Extramammary Paget's disease (EMPD) is a rare intraepithelial cancer. It is more common in women and usually develops in apocrine gland-bearing areas, Less frequenly, EMPD can affect males in the anogenital area. EMPD may present with a focal, multifocal, or an ectopic lesion. We report a case of a 56-year-old male with extra-mammary Paget's disease.
Extramammary paget disease, Inguinal paget disease, Anogenital, Paget disease
EMPD represents just 6.5% of all Paget's disease and occurs mainly among in Caucasian women and Asian men in their 60s and 70s. It is a rare neoplasm; the exact incidence is unknown [1]. Approximately 25% of all EMPD cases are associated with an underlying malignancy. The lesion is often present for years before a diagnosis rendered [2].
Here, we describe the clinical case of a 56-year-old man with a three-year history of a painless erythematous lesion on the inguinal region He underwent a punch biopsy and the pathology report came back as EMPD. Surgical excision was carried out.
A 56-year-old man was referred to our departement with a three-year history of a pruritic, painless erythematous chronic skin rash on the right emi-scrotum and inguinal region. The skin lesion had failed treatment with topical corticosteroid and antifungal ointment.
Local examination revealed an erythematous plaque extending over the base of the penis and 2 cm round peripheral rim onto the scrotum. The involved area contained whitish superficial exudates, and was scaly (Figure 1). No inguinal lymph nodes were evidenced by physical examination.
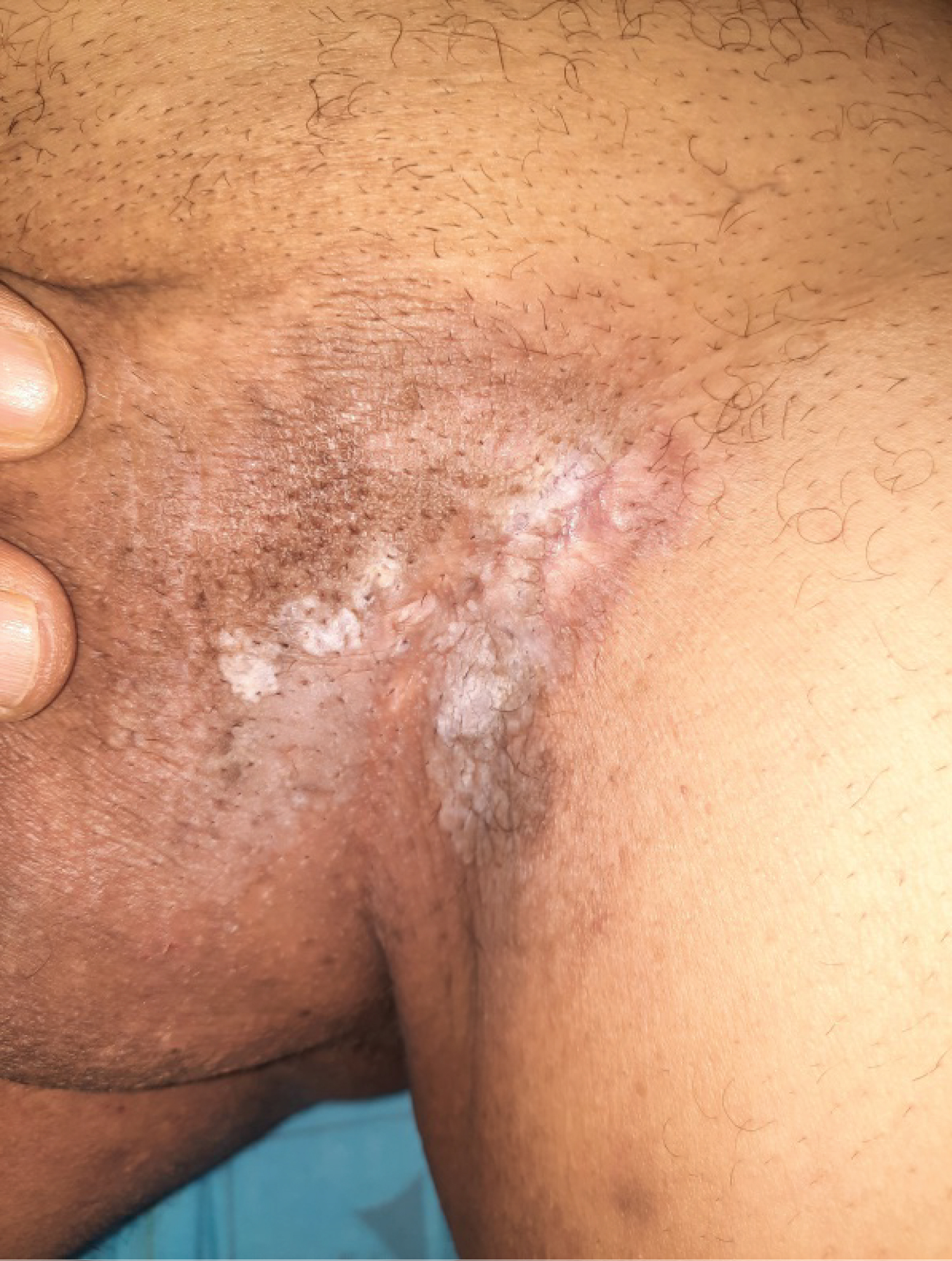 Figure 1: An eczematous, indurated patchy area on the left side of the inguinal region.
View Figure 1
Figure 1: An eczematous, indurated patchy area on the left side of the inguinal region.
View Figure 1
A survey of internal malignancy, including chest X-ray, ultrasound, and computerized tomography (CT) of the abdomen, were negative.
The patient underwent a punch biopsy and the pathology report came back as EMPD. Surgical excision was performed with a margin of 3 cm. No local recurrence or other malignancy has been found during one year of follow-up.
Paget's disease was firest described by sir James Paget in 1874. Later Radcliffe Crocker described extra-mammary Paget's disease (EMPD) in 1889, in a patient with urinary bladder carcinoma, who presented an eczematous lesion on the penis and scrotum. While the perianal location of EMPD was described by Darier and Coulillaud in 1893. The prevalence of EMPD regarding gender differs between Western and Asian populations. In studies of Caucasian populations, EMPD has a female predominance, with male-to-female ratios ranging from 1:2 to 1:7. In contrast, male predominance has been reported in Asian studies [3].
The pathogenesis of primary EMPD is not well understood. Primary intraepidermal EMPD may arise from pluripotent cells in the epidermis and/or adnexae. The condition may be derived from Toker cells, which are mammary gland-related cells found in the nipple and vulva. "Secondary" EMPD is generally accepted to be due to direct extension of an adjacent malignancy or in cases where an occult underlying malignancy is identified [4,5].
EMPD skin lesions typically present as a well-circumscribed erythema or erythematous plaques with occasional hyperpigmentation or hypopigmentation. Cases in which the main clinical presentation was hypopigmentation have also been reported. Crust, scale, or erosion on the erythematous lesions may also be seen, and such lesions may mimic various other skin disorders, such as eczema, psoriasis, lichen sclerosus, contact dermatitis and fungal infection, leading to delays in treatment of up to many years [4,5].
Dermoscopic features of EMPD lesions include milkyred areas, dotted vessels, glomerular vessels, polymorphous vessels, surface scales, linear irregular vessels and lava lake structure [4,5].
The diagnosis of EMPD is established by skin biopsy, which reveals the presence of Paget cells in the epidermis, which are characterized by atypical large cells with abundant, clear, and sometimes eosinophilic cytoplasm in hematoxylin and eosin staining [3,6]. The cells are present singly or form clusters; the tumor cells may crush the basal layer. Paget's cells are usually positive for low molecular-weight cytokeratins and epithelial membrane antigen. Gross cystic disease fluid protein-15 is typically positive in primary EMPD and negative in secondary.
Current treatment for EMPD is surgical excision and Mohs' micrographic surgery. In cases where surgery cannot be applied several alternative nonsurgical treatments, like radiotherapy, topical imuquimod (IMQ) cream, and photodynamic therapy (PDT), can be selected [7].
EMPD is a rare intraepithelial adenocarcinoma with limited cases reported in the literature. Early biopsy and histological examination are important to establish a correct diagnosis for an early surgical intervention of the lesions.
None of the authors has a conflict of interest to declare.