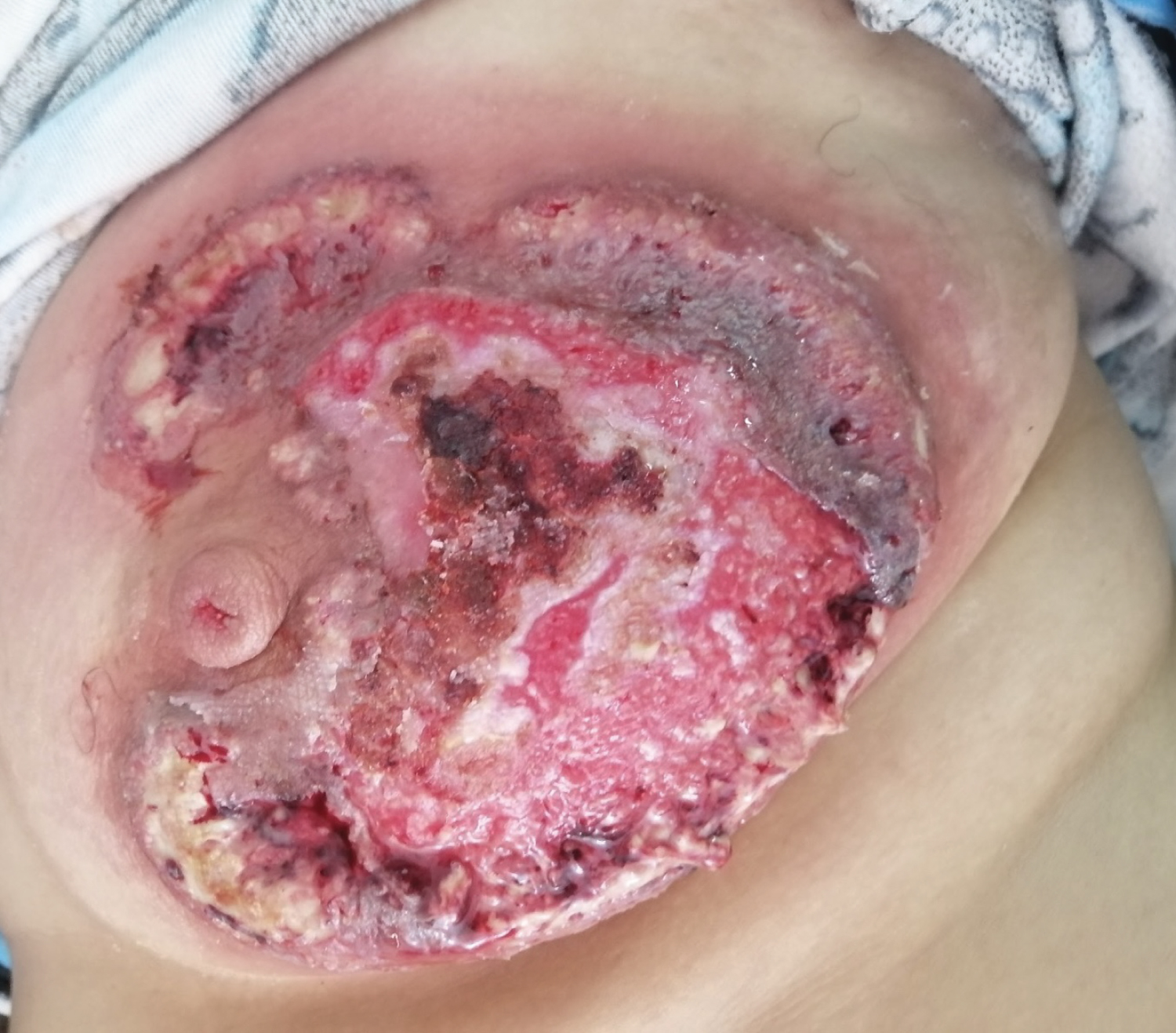 Figure 2: Inflammatory lesion of the breast (the day of consultation).
View Figure 2
Figure 2: Inflammatory lesion of the breast (the day of consultation).
View Figure 2
The diagnosis can be challenging, since there are no defined criteria for PG [3-6], it is often considered as a skin infection which results in a delay in the diagnosis and treatment. In a retrospective study in spain where the authors reviewed of all breast PG cases admitted to Cruces University Hospital over the course of 5 years the mean time for diagnosis was 10.67 months [6].
Different scores and guidelines were proposed for the diagnosis: The mayo diagnostic criteria in 2004 , the international Delphi Criteria and PARACELSUS score in 2018, all had major and minor criteria but in 2021 a cross-sectional retrospective cohort study found that the PARACELSUS score was the most accurate and precise tool to use in the diagnosis of PG [7].
The PARACELSUS score contains major criteria which are: Progressing disease and Assessment of relevant differential diagnoses, Reddish-violaceous wound border and Minor criteria: Amelioration by immunosuppressant drugs, characteristically irregular ulcer shape, extreme Pain visual analog scale > 4/10, localization of lesion at the site of trauma, suppurative inflammation in histopathology, undermined wound border, a systemic disease associated. The diagnostic criteria are scored from 3 to 1 point. The diagnosis is established when the score is greater than or equal to 10 out of 20. Our patient had all three major criteria and some of the minor criteria and a total score of 15.
It has been well documented in the literature that pyoderma gangnosum is usually associated to many different diseases such as inflammatory bowel disease, autoimmune diseases, and hematologic malignancies [1,1,7,8] but in our case we did not find any other diseases associated to PG.
For therapeutic management, there is no standardized therapeutic approach, however, it has been noted that most cases had a good response to topical immunosuppressants, in particularly dermocoticoids or calcineurin inhibitors (tacrolimus). Oral immunosuppressants are used in severe cases. Prednisolone is used in first line at a dose of 0.5-1mg /kg/day, the other options include: Cyclosporine, Azathioprine, Methtexate and Inflixumab [4,8-13].
These treatment modalities should always be accompanied by the treatment of the underlying disease if found. Our patient received topical and oral corticosteroids and had a significant reduction in the size of the lesion and the pain at one month of the treatment (Figure 3 and Figure 4) at 6 months the skin ulceration had almost completely disappeared.
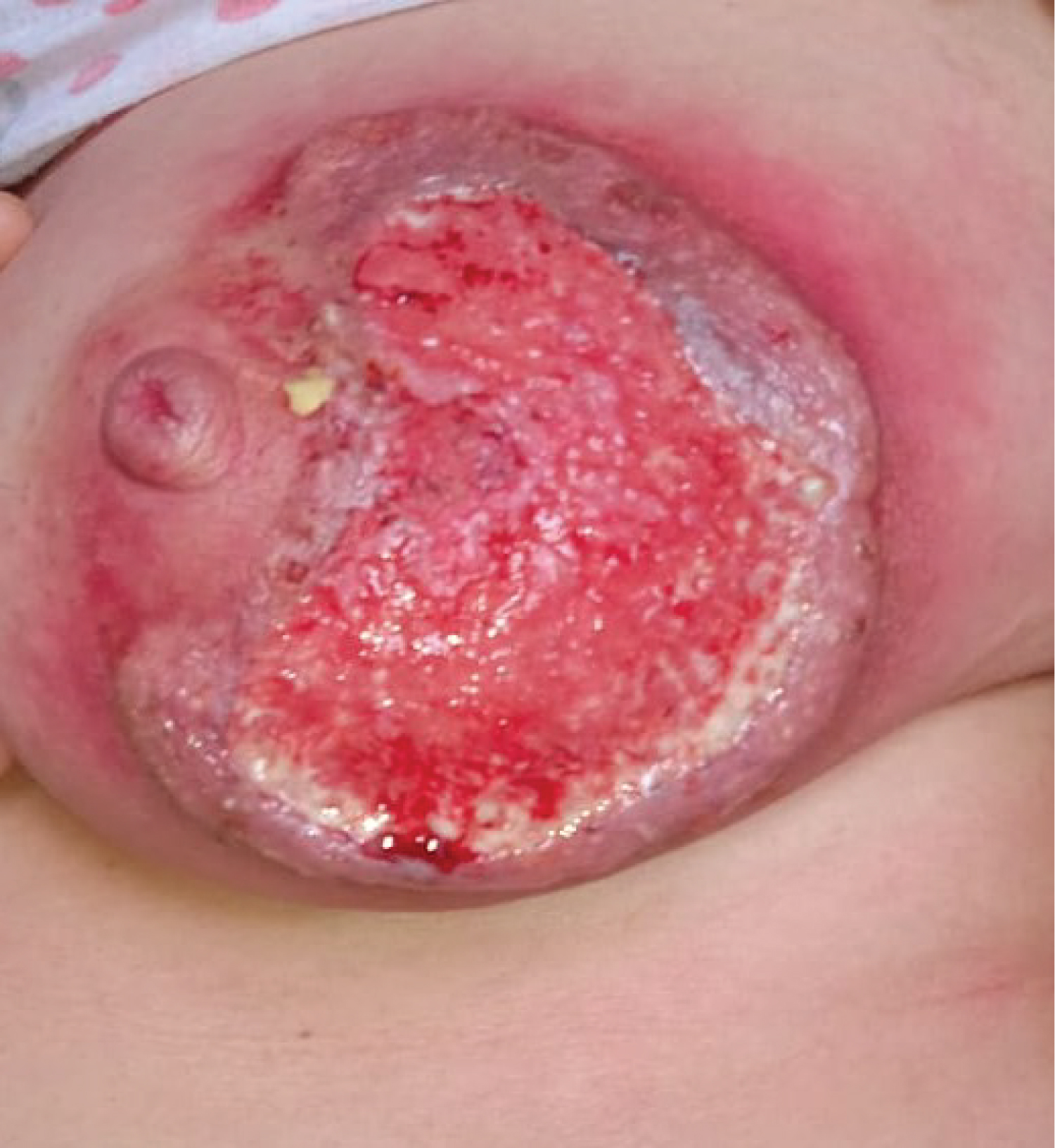 Figure 3: One month of treatment.
View Figure 3
Figure 3: One month of treatment.
View Figure 3
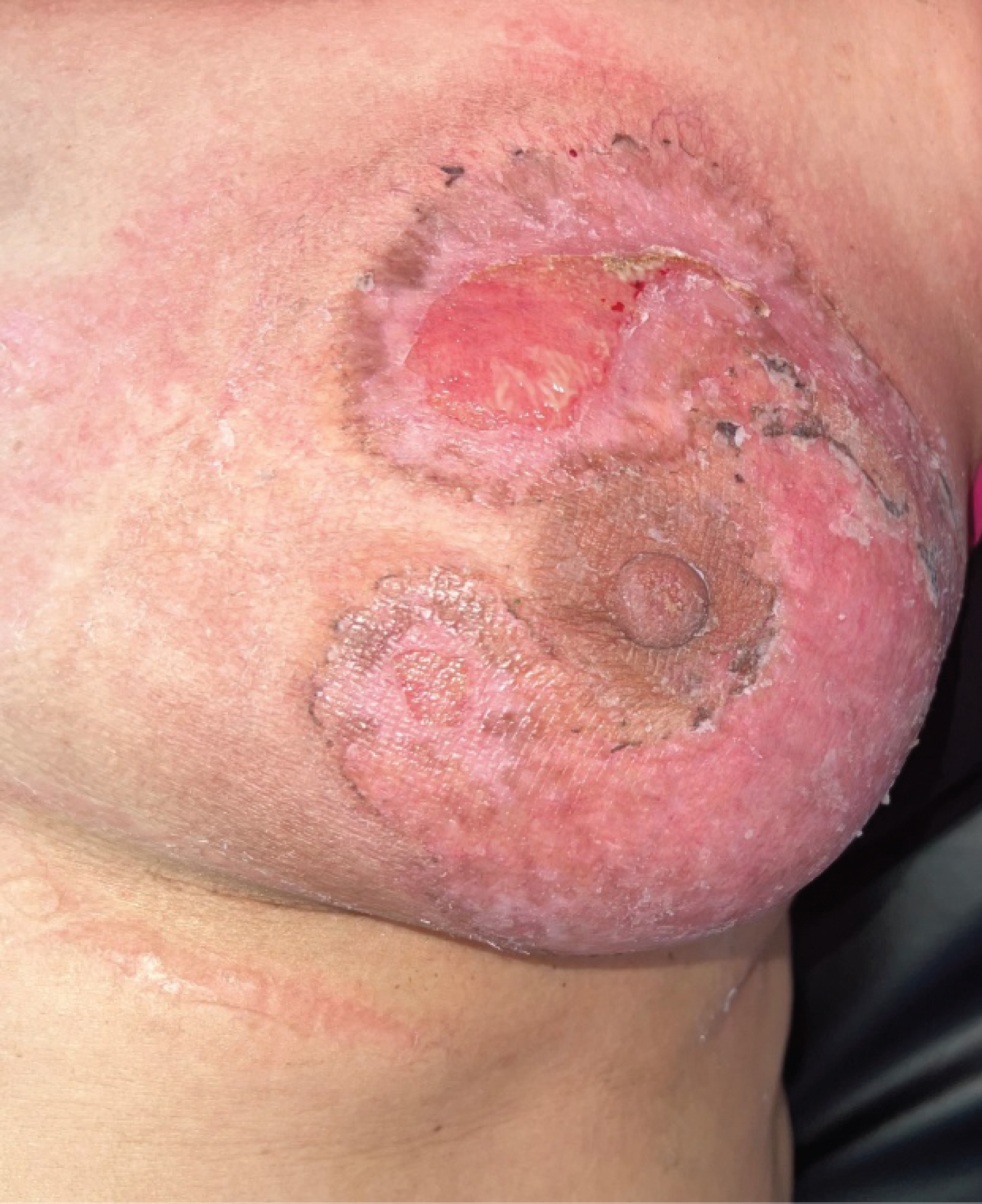 Figure 4 : Six months of treatment.
View Figure 4
Figure 4 : Six months of treatment.
View Figure 4
In conclusion, pyoderma gangrenosum is a rare auto-inflammatory disease; the breast represents one of it's possible localizations. The diagnosis is difficult given the common clinical presentation to other diseases; however it must be considered when a patient presents a chronic cutaneous ulcer of centrifugal extension. The diagnostic approach focuses on the elimination of other causes of cutaneous ulcer and the search of an underlying pathology given the frequency of association of pyoderma gangrenosum to different other diseases, essentially hematological malignancies. Treatment options are mainly based on topical corticosteroids which has shown significant improvement in patients, oral immunosuppressants are used in severe cases. Understanding and early diagnosis of this dermatoses is crucial in order to provide the best health support for our patients.