High hospital readmission rates contribute to rising health care costs and lower quality of care, particularly in cardiac patients. Transitional care programs that expedite post-discharge visits have the potential to improve this problem. This study examined the effectiveness of one such program, Bridging the Discharge Gap Effectively (BRIDGE), a single-visit, nurse-practitioner-led, cardiac transitional care program.
We retrospectively abstracted demographics, comorbidities, and 6-month outcome data on all patients referred to BRIDGE from 2008-2013. Demographics and outcomes were compared between BRIDGE attenders and non-attenders. A secondary analysis of timing and reasons for readmissions was also conducted among Acute Coronary Syndrome (ACS) and Heart Failure (HF) patients.
Of 2,367 patients referred, 1,716 (72.5%) attended BRIDGE. Few demographic differences were seen between BRIDGE attenders and non-attenders. BRIDGE appointments were scheduled much sooner than appointments with other health care providers. ACS attendees had significantly lower 30-, 60-, and 90-day readmission rates than non-attendees, but there were no differences in readmission rates for both HF and Atrial Fibrillation (AF) patients. Of ACS and HF patients who were readmitted within 30 days, greater than 50% were readmitted at 0-14 days post-discharge.
The BRIDGE clinic is an easily transportable model for transitional care and has proven effective in decreasing readmissions in the ACS population. Further research is needed to develop successful preventive strategies for the vulnerable populations identified through this and other transitional care models.
Transitional care, Hospital-to-home, Unplanned readmission, Cardiovascular disease
Cardiovascular Disease (CVD) is the leading cause of death in the United States [1]. It is estimated that nearly 1 of every 6 hospital admissions is for a cardiovascular diagnosis [2] and with readmission rates as high as 22.6% for some cardiac conditions [3], CVD is the most frequently reported diagnosis for hospitalization [1]. Not surprisingly, CVD is also among the most expensive conditions to manage, with hospitalization costs attributable to CVD estimated at $71.2 billion dollars annually. This was more than one-third of the cost for all other hospital admissions combined [2].
In a 2009 landmark study, Jencks, et al. reported that nearly 20% of Medicare patients discharged had an unplanned rehospitalization within 30 days; over half of these readmissions were attributed to patients who had not had any contact with a health care provider since index discharge [4]. In fact, early estimates suggested that as many as 76% of readmissions may have been preventable [5,6], and that readmissions alone accounted for between $12 billion [5,6] to $17 billion of Medicare costs [4]. Acute Myocardial Infarction (AMI) and Heart Failure (HF) have been cited as among the most common and costly contributors [4,7,8].
Because of national attention and financial incentives to reduce readmissions since 2009, the all cause readmission rates for AMI and HF have decreased by 13% and 7%, respectively. Unfortunately, these rates remain substantially above the desired benchmark readmission rate of 13.9% [8]. Research to understand hospital readmissions, define methods and models to identify those likely to be readmitted, and create programs to prevent readmissions continue to be a priority [9].
Hospital readmissions may be attributed to a number of factors. Among these are emergency department decision making, behaviors of the discharging hospital, communication between inpatient and outpatient providers, patient readiness for discharge or decompensation after discharge, disease monitoring strategies post discharge, patient ability to self-manage, and time to discharge follow up [10-16]. Many programs are presently active across the US to address these transitional care issues. Most of these models incorporate one or more of the following elements: enhanced discharge education, telemanagement, and home visits. Yet, despite national efforts, hospital readmissions continue to be a vexing and pervasive problem, and no single intervention has been successful enough to garner overwhelming support [4,6]. Further, the relative shortage of cardiologists in many geographic locations has exacerbated readmission management for CVD [17,18].
Bridging the Discharge Gap Effectively (BRIDGE) is a novel, "single-dose", cardiac transitional care program developed in the University of Michigan Health System that addresses a number of the aforementioned contributors of unplanned readmissions. The BRIDGE clinic began in our institution in 2008, when first available appointments for cardiac patients were averaging 50-60 days post-discharge. The program is nurse practitioner-led and strives to facilitate patients' transition from hospital to home by serving as an extension of the inpatient care cardiologist and team. The clinic is situated within an existing preventive cardiology practice that provides onsite support, including cardiology backup. Patients are scheduled for a 60-minute visit, ideally within fourteen days of hospital discharge. At these visits, nurse practitioners assess each patient's status and response to treatment, and use evidence-based guidelines to educate patients on cardiovascular disease and lifestyle modifications, make referrals, and make evidence-based medication and therapy adjustments when necessary. The purpose of this paper is to describe the outcomes of the BRIDGE program over 5 years.
The University of Michigan hospital is an academic medical center staffed by faculty who are employed by the institution in a group practice. The four-inpatient teams of the Division of Cardiovascular Medicine are each led by a cardiologist who supervises a senior and two junior residents, and several medical students. On-call teams include a cardiology fellow, and a senior and two junior residents. Discharge education is provided by the attending cardiologist, residents, and nursing staff using evidence-based protocols. Inpatient attending physicians were instructed to schedule follow-up in the following manner. All patients discharged after an index hospitalization in which the primary or secondary diagnosis was cardiac (e.g. Acute Coronary Syndrome [ACS], Heart Failure [HF], Atrial Fibrillation [AF]) and without available follow-up within 14 days of discharge, were automatically referred to the program.
The Michigan Clinical Outcomes Research and Reporting Program (MCORRP), a research laboratory within the Division of Cardiovascular Medicine specifically designed to create and manage clinical registries, developed and maintains the web-based registry for the BRIDGE program. To assure that patients' protected health information remained confidential, patients were assigned unique participant IDs, and all data were encrypted. Trained MCORRP research assistants abstracted data retrospectively from the electronic medical records of all patients referred to the BRIDGE clinic after a hospital admission, regardless of BRIDGE attendance. The data abstraction form included variables for demographics, comorbidities, admission and discharge elements, treatments, and 6-month follow-up data. For patients lost to follow-up, the Social Security Death Index was used to determine mortality status. The Institutional Review Board at the University of Michigan approved this study (HUM00035421).
To ensure data quality, the first ten cases for all abstractors were dually abstracted and compared. A further ongoing 10% of all cases were randomly audited. Principal investigators resolved all discrepancies. Basic statistical tests were performed on all data routinely to identify and correct duplicate cases, erroneous data, and inconsistencies.
Consecutive data for all adult patients referred to the BRIDGE program from June 2008 through December 2013 were collected. Patients were grouped by attendance or non-attendance for analysis (Figure 1). Patients were excluded if they were lost to follow-up or if they had an early adverse event (i.e. visited the ED, were readmitted, or died prior to their initial BRIDGE appointment date). Baseline frequencies and descriptive analyses were assessed for all demographic variables, comorbidities, and Charlson Comorbidity Index scores, and compared between BRIDGE attenders and non-attenders.
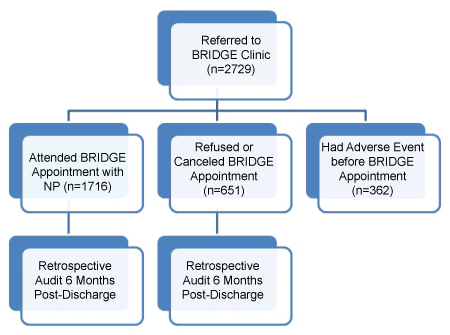 Figure 1: Patient flow diagram. View Figure 1
Figure 1: Patient flow diagram. View Figure 1
A separate analysis was conducted to determine when readmissions occurred during the first 30-days post-discharge. This analysis examined all ACS and HF patients who were referred to the BRIDGE clinic and readmitted within 30 days of index discharge, regardless of BRIDGE attendance. Patients were divided into 4 cohorts, based on the time to their readmission: 0-3 days, 4-7 days, 8-14 days, and 15-30 days. Trends in time-to-readmission were determined for both ACS and HF patients, as were reasons for the readmissions within each timeframe. Reasons for readmission were categorized as "same cardiac", "different cardiac", or "non-cardiac". Readmission rates and reasons for readmission were compared within and between groups [19].
Data were analysed using SPSS 22.0 (IBM Corp. Released 2013. IBM SPSS Statistics for Windows, Version 22.0. Armonk, NY: IBM Corp.). All variables were assessed for compliance with statistical assumptions. Missing data were excluded from the sample. Independent student t-tests and Chi-Square were used to compare groups. Pearson's Chi-square test for significance was reported, except in cases where the expected count would violate an underlying assumption; in those cases, Fisher's exact test was reported. A p-value less than 0.05 was considered significant for all analyses.
Of 2,367 patients referred to the BRIDGE program, 1,716 (72.5%) attended, and 362 (15%) were excluded from this analysis due to an early adverse event (Figure 1). Patients who were excluded were older (66.84 ± 15.58 vs. 64.88 ± 14.62; p = 0.02), had higher Charlson Comorbidity scores (5.13 ± 2.42 vs. 4.58 ± 2.34; p < 0.01), and were more likely to have depression (29.5% vs. 22.7%; p = 0.01). No other significant differences were noted between groups (Table 1).
Table 1: Characteristics of patients with and without an adverse event prior to BRIDGE Appointment (N = 2723). View Table 1
There were few demographic differences between patients who attended their BRIDGE appointment and those who did not (Table 2). Males were somewhat more likely to attend than females (74.2% vs. 70.2%; p = 0.03). No racial differences were observed between White and non-White patients. Although mean Charlson Comorbidity score was similar for BRIDGE attenders and non-attenders (4.58 vs. 4.61; p = 0.77), attenders were less likely to have vascular disease (16.0% vs. 20.4%; p = 0.01) or psychiatric disorders (29.2% vs. 34.3%; p = 0.02) than non-attenders.
Table 2: Demographic characteristics of patients referred to BRIDGE (N = 2367). View Table 2
The majority of patients were referred to BRIDGE for the following inpatient diagnoses: ACS (27.2%), HF (19.6%), and AF (15.3%). Other reasons for BRIDGE referral included primary discharge diagnoses of coronary artery disease, chest pain, cardiomyopathy, malignancy, and pericarditis. The mean number of days from hospital discharge to a BRIDGE appointment was 14.6 ± 8.6 days.
On average, patients were seen by a BRIDGE nurse practitioner earlier than any other provider (Figure 2). In particular, patients were scheduled to see cardiologists nearly 2-months post-discharge, regardless of BRIDGE attendance. However, when patients attended BRIDGE, follow-up with cardiology was later (67.6 ± 55.9 days for attenders vs. 56.3 ± 76.0 days for non-attenders). This is in part due to the BRIDGE nurse practitioners' decisions to schedule and adjust follow-up appointments based on their clinical evaluations of the patients' stability.
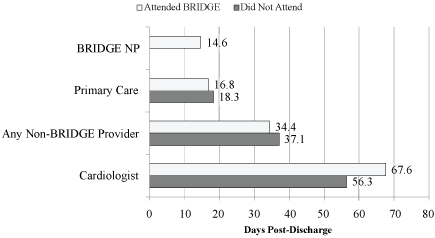 Figure 2: Average number of days from hospital discharge to first interaction with specific health care providers. Cardiologist = outpatient follow-up with their cardiac specialist; Any Provider = post-discharge follow-up with any health care provider other than their BRIDGE provider; BRIDGE = follow-up with an NP in the BRIDGE clinic. View Figure 2
Figure 2: Average number of days from hospital discharge to first interaction with specific health care providers. Cardiologist = outpatient follow-up with their cardiac specialist; Any Provider = post-discharge follow-up with any health care provider other than their BRIDGE provider; BRIDGE = follow-up with an NP in the BRIDGE clinic. View Figure 2
Readmission rates varied by diagnosis (Table 3). In the ACS subpopulation, BRIDGE attenders were significantly less likely to be readmitted at 30, 60, and 90 days post-discharge than non-attenders. However, patients with a primary discharge diagnosis of HF had more ED visits and readmissions within 180 days than non-attenders (p = 0.052). Significant differences in ED visits and readmissions between attenders and non-attenders were not observed in AF patients or any other diagnoses.
Table 3: Readmission and emergency department visit rates by diagnosis (N = 1470). View Table 3
Among ACS and HF patients, 16.8% (n = 123) and 25.4% (n = 139) were readmitted within 30 days, respectively. Of those readmitted, greater than 50% were readmitted within 14 days of index discharge for both groups (ACS and HF patients). Additionally, the steepest increase in readmission rates occurred during the 4-7 and 8-14 day timeframes (38.2% to 62.6% for ACS patients and 25.2% to 53.2% for CHF patients). The largest proportion of ACS and HF patients readmitted between 0-3 days post-discharge were readmitted for "non-cardiac" reasons; however, for every other timeframe, ACS and HF patients were most commonly readmitted for "cardiac non-ACS" and HF diagnoses, respectively [19].
There are many reasons that patients have unplanned hospital readmissions, and there are many models of care currently being tested to identify at-risk patients and prevent these hospitalizations [10,20]. BRIDGE is a unique, single-visit approach to navigate the time gap between hospital discharge and follow-up ambulatory care in which the inpatient provider will take responsibility for managing care. Previous BRIDGE studies have demonstrated similar readmission reductions for ACS patients [21], as well as a significant cost benefit due to avoided readmissions [22]. In this study, we sought to describe how this model performed over time.
It is important to note that the 15% of patients (n = 356) who were excluded from the BRIDGE analysis due to an early adverse event were older and had higher comorbidity scores (Table 1). In effect, these patients were likely more ill. According to Lochner, et al. the more comorbid conditions a patient has, the more frequently they are readmitted [23]. This, in addition to the growing number of risk prediction models, suggests that we have some ability to predict who is at risk for readmission. However, it does not seem that knowing that a patient is at risk is sufficient to avoid the readmission using our program.
Perhaps this is why, as we see in this study, BRIDGE benefits some diagnoses but not others. Patients with ACS are often younger and have fewer comorbid conditions than those with HF. Heart failure readmission rates are no different for patients who participate in BRIDGE and those who do not; atrial fibrillation is even more unique. In this sample, there is no statistical difference between AF attenders and non-attenders in readmission or ED visit rates. However, there was a trend for higher readmission rates in attenders. Again, one possible reason for this may be different baseline characteristics of AF patients versus HF and ACS patients. Another possible reason is due to patient instability, and BRIDGE nurse practitioners therefore encouraging the patients' ED visit or hospital admission. In our program, BRIDGE consistently demonstrated success in reducing readmissions for ACS patients, but not for HF or AF patients.
Further, this study demonstrates that at this institution, there continues to be delays in follow-up when patients pursue usual care avenues, such as cardiology or primary care. Given that we are able to identify who and when patients are likely at risk for readmission, greater efforts should be aimed at coordinating and communicating transitional efforts with multiple departments. It is essential that all patients, not only those enrolled and participating in readmission avoidance studies, have access to early, appropriate, and guideline-based transitional care.
Results from the BRIDGE experience offer cautious optimism for the transitional care of cardiovascular patients. In a study conducted by Kociol, et al. of 100 hospitals participating in the Get With The Guidelines-Heart Failure (GWTG-HF) quality improvement initiative, it was noted that there was wide variation in strategies being implemented to reduce HF readmissions [24]. Of note, efforts to enhance transitional care appeared to be associated with modest reductions in short-term readmission rates. No other care processes were reliably and consistently associated with these reductions. This reinforces the need for an evidence base from which to create best practices and provides support for transitional care practices like the BRIDGE clinic.
Although this program has been successful, there are some limitations to consider. This study is from an observational registry and lacks randomization, which may limit generalizability; causality should not be assumed. Further, at the onset of the BRIDGE program, 14 days was a reasonable time for discharge follow-up. It is now widely accepted that, for many diagnoses, follow-up needs to be sooner [24], ideally, within 7 days. Finally, 30-day readmission rates analyses are complicated by the exclusion of patients with early adverse events. As a result, it was only possible to provide comparison data for the brief 14-30 day post-discharge period, as those with an adverse event before this timeframe (i.e. the time of their scheduled BRIDGE appointment) were excluded from analysis.
Many institutions and groups are working to design and implement their own transitional care models [9]. The BRIDGE program is a simple model that can be easily incorporated into an existing hospital-based cardiology practice. Participation rates in BRIDGE were high, especially for patients with multiple comorbidities, and BRIDGE was associated with lower 30-day readmission and ED visit rates in the ACS population. BRIDGE is an effective strategy to address the paucity of transitional care for cardiovascular patients. To some degree, we are able to identify who, when, and why many patients will be readmitted. What we have yet to learn is how to best prevent these readmissions. Clearly, this is a call for enhanced transitional care. Only through better collaboration between discharge providers, primary care teams, and subspecialists can we hope to further reduce readmissions.
The authors would like to acknowledge the BRIDGE clinic nurse practitioners for their hard work in the clinic and their contribution to the registry. Additionally, we would like to acknowledge Janice Norville for her continued support of and dedication to the BRIDGE program.
This study, which involved data from the electronic medical records of human participants, was in accordance with the ethical standards of the institutional review board at the University of Michigan and with the 1964 Helsinki declaration and its later amendments.
The authors declare no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.