Infected (mycotic) aneurysms (MA) are uncommon, and the aorta is the main vessel involved, with gram-positive bacteria being the most frequent causative agent. Their morbidity and mortality are important and an early diagnosis is challenging owing to their unspecified manifestations.
A 72-year-old female was admitted with sepsis and back pain. She was diabetic, had peripheral vascular disease and chronic renal failure undergoing dialysis. A methicillin-sensitive Staphylococcus aureus bacteremia was documented, and Computed Tomography (CT) scan revealed a pseudoaneurysm of the abdominal aorta, and a periaortic lesion suggestive of MA. Taking into account the patient's comorbidities and the location of the lesion, a more conservative approach was adopted, with antibiotic treatment only. The patient responded well, with clinical improvement and reduced inflammatory markers.
This case illustrates the difficult process of diagnosing a MA, often characterized by frequent and non-specific symptoms. It also highlights the fact that older people with chronic diseases are a main target population due to atherosclerosis, immunosuppression and multiple vascular punctures. Imaging features on CT scan include a lobulated vascular mass and a perianeurysmal inflammatory mass, resembling a mushroom. Familiarity with the imaging appearances of infected aneurysms is essential for an early diagnosis and adequate treatment.
Mycotic aneurysm, Aorta, Bacteremia, Staphylococcus
Infected/mycotic aneurysms (MA) correspond to an infection of the arterial wall with formation of saccular structures adjacent to the arterial lumen [1,2]. Its true prevalence is unknown, but it is a rare entity, corresponding to 1-4% of all aneurysms [1,2].
In about 50-80% of all cases, an etiologic agent is identified [3,4]. Streptococcus and Staphylococcus species are the microorganisms with most affinity for the vascular wall and are responsible for 28-71% of all MA [4]. When identified, gram-negative microorganisms may be involved in up to 50% of all cases, with Salmonella species being the most common microorganism of this group [1,3].
The initial presentation may include a wide spectrum of clinical manifestations and severity, ranging between a fever of unknown origin and a series of catastrophic events including septic or haemorrhagic shock [3,4]. In fact, the initial diagnosis is often a challenge because of the non-specific character of most of these symptoms, which may delay the final diagnosis, and worsen the outcome [1,2,4].
A 72-year-old female with multiple cardiovascular risk factors (hypertension, obesity, diabetes), peripheral artery disease (with amputation of both lower limbs), and chronic kidney disease on haemodialysis through an arteriovenous fistula, presented with a 2-month history of increasing low back pain radiating to the right abdominal quadrants. These complaints motivated a very recent in-hospital evaluation, with no defined aetiology after an extensive study. She also had multiple hospital admissions in the previous 6 months due to recurrent bacteraemia caused by different microorganisms. On admission, fever and increased inflammatory markers were documented (C-Reactive Protein 155 mg/L; 12400 leucocytes/µL), with hemodynamic stability (blood pressure 148/62 mmHg; heart rate 89 bpm) and no evidence of organ failure. She had diffuse abdominal discomfort on physical examination, with no signs of peritoneal irritation. There was no evident source of infection on the initial study. Empirical therapy was started with broad-spectrum antibiotic, de-escalated to ceftriaxone 2 gr after identification of methicillin-sensitive Staphylococcus aureus (MSSA) in blood cultures. Despite the directed antibiotic treatment, the clinical and analytic responses were slow. Study with transthoracic and transesophageal echocardiogram excluded endocarditis. A lumbosacral spine MRI and thoracoabdominopelvic CT were performed, with no evidence of spondylodiscitis, but showing a periaortic lesion with 60 × 50 × 40 mm, posterior to the crura of the diaphragm, extending from the thoracoabdominal aortic transition down to the origin of the superior mesenteric artery. A 12 mm pseudoaneurysm was also noted, with imaging pattern suggestive of a MA (Figure 1 and Figure 2).
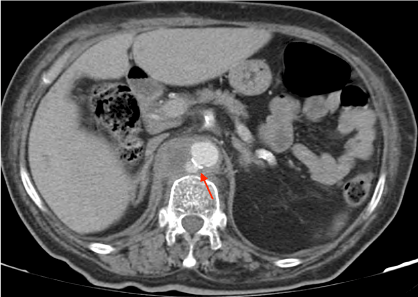 Figure 1: Mycotic Aneurysm (CT scan with intravenous contrast).
View Figure 1
Figure 1: Mycotic Aneurysm (CT scan with intravenous contrast).
View Figure 1
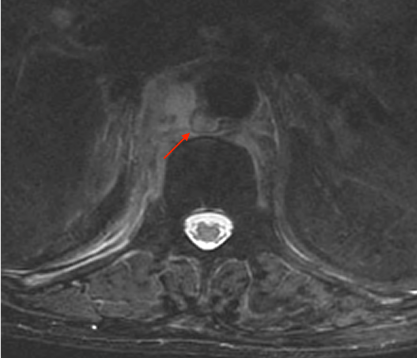 Figure 2: Mycotic Aneurysm (MRI, T2-weighted image).
View Figure 2
Figure 2: Mycotic Aneurysm (MRI, T2-weighted image).
View Figure 2
After reviewing the case with vascular surgeons, a conservative approach was defined because of the extremely high risk associated with a conventional procedure in this patient, and the localization of the aneurysm, which limited an endovascular procedure.
Long-term antibiotic therapy with intravenous cephalosporin was maintained, with definitive duration to be defined according to the patient's response over time. In the meantime she became asymptomatic and the inflammatory syndrome resolved, allowing hospital discharge.
MA are infrequent but they can virtually involve any arterial territory [1-4]. The aorta is the predominantly affected artery followed by extremities, cerebral and splanchnic circulations, often at points of vessel bifurcartion [4]. Risk factors for infected aneurysm include trauma, endocarditis, impaired immunity and advanced age.
The clinical manifestations depend upon the site of the aneurysm. Its typical presentation includes an important systemic inflammatory response with fever and increased inflammatory markers, associated with a painful and pulsatile mass with growing dimensions [3]. However, this scenario is often limited to the situations where the vessels involved are peripheral arteries, easier to access during physical examination. In the presented case, in an obese patient with involvement of the abdominal aorta, the only symptom described was pain, with no sign suggestive of an aneurysm. In fact, a retrospective study from Huang YK, et al. showed that the most frequent manifestations of aortic aneurysms included fever and pain referred to the abdomen (84.1%) or back (70.4%) [5].
- Dissemination of septic emboli that occlude the vasa vasorum of the vessel or the vessel lumen itself, leading to vascular wall infection;
- Infection of a previous intimal injury/pre-existing aneurysm/atherosclerotic plaque by a circulating microorganism;
- Involvement of the vessel by contiguous infection;
- Direct bacterial inoculation at the time of vascular injury [1-3].
In contrast to what happened in the pre-antibiotic era, when the majority of MA was a consequence of infectious endocarditis, nowadays the high risk populations include intravenous drug users, immunosuppressed patients (with diabetes, neoplasms or other chronic diseases), and the ones submitted to endovascular procedures [1-3]. According to this, in a retrospective study that included 44 patients, the most frequent comorbidities were hypertension (86.4%), diabetes (54.6%), cerebrovascular disease (30.5%), chronic kidney disease (18.2%) and peripheral artery disease (11.4%) [5].
In fact, this patient had multiple risk factors for the development of infected aneurysms - she was already at an advanced age, with very important atherosclerotic disease and several other comorbidities that led to some degree of immunosuppression (diabetes, chronic kidney disease). Furthermore, there were multiple recent episodes of bacteraemia, with the arteriovenous fistula used for haemodialysis being a potential portal of entry for infections.
Similar to this case caused by a MSSA, MA most frequently involve gram-positive bacteria, but they may also correspond to a severe and rare complication of salmonellosis [1,2,4]. Other gram-negative bacteria and fungi are also potential causative microorganisms, although not very common and usually involved in cases of intravenous drug abuse and severe immunosuppression [2,3].
Angio-CT is currently the gold standard in the evaluation of patients with suspected MA. Conventional angiography is still one of the best techniques in the diagnosis of this entity but it is an invasive procedure and does not allow evaluation of potential extravascular disease [1,3]. Typical imaging findings include an eccentric saccular aneurysm with an irregular arterial wall, severe oedema and a surrounding inflammatory mass as in this case [1,3].
Treatment of MA requires a multidisciplinary approach and must be adjusted to the patient and the characteristics of the aneurysm itself (localization, morphology, presence and extension of hematoma). There are no randomized trials to guide the management of infected aneurysms. Management strategies are primarily based upon clinical experience guided by case series. They may include open surgery, endovascular procedures (stent versus embolization), medical treatment or a combination of these options [1-3]. Small aneurysms with no evidence of rupture and no associated symptoms are usually managed with a more conservative approach with long-term parenteral antibiotic therapy. In the remaining cases, particularly when there is evidence of a growing aneurysm, the initial approach may include surgery. Recent endovascular techniques are a potential alternative to the conventional surgical approach associated with a 40% mortality rate [2], but there is still a lot of controversies concerning the placement of an endovascular prosthesis in a contaminated environment [1,2].
In the case of this particular patient, because of all the comorbidities, the risk of a mandatorily extensive surgery for vascular reconstruction was considered extremely elevated. Furthermore, the localization of the aneurysm near great splanchnic vessels limited an endovascular approach. As a result, the treatment strategy was conservative, involving directed antibiotic therapy with parenteral cephalosporin for an undetermined period of time.
The ideal duration of antibiotic therapy for MA is unknown, and depends on multiple factors: The immunologic status of the patient, localization of the infection, causative microorganism, response to treatment and potential surgical/endovascular approach [2,3]. In fact, most authors recommend a treatment of at least 6 weeks, and some of them suggest a lifelong antimicrobial therapy, depending on the previously described factors. Some studies also recommend the parenteral administration of two antibiotics with synergistic activity, particularly when the infection is caused by gram-negative bacteria, because of its invasive potential that worsens the prognosis [2]. In this patient, monotherapy with ceftriaxone was considered the best treatment option, maintained after hospital discharge.
Most MA have poor prognosis, with increased mortality due to haemorrhagic or infectious complications - according to a retrospective study, about 75% of the patients managed with a conservative strategy died in the first three years after diagnosis [5].
The elevated suspicion index and recognition of the typical imaging characteristics of a MA are therefore essential for an early diagnosis and treatment, improving the outcome of this patients, even when surgical treatment is not an option, similar to this case report.
This case illustrates the challenging process of diagnosing an aortic MA, often presenting with common and unspecified symptoms. It also highlights that older patients with chronic diseases are the main targets for an infected aneurysm: Atherosclerosis, repeated venous punctures and immunosuppression.
- Diagnosing a MA can be a very challenging process, due to its common and non-specific manifestations.
- Older patients with chronic diseases are particularly at risk for an infected aneurysm: Atherosclerosis, repeated venous punctures, and immunosuppression.
- Familiarity with the imaging appearances of infected aneurysms is essential for an early diagnosis and adequate treatment.
The authors declare no conflict of interests.
There were no external financing sources used in this work.