HPV infections are caused by human papillomaviruses. These viruses create cutaneous or mucous membrane tumors, including some warts. Warts are extremely common and easy to recognize, but when the location is atypical, histological confirmation is required. We report a HPV infection case localized in the ear's external auditory canal in a 30-year-old young that is admitted to the ENT department of the Ziguinchor Peace Hospital. The examination found: auricular pruritus, a full ear feeling and a mass of the right ear's external auditory canal, evolving for about 3 months. Histological examination confirms the papilloma by showing a specific cytopathogenic effect in keratinocytes (koilocytes). Our patient underwent surgical resection of the mass with no relapse after 3 months.
Wart, External auditory canal, HPV, Ziguinchor
Warts are generally defined as benign infectious epitheliomas of the cutaneous and mucous membranes [1]. Some warts are the clinical expression of human papillomavirus (HPV) infection [1,2]. On the skin, the virus develops in the epidermis and causes abnormal proliferation of cells [3]. The exact prevalence of carriers of warts is not known, but it is estimated at around 7 to 10% in the general population, which has increased significantly over the past two or three decades, [2,4]. Children of school age and young adults are the most affected, with a peak incidence between 9 and 15 years [5]. Each type of papillomavirus has a particular tropism. Thus, most HPVs can be classified into skin tropism virus and mucosal tropism virus [5]. Transmission likely occurs from skin to skin or through contaminated surfaces.
Small erosions and microtraumas can allow the virus to enter the skin, or from another individual or by self-inoculation [5]. Little is known about the incubation period, estimated to range from a few weeks to over 1 year [6]. The ear region is anatomically complex and can be the site (or the starting point) of various pathologies. The outer ear is formed by the pinna, made up of an elastic cartilaginous framework covered with skin and having different reliefs and the external auditory canal, lined with a cutaneous covering. The wart may develop there, but this location is rare and very uncharacteristic. It requires a precise pathological diagnosis [3,4]. We report a rare case of an outer ear wart whose histology was in favor of a papilloma of the external auditory canal.
It was about a 30-year-old patient, a construction worker, in whom a notion of manipulation of the ear by the use of cotton swabs was found. He lived in the town of Sédhiou located 116 km from Ziguinchor. He was consulted in the ENT department of the Ziguinchor peace hospital for: An atrial pruritus, a feeling of full ear, no notion of hypoacusia and a mass of the right ear's external auditory canal (EAC), evolving since about 3 months. The appearance of this mass in the right ear was spontaneous and gradually increased in size (Figure 1).
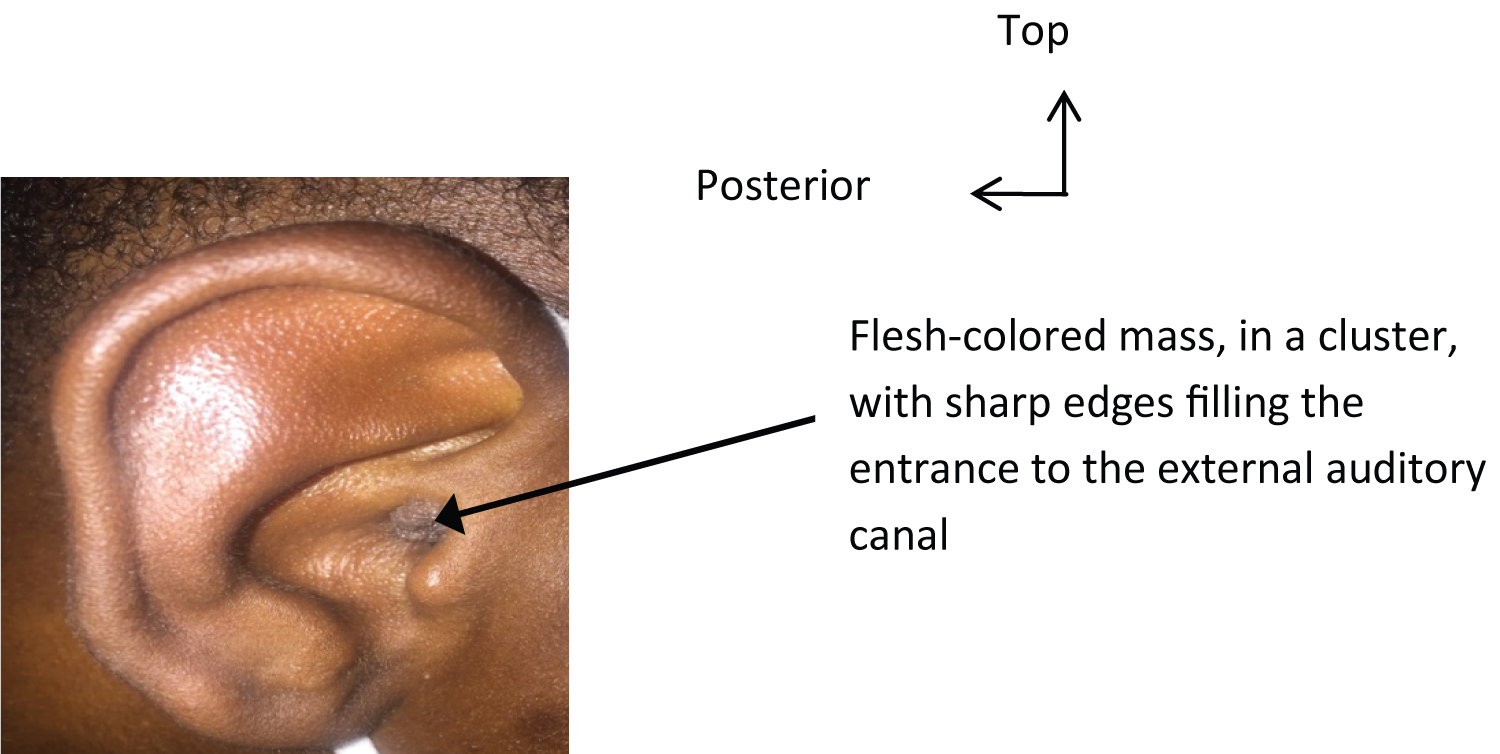 Figure 1: The external auditory canal wart.
View Figure 1
Figure 1: The external auditory canal wart.
View Figure 1
A notion of self-medication based on an antibacterial ointment, and an antibiotic of an unspecified nature by general route was found. This treatment was without improvement. Clinically, the otological examination objected to the right, a flesh-colored outgrowth, with a clear border, grouped in clusters, developed at the expense of the skin of the EAC, painless, filling the entrance to the EAC at its lateral wall. It measured about 4 mm long axis. The contralateral ear was normal and the remainder of the ENT examination was unremarkable. No other localization was found in this patient. Our patient had not benefited from a virological assessment because it was not available. A biopsy of the mass was taken and sent for histological analysis. The anatomopathological study found a keratinized squamous epithelium, papillomatous, thickened, hyperplastic, ortokeratotic, site of high-grade dysplasia with koilocytic cytopathy (Figure 2 and Figure 3). The diagnosis of papilloma of the external auditory canal was accepted.
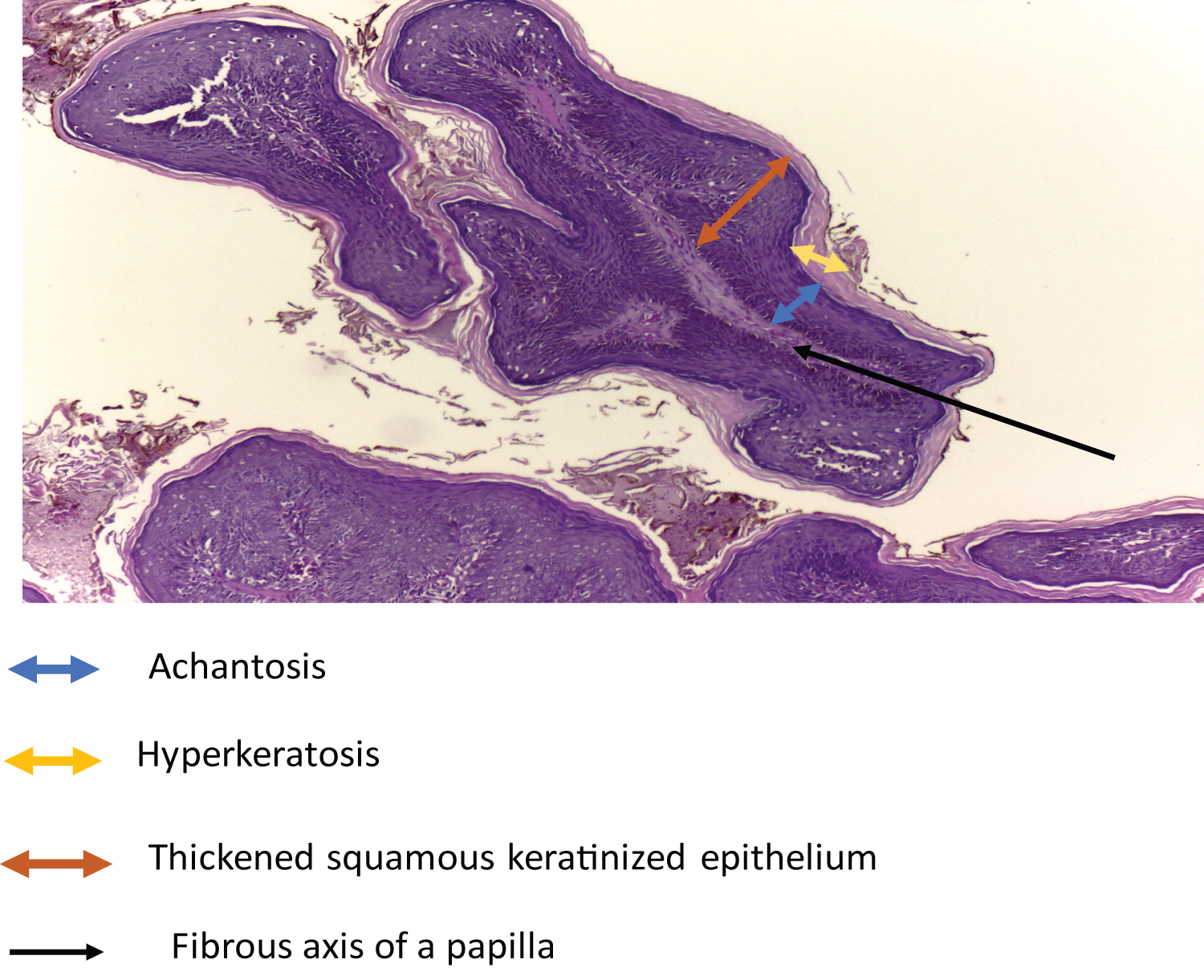 Figure 2: EAC papilloma seen under an optical microscope (HE × 100) in our patient.
View Figure 2
Figure 2: EAC papilloma seen under an optical microscope (HE × 100) in our patient.
View Figure 2
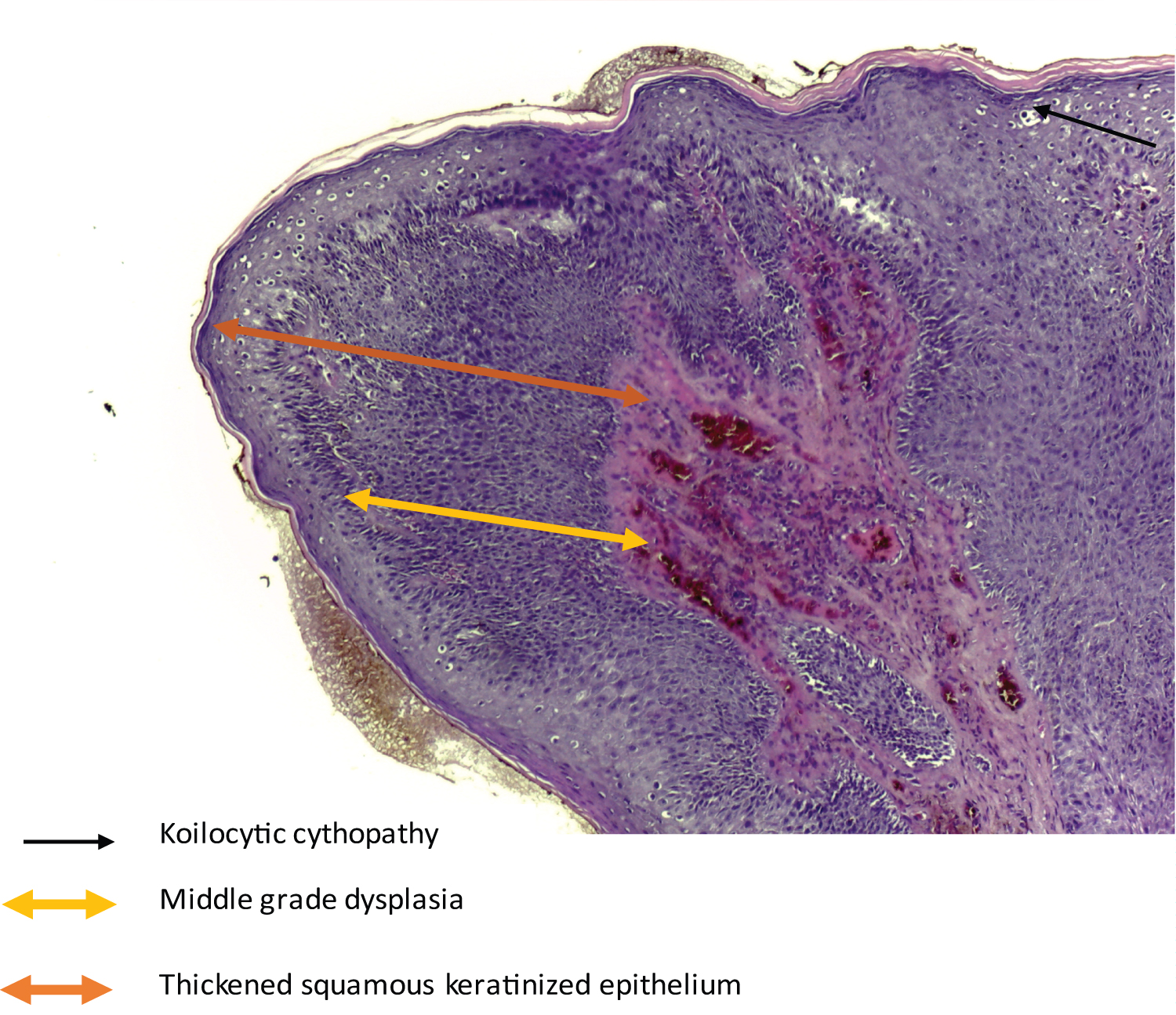 Figure 3: Papilla consisting of a squamous epithelium, seat of high-grade dysplasia with koilocytic cytopathy seen under an optical microscope (HE × 100) in our patient.
View Figure 3
Figure 3: Papilla consisting of a squamous epithelium, seat of high-grade dysplasia with koilocytic cytopathy seen under an optical microscope (HE × 100) in our patient.
View Figure 3
Considering the location and the small size of the lesion, we proceeded to a surgical excision in our patient under local anesthesia. No recurrence was noted, with a current follow-up of 3 months. The patient will be followed on a six-monthly basis in the ENT department (Figure 4).
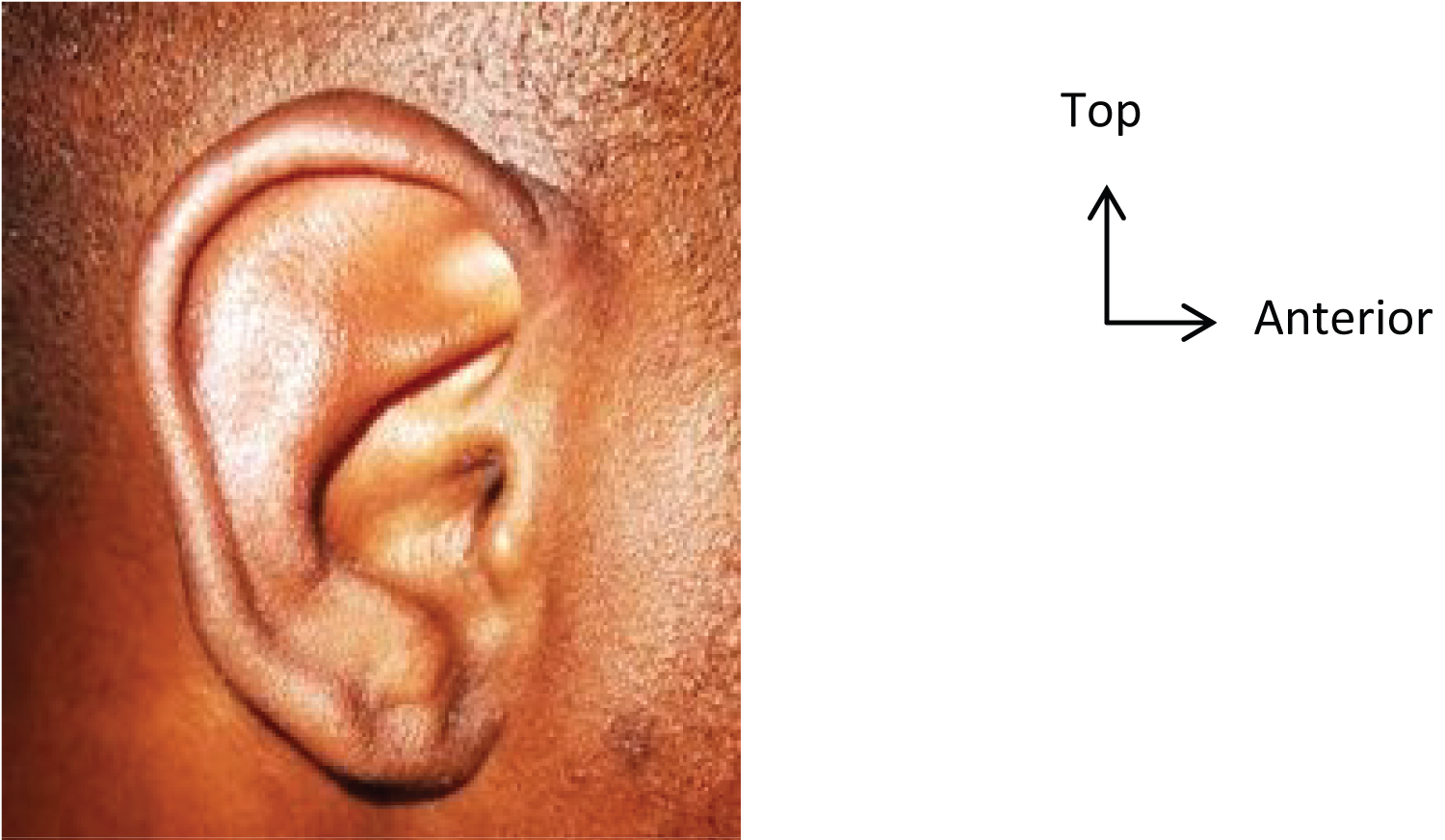 Figure 4: The skin of the external auditory canal has healed well after 3 months of excision of the mass.
View Figure 4
Figure 4: The skin of the external auditory canal has healed well after 3 months of excision of the mass.
View Figure 4
Transmission to HPV is promoted by small erosions which can allow the virus to enter the skin, from another individual or by self-inoculation [2]. Microtrauma of the external auditory canal by regular use of cotton swab could be incriminated in our patient. The sharing of soiled toiletries, common baths (sauna, jacuzzi) and frequentation of swimming pools and gymnasiums is regularly questioned in the literature [2,7]. However, a recent study [7,8] showed the absence of the links between the use of public swimming pools, sports halls (showers) and the presence of warts. The prevalence of warts is higher in certain professions (butchers, veterinarians, slaughterhouses, fishmongers) [2]. A background of atopy and immunosuppression constitutes a high risk factor in the acquisition of warts (HPV 3, 10 and 28) [1,9]. More than 100 different types of viruses currently known cause different clinical pictures on the skin and mucous membranes. Most are benign, but they can also cause malignant changes [1]. In our patient, high-grade dysplasia was found. The skin Papilloma have many appearances. The appearance can vary considerably depending on the location [1]. HPV-induced skin lesions are most often verruciform. They have variable locations. These are either common warts (HPV 2, 4, 29) which preferentially affect the backs of the hands and fingers [1,5] or plantar warts (HPV 1, 2) which can produce a clinical picture of myrmecia or mosaic and superficial [5], either filiform and finger-like warts of the face and neck which can be disseminated by shaving [5] or flat warts (HPV 3, 10, 28) located preferentially on the face, forearms and hands [1,5]. These cutaneous locations are also periorificial, perinarinary, perioral inoculated by a licking tic, or in the scalp and cervical region due to self-inoculation by shaving (HPV 2, 4, 5) [2,4,5]. Muco-cutaneous or only mucous membrane attacks can occur in the anogenital or oral sphere. The locations are the cervix and anus, the oral cavity and the pharynx [1]. Doumbia, et al. reported a case of tongue papilloma [10]. Localizations of the nasal cavities' papilloma have also been described in the literature [11]. The involvement of the external auditory canal, as in our patient, is rarely raised. Abil, et al. reported one case [4].
The diagnosis of warts is clinical but when localization is rare and there is doubt as was the case in our patient, biopsy is necessary [4,7]. Histological examination confirms the papilloma by showing a specific cytopathogenic effect in keratinocytes (koilocytes). Virological diagnosis by molecular analysis of viral DNA is not done routinely. PCR is the most sensitive method to determine the type of human papillomavirus. It is useful for detecting oncogenic viruses or when in doubt about the existence of sexual abuse.
Although spontaneous regression of warts is the rule [2], the functional or aesthetic repercussions and contagiousness of warts often require therapeutic measures [2,8]. The treatment of skin warts remains a difficult problem and is not consensual. The therapeutic warts treatment must take into account the location, the benign character, the painful character, the possibility of spontaneous disappearance or relapse [2]. Even after the wart has healed, HPV can persist on healthy or scarred skin and be responsible for relapses. Thus, currently, no treatment guarantees against a relapse in the weeks or months following recovery. The basis of treatment is the physical destruction of infected cells. The existence of multiple treatment modalities reflects the poor efficacy of the treatments offered with an average cure rate at 3 months between 60 and 70%. The most commonly used treatments are cryotherapy and salicylic acid preparations [2]. Surgical destruction by electrocoagulation or with a CO2 or pulsed dye laser requires local anesthesia and 2 to 3 weeks to heal [5]. In our patient, we performed a surgical excision by electrocoagulation under local anesthesia. No recurrence was noted with a 3-months current regress.
The message of this case report is that localization of HPV infections is rare in the external auditory canal. Treatment should be multidisciplinary between ENT surgeons, dermatologists, internists and pathologists. On the skin, the diagnosis is obvious because it is easy to recognize, but when the location is atypical, as was the case in our patient, histological confirmation with pathological examination is required. In our patient, the treatment consisted of the mass resection. However, integration with CAE-level wart diagnosis and treatment algorithms requires further large-scale and national studies due to our small sample size.