Laparoscopic cholecystectomy is guided by working knowledge of bilio-vascular anomalies to prevent common bile duct injuries and bleeding during surgery. Less importance is given to the dissection of the gall bladder from the gall bladder bed where the middle hepatic vein or its large branch can be encountered. The lack of awareness of this presence can result in uncontrolled bleeding and result in significant morbidity or mortality in a seemingly uneventful procedure. It is important to educate all surgeons performing this procedure about the possibility of encountering this vein in a very simple step of the surgery as we did in our case and be wary of its eminent danger.
Middle hepatic vein, Laparoscopic cholecystectomy, Uncontrolled bleeding, Gall bladder bed, Doppler venous ultrasound
Laparoscopic cholecystectomy is one of the most commonly performed surgery in the world. Safety of the procedure is mainly directed towards preventing biliary tract injuries and major vascular injuries [1,2]. Dissecting the gall bladder off the gall bladder bed on the liver is usually uneventful and only met with occasional liver bed oozing which is controlled by compression or cautery. Through our case report we would like to bring into notice the middle hepatic vein which can lie either in close proximity to the gall bladder bed or even as in our case completely exposed allowing a chance of catastrophic injury and bleeding during an seemingly easy cholecystectomy.
A 36-year-old female patient was selected for laparoscopic cholecystectomy for symptomatic cholelithiasis. She had no evidence of cholecystitis or any history suggesting hepato-biliary infection or disease in the past. She had delivered a healthy baby 6 months ago and had no peripartum complications.
Intraoperatively, the liver was found to be normal in size and with no evidence of cirrhosis or scarring. The gall bladder was seen to be normal in appearance with no evidence of adhesions or cholecystitis. The surgery proceeded with dissection of the Calot's triangle to skeletonize, clip and cut the cystic artery and duct. Once the artery and duct were separated from the gall bladder the gall bladder was dissected off the gall bladder bed. Minor ooze encountered during the release of peritoneal reflections over gall bladder encouraged caution in dissecting the gall bladder (Figure 1). An exposed large middle hepatic vein was seen underneath the gall bladder on the gall bladder bed. The vein was intact with no injury and had venous pulsations to guide identification (Figure 2). The gall bladder was dissected with extreme care to avoid any handling or injury to the vein and once gall bladder was dissected free the gall bladder bed was packed with AB GEL to prevent venous blowout or injury.
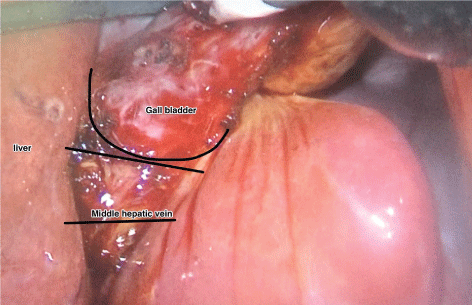 Figure 1: Gall bladder over the exposed middle hepatic vein in the gall bladder bed. View Figure 1
Figure 1: Gall bladder over the exposed middle hepatic vein in the gall bladder bed. View Figure 1
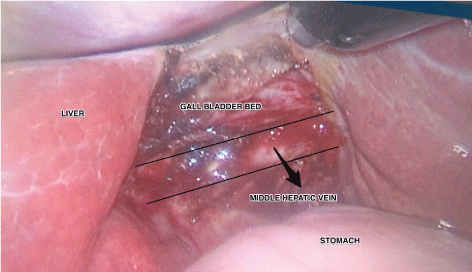 Figure 2: Exposed middle hepatic vein in gall bladder bed after removal of gall bladder. View Figure 2
Figure 2: Exposed middle hepatic vein in gall bladder bed after removal of gall bladder. View Figure 2
Patient was observed for 24 hours and discharged on second postoperative day after tolerating diet. A doppler venous study was done postoperatively to confirm the middle hepatic vein anatomy and its relation to the gall bladder bed (Figure 3). Patient was symptom free with no complaints or complications on post-operative visit.
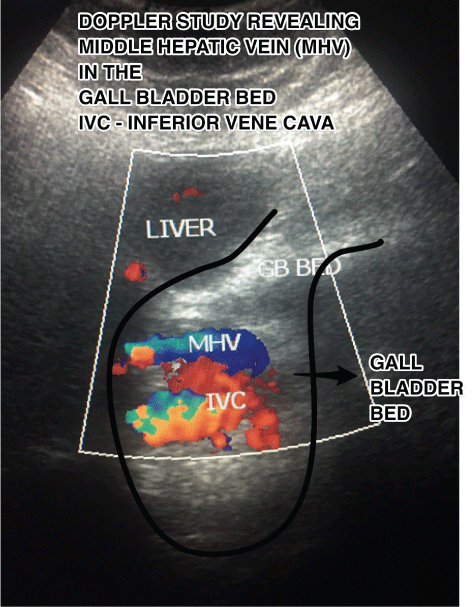 Figure 3: Doppler study revealing middle hepatic vein in gall bladder bed. View Figure 3
Figure 3: Doppler study revealing middle hepatic vein in gall bladder bed. View Figure 3
The gall bladder and the bilio-vascular structures surrounding it are known to exhibit variations of all forms and types [1]. This fact is highlighted in all forums of teaching and training for laparoscopy for gall bladder surgery to avoid bilio-vascular injuries which can be morbid and even catastrophic [2]. Once the Calot's triangle is safely dissected the artery and duct are identified, clipped and cut. This step is followed by dissection of the gall bladder from the gall bladder bed on the liver. Many surgeons usually proceed without caution in this region and only encounter mild oozing from liver bed which is effectively controlled by cautery or compression.
Recent understanding of the liver anatomy brings into light the presence of the middle hepatic vein in close proximity to the gall bladder bed [3,4]. The middle hepatic vein or its major branch may be adhered to the gall bladder bed especially near the right side of the longitudinal axis of the gall bladder [5]. The mean distance from the middle hepatic vein or its largest branch to the gall bladder has been seen to be around 1 to 1.7 mm approximately [3,6,7]. Thus, the liver tissue overlying the vein may be sometimes negligible [3-6]. Though not always encountered in dissection the gall bladder from the liver bed, still a working knowledge of its presence in close proximity would guide surgeons to proceed in caution and prevent its injury and catastrophic bleeding in any suspicious presentation if any.
There have been even studies which highlight the importance of Doppler venous ultrasound of the hepatic veins and its major branches prior to a laparoscopic cholecystectomy to allow better understanding of this anatomic presence [3,4,6-8]. Evidence from autopsy in cases of mortality from bilio-vascular injury also highlights the middle hepatic vein as a cause many cases. Approximately 0.1% to 2.0% cases have uncontrolled bleeding during laparoscopic cholecystectomy and around 80% of them are from the gall bladder bed. Bleeding from the middle hepatic vein may result in cases where the vein is directly exposed or adhered to the gall bladder bed which is around 10% of cases [5].
Chronically scarred or contracted gall bladder during surgery or even cirrhotic livers predispose of this situation in much prominence and thus allowing more chances of bleeding and the following sequelae [5,9].
All the said detail does make it evident that the middle hepatic vein or its major branch can very well be present in extreme proximity of the gall bladder bed and any untoward injury should be anticipated especially in diseased conditions of the gall bladder and liver. In present day day-care safe surgery scenario, it is of prime importance to highlight all possible vital structures a surgeon can encounter to allow smooth execution of the surgery and uneventful recovery of the patient.
The middle hepatic vein can be encountered either completely exposed or in very close proximity to the gall bladder bed during laparoscopic cholecystectomy. Its anatomic knowledge should caution surgeons performing laparoscopic cholecystectomy especially during the dissection of the gall bladder from its bed. Just caution at the Calot's triangle would be insufficient and this added knowledge should be incorporated in all surgeons' knowledge for performing safe laparoscopic cholecystectomy.