Dysmenorrhea is the most common gynaecological symptom among young women. It results in negative physical and psychological consequences. The aim of this study was to investigate the epidemiology of dysmenorrhea and detect the sources of knowledge about menstrual disorders among female students in Beni-Suef University, Egypt.
A total of 1908 university female students attending all faculties (n = 28) of Beni-Suef University and representing all academic years were selected, using a multi-stage random sampling, to participate in this cross-sectional study. An Arabic-language structured questionnaire was designed and included questions about the socio-demographic characteristics of the university students, menstrual history and history of dysmenorrhea during 2017 and sources of knowledge about dysmenorrhea.
Of the interviewed students, 92.9% experienced dysmenorrhea during 2017. Age, residence, educational level of parents, exposure to passive smoking, circumcision and physical activity showed no statistically significant differences between students who experienced dysmenorrhea and those who did not (p >0.05). Backaches, nervousness and irritation, and acne and flushing were the most common symptoms associated with menses, 65.7%, 51%, and 47.3%, respectively. Students referred to family members (72.8%), friends (24.3%), teachers or lecturers (21.4%), TV and the Internet (17.2%), and physicians or nurses (6.9%) to acquire information about dysmenorrhea.
Dysmenorrhea is highly prevalent among university students in Beni-Suef. Further research should focus on the adaptive techniques used by the students to mitigate the negative impacts of dysmenorrhea.
Dysmenorrhea, University students, Risk factors
Dysmenorrhea or painful menstruation is a state of unpleasent cramping sensation of uterine origin. Although it may present alone, variant complaints usually accompany in the form of achings and spasms, gasterointestinal tract (GIT) symptoms or irritation and nervousness [1]. Dysmenorreha usually affect young women at school/university age leading to school/university absence, academic underachievement and undermined quality of life [1-3]. However, the awareness of young women about dysmenorrhea, which depends mainly on the source of knowledge, may have an impact on their ability to cope with such symptoms [4]. Physicians could play a pivotal role in controlling dysmenorrhea and its associated symptoms by providing comfort measures and helping in anxiety relief. They could also check for the physical and psychological wellbeing of the young women and offer them the required knowledge [4].
Various risk factors have been suggested to be associated with dysmenorrhea such as hormonal imbalance, failure to cope with stress, greater BMI, younger age of menarche, nutritional deficiencies, smoking or exposure to passive smoking, and lack of physical activity [5-10]. Although many international studies have investigated the epidemiology of dysmenorrhea among young women [11-14], only few national studies did [15-17]. Understanding the epidemiology of dysmenorrhea among university students in Beni-Suef may help in designing awareness programs tailored to suit the social and cultural criteria of the community and help students get over the negative health consequences of dysmenorrhea.
In this regards, this study aims at detecting the occurence and correlates of dysmenorrhea among female students in Beni-Suef University and exploring the sources of information they use to know about menstruation and menstrual disorders.
This cross-sectional study was conducted on a total of 1908 female university students attending 28 faculties in Beni-Suef University throughout the first term of the academic year 2017/2018 between September 2017 and January 2018. The study population age ranges between 18 and 23 years in all grades of different faculties. They live in urban or rural areas of Beni Suef City. To be included in the study, female students must have had a period for the year 2017. Beni-Suef University is one of the largest educational institutions in Upper Egypt with more than 45,000 students registered in its 28 faculties; 12 faculties of humanities, social and behavioural sciences, 9 faculties of health sciences, and 7 faculties of engineering and computer sciences.
The sample size was calculated using Epi-Info version 7 Stat Calc, [Center for Disease Control (CDC), WHO], based on the following criteria; dysmenorrhea rate of 70%, confidence level of 95%, and margin of error of 5%. A multi-stage random sampling methodology was used to include female students from all faculties and all academic years. Later, random sampling was applied from every grade level in every faculty with a minimum sample of 10% of total female students registered in each academic year.
The protocol of the study has been approved from the Research Ethics Committee of Faculty of Medicine, Beni-Suef University, and then institutional approvals were obtained. The students were informed of the purpose of the study with confirming confidentiality of data. Informed verbal consents were obtained from all students before participation.
For data collection, we prepared an Arabic-language structured questionnaire of two sections; section one included socio-demographic characteristics, whether the university student was physical active or not, marriage status, circumcision and sleep quality (assessed by the tool called the Pittsburgh Sleep Quality Index (PSQI). This version was translated and adjusted to be easy for students to answer. Quality of sleep during menstruation was assessed. PSQI consisted of ten questions, which defined seven parts: Subjective sleep quality; sleep latency; duration of sleep (sleeping hours); sleep efficiency; sleep disturbance; need for medications to sleep; and day dysfunction due to sleepiness. The maximum score is 21 points. Students scoring more than five points were classified as bad sleepers) [18]. Also in section one, students answered questions about exposure to passive smoking, age at menarche, duration of the menstrual cycle and flow days (counting the number of days of menstruation by students has been used to assess menstrual blood loss. Based on this method, increased menstrual flow is documented if the menstrual period lasts for more than seven days/cycle [19]. The second section questioned if the girl had experienced dysmenorrhea, its frequency and duration during the previous year of the study (2017), details of menstrual pain (onset, location, type, duration etc), any medications received for menstrual pain, other clinical manifestations associated with menses, history of infertility in married females, history suggestive of endometriosis (pelvic pain that worsens with menstruation, dyspareunia and painful bowel movements or urination) and the main sources of information about dysmenorrhea girls resorted to. Dysmenorrhea was defined as menstrual pelvic pain that required rest or interfered with regular activities rather than occasional cramping pains [20]. Dyspareunia was described as genital pain occurs during sexual intercourse [21]. Quantification of dysmenorrhea and severity grading were evaluated using visual analogue scale (VAS).
The VAS was drawn as a 10-cm line explaining female student's opinion of the degree of pain. One side of the line represented "unbearable pain", and the other side represented "no pain at all". Students were asked to rate the degree of pain by making a mark on the line. The scores received from the scale were classified into mild dysmenorrhea if it was between 1 and 3 points moderate between 4 and 7 points, and severe between 8 and 10 points [22].
A pilot study was conducted on 200 students of the recruited sample to assess clearance of questionnaire items and their suitability for the study. Accordingly a structured questionnaire form was finalized and used for collection of data for all participants equally. It included two sections with items described above. Each participant answered the given questions in 60 minutes without interference from any interviewer. The Cronbach's alpha for the reliability of the questionnaire was 0.76 while content validity was again judged by a professor of public health and a professor of gynecology and obstetrics. A trained team of medical students with a supervisor from the Public Health Department interviewed the university students, collected and analyzed all data. Analysis of information in each questionnaire was done into 3 stages. The first stage of analysis included the process of initial coding, whereby each line of the data was considered to identify keywords; these were highlighted because they retained participants' words. The next stage of information analysis involved bringing similar categories together into broader themes. Third stage included further category development leading to final themes to be statistically analyzed [23].
Data were analyzed using the software, Statistical Package for Social Science (SPSS Inc. Released 2009, PASW Statistics for Windows, version 18.0: SPSS Inc., Chicago, Illinois, USA). Frequency distribution as percentage and descriptive statistics in the form of mean and standard deviation were calculated. Chi-square, t-test and correlations were done whenever needed and p values of less than 0.05 were considered significant.
A total of 1908 university students with a mean age of 20.8 ± 1.7 years participated in this study. Of them, 61.9% were living in urban areas and 38.1% were residing rural areas. The educational level of the parents of the participating students was as the following; 7.7% and 20.9% illiterate fathers and mothers, 16.8% and 16.9% completed their elementary education and 75.5% of fathers and 68.2% of mothers had a higher degree. Less than 20% of girls reported regular exercise activity, 4.6% were married, 41.4% stated exposure to passive smoking, and 50.2% were circumcised. The mean hours of sleeping per day were 8.3 ± 1.6 hours/day while mean sleep quality score was 3.5 ± 2.0 points. The participants' age of menarche was 13 ± 1.4 years, and the menstrual cycle duration was 28.4 ± 5.9 days, with 5.2 ± 1.4 flow days (Table 1).
Table 1: Socio-demographic and gynecological characteristics of the participating university students, Beni-Suef University, 2017-2018. View Table 1
Of the 1908 interviewed students, 1773 (92.9%) experienced dysmenorrhea during 2017 (Figure 1). Neither the socio-demographic factors such as residence and parents' education, nor the gynaecological factors such as age of menarche, circumcision, menstrual cycle duration, and flow days were associated with having dysmenorrhea during 2017 (p >0.05). Also, exposure to passive smoking and physical inactivity were not related to dysmenorrhea (p >0.05). However, sleep quality score was related to dysmenorrhea (p < 0.0001) (Table 2). Backaches, nervousness and irritation, and acne and flushing were the most common symptoms associating with menses, 65.7%, 51%, and 47.3%, respectively (Table 3). The main sources of information about menses and dysmenorrhea were mainly family members (72.8%), friends (24.3%), teachers/lecturers (21.4%), and TV/Internet (17.2%), while only 6.9% of the students resorted to physicians/nurses (Table 4).
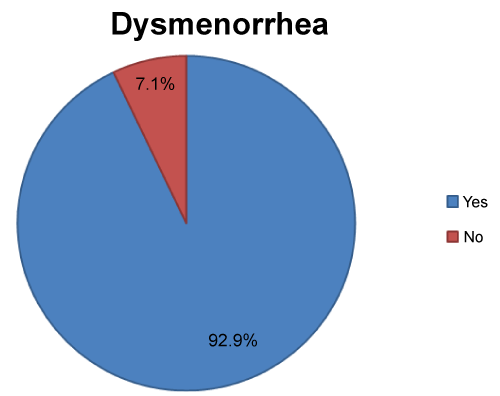 Figure 1: Occurrence of dysmenorrhea during the previous year as reported by the participating university students, Beni-Suef University, 2017-2018. View Figure 1
Figure 1: Occurrence of dysmenorrhea during the previous year as reported by the participating university students, Beni-Suef University, 2017-2018. View Figure 1
Table 2: Factors associated with occurrence of dysmenorrhea during the previous year among the participating university students, Beni-Suef University, 2017-2018. View Table 2
Table 3: Other clinical manifestations associated with menses as reported by the participating university students, Beni-Suef University, 2017-2018. View Table 3
Table 4: Main sources of information about dysmenorrhea and menses as reported by the participating university students, Beni-Suef University, 2017-2018. View Table 4
Among those who reported menstrual pain or dysmenorrhea (92.9%), detailed results of pain namely frequency, onset, duration, type and site presented as follows: Frequency of dysmenorrhea: Majority of students (90.2%) experienced dysmenorrhea each month. Onset of pain: Most of students (73.3%) have reported onset of pain on first day, 18.7% reported pain to start before menstruation, 7.6% declared to have pain started on day 2 or 3 and only 0.3% of participants reported end of pain after stoppage of menstrual flow. So, it was shown in results that most of participants reported dysmenorrhea on day 1 of menses. Duration of menstrual pain as reported by students: Sixty seven percent declared to have menstrual pain for 2 days, 17.3% reported 2 days of pain, and 13.7% reported pain for 4 days while only 1.9% had pain for 1 day after stoppage of menses. Menstrual pain site was reported to be lower abdominal pain in two thirds of students (62%), in addition to lower backache in (18%) and radiation of supra pubic pain to thighs in (4.5%). Moreover, 15.5% suffered from generalized body aches. Type of pain was reported as spasmodic by most of students (76.9%) but 13.2% described piercing type of pain. Shooting pain was declared by 3.5% while stabbing type was reported by 6.3% of girls.
Dysmenorrhea was prevalent in 1773 (92.9%) of study population. VAS scale was used for quantification of dysmenorrhea. Twenty eight percent of students reported severe pain (8-10). Forty nine percent reported moderate score of pain (4-7) and the rest of (23%) students had mild pain. Twenty percent of students who experienced dysmenorrhea reported receiving pain killers for menstrual pain. The rest of participants reported taking rest and hot drinks that helped in relieving pain.
Eighty seven (4.6%) students were married; none of them gave history of infertility. Only 5.7% reported history of infertility. Among those who reported dysmenorrhea (1773), 0.7% reported worsening of pain with menstruation. None of married students had dyspareunia. None of participants reported painful bowel movements or urination.
Dysmenorrhea is a public health concern as it carries negative impacts on physical and emotional health, school attendance, and academic achievement [1,3]. In this cross-sectional study, the occurrence of dysmenorrhea and its associations during 2017 amongst female students in Beni-Suef University were evaluated. A total of 1908 university students representing 92.9% of the participants reported dysmenorrhea. In a study conducted over 664 girls attending secondary and nursing schools in Mansoura (north of Egypt), the results put the prevalence of dysmenorrhea at 75% [15]. Another study on 845 girls attending four secondary schools in Assiut (upper Egypt) reported a prevalence of 76.1% [16]. However, both studies detected the rates of dysmenorrhea during only three months prior to the study. On the other hand, a study on girls attending two nursing schools in Minia (upper Egypt) showed a high prevalence of dysmenorrhea reaching 94.4% of the participants, however this study included only 160 students and did not clarify the length of dysmenorrhea recall [17]. Worldwide, the prevalence of dysmenorrhea varied widely according to the age of the study group, the length of recall/follow-up, and definition of pain whether any pain or pain interrupting with daily activities. In Japan, a prevalence of only 15% was detected in a one-month prospective study over 823 women (18-51 years) [24], while in a study on Chinese women (20-34 years), the 12 months follow-up resulted in a prevalence of 44.4% [8]. The rates reached 60% among Canadian women [11], 61% in Saudi Arabia [14], 76% in the USA [25], and 85.1% in Ethiopia [12].
In the current study, age played no role in the occurrence of dysmenorrhea which contradicted many previous studies [13,16,26]. However, it should be taken into consideration that the age of the university students ranged from 18 to 23 years, and this tight range might explain why the impact of age was not detected in the current study. Other reports concluded that dysmenorrhea peaks in late adolescence, then the incidence falls with increasing age [11,24,25,27].
Also, early menarche was not associated with occurrence of dysmenorrhea which consisted with previous studies [11,28], but did not agree with others [15,16]. It is suggested that older women and those with earlier menarche (more gynaecological years) have been exposed for longer period to uterine prostaglandins making them more prone to experience dysmenorrhea [29]. In our study, students with dysmenorrhea suffered poor quality of sleep. In agreement with our result, it was found that dysmenorrheic women had more disturbed sleep and subjective sleepiness than controls. Their sleep efficiency was reduced when experiencing menstrual pain, with increased wakefulness, movement [30].
Besides, exposure to passive smoking and physical inactivity were not associated with dysmenorrhea which consisted with previous reports [25,28]. It is thought that Nicotine might minimize the endometrial blood flow in addition to its disturbing effect on the hormonal levels [9,10], while physical activity could enhance the blood flow to the uterus and decrease the water retention [31]. Our results also showed that menstrual cycle duration and flow days showed no difference between students who experienced dysmenorrhea and those who did not, a finding that contradicted that of Shiferaw, et al. [12], El-Gilany, et al. [15], Mohamed [16], and Weismann, et al. [25] who concluded that women with longer menstrual cycles were more likely to have dysmenorrhea.
Our students stated that backaches, nervousness and irritation, and acne and flushing were the most common symptoms associated with menses, 65.7%, 51%, and 47.3%, respectively. A previous study on Egyptian women showed also that backaches and nervousness were common symptoms during menses [32].
VAS scale was used for quantification of dysmenorrhea. Pain was divided into mild, moderate and severe pain in this 3 point scale. In our study (28%) of students reported severe pain (8-10). Forty nine percent reported moderate score of pain (4-7) and the rest of (23%) students had mild pain. In contrast to other study where it was revealed that 53.93%, 21.34% and 24.42% of students had mild, moderate and severe pain (dysmenorrhea) respectively [22]. Twenty percent of students who experienced dysmenorrhea reported receiving pain killers for menstrual pain. However, in a study including 408 students, the need for medication was reported in 225/408 (55.2%) subjects [20].
Family members and friends were the main sources of information regarding dysmenorrhea; 72.8% and 24.3%, respectively which come in accordance with previous reports [17,32-34]. Only 4.9% of girls in our study sought information related to dysmenorrhea from physicians or nurses. This could be attributed to the sensitivity of menstrual issues and fear of young women to share private data. Meanwhile, students feel reluctant to seek medical advice and prefer their family members and close friends instead. Further, it seems that there are no available programs or awareness sessions about menstrual disorders offered by Beni-Suef University.
In conclusion, occurrence of dysmenorrhea among university students in Beni-Suef was very high. Family and friends were the main sources of knowledge. Further research should focus on investigating the coping strategies of the students to manage their dysmenorrhea and designing educational programs that allow physicians and/or nurses to discuss the menstrual problems with the university students or young females.
Implications for Practice and/or Policy include encouraging awareness of medical health problems through improving sources of knowledge. This will give systematized methods of treatment involving well informed patients in the treatment plan. Policy development can be through extended process of communication and interaction.
One of the limitations of our study that population of high education level was chosen. Results of main sources of information about dysmenorrhea might have been biased. However, from other studies in a systematic review of prevalence of dysmenorrhea, it was found no association with woman's education or education years [35]. In addition, as described above, health programs or awareness sessions about menstrual disorders are still not offered by Beni-Suef University. Moreover, our results revealed that students preferred to ask a family member or a friend more than seeking a health giver advice.
We thank all our participants.
All authors contributed in design of the study, collection of data, interpreting results and writing discussion in addition to revising work.