Systemic lupus erythematosus (SLE) is a chronic autoimmune disease characterized by a multitude of autoantibody production. Lupus nephritis (LN) is one of its most severe manifestations and its treatment is well established with the usage of immunosuppressions [1-5]. However the use of these immunosuppressions at high doses are fraught with adverse effects including infections, subfertility and even malignancy. A multi-targeted approach has been used in the remission-induction of LN, which includes the use of plasmapheresis. Plasmapheresis (PP) 'physically' removes the autoantibodies involved thus reducing the antibody burden. Dual filtration PP (DFPP) uses two different pore sized filter thus permits back diffusion of albumin into the patient thus minimizing plasma resubstituition with 5% albumin.
Systemic lupus nephritis (SLE) is an autoimmune disease and lupus nephritis (LN) is one of its most severe manifestations. The standard therapy with intravenous steroids and cyclophosphamide as remission-induction is established and well tolerated [1]. As the standard therapy is not without side effects, other modalities are explored which include other immunosuppressive agents and the usage of plasmapheresis.
Plasmapheresis includes plasma exchange, plasma adsorption and double filtration plasmapheresis (DFPP). DFPP is a form of plasmapheresis, which uses 2 filters of different pore sizes. The first larger pore sized filter as a standard hemofiltration. The second smaller pore size filter allows smaller molecules to revert back to patients' circulation thus minimizing the amount of replacement fluid. This would in turn minimize the complications related to the use of substituition fluid. DFPP had been used in other autoimmune diseases such as mysthaenia gravis and Guillan Barre syndrome.
Amongst the complications of DFPP are headache, nausea and vomiting. As other forms of plasmapheresis, the major complication of DFPP is bleeding as it not only removes the desired autoantibodies but also other molecules such as the serum fibrinogen and coagulation profile. Thrombocytopenia has also been reported. Another major concern is catheter related complications which include catheter related sepsis, deep vein thrombosis and bleeding from the catheter site.
At our center, a multi-targeted approach had been practiced in the remission-induction of severe LN, which consists of low dose intravenous steroids, plasmapheresis and intravenous cyclophosphamide. This study is to determine the tolerability of using DFPP in the remission-induction of severe LN.
To determine the tolerability of DFPP in remission-induction of patients with severe LN.
Eight patients with new onset or relapse LN of classes III/IV + V were recruited to receive one session of DFPP every other day for a total of three sessions. Each patient was pulsed with 250 mg intravenous methylprednisolone for three days and put on oral prednisolone, which was tapered, gradually.
All patients were subjected to DFFP for three sessions, which was carried every other day. Each session lasted for two hours. DFPP was carried out using the Plasmaflo OP-05W (L) and DFPP Cascadeflo (ASAHI). The target plasma volume was 50 mls/kg each session, blood flow rate at 100 mls/min, plasma flow rate at 30 mls/min, and the effluent flow rate at 1-3 mls/min. Two units of fresh frozen plasma were given to all patients post each session.
Blood pressure (BP) was recorded prior and after each DFPP procedures. Hemoglobin, platelets, serum fibrinogen and coagulation profile (PT, APTT and INR) were measured before and after each session of DFPP. Femoral vein was used as vascular access in all patients.
A total of 23 DFPP sessions were carried out. Seven patients received all three sessions of DFPP as scheduled. One patient only received two sessions of DFPP as she developed catheter related infection, which resolved completely after a course of intravenous antibiotics.
There was a significant drop of BP after the first DFPP session (p = 0.017). There was no drop in BP post second and third session (p = 0.176 & p = 0.684) (Table 1, Figure 1 and Figure 2).
Table 1: Blood pressure profiles pre and post DFPP sessions. View Table 1
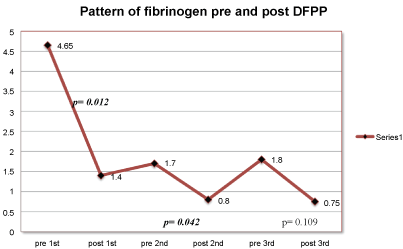 Figure 1: Pattern of serum fibrinogen post each DFPP.
Figure 1: Pattern of serum fibrinogen post each DFPP.
Coagulation profile was also significantly prolonged post procedures as shown below. View Figure 1
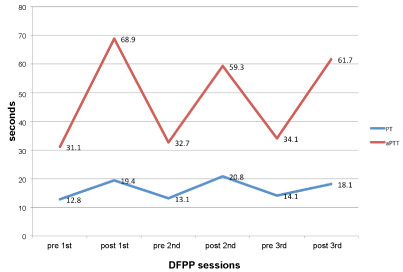 Figure 2: Coagulation profile post procedure.
Figure 2: Coagulation profile post procedure.
Platelets were stable in all patients. No patients bled pre and post DFPP despite the significant drop in the fibrinogen level and the prolongation of the coagulation profile. View Figure 2
LN is a one of the most severe manifestations of SLE. The standard therapy with intravenous steroids and cyclophosphamide is well established and tolerated. Other therapies have been explored in the remission induction of severe LN including the use of plsamapheresis. DFPP is a form of plasmapheresis, which uses two different pore sized filters and enable selective autoantibodies to be removed according to its molecular weight [6]. It also allows smaller molecules such as albumin to move back to the patients' circulation thus minimizing the amount of replacement fluid.
Amongst the complication of DFPP are headache, nausea and vomiting. The major complications include bleeding, hypotension and catheter related complications.
From our study, a total of eight patients underwent a total of 23 sessions of DFPP. Seven patients had three sessions while one had two sessions of DFPP. Plasmapheresis in general does not only remove the desired autoantibodies. It also removes other smaller molecules such as the clotting factors and serum fibrinogen.
From our observation, there was a significant drop in the serum fibrinogen post each DFPP session. The serum fibrinogen normalized within 24 hours post procedure. This is in contrast with the report from Yeh, et al. [7] who reported that normalization of serum fibrinogen post DFPP takes about 3-4 days post procedure. There was also a significant prolongation of the coagulation profile, which was monitored by measuring the aPTT, PT and INR. Despite the significant abnormalities in the serum fibrinogen and coagulation post DFPP, no bleeding occurred.
A local report in UKMMC by Loo, et al. [8] documented the occurrence of thrombocytopenia post DFPP. Although the membranes used were 'biocompatible', some patients may have an idiosyncratic response to the membrane constituents with activation and trapping of platelets. In our study, the serum platelets were stable and normal pre and post procedures.
Hypotension is another concern in plasmapheresis in general. In patients with severe LN, the nephrotic state itself predisposes patient to developing hypotension post procedure as they are intravascularly depleted. Post first DFPP procedure, there was a significant drop in the systolic BP compared to the second and third sessions. Despite no significant improvement in the terms of serum albumin pre and post procedure, we postulate that, at the beginning of the treatment (ie post 1st DFPP session), patients were not as nephrotic as compared to the mid treatment (ie post 2nd and 3rd DFPP. Hence the lower serum albumin at the beginning, made them more vulnerable to hypotension as DFPP removes autoantibodies which are protein making them more depleted intravascularly. However all patients were asymptomatic of hypotension.
Bleeding and hemolysis can also lead to hypotension in patients who undergo DFPP. From our study, the hemoglobin was stable in all patients' pre and post DFPP without a significant drop. No patients develop hemolysis.
A complication, which is specific for the use of plasmapheresis, is vascular access related. Among the catheter related complications are bleeding, vein thrombosis and catheter related sepsis. Yeh, et al. reported that the incidence of catheter related thrombosis is 0.8% and catheter related sepsis was 4.1% in study cohort of a 335 patients who received DFPP, which was performed in mainly neurological autoimmune diseases.
The incidence of catheter related sepsis in our study seemed fairly high despite all precautions (12.5% patients), as these patients were immunocompromised, given their nephrotic state. The one patient who developed catheter related infection recovered well after the appropriate antibiotics.
Two patients in our study developed superficial vein thrombosis. Again this could be explained to the fact that they are nephrotic which by itself is a risk factor for developing venous thrombosis.
As a conclusion, DFPP is well tolerated by severe LN patients. However, given the underlying nephrotic state of the patient which by itself is a risk factor of developing the complications mentioned, utmost precautions should be taken when administering this mode of treatment in patients with LN.