Globally, India has one of the highest burdens of tuberculosis (TB). The diagnosis of tuberculosis is challenging, particularly in young children due to a high rate of extra-pulmonary and meningeal disease. Scrofuloderma is cutaneous tuberculosis, accounting for approximately 1.5% of extra-pulmonary cases. Mycobacterium tuberculosis is the main etiological agent and, rarely, by Mycobacterium bovis. The cutaneous variants of tuberculosis have a variable clinical appearance, significance and prognosis. Here, we describe the case of a 9-year-old boy presenting with multiple abscesses and discharging sinuses over neck since 1 year. Skin punch biopsy from anterior aspect of lesion was suggestive of scrofuloderma. It constitutes very small percentage of extra-pulmonary tuberculosis and rarely seen in pediatric age group.
Scrofuloderma, Tuberculosis, Lymphadenopathy
Cutaneous tuberculosis or Scrofuloderma is caused by Mycobacterium tuberculosis, M. bovis and rarely Calmette-Guerin bacillus. Scrofuloderma is also known as "tuberculosis cutis colliquativa", a commonly used term for cutaneous tuberculosis in children and young adults. The introduction of the organism may be by exogenous inoculation, hematogenous route or by direct spread through underlying foci. The immune status of an individual determines the clinical presentation of cutaneous tuberculosis [1]. Cervical group of lymph nodes are most often involved followed by axillary, inguinal group of lymph nodes [2]. Scrofuloderma begins as firm, deep seated nodule adherent to skin followed by softening, suppuration, perforation and then, lastly formsan ulcer or sinus. Later on, a scarred tract develops and bridges the ulcerative areas [2,3]. Here we report a rare case of scrofuloderma in pediatric patient.
A 9-year-old boy, presented with complains of multiple abscesses and discharging sinus over neck for duration of 1 year. He also complained of swelling in the right axillary region since 1 week. There was no history of any respiratory, urinary or gastro-intestinal symptoms. General examination revealed mild pallor. Multiple bilateral cervical lymph nodes were palpable. Vital signs showed that body temperature was 36.7 °C, blood pressure was 104/60 mmHg, heart rate was 88 beats/min, respiratory rate was 20/min, and pulse oximetry was 96%. On local examination, multiple undermined black colored ulcerative lesions were present with discharging pus sinuses with puckered scar marks over the anterior aspect of the neck (Figure 1). In the right axilla, a single soft, non-tender, fluctuant swelling measuring 1.5 × 1.5 cm was present (Figure 2). On abdominal examination, spleen was just palpable and liver was palpable 2 cm below the right costal margin with normal consistency. Respiratory and cardiovascular systems were normal. Investigations revealed a hemoglobin of 8.3 g/dl, total leukocyte count of 6100 cells per cumm with normal differential count, and platelet count of 5,60,000 per cumm. Peripheral smear showed a normocytic moderately hypochromic with few microcytes and occasional pencil cells. Erythrocyte sedimentation rate was 65 mm/hr. Mantoux test done showed an induration measuring 30 mm at 72 hours. Biochemical parameters were normal. Serologic testing for human immunodeficiency virus (HIV) was negative. Sputum for acid fast bacilli (AFB) was negative. Chest X-ray was normal. Ultrasonography of abdomen showed borderline splenomegaly. Skin punch biopsy from anterior aspect of lesion present over neck region was taken which showed atrophied epidermal lining with loss of rete pegs and islands of epidermis trapped in the dermis. Underlying the dermis, chronic inflammatory infiltrate composed predominantly of lymphocytes and few polymorphs with multinucleated giant cells at places were present. No areas of congestion, edema, hemorrhage or necrosis were seen. The histopathological features were suggestive of cutaneous tuberculosis or scrofuloderma. On the basis of local examination of ulcer, skin biopsy findings and a positive mantoux test, a diagnosis of extra-pulmonary tuberculosis of cutaneous tuberculosis (Scrofuloderma) was made. Patient was started on four druganti-tuberculosis treatment (ATT) with isoniazid, rifampicin, pyrazinamide and ethambutol daily under category I according to Revised National Tuberculosis Control Program (RNTCP) -Directly Observed Treatment Short-course (DOTS) strategy. The condition of the patient has improved after treatment with ATT.
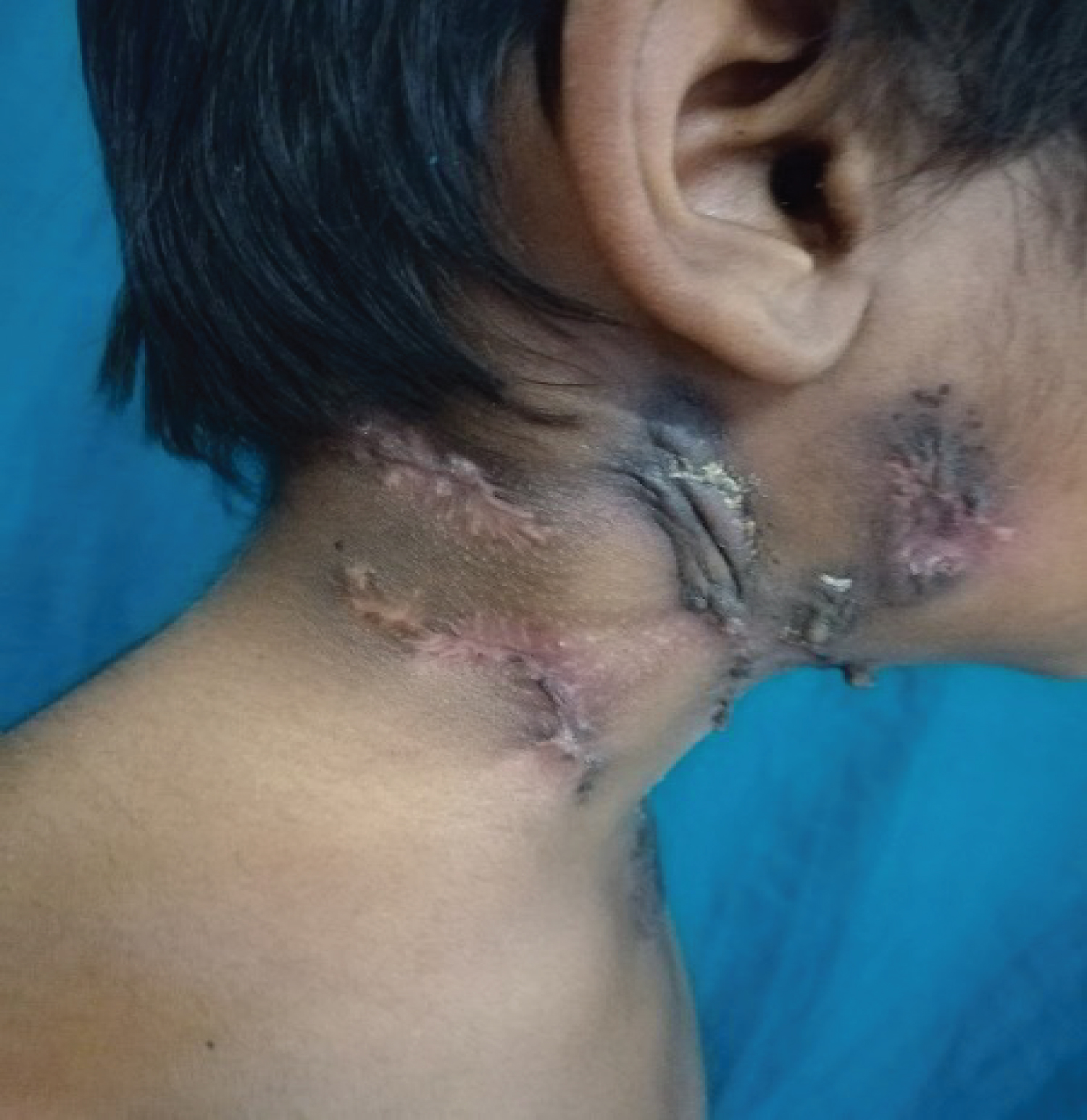 Figure 1: It shows multiple undermined black colored ulcerative lesions present with pus discharging sinuses with puckered scar marks on the neck.
View Figure 1
Figure 1: It shows multiple undermined black colored ulcerative lesions present with pus discharging sinuses with puckered scar marks on the neck.
View Figure 1
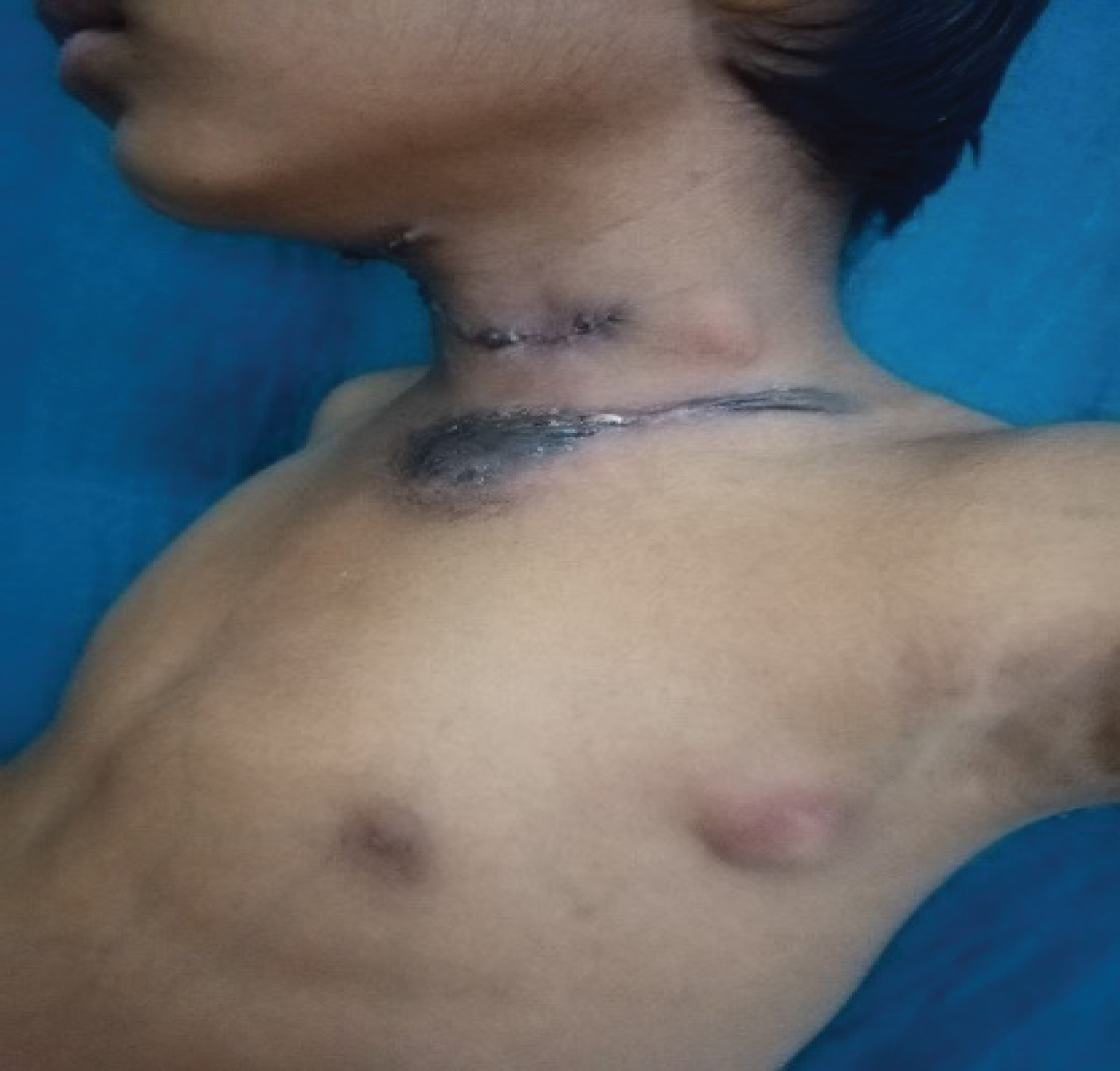 Figure 2: It shows single soft swelling over left axillary region.
View Figure 2
Figure 2: It shows single soft swelling over left axillary region.
View Figure 2
Tuberculosis is one of the biggest health crisis in India accounting for 2.2 million cases each year [4]. Cutaneous tuberculosis accounts for only 0.1-0.9% of total out-patients in dermatology in India. Most commonly affected are adolescents belonging to 10-14 years age-group [3,5]. Shrestha SB, et al. [6] observed that scrofuloderma was the most common form of cutaneous tuberculosis accounting for 47% (8/17) of total cases of cutaneous tuberculosis in children. Scrofuloderma results from the contiguous spread to the overlying skin from adjacent structures such as lymph node, joint, bone or the epididymis. Most commonly neck, axillae or groin are involved. Clinically, it presents as a firm subcutaneous nodule that enlarges, becomes confluent, ulcerates and forms draining sinus tracts of caseous material [7]. Histopathologically, ulcerated dermal abscess with scattered histiocytes with few lymphocytes and marked caseative necrosis containing abundant bacilli can be seen [8]. A study by Kar, et al. [9] described two pediatric cases, one with ulcerated lesion with undermined edges over upper chest with axillary lymphadenopathy while the other case presented with multiple pustular lesion over right post auricular, right supraclavicular region and right axillary region. Our patient also presented similarly with multiple abscess and discharging sinus from the cervical nodes. Scrofuloderma may also be a manifestation of systemic tubercular disease and can result from direct extension or hematogeneous spread of the infection. Systemic involvement has been reported to be associated with 21.3% of children with cutaneous tuberculosis [10]. However, there was no evidence of systemic involvement in the index case. Diagnosis of scrofuloderma is complicated and requires a full work-up, including a detailed history and physical examination, clinical presentation, blood investigation including complete blood count, ESR, skin biopsy with histological analysis and special staining methods for identification of AFB. Mantoux test is a good screening test for tubercular infection. The use of other diagnostic tests, such as chest X-ray and culture for Mycobacterial culture remains the most reliable method [11]. Differential diagnosis of discharging sinuses are atypical mycobacterium due to M. scrofulaceum and M. avium, actinomycosis, sporotriciasis, botyomycocsis, nocardiosis, hidradenitis suppurativea [9,11-13].
Treatment of scrofuloderma follows similar recommendations as other forms of TB with multi-drug therapy (MDT) and ideally adjusted as the culture and susceptibility data. Our patient was started on ATT with four drug intensive phase comprising of Isoniazid (H), Rifampicin (R), Pyrazinamide (Z) and Ethambutol (E) (HRZE) in daily doses (as per four weight band categories) for eight weeks and later put on continuation phase with three drugs with Rifampicin, Isoniazid, and Ethambutol (HRE) for 16 weeks. In the meanwhile, liver enzymes and total blood counts were steadily monitored. Lesion has almost completely resolved with no active pus discharge and is currently on a follow-up of 6 months post completion of ATT with no active complaints. Rarely surgery may be required in the management of extensive scrofuloderma, however, it was not needed in our patient. In conclusion, although scrofulodermais a known entity but poses a big diagnostic difficulty and it can be effectively treated with the current regimen of ATT drugs.
None.
None.
None.