The surgical procedure for dental implants presents predictable long-term results. An important part of the surgical procedure is suture, which plays an important role in healing, reconstructing and remodeling soft tissue and promoting hemostasis of the region. The purpose of this case report is to introduce an alternative technique for performing suture in implant surgery of lower total arch. Four implants were placed in the patient's lower jaw, all with a minimum torque of 60 Ncm. A small perforation it was performed in the lingual/buccal face of alveolar bone, between implants previously placed, using a straight handpiece with a 1.1 mm diameter drill at a 45 degrees inclination to the bone platform. Suture it was performed with mononylon (from the buccal soft tissue to the channel created (towards the lingual bone) and was closed through the lingual soft tissue. This procedure can be done between all implants placed. On the third day, the inferior protocol was installed and simultaneous bilateral contacts were adjusted. This suture reduces the possibility of penetration of impression material into implant surgeries with immediate prosthetic rehabilitation. It might reduces the risk of infection and promotes faster healing. After 12 months of follow-up, the implants and prosthesis were in good condition, maintaining the rehabilitation success.
Dental implantation, Dental prosthesis, Surgery, Sutures
Surgery for dental implants placement is a known and safe procedure, with predictable results in the long term [1,2]. Implant survival and success rate in full edentulous patients are high, independent of the loading protocol followed, if conventional, delayed or immediate [3-5]. Multiple aspects must to be controlled during a surgery in order to have success and suture is one of them. A proper and stable suture results in better tissue healing and right biological reactions. Suture plays an important role in healing, enabling reconstruction and reassembly of the soft tissue separated by the surgical procedure and at the same time facilitate and promote healing and hemostasis [6].
In case of immediate loading procedures, correct suturing avoids impression material penetration and facilitates the prosthetic hygiene. Wound dehiscence after surgeries compromise the potential of reparation and regeneration, increasing implant crestal bone loss [7] and the risk of infection [8].
Well known full arch technique treatment has been used for protocols of immediate loading. This technique involves the placement of four implants for rehabilitation of fully edentulous dental arches and with diminished bone volume. The implants should be well anchored, tilted 45 degrees (achieving a primary stability of at least 30 Ncm). The success rate for this technique has been described with a high success rate (98% for the maxilla and 98.1% for the mandible after 5 to 10 years of follow-up [9].
As transosseous suture is a technique commonly used in orthopedics in order to reapproximate tissues and adequate closure of the surgical wound is one of the most important aspects of an implant surgery [10]. The aim of this communication is to introduce an alternative technique for suture after a full arch implant surgery, reducing incidences of wound dehiscence.
A 52-year-old man presented at the Oral Implant Dentistry Department of the Faculty Ilapeo, Curitiba, Brazil. The same complained of generalized mobility in the lower teeth. At the first moment, anamnesis and radiographic examination were performed. At the time of the clinical and radiographic examination was noted the presence of periodontal disease with points of exacerbation, generalized bone loss and mobility grade 2 in teeth (Figure 1 and Figure 2). It was suggested the extraction of the inferior dental elements for placement of dental implants and installation of a denture about implants with immediate loading.
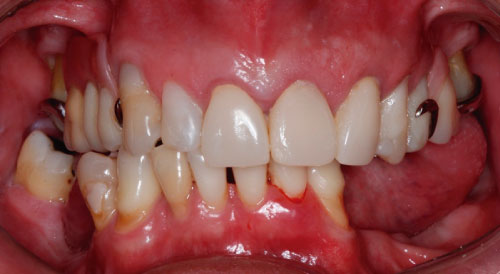 Figure 1: Clinical image showing the initial oral condition of the patient.
View Figure 1
Figure 1: Clinical image showing the initial oral condition of the patient.
View Figure 1
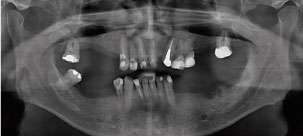 Figure 2: Preoperative panoramic radiography.
View Figure 2
Figure 2: Preoperative panoramic radiography.
View Figure 2
The implants selected for this case present some important characteristics: 1) Hybrid conical implants with compacting threads in the coronal area and cutting threads in the medial and apical third; 2) Double threads for minimal trauma and faster placement; 3) Conical apex with low-activity cameras and helical flutes designed to optimize primary stability. Regarding the abutments, it was installed mini conical angled abutment which has an anatomical design to improved soft tissue accommodation (Figure 3).
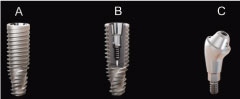 Figure 3: A,B) Helix Grand Morse Acqua implant (Neodent, Curitiba, Brazil); C) Mini conical angled abutment (Neodent).
View Figure 3
Figure 3: A,B) Helix Grand Morse Acqua implant (Neodent, Curitiba, Brazil); C) Mini conical angled abutment (Neodent).
View Figure 3
After the local anesthesia, supracrestal and oblique incision and detachment of the flap was performed, and after alveolar bone regularization, the proper implant length was checked. Multiple teeth extractions were performed and the drill sequence was followed by conical drill 3.5 mm, 3.75 mm and conical contour 3.75 drill. Four implants Helix GM Aqua 4.0 × 16 mm (Neodent) were placed 2 mm subcrestal, all with minimum torque of 60 Ncm. Four mini conical abutments (Neodent) were installed at 2.5 mm of gengiva height (Straight abutment for the anterior implants and 17 degrees angled in the posterior implants). A small perforation was performed in the lingual/buccal face of alveolar bone, between implants previously placed, using a straight handpiece with a 1.1 mm diameter drill for grafting screws, (Neodent) at a 45 degrees inclination to the bone platform (Figure 4).
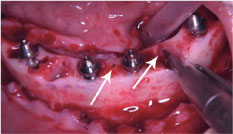 Figure 4: Perforation performed in the lingual/buccal face of alveolar bone, between implants previously placed, using a straight handpiece with a 1.1 mm diameter.
View Figure 4
Figure 4: Perforation performed in the lingual/buccal face of alveolar bone, between implants previously placed, using a straight handpiece with a 1.1 mm diameter.
View Figure 4
Suture was performed with mononylon (4-0, J&J Ethicon, Cincinnati, USA) from the buccal soft tissue to the channel created (towards the lingual bone) and was closed through the lingual soft tissue (Figure 5 and Figure 6).
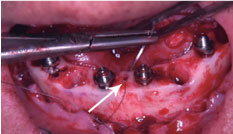 Figure 5: Needle passing through the soft lingual tissue.
View Figure 5
Figure 5: Needle passing through the soft lingual tissue.
View Figure 5
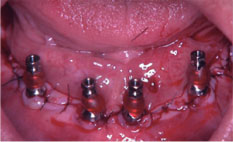 Figure 6: Suture of the finished region.
View Figure 6
Figure 6: Suture of the finished region.
View Figure 6
This procedure should be done between all implants placed. After suturing the mandibular region, impression copings were positioned in the mini conical abutments and attached to the multifunctional guide by acrylic Pattern Resin (GC America Inc, Alsip, USA). With the upper and lower guides in position, a 3-point occlusal registration was performed considering the vertical dimension previously determined. The impression was done with condensation silicone Speedex (Coltene, Altstätten, Switzerland). The impression copings were unscrewed, the impression was removed and sent to the laboratory for manufacture the metal bars and the teeth assembly (Figure 6). The prosthesis was acrylated and installed in the third postoperative day. The occlusal adjustment was performed maintaining bilateral stability at maximum intercuspation, contacts and occlusal forces equally distributed, anterior guide and smooth lateral mandibular excursions without work-side and non-working interferences.
The suture was removed 15 days after surgery and oral hygiene orientation was performed.
The clinical and radiographic control was done after 1, 2, 3, and 4 and 12 months (Figure 7 and Figure 8).
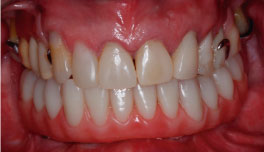 Figure 7: Final condition of the patient with the inferior prosthesis installed.
View Figure 7
Figure 7: Final condition of the patient with the inferior prosthesis installed.
View Figure 7
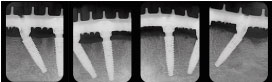 Figure 8: Healing around the mini-abutments after 12 months of surgery.
View Figure 8
Figure 8: Healing around the mini-abutments after 12 months of surgery.
View Figure 8
The presence of a marginal space between the implant and the abutment may lead to greater marginal bone loss due to the penetration of bacteria at the implant-abutment interface [11]. The conical implant-abutment systems have delayed or even prevented bacterial colonization through the use of the platform switching concept, resulting in improved implant system performance [11,12]. Another important point is the precision of the adjustment or passive adaptation, and several factors can influence the final adaptation: The structure of the wax pattern, the casting process, the production of the final prosthesis and the delivery of the same [13].
Over the years complications associated with misfit in the prosthesis-implant or implant-abutment structure have been reported, such as: Mechanical failures, pillar rotation, loosening or fracture of prosthetic screws, poor distribution of forces and biological failure, such as adverse tissue reactions, sensitivity and pain [14]. However, peri-implant bone remodeling seems to alleviate the magnitude of the misfit, implying that structural misfit is not the cause of bone resorption and loss of implants [15].
The success of the immediate loading can be partially attributed to the splinting effect provided by a full bar, joining all the implants, the rigorous oral hygiene regime and the standardization of surgical and prosthetic procedures [16]. The short-term success of immediate loading in mandibular protocols was comparable to that of late loading protocols [15]. Papaspyridakos, et al. [17] suggested the immediate loading as an excellent alternative to overcome the problems of conventional loading. The technique proposed in this case may exemplify an alternative to rehabilitate our patients in a less morbid way. The present study demonstrated excellent stability of implants with immediate loading over a period of 12 months, without early failure and complications.
A modified suture was presented, which reduces the possibility of penetration of impression material in implant surgeries with immediate prosthetic rehabilitation. It might reduces the risk of infection and promotes faster healing. After 12 months of follow-up, the implants and prosthesis were in good condition, maintaining healthy of soft tissue and bone around the implant platform. More studies are needed with a greater number of patients and longer time of proservation.
A consent form to publish the case with the clinical photography and radiography was signed by the patient.
This research did not receive any specific grant from funding agencies in the public sectors.
The authors Thome G, Trojan LC, Cartelli CA, Moura MB, Bernardes SB declare a conflict of interest. Both authors work at Neodent, manufacturer of the implants and components used in this case report. However, the authors had no influence on the results.
Thome G: contributed with the conception of the work; data acquisition and analysis, drafting the work; and final approval of the work. Berry T: contributed with data acquisition; drafting; and final approval of the work. Thome G and Trojan CL: contributed with data acquisition; drafting; and final approval of the work. Trojan CL: contributed to the conception of the work; revising; and final approval of the work. Cartelli CA: contributed with data acquisition; drafting; and final approval of the work. Moura MB and Bernardes SB: contributed to the conception of the work; revising; and final approval of the work.