Tongue abscess is rare but can be life-threatening especially if the cause of it is not removed promptly. It usually results from trauma, foreign body, lingual tonsils pathology, thyroglossal duct remnants or dental diseases. The etiology of the disease can be found out by obtaining a detailed history from the patient and physical examination with the assistance of lab investigation, laryngoscope, imaging tools such as Computed tomography (CT), Magnetic Resonance Imaging (MRI) and Ultrasonography (US). The main principles of the management of tongue abscess are maintaining the patency of the airway, draining the abscess, antibiotics therapy or even surgical approach. We present a tongue abscess case which the etiology was a fish bone sits deeply in the tongue.
Tongue abscess, Foreign body
Tongue abscess is seldom seen but can be a life-threatening disease which can end up in airway compromise or sepsis. There were few cases reported before but the recent documented cases from 1993 to 2008 in English language are about 33 cases [1]. Predisposing factors for the formation of tongue abscess are genders (mainly male), smokers, unhygienic oral condition, diabetes mellitus, immunodeficiency, chemotherapy and others [2]. The location of abscess also can be either anteriorly or posteriorly. For the tongue abscess located at anterior two thirds, it is usually a result of accidental self-biting, traumas, and foreign bodies, while lingual tonsillitis or malignancy, dental diseases involving first and second molars and the thyroglossal duct remnants contribute to the posterior third tongue abscess. It can also involve both sides in a chronic setting like this case.
A 56-year-old gentleman with underlying hypertension and gout, presented with tongue swelling and pain for one month, associated with poor speech conveyance. Prior to the incident, he accidentally bit over the left tongue while eating and noted bleeding and swelling over the injury site for one week. The swelling resolved as he received antibiotic following a procedure to remove the tophi of over his bilateral elbows. However, the swelling and pain over the left aspect of tongue recurred one week after the completion of antibiotics and the condition worsened. He had no fever or constitutional symptoms; and he tolerated orally minimally due to the pain. He denied any foreign body or seafood consumption and had no high-risk sexual behaviour.
Ear and nose examination were unremarkable, and he had no neck nodes palpable. Oral examination revealed swollen left tongue, almost occupying the entire lateral aspect, from its anterior to the middle third (Figure 1). It was tender, soft and smooth upon palpation, about the thickness of 2 cm as compared to the right tongue and there was no mass or ulcers over the tongue. No foreign body was felt, and his dental hygiene was good. Flexible laryngoscope showed a bulging site above the left base of tongue with mild narrowing of the pathway to the supraglottic region (Figure 2).
 Figure 1: (a & b) Swelling over the anterior and lateral aspect of left tongue respectively (red arrows).
View Figure 1
Figure 1: (a & b) Swelling over the anterior and lateral aspect of left tongue respectively (red arrows).
View Figure 1
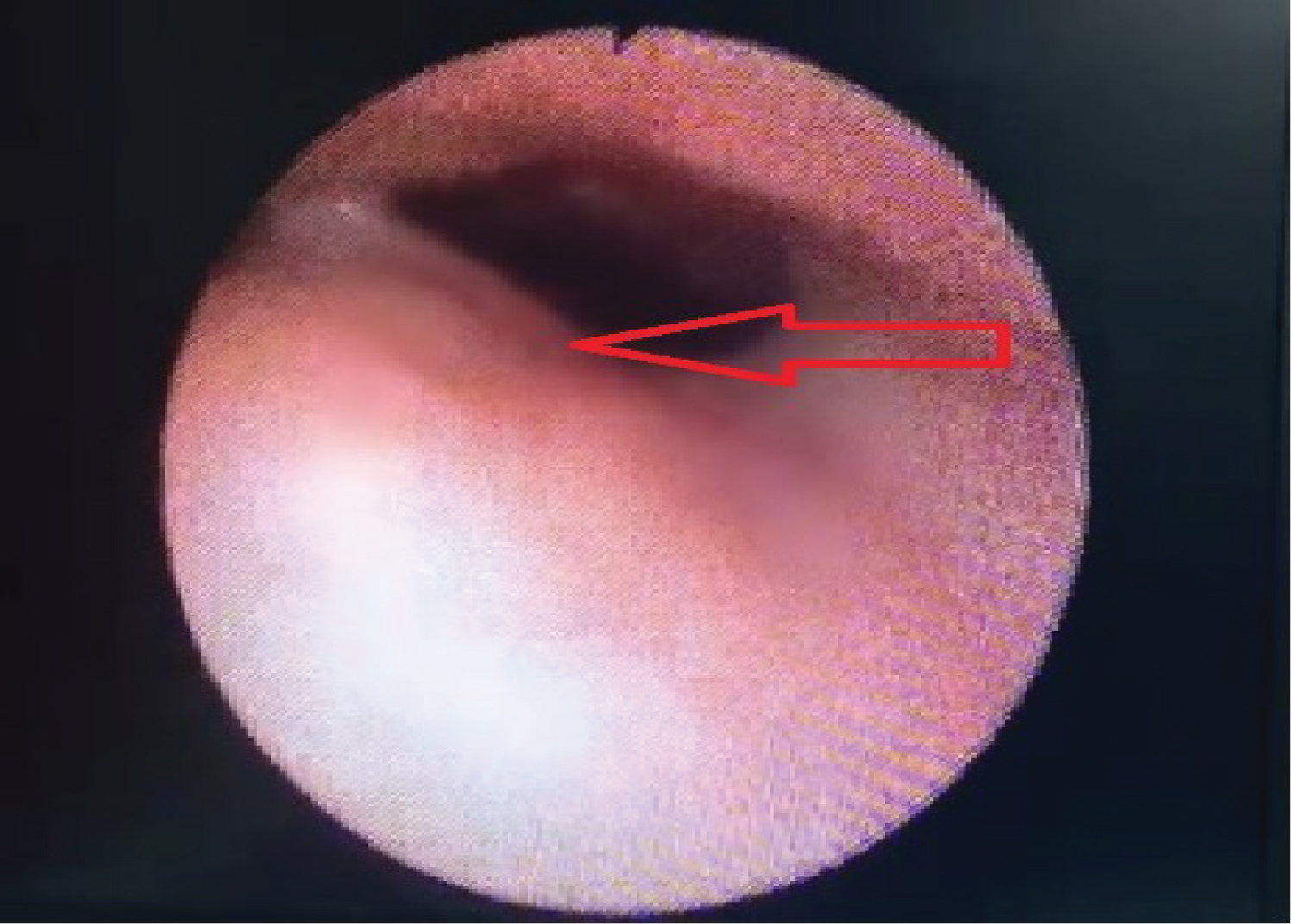 Figure 2: Flexible laryngoscope findings, noted bulging site above his left base of tongue, slightly narrowing the pathway to the supraglottic region (red arrow).
View Figure 2
Figure 2: Flexible laryngoscope findings, noted bulging site above his left base of tongue, slightly narrowing the pathway to the supraglottic region (red arrow).
View Figure 2
Otherwise, the vallecula, epiglottis and bilateral arythenoids, pyriform fossa and vocal cords were normal, and no foreign body or pus discharge was seen. Aspirations were attempted over the anterior and lateral left tongue after given 2% lignocaine gel, but no pus or discharge was aspirated. Computed Tomography (CT) scan of the neck was arranged, and it showed bulky left tongue and left oropharyngeal wall with mild narrowing of the oropharyngeal lumen on the left side and no definite rim enhancing collection or foreign body was seen (Figure 3). Full blood count showed mild elevation of white blood cells (WBC), mainly neutrophils.
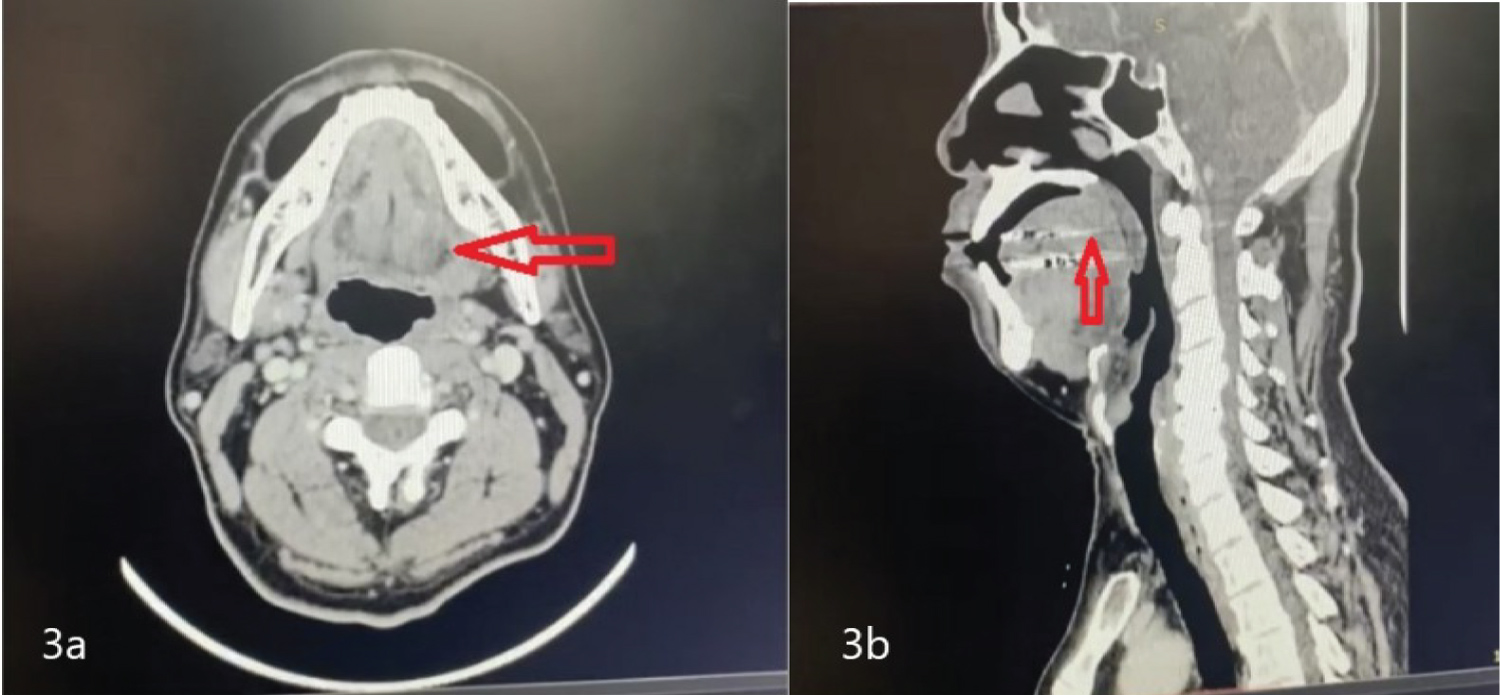 Figure 3: CT scan in soft tissue setting (a) Axial view, bulky left tongue and left oropharyngeal wall (red arrow); (b) Sagittal view, bulky left tongue and left oropharyngeal wall causing mild narrowing of the oropharyngeal lumen.
View Figure 3
Figure 3: CT scan in soft tissue setting (a) Axial view, bulky left tongue and left oropharyngeal wall (red arrow); (b) Sagittal view, bulky left tongue and left oropharyngeal wall causing mild narrowing of the oropharyngeal lumen.
View Figure 3
He was admitted and started on intravenous (IV) Augmentin. On day 2 of antibiotics, the swelling site resolved minimally, and the patient claimed his speech improved. Oral examination revealed a punctum over the swelling site and minimal pus discharged upon milking. No culture was sent in view of minimal amount of pus being milked and mixed with saliva. During hospitalization, no fever was documented; and the vital signs were stable, and he could tolerate orally as usual. He was discharged after three days of admission with oral antibiotic to be completed for total of one week. Three days after discharge from the hospital, his left tongue swelling receded, but he felt something sharp over it. When he examined the tongue, he noticed there was a sharp object protruding from the left tongue and removed it uneventfully. He then recalled that he had consumed a Mackerel fish 1 month ago. During his visit to our clinic at the following day, he was well and the tongue appeared normal (Figure 4). The foreign body was indeed a fish bone around 1 cm in length (Figure 5).
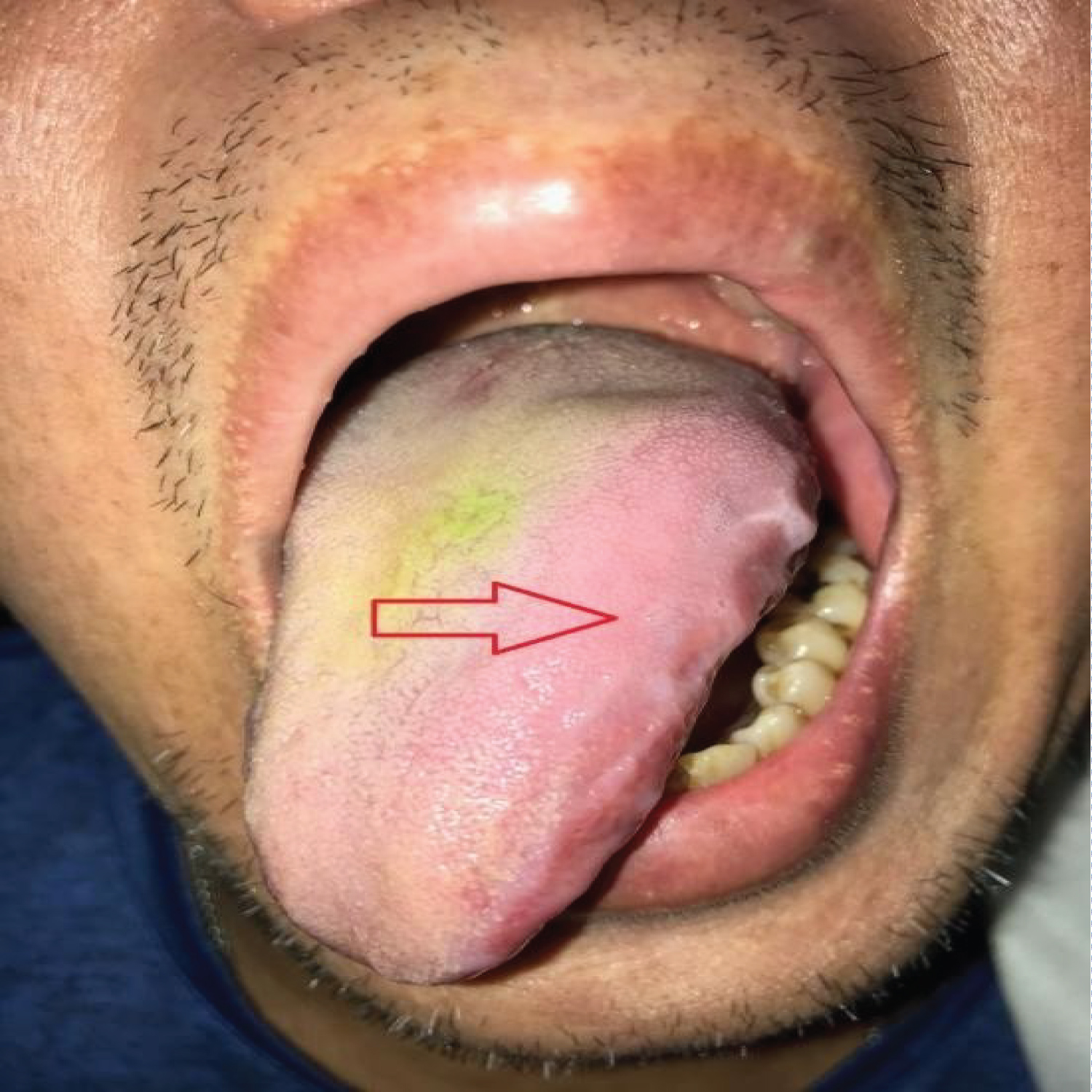 Figure 4: The entire left tongue swelling resided with groove of teeth compression (red arrow) noted after day 6 of antibiotics.
View Figure 4
Figure 4: The entire left tongue swelling resided with groove of teeth compression (red arrow) noted after day 6 of antibiotics.
View Figure 4
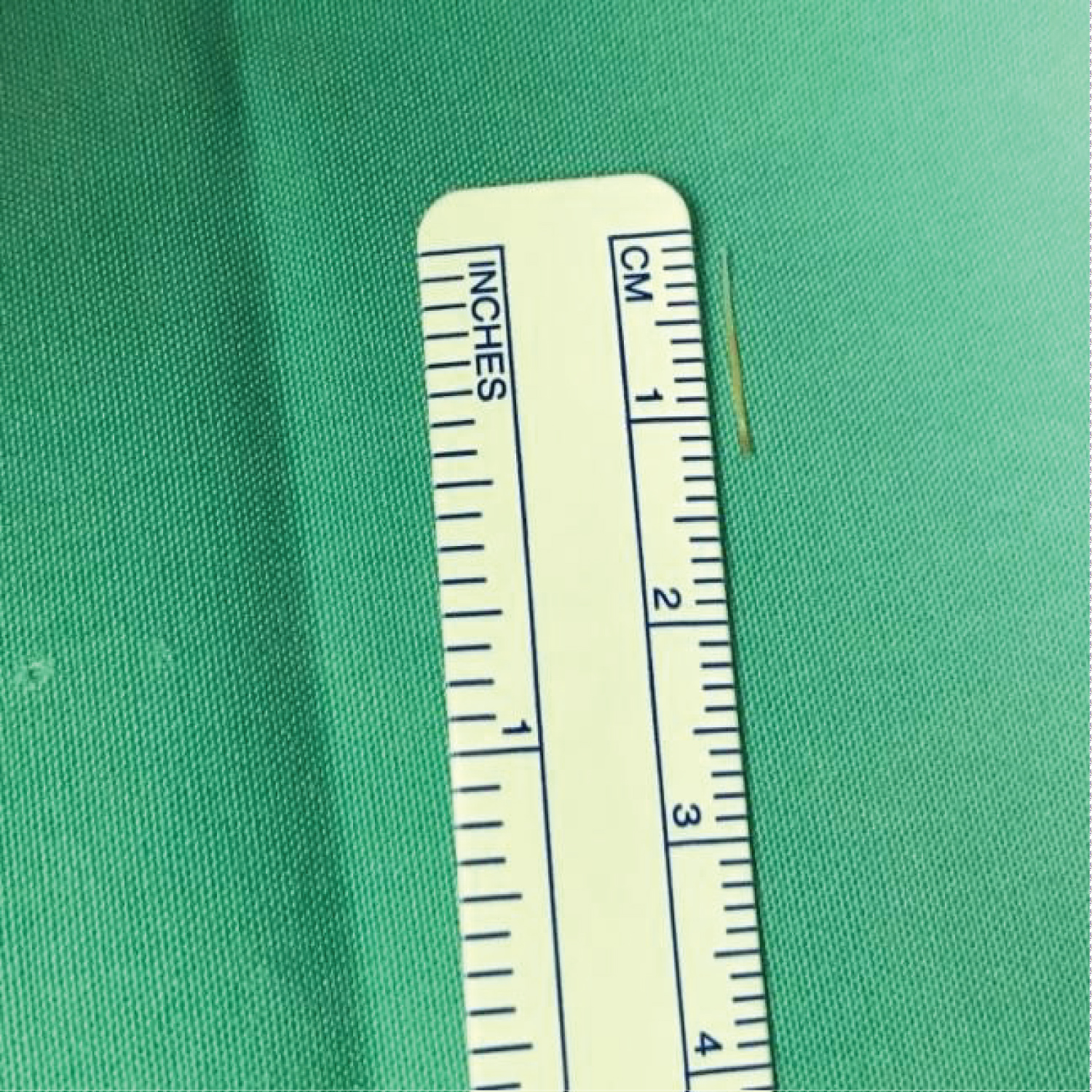 Figure 5: Fish bone around 1cm in length found.
View Figure 5
Figure 5: Fish bone around 1cm in length found.
View Figure 5
Fish bone ingestions are frequently seen in otorhinolaryngology (ORL) practice; and commonly, the fish bones lodged at the palatine tonsils, base of tongue and vallecula. The impaction of a fish bone in the pharynx usually occurs at the base of the tongue or in the vallecula. However, deeply seated fish bone found on the mobile tongue is indeed rare, as foreign body on this mobile part of the tongue is generally superficial and it can be easily removed by the general practitioner or the patients themselves [3].
Obtaining a detailed clinical history is crucial in looking for the cause of tongue abscess. In our scenario, the patient was unable to recall the history regarding foreign body injury to his tongue at the first examination, causing him to have a neglected fish bone in the tongue which led to tongue abscess formation. The formation of tongue abscess in our patient may be further explained by the disruption of his own defense system and growth of pathological bacteria [2,4]. The protective mechanisms of infection, i.e., the tongue is highly vascularized with rich lymphatics, rigidity of tongue muscles, integrity of the original tongue's squamous epithelium, mobility of the tongue, and defensive properties of saliva [2,5-9]. Our patient's lesion was on the anterior tongue which usually presents with symptoms like odynophagia, dysphagia, tender and swollen tongue, limitation of tongue movement, and problem with word pronunciation or speech and afebrile. Impending airway obstruction is not uncommon as the tongue abscess at the anterior part easily involves the sublingual space. Thus, the pathophysiology of causing airway obstruction is akin to Ludwig's angina. Besides, the differential diagnosis of anterior tongue lesion should include neoplasms in elderly, lingual artery false aneurysm, infectious diseases in areas of high endemicity such as tuberculosis, syphilis and actinomycosis. Other risk factors like smoking, poor oral hygiene, immunodeficiency status, and diabetes contribute to the development of tongue abscess.
Besides meticulous history taking from the patient, the diagnosis of tongue abscess is also made based on thorough otorhinolaryngology physical examination, which includes palpation of the tongue as well as the other subsites of the oral cavity. The use of laryngoscope is mandatory if it is suspicious of foreign body in situ. Minor surgical intervention such as needle aspiration, laboratory investigations and imaging, do provide further information. Mostly, the patients will have normal level of white blood cells (WBC) or mild leucocytosis [6,7] which was similar to our patient. Needle aspiration aids to confirm a diagnosis and decide further treatment. Contrast-enhanced CT scan provides us the valuable information regarding the extension of the tongue abscess as well as the potential deep neck spaces involvement. Magnetic resonance imaging (MRI) enables us to evaluate soft-tissue structures and highlight the contrary of the abscesses but in view of its time-consuming factor and its availability, it is not practical in patients with impending airway compromise. In our case, although there was no collection or foreign body seen in CT, MRI can still be considered if the tongue lesion was highly suspicious of foreign body injury. Alternatively, ultrasonography (US) can be used as an advantageous diagnostic tool for its non-ionized method, noninvasive, and cost-effectiveness [10,11].
The main principles of the management of tongue abscess for the successful outcome include maintaining the airway, draining the abscess, and antibiotics therapy [6,9,12]. Maintaining the airway is significant, though posterior tongue lesion is frequently associated with airway compromised; the anterior tongue abscess which involves the sublingual space does potentially lead to airway obstruction. Regular vital signs monitoring as well as signs of respiratory distress should be identified, and promptly tracheostomy when indicated. Draining the abscess can be done either by needle aspiration or open surgical drainage. The needle aspiration is advantageous as it avoids general anaesthesia which may aggravate the airway oedema during intubation and this procedure is repeatable if indicated [13,14]. Surgical drainage of tongue abscess by making a small incision over the punctum or the most bulging part can release the tension and tenderness, drain and collect the pus for culture or biopsy if malignancy is suspected [6] and reduce of the chance of reinfection [15]. Broad spectrum antibiotics, i.e., Augmentin (combination of amoxicillin and clavulanic acid), clindamycin [6], or a combined agent such as Augmentin or clindamycin or metronidazole plus cephalosporin groups, could be administered to target the possible organisms originating from the oral cavity and oropharynx which usually comprise gram positive, anaerobic, and gram-negative bacteria [2,13,14]. Indeed, the antibiotic treatment should be adjusted according to the pus's culture and sensitivity [6,12].
The tongue abscess is a rare but potentially life-threatening disease. The causes and risk factors of this disease have to be considered in order to eradicate the root of it. Patient's clinical history, general condition, and our physical examination in combination of (ORL) scope are vital in excluding airway compromise and finding the cause of abscess formation. CT imaging assists in diagnosing and evaluating any deep neck spaces involved. The antibiotic therapy together with surgical drainage is the treatment of choice for tongue abscesses but any foreign body or patient's underlying habits or diseases such as smoking and diabetes should be well modified to prevent recurrence.