Mucosa-associated lymphoid tissue lymphomas are a relatively recently recognized subset of B-cell non-Hodgkin's lymphomas. Generally, mucosa-associated lymphoid tissue lymphomas in the thyroid gland are known to have good prognosis, but recurrence and metastasis have also been reported.
A 70-year-old man visited our clinic with a 2-month history of a painless, rapidly growing mass in the neck associated with dysphagia. Left hemithyroidectomy was performed due to dysphagia. The histologic examination and immunohistochemistry showed an extranodal marginal B cell-type mucosa-associated lymphoid tissue lymphoma. He remains alive 57 months after the surgery.
If a diagnosis of a thyroid mass is unclear in a patient who exhibits symptoms of the neck, surgical treatment may be helpful for diagnosis and to relieve symptoms.
Primary thyroid lymphomas, Thyroidectomy, MALT lymphoma
PTL: Primary Thyroid Lymphomas; NHL: Non-Hodgkin's Lymphoma; MALT: Mucosa-Associated Lymphoid Tissue; CT: Computed Tomography; CD: Cluster of Differentiation
Primary thyroid lymphomas (PTLs) constitute up to 5% of all thyroid malignancies and can be divided into non-Hodgkin's lymphomas (NHLs) of B and T cell types and Hodgkin's lymphomas [1]. Most thyroid lymphomas are the B cell-type NHL, but the T cell-type and Hodgkin's lymphoma have also been reported. Usually, lymphomas are classified as low-, intermediate-, or high-grade, according to their clinical course or aggressiveness, and PTLs show various clinical courses [2]. Mucosa-associated lymphoid tissue (MALT) lymphomas are a relatively recently recognized subset of B cell-type NHL, and they are listed as extranodal marginal zone lymphomas according to the revised European-American lymphoma classification [3]. MALT lymphomas frequently occur in the mucosa of the gastrointestinal tract. However, they may also occur in the lungs, salivary glands, skin, and at other sites, including the thyroid gland [4]. MALT lymphomas do not commonly develop in healthy tissues and are thought to be caused by chronic inflammatory reactions or autoimmune diseases. In the thyroid gland, which is normally devoid of lymphocytic tissue, chronic autoimmune thyroiditis (Hashimoto's disease) has been associated with an increased risk of lymphoma, including MALT-type [4]. Therefore, it is difficult to diagnose MALT lymphomas based only on cytology or histology because medical conditions of the thyroid gland involve reactive and neoplastic processes in the thyroid gland. This has led to the use of immunohistochemistry, flow cytometry, and molecular techniques (Southern blotting, PCR) to confirm or exclude the diagnosis. In general, MALT lymphomas are known to have a better clinical course than other lymphomas [4]. We report a case of MALT lymphoma of the thyroid gland that was treated by surgery.
A 70-year-old man presented to our outpatient clinic with a 2-month history of a painless, rapidly growing mass in the neck that was associated with dysphagia. There was no significant family history. He had a previous history of hypertension and was taking aspirin after undergoing coronary artery angioplasty in 2008. His general physical examination appeared normal without any obvious deformities or abnormalities. Local examination revealed diffuse smooth swelling of the left lobe of the thyroid gland, which was firm in consistency.
Thyroid function blood tests revealed elevated serum thyrotropin (TSH = 31.79 mLU/mL; normal, 0.27 to 4.2 µLU/mL), normal serum triiodothyronine (T3 = 0.90 ng/mL; normal, 0.58 to 1.59 ng/mL), and normal serum free thyroxine (free T4 = 1.02 ng/dL; normal, 0.70 to 1.48 ng/dL) levels. The antithyroid peroxidase (anti-TPO) antibody titer was positive (> 1000 IU/mL), and TSH receptor antibody level was 0.17 IU/L (normal, 0-1.5 IU/L).
Ultrasound and computed tomography (CT) scans revealed a diffuse enlargement of the left lobe (6.1 × 4.2 cm in size) with no calcification (Figure 1a). Fine-needle aspiration cytology was suggestive of lymphocytic thyroiditis.
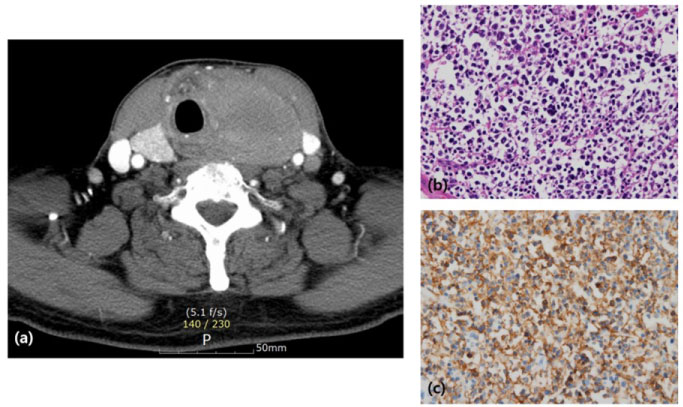 Figure 1: a) Diffuse, large mass of Lt. thyroid in computed tomography finding; b) Thyroid tissue was replaced by atypical lymphoid cells admixed with some thyroid glands, normal lymphocytes and irregular-shaped hyalinized fibrillar bands. (H&E stain, ×400); c) Atypical lymphoid cells were immunoreactive against CD20 (immunostaining, × 400).
View Figure 1
Figure 1: a) Diffuse, large mass of Lt. thyroid in computed tomography finding; b) Thyroid tissue was replaced by atypical lymphoid cells admixed with some thyroid glands, normal lymphocytes and irregular-shaped hyalinized fibrillar bands. (H&E stain, ×400); c) Atypical lymphoid cells were immunoreactive against CD20 (immunostaining, × 400).
View Figure 1
The patient underwent a left hemithyroidectomy because of dysphagia. The histologic examination and immunohistochemistry showed an extranodal marginal B cell-type MALT lymphoma. Thyroid tissue was replaced by atypical lymphoid cells admixed with some thyroid cells; normal lymphocytes; and irregular-shaped, hyalinized, fibrillar bands (Figure 1b). MALT lymphomas express B cell-associated antigens (cluster of differentiation (CD20, CD22, and CD79a) and are negative for CD5, CD10, and CD3 [5]. In this case, all the colonizing neoplastic B cells tested positive for CD20 (Figure 1c). The patient remains alive 57 months without any other treatment after the surgery.
Mucosa-associated lymphoid tissue usually protects the gastrointestinal mucosa or respiratory epithelia from damage by potential antigens. The local immune response caused by the systemic immune response associated with an inflammatory response can cause problems in weak gastrointestinal mucosa or respiratory epithelia. For this reason, a systemic immune abnormality can spread to other mucosal surfaces. Sensitized T and B lymphocytes are transported through the efferent lymphatics to all the mucosal surfaces of the body.
NHLs may involve the thyroid gland as part of systemic lymphoma or may arise primarily in the thyroid gland. The most common histological subtype is diffuse large B-cell lymphoma. About 3% of NHLs are thyroid lymphomas. The incidence of malignant lymphomas in the thyroid gland is 5% [1,2].
The clinical feature of thyroid lymphomas is rapid, non-tender enlargement of the thyroid gland, accompanied by compressive symptoms in about 30% of them, like hoarseness, dysphagia, or dyspnea. Most primary thyroid lymphomas, including MALT lymphomas, are observed in elderly individuals, with a peak incidence in the seventh decade, and the female/male ratio varies from 3:1 to 4:1 [6].
Since the concept of MALT lymphomas was described by Isaacson and Wright [7], various locations have been described.
Recently, low-grade B-cell MALT lymphomas are a recognized distinct morphological and clinical subtype of low-grade B-cell lymphomas.
Histologically, MALT lymphomas of the thyroid gland are showed by the presence of atypical lymphoid cells, which derived from the marginal zone of the lymphoid follicles and can extend into the interfollicular space and/or into the germinal centers (follicular colonization) [8]. The thyroid gland contains no native lymphoid tissue. Intrathyroidal lymphoid tissue is accrued in various pathological conditions, but more evidently during autoimmune thyroid disease, notably chronic autoimmune thyroiditis (Hashimoto's thyroiditis). Histologically, this acquired lymphoid tissue can evolve to lymphoma, including the MALT type [9]. In our case, when the patient visited the hospital with a mass rapidly growing in the neck, fine-needle aspiration cytology was performed, and the test result at that time was also suggestive of lymphocytic thyroiditis, so the patient's was suspected to have Hashimoto's thyroiditis. However, the neck mass did not respond to medications, and thyroidectomy was performed because of the development of severe compressive symptoms, such as dysphagia. There is no consensus regarding the optimal therapy and follow-up for patients with MALT lymphomas of the thyroid gland [1,2]. PTLs are preferred for combined therapy (chemotherapy and radiotherapy). However, in some cases of MALT lymphoma, surgical treatment alone may also be effective [10]. Usually, surgery is performed for pressure-associated symptoms or when the diagnosis is in doubt, as was the case herein where fine-needle aspiration cytology findings were not conclusive. The usual treatment is radiotherapy for localized disease and chemotherapy for disseminated disease, and recurrence can be treated with either radiotherapy alone or with a combination of radiotherapy and chemotherapy.
MALT lymphomas are slow-growing lymphomas, and previous studies have also shown that MALT lymphomas of the thyroid gland generally confer a good prognosis [1-3]. However, they can recur at any other mucosal surfaces; thus, guidelines for long-term follow-up (e.g. abdominal ultrasound, neck CT, bone marrow biopsy, stomach endoscopy, and colonoscopy) are needed for the treatment of this disease.
In conclusion, low-grade NHLs of MALT-type of the thyroid gland arises in the setting of chronic autoimmune thyroiditis. They could be treated by non-invasive methods, such as chemotherapy or radiotherapy, but exact diagnosis is difficult.
In cases of symptomatic thyroid MALT lymphoma, surgery could play multiple roles in diagnosis, symptom relief, and treatment of the disease.
Written informed consent was obtained from the patient for publication of this Case report and any accompanying images.
Approval was granted by the Institutional Review Board of Pusan National University Yangsan Hospital (IRB file No. 05-2017-107). Patient records and information were anonymized to protect the personal information.
None.
The authors have no conflict of interest to declare.
Investigation: Hyun Yul Kim; Resources: Jeong Hee Lee; Writing - original draft: Dong-il Kim, Hyun-june Paik; Writing - review & editing: Dong-il Kim, Youn Joo Jung.