Diabetes mellitus is associated with a wide variety of musculoskeletal manifestations which can significantly affect a patient's quality of life. One of these manifestations is Limited joint mobility syndrome (LJMS) also known as diabetic cheiroarthropathy (DCA) which affects the hands. Herein is a case of a 50-year-old female patient with type 2 diabetes mellitus who was diagnosed with DCA after complaining of limited movements of all joints in her hands and tightening of the skin. Her diabetes mellitus was uncontrolled, and she was found to have diabetic nephropathy and non-proliferative diabetic retinopathy.
Physicians taking care of diabetic patients should be able to diagnose this condition and recognize its association with diabetic complications.
Musculoskeletal disorders such as Achilles tendon pathology, trigger finger, Dupuytren's, limited joint mobility syndrome (LJMS), carpal tunnel syndrome, frozen shoulder and plantar fasciitis have been found to occur more often in subjects with diabetes compared to those without diabetes [1].
LJMS is one of the musculoskeletal disorders and is rather underexposed and under diagnosed compared to the well-known micro- and macrovascular complications of diabetes. The diagnosis of LJMS is based on clinical examination and can identify patients who are at risk for serious diabetes complications.
A 50-year-old female with a 10-year history of type 2 diabetes mellitus, was referred to the rheumatology clinic with reported pain and stiffness in both hands of one-year duration.
She reported stiffness in her through the day. She has limited movements in all joints in her hands with associated tightening of the skin. She denied any changes in the color of her skin in her fingers with cold weather. There was no dysphagia, no dry eyes, and no dry mouth.
Review of her chart showed that she lost to follow up on her diabetes for about a year and presented to her primary care physician with symptoms of uncontrolled DM, in addition to her hand's symptoms.
Her glycosylated hemoglobin (HbA1c) was 10%, she was on treatment with oral hypoglycemic agents.
Her hands examination showed thick, tight, waxy skin with limited joint range of motion (inability to fully flex or extend the fingers) (Figure 1). She had positive “prayer” and “table top” signs. The prayer sign is said to occur whenever there is incomplete approximation of one or more of the digits when the patient attempts to approximate the palmar surfaces of the proximal and distal interphalangeal joints with palms pressed together and the fingers abducted (Figure 2). She was not able to completely lay her palms flat on a horizontal surface which denotes a positive tabletop sign.
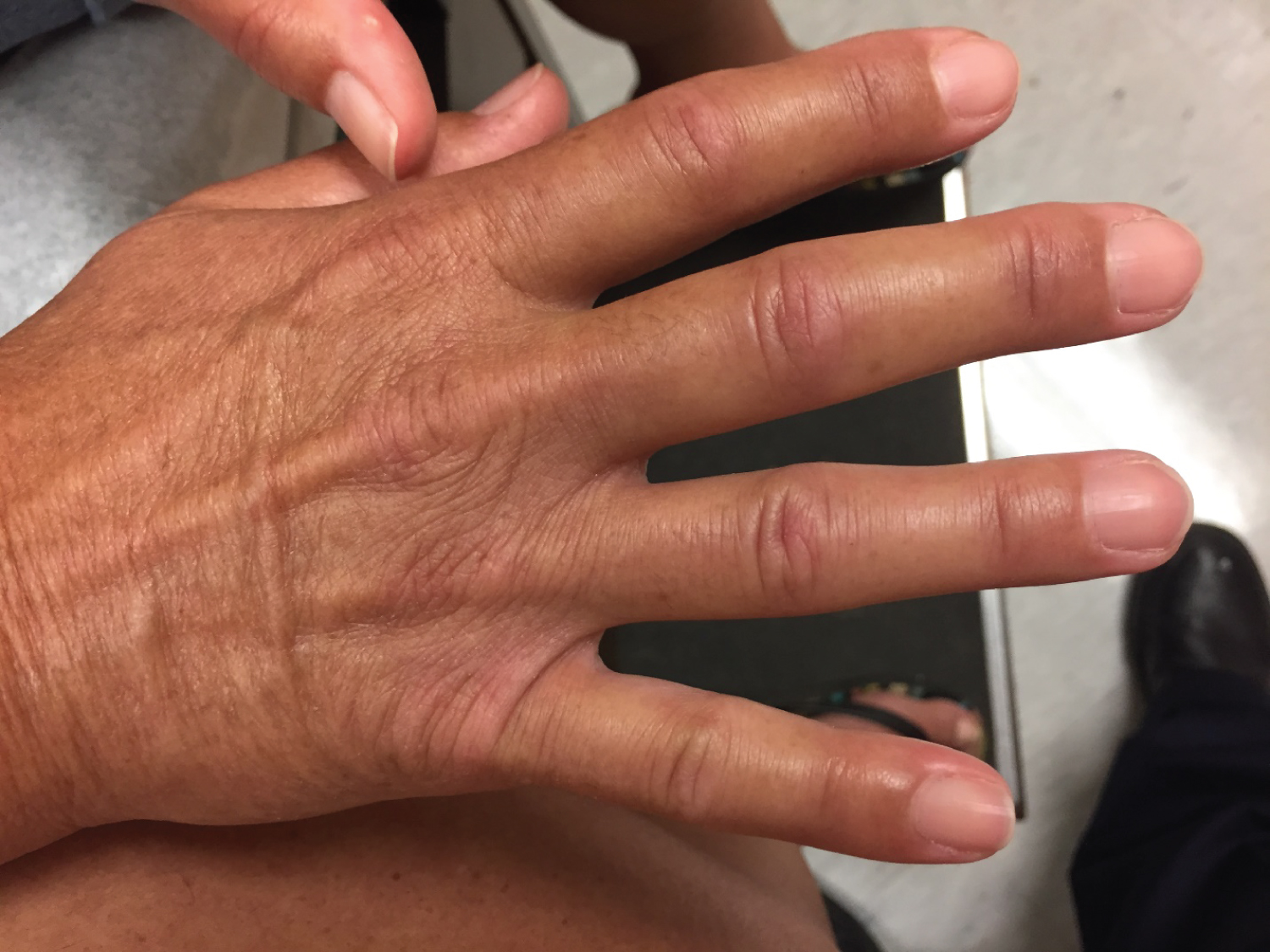 Figure 1: Diabetic hand with tight, thick waxy skin and incomplete extension. View Figure 1
Figure 1: Diabetic hand with tight, thick waxy skin and incomplete extension. View Figure 1
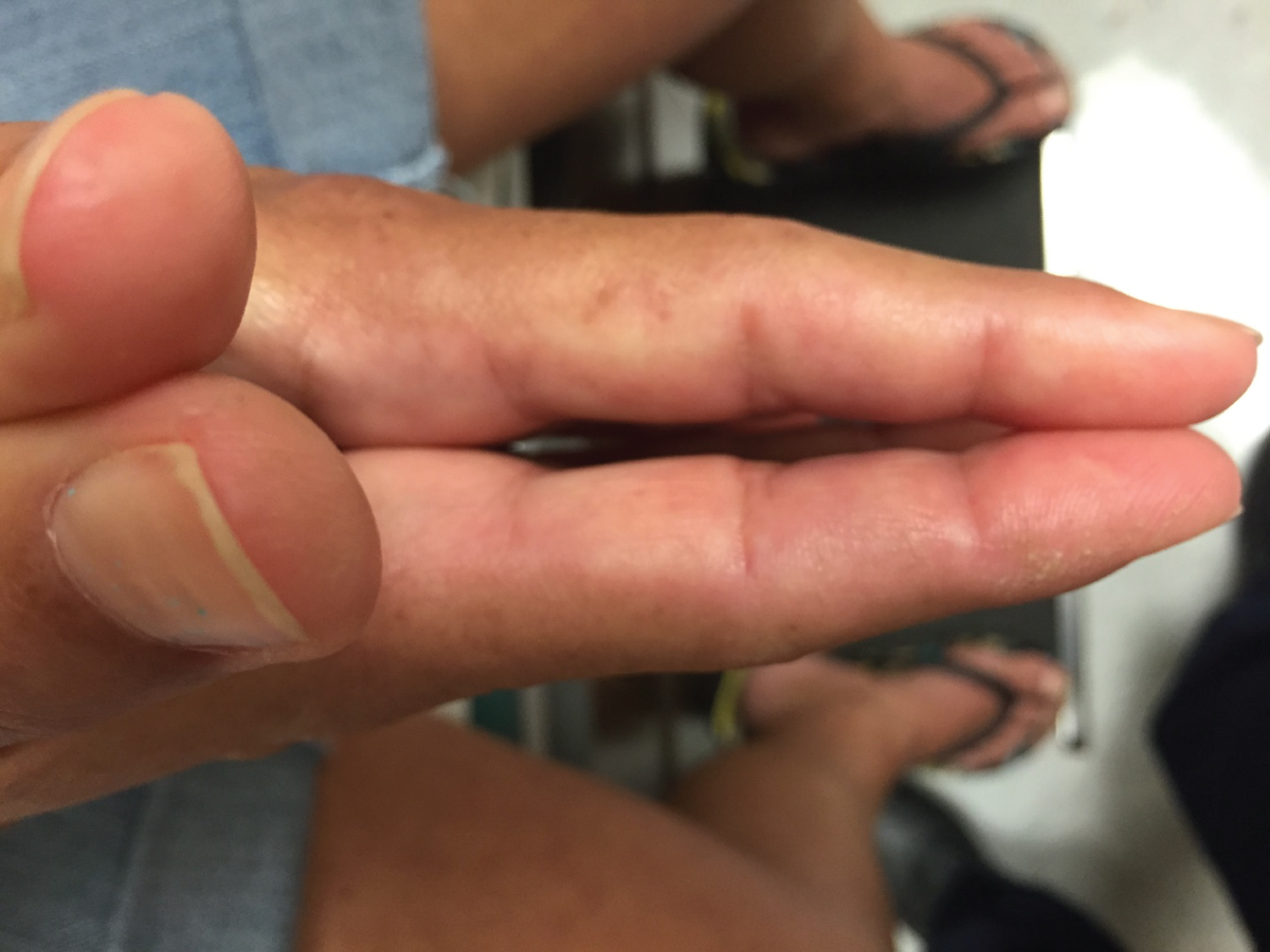 Figure 2: Positive prayer sign. View Figure 2
Figure 2: Positive prayer sign. View Figure 2
She also had early Heberden's nodes in her distal interphalangeal joints indicating osteoarthritis in her hands.
There was no evidence of Duputren's contracture. She had negative Tinel's and Phalen's tests. There was no evidence of flexors tendons synovitis.
Her investigations showed normal ESR, CRP, Negative rheumatoid factor, anti-CCP. Radiographs of her hands showed mild osteoarthritis.
She was advised to follow closely with her primary care physician for tight control of her diabetes mellitus. Further work up done by her primary care physician showed microalbuminuria indicating diabetes nephropathy, and non-proliferative diabetes retinopathy.
Stiff hands in long-term diabetes have been described for the first time by Lundbaek in 1957 [2]. There was little publication about the LJMS until 1974, when Rosenbloom, et al. [3] exhibited renewed interest in this syndrome. Joint stiffness and contractures were described as a common feature in children with type 1 diabetes mellitus.
The reported prevalence in diabetes mellitus apparently varies between 8%-58%, depending on the different diabetes patients' cohorts and the applied definitions of LJMS [4]. The prevalence of LJMS in subjects without DM is difficult to estimate and may vary between 4%-26% [5]. Generally, no clear gender or racial preferences have been found in the development of LJMS in diabetes.
Limited joint mobility occurs in both type 1 (insulin-dependent) and type 2 (non-insulin-dependent) diabetes [6]. The risk increases with increasing glycated hemoglobin (A1C) values [7] and the duration of diabetes [8]. The prevalence also increases with age and cigarette smoking [9].
Rosenbloom and associates in 1981, demonstrated a strong association between the increasing severity of joint limitation and the increased prevalence of microvascular disease in type 1 diabetes mellitus [10]. They reported a 3-fold risk of clinically apparent microvascular disease in patients with DCA. They concluded that limited joint mobility identifies a population that is, at increased risk for early onset microvasculopathy. Subsequent studies have supported this finding [11]. Our patient had evidence of nonproliferative retinopathy and nephropathy at the time when she presented with symptoms related to her hands.
As the presence of LJMS is associated with nephropathy, retinopathy and neuropathy, it is not only important to diagnose LJMS per se, but also because it can be an early warning signal of the possible presence of one or more of the microvascular complications. In some cases, it might be the first feature of tissue damage in diabetes which should alert physicians to actively screen or search for the presence of microvascular complications as well.
Besides a variable genetic susceptibility, high oxidative stress levels seem to be one of the factors involved. Intracellular hyperglycemia will cause high levels of oxidative stress and the formation of advanced glycation end products (AGEs). These AGEs are damaging glycosylation products, nonenzymatically formed under circumstances of hyperglycemic and oxidative stress. In such an unfavorable environment, increased production of reactive oxygen species will be induced that can initiate the inflammatory cascade leading to the production of several cytokines and growth factors causing the hyperglycemia-induced cellular damage [12]. Furthermore, besides their damaging effects on the vascular endothelium, these accelerated formatted AGEs also form cross-links with long-lived proteins such as skin collagen, tendons and ligaments altering their biological structure and function [13]. Collagen has a long half-life, which means that collagen degradation will take a long time: for more than ten years. Therefore, the AGE-cross links to collagen will extensively accumulate in the skin, tendons and ligaments and are considered to play an important role in the development of LJMS.
The diagnosis of diabetic LJMS is mainly clinical by eliciting positive “prayer” and “table top” signs. Sometimes LJMS occurs with other others musculoskeletal complications of diabetes in the hands, like Flexor tenosynovitis (trigger finger), Dupuytren's contracture, and carpal tunnel syndrome.
The sonography findings of diabetic cheiroarthropathy are thickening of the flexor tendon sheaths and subcutaneous tissues [14]. The Magnetic Resonance Imaging findings of diabetic cheiroarthropathy are thickening and enhancement of the flexor tendon sheaths. Other causes of tendon sheath inflammation include trauma, collagen vascular diseases, and infection [15].
LJMS seems to be an irreversible disorder with no specific curative treatment options. Only symptomatic therapy, such as analgesics, non-steroidal anti-inflammatory. Exercising, which include daily stretching exercises of the palm of the hands to prevent or further delay the development of progressive joint stiffness in case of limited joint mobility.
The most important approach like other diabetic complication is optimum glycemic control, to avoid or limit further disease progress. Correct diagnosis is important to avoid unnecessary medications for wrong diagnosis of LJMS as inflammatory connective tissue disease.
It is important for physicians to be aware of diabetic cherioarthrpathy, the diabetic limited joint mobility syndrome. Careful hands examination should be part of clinical examination for diabetic patients. Diagnosis of DCA is an indication for poor glycemic control and should prompt attention for other diabetic microvascular complications.
The Author has no conflict of interest.