Acute pulmonary embolism (APE) or acute aortic dissection is one of the most serious clinical presentations at emergency department. Chest pain and elevated serum D-dimer level can be found in both APE and AAD. Echocardiography can be used as first line imaging modality for differential diagnosis. Computed tomography angiography is the main diagnostic test for APE and AAD. We aimed to emphasize differential diagnosis of chest pain with this case report.
Aortic dissection, Pulmonary embolism, D-dimer
An elderly man aged 82 years who had hypertension for 22 years was admitted to the emergency department with severe chest and back pain. According to information gained from the patient, he has used regularly hypertension medical (perindopril + indapamide 4/1.25 mg) and he had no history of other chronic disease (cardiac disease, kidney disease, diabetes mellitus or connective tissue disorder), operations, or hospitalization. When he arrived at the hospital, his blood pressure was 140/70 mmHg, heart beat was 72 beats per minute, electrocardiography was normal, and D-dimer was high (1390 ng/mL). The patient was referred to our hospital with a diagnosis of pulmonary embolism. Transthorasic echocardiography (TTE) showed that the diameter of ascending aorta was nearly 10.3 cm (Figure 1) and, in the apical four chamber view decending aorta had dissection with true and false lumen (Figure 2). TTE revealed that his ejection fraction was 60% (used modified Simpson calculation), and there was minimal regurgitation of the aortic valve. Thoracal computed tomography angiography (CTA) showed type B aortic dissection (Figure 3). There was a aortic aneurysm that started from aortic valve and including the ascending aorta and there was a aortic dissection with clearly visible true and false lumen on the decending aorta. The diameter of ascending aorta was 92.9 mm on CTA. IV esmolol and sodium nitroprussid infusion was initiated and the patient was consulted with cardiovascular surgeon. Due to unwillingness of the patient’s relatives and no malperfusion, thoracic endovascular aortic repair (TEVAR) or any surgical procedure was not performed.
 Figure 1: Parasternal long axis echocardiographic view of dilated ascending aorta. View Figure 1
Figure 1: Parasternal long axis echocardiographic view of dilated ascending aorta. View Figure 1
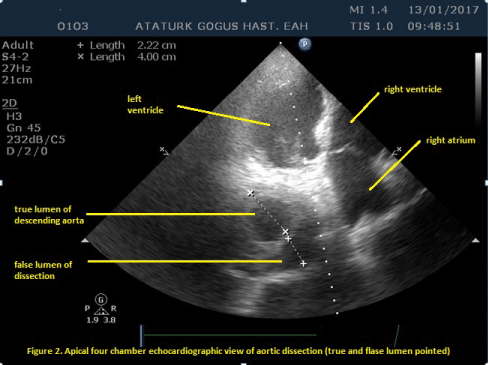 Figure 2: Apical four chamber echocardiographic view of aortic dissection (true and false lumen pointed). View Figure 2
Figure 2: Apical four chamber echocardiographic view of aortic dissection (true and false lumen pointed). View Figure 2
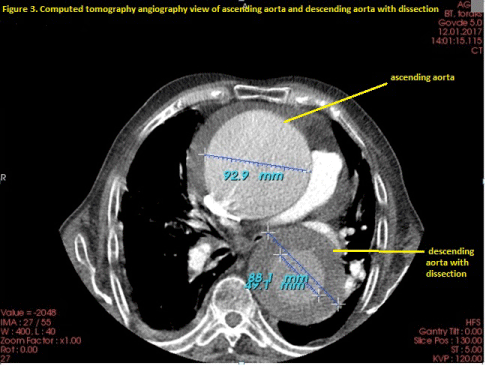 Figure 3: Computed tomography angiography view of ascending aorta and descending aorta with dissection. View Figure 3
Figure 3: Computed tomography angiography view of ascending aorta and descending aorta with dissection. View Figure 3
Acute pulmonary embolism (APE) is one of the most serious clinical presentations at emergency department associated with significant short- and long-term complications, and a mortality rate of 15-20% [1]. Suspected APE with shock or hypotension is a life-threading clinical problem and the differential diagnosis includes acute coronary syndrome (ACS), aortic dissection, tamponade or acute valvular dysfunction. The most useful initial test in this situation is transthorasic echocardiography [2]. Suspected APE without shock or hypotension, computed tomographic angiography (CTA) is the main thoracic imaging test but in the emergency department, plasma D-dimer measurement is the first diagnostic step and a normal D-dimer level allows to be ruled out APE diagnosis in around 30% of patients [3]. D-dimer levels are elevated in plasma with acute thrombosis as a result of coagulation and fibrinolysis.
Aneurysm is the second most frequent disease of the aorta after atherosclerosis. Patients with thorasic aorta aneurysm are most often asymptomatic and the diagnosis is made incidentally with other investigative reasons or screening purposes. Surgical decision is based mainly on aortic diameter. Surgery should be performed in patients with Marfan syndrome, who have a maximal aortic diameter ≥ 50 mm [4]. With the diameter is 45 mm, surgical decision can be considered in patients with additional risk factors, including family history of dissection, size increase 0.3 mm/year (in repeated examinations using the same technique and confirmed by another technique), severe aortic regurgitation, or desire for pregnancy [5].
Aortic dissection is defined as separation of the aortic wall layers and subsequent formation of a true lumen and a false lumen with or without communication. Generally, a tear in the intimal layer is the starting condition, results as a new track for the blood and the blood enters the intima-media space (false lumen). Aortic dissection classified Type A (dissection includes asendan aorta) and Type B (dissection includes decendan aorta-distal from left subclavian artery) [6]. For the Type A dissection, surgery is the only treatment choice. Acute Type A dissection has a mortality of 50% within the first 48 hours if not operated. Patients with uncomplicated (especially not caused malperfusion for visseral organs). Type B dissection must receive medical therapy to control pain, heart rate, and blood pressure. Thoracic endovascular aortic repair (TEVAR) is a treatment choice, aims stabilization of the dissected aorta [7]. The proximal intimal tear is obliterated by implantation of TEVAR, blood flow is redirected to the true lumen. TEVAR is the treatment of choice in complicated acute Type B dissection [7].