Pseudo-epitheliomatous hyperplasia (PEH) is a histopathological reaction due to various stimuli, which includes trauma, infection, inflammation, neoplasia. We report a case of a patient with cauliflower outgrowths on an amputation stump simulating a squamous cell carcinoma.
62-year-old patient, diabetic on insulin therapy for 20 years, complicated by arteriopathy and diabetic neuropathy; who benefited from a trans-tibial amputation with prosthesis wear for 6 years. He consults in dermatology for warty, papillomatous, painless outgrowths taking the appearance of "cauliflower lesions" at the level of the amputation stump appeared 1 year ago. The rest of the examination was normal and the popliteal pulses were present. In front of this clinical aspect, we have mentioned a squamous cell carcinoma, skin metastases, soft tissue sarcoma, cutaneous B lymphoma, lymphangiectasia. Two skin biopsies were performed showing a hyperkeratotic, acanthotic epidermis, a fibrous dermis harboring a perivascular mononuclear inflammatory infiltrate evoking a PEH (Figure 1).
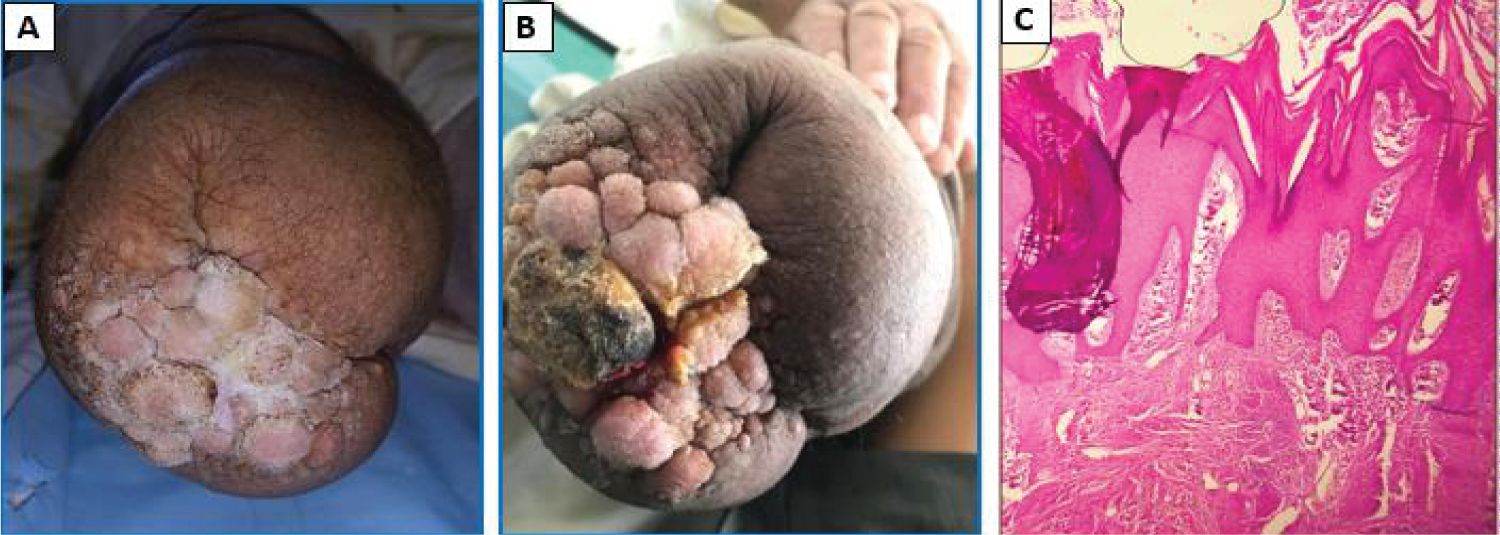 Figure 1: (A, B) Clinical picture of warty cauliflower outgrowth on amputation stump (knee) seen from below; (C) Histology (Hematoxylin-Eosin Stain): Hyperkeratotic, acanthotic epidermis with a fibrous dermis harboring a perivascular mononuclear inflammatory infiltrate.
View Figure 1
Figure 1: (A, B) Clinical picture of warty cauliflower outgrowth on amputation stump (knee) seen from below; (C) Histology (Hematoxylin-Eosin Stain): Hyperkeratotic, acanthotic epidermis with a fibrous dermis harboring a perivascular mononuclear inflammatory infiltrate.
View Figure 1
PEH is a benign condition, characterized by hyperplasia of the epidermis linked to chronic inflammation [1]. It can be primary affection or due to many dermatoses such as a vegetative mycosis (chromomycosis. candidiasis, blastomycosis, cryptococcosis, histoplasmosis, coccidioidomycosis), a mycobacteriosis, a syphilide or a vegetative piannid. It can also be due to exogenous factors such as: chronic irritation or red tattoo pigments [2]. In our case, the lesions are due to mechanical stress between the socket of the prosthesis and the amoputation stump. Clinically, PEH comes in the form of well-defined budding plaques or nodules with flaking and scales. Papules or nodules can vary from < 1 cm to several centimeters. The color of the lesion can be identical to the skin itself or hyperpigmented.
The diagnosis of PEH is sometimes difficult; especially when the etiology does not appear obvious, and is often confused with an epidermoid carcinoma. It is therefore necessary to carry out deep and wide biopsies arriving to the reticular dermis, and do not hesitate to repeat them in order to guide the pathologis, because the treatment and the prognosis change. An incorrect diagnosis of malignancy will lead to radical surgery with the risk of postoperative complications.
None.
Farah El Hadadi and Line Mezni carried out the case report and wrote the manuscript with support from Meriem Meziane and Kaoutar Znati. Leila Benzekri and Karima Senouci supervised the project.